Abstract
Ocular drug delivery has constantly challenged ophthalmologists and drug delivery scientists due to various anatomical and physiological barriers. Static and dynamic ocular barriers prevent the entry of exogenous substances and impede therapeutic agents' active absorption. This review elaborates on the anatomy of the eye and the associated constraints. Followed by an illustration of some common ocular diseases, including glaucoma and their current clinical therapies, emphasizing the significance of drug therapy in treating ocular diseases. Subsequently, advances in ocular drug delivery modalities, especially nanotechnology-based ocular drug delivery systems, are recommended, and some typical research is highlighted. Based on the related research, systematic and comprehensive characterizations of the nanocarriers are summarized, ho** to assist with future research. Besides, we summarize the nanotechnology-based ophthalmic drugs currently on the market or still in clinical trials and the recent patents of nanocarriers. Finally, inspired by current trends and therapeutic concepts, we provide an insight into the challenges faced by novel ocular drug delivery systems and further put forward directions for future research. We hope this review can provide inspiration and motivation for better design and development of novel ophthalmic formulations.
Graphical abstract

Similar content being viewed by others
Introduction
The eye, a highly complex, isolated and specialized organ, is the most significant sensory organ of the human body because about 80% of all sensory input is acquired via the eye [1]. Anatomically, ocular tissues are protected by dynamic and static barriers [2]. Tear turnover, reflex blinking, and nasolacrimal drainage prevent foreign substances away from the eye surface [2, 3]. The eyelid, conjunctiva and corneal epithelium cover and protect the eye surface [4]. In addition, the blood- aqueous barriers (BAB) and blood-retina barriers (BRB) limit the entry of compounds from the systemic circulation [5]. This defense system is further assisted by enzymes and other barriers (sclera, retinal etc.) [6, 7].
Although there are multiple protective mechanisms, the eyeball is still vulnerable to infection, trauma and other injuries due to its communication with the outside [8]. The World Health Organization reports that at least 2.2 billion people around the world have visual impairment [9]. Ocular diseases, such as keratitis [10], cataract [11], glaucoma [12], age-related macular degeneration (AMD) [13] and diabetic retinopathy (DR) [14] can seriously damage the patients' visual acuity and affect their life quality. The National Eye Institute estimated that the annual economic burden associated with eye conditions and vision impairment in the US is about $139 billion [15].
Drug therapy is the primary treatment for most eye diseases [16]. Delivering drugs to target eye tissues at the desired therapeutic concentration without damaging healthy tissues is a current research hotspot [17]. Ocular drug delivery systems (ODDS) are designed to: (1) overcome ocular barriers to deliver drugs to target eye tissues, (2) improve drug stability and treatment efficiency, (3) prolong drug retention time and reduce dosing frequency, (4) enable multiple drug combinations, and (5) improve patient adherence and reduce drug-related adverse events [18, 19].
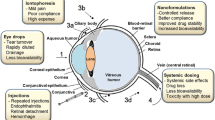
Traditional administration methods, such as topical eye drops, conjunctival and scleral administration, intracameral administration, intravitreal injection, retrobulbar injection and systemic administration, are widely used clinically and have achieved certain therapeutic effects [20]. However, as mentioned earlier, the presence of ocular barriers poses a significant challenge for therapeutics in terms of reaching the intended site and staying there for a sufficient duration. As a result, the bioavailability of these therapeutics is often limited, typically less than 5% [21].
With the development of nanotechnology, dynamic progress has been made in the field of ocular drug delivery, which provides new therapeutic interventions for ocular diseases [21, 22]. Compared with traditional drug administration, nanocarriers offer numerous advantages, including the capacity to overcome ocular barriers, promote transcorneal permeability, prolong drug residence time, reduce drug degradation, reduce dosing frequency, improve patient compliance, achieve sustained/controlled release, drug targeting and gene delivery [23]. Novel drug carriers, such as nanomicelles, nanoparticles (NPs), nanoemulsions (NEs), microemulsions, nanofibers, dendrimers, liposomes, niosomes, nanowafers, microneedles (MNs), have been investigated for the therapy of anterior and posterior ocular diseases [24].
In this review, we attempted to provide a holistic overview of novel ODDS reported in the past five years. First, we described the specific anatomy of the eye and the ocular barriers, illustrating the key factors that lead to the low bioavailability of the therapeutics. Subsequently, based on the current treatment status of ophthalmic diseases, several conventional and alternative routes of administration were summarized and compared, especially their limitations and innovative progress. Then, we discussed the recent advances in novel nanocarriers, such as nanomicelles, NPs, nanosuspensions, microemulsions, dendrimers, liposomes, etc. and highlighted some recent research. In particular, we also introduced gene therapy, exosome and self-nano emulsifying drug delivery systems (SNEDDS), which have huge potential in ocular drug delivery. In view of the reports of these ODDS, we highlighted their characteristics to assist with future related research. Meanwhile, ophthalmic drugs currently on the market or still in clinical trials were summarized, as well as the recent patents of nanocarriers. Finally, inspired by current trends and therapeutic concepts, we focused on novel non-invasive ODDS to overcome ocular barriers, sustain drug release, and maintain effective drug levels at the therapeutic target. Although most current research is still in the basic research stage, ocular drug delivery based on nanotechnology is expected to become the main means of ocular drug therapy.
The anatomy and barriers of the eye
The anatomical structure of the eyeball can be divided into the anterior and posterior segments based on the lens. Figure 1 illustrates the anatomy of the human eye. The anterior segment includes the cornea, conjunctiva, iris, ciliary body, aqueous humor and lens, while the posterior segment includes the sclera, choroid, retina and vitreous body [25, 26].
Various absorption barriers exist in the human eye (Fig. 2) [27]. They are briefly divided into static and dynamic barriers to prevent foreign substances, including therapeutic agents, from targeting various eye tissues [28]. Static barriers of the eye mainly include cornea, conjunctiva, sclera, vitreal barrier, BAB and BRB, while dynamic barriers primarily include tear film, tear turnover, nasolacrimal duct drainage, conjunctival and choroidal blood flow and lymphatic clearance [29,30,31]. These barriers limit the passive absorption of diverse therapeutic molecules, thereby reducing the ocular bioavailability of different agents. Details are described below to understand the absorption barriers further.
Drug delivery barriers in ocular routes [26]. The absorption barriers of the eye mainly include tear film barrier, corneal barrier, conjunctival and scleral barriers, vitreal barrier, blood-aqueous barrier, blood-retinal barrier.
Tear film, tear turnover, nasolacrimal duct drainage
The tear film is a thin, transparent fluid layer consisted of three layers: a surface lipid layer, an intermediate aqueous layer, and an inner mucin layer [32]. The lipid and water layers act as barriers for hydrophilic and hydrophobic drugs, respectively [33]. Mucins are negatively charged macromolecules that attract or repel drugs through electrostatic interactions and protect the eye's surface from harmful external stimuli and pathogens [34]. At the same time, the non-specific binding of drugs to tear enzymes (such as lysozyme), mucin layers, and proteins (such as albumin) prevents drugs from reaching the cornea and anterior chamber [35].
In addition, tear turnover increases after topical insolation of drugs, resulting in rapid clearance of drug molecules through nasolacrimal drainage (within one to two minutes) [6, 36]. Meanwhile, due to the limited surface area of the eye, ~ 30 μL of the drug dropped into the eye is quickly expelled down the lacrimal passage until the tear fluid returns to the normal volume (7–9 μL) [37]. Approximately 60% of the drug is eliminated 2 min after treatment with topical eye drops. After 8 min, the drug is diluted to 0.1%, and after 15 to 25 min, almost all the active ingredients are removed from the corneal surface [38].
Cornea
The healthy cornea is a clear, avascular tissue and the main barrier for foreign substances to enter the anterior chamber [39]. Structurally, it comprises five layers: the outer epithelium, Bowman's membrane, intermediate stroma, Descemet's membrane and endothelial layer [40]. The barriers preventing drug penetration into parenchyma are mainly epithelial, stromal and endothelial layers [41].
The corneal epithelium is characterized by tight junctions within the surface cell layer [37]. Due to its lipophilicity, it is an obvious obstacle, especially for hydrophilic compounds [42]. Besides, the existence of cytochrome P450 (drug-degrading enzymes) and drug efflux pumps in epithelial cells is another reason for low drug bioavailability [24, 117].
Retrobulbar injection
The retrobulbar route involves injecting needles through the eyelid and orbital fascia to deliver drugs to the retrobulbar space [118, 119]. Retrobulbar injection of triamcinolone acetonide treats macular oedema caused by retinal vein occlusion [120]. The antifungal effect of retrobulbar injection of amphotericin B is higher than intravenous injection [121]. Retrobulbar injection of chlorpromazine is used to treat painful blind eyes [122].
Systemic administration
Systemic administration (including parenteral and oral dosing) is an alternative method of drug delivery. At present, systemic administration has been used to deliver antibodies, antibiotics, and carbonic anhydrase inhibitors to treat diseases such as endophthalmitis, elevated intraocular pressure, and uveitis [123,124,125,126]. Nevertheless, due to the ocular barriers and the tight junctions of the retinal pigment epithelium that allow only one to two per cent of the drug to reach the retinal and vitreous regions, frequent administrations are required to obtain the desired therapeutic effect, which may contribute to systemic side effects and poor patient compliance [108, 127]. Therefore, it is not an ideal mode of administration.
Pharmacokinetics
Based on the ocular barriers and drug administration described above, ocular pharmacokinetics, including penetration and elimination, are discussed in detail. As shown in Fig. 4 [6, 128], it mainly contains the following pathways: (1) through the tears and cornea into the anterior chamber, (2) non-corneal permeation into the anterior uvea through the conjunctiva and sclera, (3) drug from the bloodstream cross BAB to the anterior chamber, (4) drug from the aqueous humor cross BAB to the systemic circulation, (5) drug elimination from the aqueous humor to the trabecular meshwork and Schlemm's canal, (6) drug distribution from the circulation through BRB to the posterior segment of the eye, (7) intravitreal administration, (8) elimination from the vitreous body into the posterior compartment via an anterior route, and (9) elimination from the vitreous body via a posterior route through BRB.
Nanotechnology-based ocular drug delivery systems
To overcome ocular drug delivery barriers and improve drug bioavailability, novel drug delivery systems have been developed. Nanocarriers' development offers many advantages, including overcoming ocular barriers, promoting transcorneal permeability, prolonging drug residence time, reducing the dosing frequency, improving patient compliance, reducing drug degradation, achieving sustained/controlled release, drug targeting and gene delivery [23]. Many ocular drug delivery systems such as nanomicelles, NPs, nanosuspensions, NEs, microemulsions, nanofibers, dendrimers, liposomes, niosomes, nanowafers, MNs and exosomes (Fig. 5), have shown splendid delivery potential in both vitro and vivo studies, enhancing drug permeability across the ocular barriers and prolonging the residence time in the eye [23, 129].
Nanomicelles
Nanomicelles are core–shell nanocarriers formed by spontaneous assembly of amphiphilic copolymers with hydrophobic groups as the core and hydrophilic groups as the outer shell [130]. Usually, the particle size ranges from 10 to 100 nm and can be divided into three categories: polymers, surfactants, and multi-ion composite nanomicelles [131]. Besides, hydrophobic interactions, hydrogen bonds, electrostatic interactions, etc., are the driving forces for polymer micelle formation [132]. Positive micelles are generally formed when the hydrophobic moiety forms clusters within the core and the hydrophilic moiety is aligned outwards to increase contact with water. Likewise, when the opposite arrangement occurs, the aggregates are referred to as reverse micelles [133]. Positive micelles are used to encapsulate, solubilize, and deliver hydrophobic drugs, whereas reverse nanomicelles are used to encapsulate and deliver hydrophilic drugs [134]. The unique chemical structure of nanomicelles can solubilize drugs internally, reduce adverse reactions, improve the stability of drugs, and have a sustained release effect, regarded as safe alternatives for ocular drug delivery [135, 136].
Cyclosporine is an immunomodulatory drug employed in treating DED. Given its relatively high molecular weight and poor permeability, Ghezzi et al. prepared micelles using tocopherol polyethene glycol 1000 succinate (TPGS) and Solutol®HS15 for cyclosporine delivery. Meanwhile, the addition of α-linolenic acid was evaluated based on the results of using fatty acids for micelle preparation [137, 138] and drug loading [139, 140]. Also, the effect of TPGS as a corneal permeability promoter and irreversible changes in tissue permeability were analyzed. It was demonstrated that TPGS micelles (approximately 13 nm in size), loaded with 5 mg/mL cyclosporine, facilitated drug retention in the cornea and sclera and possessed good tolerance for ocular applications [141].
Besides, XU et al. developed chitosan oligosaccharide-valylvaline-stearic acid (CSO-VV-SA) nanomicelles and hydrogen-castor oil 40/octyl alcohol 40 (HCO-40/OC-40) hybrid nanomicelles for topical ocular drug delivery. Neither nanomicelles produced significant cytotoxicity in human corneal or conjunctival epithelial cells. Dexamethasone in both nanomicelles was detectable in rabbit tears for over 3 h. Notably, the delivery efficiency of CSO-VV-SA nanomicelles was not inferior to HCO-40/OC-40 hybrid nanomicelles at both cellular and animal levels, which suggested that CSO-VV-SA nanomicelles would have further potential for clinical translation as novel drug delivery carriers [142].
Traditional intravitreal injection of anti-VEGF into the posterior part of the eye to treat retinal diseases is invasive and accompanied by various complications. A nano-micelle drug delivery system composed of polyethene glycol (PEG), polypropylene glycol, and polycaprolactone (PCL) fragments was developed to avoid these. The copolymer EPC (nEPC) locally delivers aflibercept to the posterior segment of the eye via the corneal-scleral routes. Animal experiments have shown that aflibercept-loaded nEPCs (nEPCs + A) can penetrate the cornea in an ex vivo porcine eye model and deliver aflibercept to the retina to promote choroidal neovascularization (CNV) regression in a mouse model of laser-induced CNV. Besides, nEPCs + A showed good biocompatibility and intrinsic anti-angiogenic properties. These findings suggest that nEPCs may be promising candidates for further clinical applications [143].
NPs
NPs are colloidal drug carriers with ideal sizes ranging from 10 to 100 nm [21]. They are mainly divided into polymer and lipid NPs [144]. NPs used in ocular preparations are composed of lipids, proteins, and natural or synthetic polymers such as albumin, sodium alginate, chitosan, polylactide-coglycolide (PLGA), polylactic acid (PLA), and PCL [145]. Besides, the surface charge of NPs highly affects their effective ocular absorption. Since corneal and conjunctival tissues have negatively charged surfaces, cationic NPs have a higher retention time on the ocular surface than anionic NPs [146].
To date, NPs have been used widely to deliver drugs to the targeted tissue in the eye, with the advantages of: (1) smaller and less irritating; (2) providing sustained drug release to avoid repeated dosing; (3) preventing non-specific uptake or premature degradation; (4) providing better absorption and improving intracellular penetration; and (5) targeted delivery to desired tissues [42, 147,148,149].
As a synthetic polymer, PLGA has been widely used to prepare NPs for ocular drug release due to its biodegradability, excellent biocompatibility, and capacity to modulate drug release by altering molecular weight, terminal groups, and the lactide-to-glycoside ratio [150, 151]. The US Food and Drug Administration (FDA) has approved various drug delivery products with PLGA.
In one study, chitosan-coated polylactide-glycolic acid NPs (CS-PLGA NPs) were developed to deliver Bev (an anti-VEGF drug used widely for treating DR) to the posterior chamber of the eye. The confocal laser scanning microscopy and pharmacokinetics showed that CS-PLGA NPs had better permeability than the traditional drug solution, with higher concentrations of Bev (above 22 ng/mL for 6 weeks) in the posterior ocular tissues. In the retinopathy model, subconjunctival injection of CS-PLGA NPs significantly reduced the level of VEGF in the retina for 12 weeks compared with local and intravitreal injections. Thus, CS-PLGA NPs can potentially be used to target the retina for drug delivery [152].
Kim et al. delivered NPs loaded with the drug latanoprost into the eye by iontophoretic method to treat glaucoma. These NPs were made of PLGA and had the advantages of releasing the latanoprost sustainably and prolonging the drug residence time. The 300 nm NPs showed the most durable drug effect in vivo. It lasted more than 7 days and increased its efficacy by approximately 23-fold compared to Xalatan® (a commercially available latanoprost eye drop), which offers a new strategy for prolonging the efficacy of drugs and reducing the frequency of drug administration in the treatment of glaucoma [153].
Likewise, Nguyen et al. developed hollow polylactic acid NPs and innovatively investigated the role of shell thickness in develo** long-acting drug carriers to treat glaucoma effectively. Among the four NPs with an adjustable shell thickness of 10 to 100 nm (~ 10, 40, 70, and 100 nm), a medium-thickness shell (~ 40 nm) manifested the most effective release curve of pilocarpine and sustained relief of high IOP for more than 56 days in the rabbit glaucoma model, which may protect the structural integrity of the corneal endothelium, as well as attenuate retinal and optic nerve degeneration (Fig. 6). Thus, this finding implies the potential of the shell thickness effect in develo** long-acting drug delivery systems that can be used to treat some chronic eye disorders [154].
The representative images of rabbit eyes taken with a slit-lamp biomicroscope after intracameral administration of pilocarpine-loaded HPLA NP (st10, st40, st70, and st100) dispersions or BSS buffer (Ctrl group) at 0 (a) and 56 (b) days. c The scores of slit-lamp examinations at 56 days d Central corneal thickness at 56 days. e The histology of corneal tissues at 56 days postoperatively
In contrast to polymeric NPs, lipidic formulations are known to be less stable for sustained drug release. Recently, adding polymers to lipidic NPs formulations has gained wide interest in increasing the stability of nanocarriers [16]. Schnichels et al. investigated lipid DNA NPs functionalized for the loading of brimonidine through specific aptamers and via hydrophobic interactions with double-stranded micelles. Both NP types significantly reduced IOP in living animals. Overall, IOP reduction was observed in 74% (SEM: ± 3%) and 54% (SEM: ± 1%) of the number of animals treated with two types of DNA NPs once daily for 5 weeks, compared to the animals treated with the original brimonidine(36%, SEM: ± 3%). Importantly, NPs loaded with brimonidine showed no toxicity and improved efficacy. In conclusion, these drug delivery systems offer great opportunities to treat glaucoma [155].
To improve the biocompatibility of the NPs, it is worth noting that the combination of biomimetic technology and NPs has brought new ideas for non-invasive drug delivery to the eye. Chen et al. reported adhesive and therapeutic biomimetic nanocoatings on ocular surfaces using sebocyte membranes with integrin-β1 overexpressed to coat NPs. The NPs specifically bind to the Arg-Gly-Asp sequence of fibronectin in the ocular epithelium, which is critical in supplementing the lipid layer, stabilizing the tear film and prolonging the retention time for 24 h. In mouse and rabbit DED models, dexamethasone-loaded nanocoatings effectively reduced corneal opacity and inflammatory cytokine levels, improved corneal epithelial recovery and restored tear secretion. This study provides new insights to protect the ocular surface and prolong the retention time of the drug [245]. Since hydrogels can improve the therapeutic effect of ophthalmic drugs through the following mechanisms, including (1) prolonging the retention time of drugs at the site of drug delivery, (2) sustained drug release at the target site, and (3) the co-delivery of multiple drugs to their function [97, 116, 246, 247].
The combination of nanotechnology and hydrogels has significantly progressed the treatment of ocular diseases [18]. Various nanoformulations such as NPs, nanomicelles, MNs, and nanofibers have been combined to prepare composite systems to further prolong the retention time of drugs on the ocular surface and improve their bioavailability [248]. Some representative hydrogels used in ocular drug delivery will be detailed in the following sections and emphasized with a few appealing examples.
Fang et al. developed a polypseudorotaxane hydrogel for treating anterior uveitis by mixing Soluplus micelles (99.4 nm) with cyclodextrins solutions. The optimized hydrogel exhibited shear thinning and sustained release properties. In the endotoxin-induced rabbit uveitis model, the hydrogel significantly improved the drug retention ability (21.2 folds), corneal permeability (1.84 folds), intraocular bioavailability (17.8 folds), and anti-inflammatory effect compared with drug solutions. In addition, cytotoxicity and eye irritation studies also confirmed the good biocompatibility of the hydrogel. In conclusion, this study demonstrated that γ- cyclodextrins-based hydrogels have great potential for treating anterior uveitis [249].
Patients with wet AMD require an intravitreal injection of Bev or other drugs. Jung et al. developed an in situ formed hydrogel consisting of Bev and hyaluronic acid cross-linked to poly (ethylene glycol) diacrylate, which was slowly released after Bev injection into the suprachoroidal space of the eye using MNs. The in-situ formed Bev-hyaluronic acid hydrogel was well tolerated and released Bev for over 6 months in the rabbit eye, which could be used in treating posterior ocular diseases in the future [250].
Recently, Gao et al. developed an injectable antibody-loaded supramolecular nanofiber hydrogel by mixing betamethasone phosphate, the gold-standard anti-VEGF agent for AMD, with CaCl2. This betamethasone phosphate-based hydrogel can release anti-VEGF to inhibit retinal vascular proliferation, attenuate CNV for a long time, and remove ROS to reduce local inflammation (Fig. 10). Notably, the duration of anti-VEGF can be effective for approximately threefold longer than conventional administration, can reduce the frequency of administration and improve patient compliance [251].
The long-term effect of the laser-induced mice CNV model using Anti-VEGF@BetP-Gel. a Experimental design to evaluate the impact of Anti-VEGF@BetP-Gel. b Fluorescence IVIS imaging demonstrating the in vivo retention of IgG-Cy5.5 at various time periods after intravitreal injection of free IgG-Cy5.5 or IgG-Cy5.5@BetP-Gel. c H&E-stained transverse CNV sections after 4 weeks intravitreal injection. d The typical fluorescein fundus angiography images of laser-induced mice CNV model taken at 1, 2, and 4 weeks following intravitreal injection. e The graded and measured angiogenic vascular leakage values
In short, combining hydrogels and nanotechnology expands the range of biomedical applications and opens new windows for ocular drug delivery.
Microneedles
Microneedle technology is an attractive, minimally invasive strategy with the advantages of easy drug administration, controlled drug release, and low manufacturing cost [252]. It has been widely studied for transdermal delivery of various therapeutic drugs (e.g., anti-diabetes, anti-obesity drugs, and vaccines) [253]. Various MNs have been exploited and tested, such as solid MNs, hollow MNs, and dissolved MNs [254, 255]. Due to its excellent patient tolerance and efficacy have prompted researchers and pharmacists to explore its use in treating ocular diseases.
Fungal keratitis (FK), an infectious corneal disease, is a serious cause of visual impairment worldwide. Shi et al. manufactured a dissolved microneedle array patch based on PLA and hyaluronic acid to treat FK. Among them, a 30% PLA-hyaluronic acid MN patch reversibly penetrated the corneal epithelial layer, and the cornea recovered completely within 12 h. More importantly, it demonstrated that the therapeutic effect of self-implantation of drug-loaded MN patches as a controlled release reservoir for local drug delivery is much better than that of eye drops in the rabbit model of FK. Hence, the MN patch serves as an ocular drug delivery system with efficient and rapid corneal healing ability, which may also open a new avenue for the clinical treatment of FK [256].
Besides, Cui et al. developed cryo-MNs for the ocular delivery of living bacteria. In cell experiments, the device delivered predatory Bdellovibrio bacteriovorus, which could successfully inhibit the proliferation of gram-negative bacteria. In a mouse ocular infection model, infection was reduced by nearly six-fold after 2.5 days of treatment, and corneal thickness and morphology were unaffected; this brings new insights for the safe and effective delivery of novel antimicrobial agents to the impermeable ocular surface [257].
Lee et al. developed a self-plugging MN (SPM) to perform intraocular drug delivery and seal the scleral tissues at the same time. SPMs were fabricated by a thermal stretching process and then coated with a drug-loaded polymer carrier and a biocompatible hydrogel. Each coating functional layer was characterized and explained in vitro and ex vivo experiments. The 10 mm-long SPM released over 95% of the coated drug (27.9 μg) gradually within 24 h. Furthermore, the ability of SPM to achieve rapid closure and sustained intraocular delivery was confirmed using a porcine model [258].
However, MN products' performance and quality evaluation involves several vital technical parameters, such as bending property, loading capacity, and safety in use. At the same time, MNs can cause tissue damage and have high technical requirements for clinicians, so there is still a long distance to realize the clinical transformation of MNs.
Other promising ocular drug delivery methods
Gene therapy
Gene therapy is a hot topic in the research of modern ophthalmic diseases. There are two strategies for gene therapy: (1) restoring the function of nonfunctional or missing proteins (gene addition or gene editing) and (2) knocking down proteins to block their function (gene silencing) [259].
The eye has important features well suited for gene therapy: well-defined anatomy, relative immunological privilege, accessibility, simplicity of diagnosis, and one eye can be used as an experimental target and the other as a control in the same subject [259]. There are more than 350 hereditary eye diseases, including choroiditis, retinitis pigmentosa, Leber congenital amaurosis, etc., involving various genetic loci [260, 261]. In addition, gene therapy approaches are also being exploited and extended to diseases not unrelated to a single genetic defect, such as corneal and retinal vascular disease or AMD [262, 263]. Gene delivery systems primarily include viral vectors, non-viral vectors, gene editing techniques (mainly CRISPR-Cas9), and epigenetic treatments with antisense oligonucleotide (ASO) and RNAi therapeutics [264].
Viral vectors
Viral vectors are often therapeutic gene vectors due to their high transduction efficiency. Several viral vectors, such as adenovirus, adeno-associated virus (AAV), retrovirus and lentivirus, have been widely used in ocular gene therapy [23]. The stability of different nano-systems can be estimated by short-term stability (3 months), centrifugation test, freeze–thaw cycle, heating–cooling cycle and high-temperature storage [314]. A promising approach to improve biological stability is pegylated. As a hydrophilic non-ionic polymer with high chain flexibility, PEG-coated or coupled on the surface of nanocarriers can prevent macrophage clearance by reducing contact with the surrounding environment (oxidants, enzymes, and other degraders) [315,316,317]. Besides, in vivo drug flux studies have shown that pegylated nanostructured lipid carriers have nearly twofold higher levels of ciprofloxacin in all ocular tissues than non-pegylated nanostructured lipid carriers at 2 h after administration [315].
Refractive index (RI)
Refractive index is measured by Abbe’s refractometer to determine soft contact lenses' water content, salinity and sugar concentration [318]. The tear RI was generally between 1.340 and 1.360. Therefore, the recommended RI value for ocular formulations must be < 1.476 [319, 320]. For instance, the RI values of intraocular NEs prepared by Ismail et al. ranged from 1.334 to 1.338, which was satisfactory to meet the demands [179].
pH
pH measurement plays a critical role in preparing stable and non-irritating ocular formulations. It has been reported that acidic (pH < 4) or alkaline (pH > 10) solutions can cause chemical damage to the eye [61]. Therefore, the appropriate pH of topical ophthalmic formulations ranges from 6.6 to 7.8 [321]. Compared with Travatan® eye drops, the pH value of the prepared NEs is between 5.5 and 5.9, which is suitable for ocular instillation and can treat DED [179].
Retention
Ocular retention is a fundamental property of ocular delivery systems because it prolongs the duration of drug action, reduces the frequency of drug administration, and improves drug bioavailability [17]. Nanosystems with larger surface areas, such as thin films, hydrogels, have longer diffusion and contact time on the corneal surface, which enhance eye retention. In general, γ-scintigraphy, texture analysis, fluorescence imaging and surface plasmon resonance spectroscopy are used to determine the intraocular retention of nano preparations [17, 61, 322].
Viscosity
The viscosity of ocular preparations is generally less than 20.0 mPa [323], while the appropriate viscosity of ocular preparations is generally 2–3 mPa [311]. It was reported that the nano-formulations with higher viscosity and lower surface tension could prolong retention times [324]. Synthetic polymers (such as polyacrylate and PVA) and natural polymers (such as hyaluronic acid, alginate) can be used as viscosity enhancers. For example, in vivo anterior corneal retention assay showed that the Chitosan Oligosaccharides-coated nanostructured lipid carrier increased 7.7-fold compared with the uncoated lipid carrier [325].
Osmolality/Isotonicity
Osmolality was determined based on four properties of ocular or tears formulation parameters known as vapor pressure, osmotic pressure, boiling point, and freezing point [326]. In addition, osmolality can also be measured in terms of the number of moles of solution per liter or kilogram [327]. It was reported that ocular preparations with osmolarity less than 100 mOsm/kg or more than 640 mOsm/kg were named as eye irritants depending on the droplet volume [61].
Drug loading and release
Drug loading and release are essential to the ocular drug delivery system. Nanocarriers require a high drug payload, which can improve biocompatibility and achieve better therapeutic effects [94]. The primary determinant of drug load is drug solubility. The drug is released continuously in nanocapsules with high encapsulation efficiency, and the release rate is critical to achieve an effective therapeutic effect and avoid drug toxicity. [328]. Pharmacokinetics can be studied via a series of in vivo and in vitro experiments. For example, the content of drugs can be detected in tears and aqueous humor through ELISA (Enzyme-linked Immunosorbent Assay) or HPLC (High Performance Liquid Chromatography) in vitro [329, 330]. Alternatively, fluorescence-labeled drugs could be used and then detected by confocal microscopy in vivo [331]. Besides, the results can be analyzed by some pharmacokinetic parameters, such as the maximum drug concentration (Cmax), the time required to reach Cmax (Tmax), and the area under the concentration–time curve (AUC0-t) [332].
Biocompatibility and safety
Biocompatibility and safety are critical for nanocarriers. The primary safety concerns of nano-formulation arise from the surfactants and cationic lipids used in the formulation, which may damage corneal epithelial cells during long-term use [333,334,335]. The safety of eye preparations was evaluated by various tests, such as HEM-CAM test, Schimer's test, Draize's test, histopathological studies and cell viability studies [23]. Using surfactants and cationic lipids may create safety issues that should be further optimized and improved during development [333]. In the HEM-CAM test, ocular toxicity and irritation were predicted by observing the changes in blood vessels [336].
Approval and under clinical status of nanotechnology-based delivery systems for ocular diseases
With the increasing number of products on the market, the development of nanotechnology for the treatment of ocular diseases seems promising. Table 2 lists some FDA-approved nanocarriers for ocular diseases.
For example, Restasis® was the first cyclosporine A (CsA) oil-in-water emulsion approved by the FDA for the treatment of DED in 2002 [337]. It used polysorbate-80 as an emulsifier and 0.5 mg/ml CsA was dissolved in castor oil. Importantly, the preservative-free emulsions (particle size 100–200 nm) effectively avoided the toxicity shown by earlier preservative-containing formulations. Nevertheless, Restasis® is still accompanied by side effects such as epiphora, eye irritation and instillation pain [338].
Besides, Cequa® is a nano-micellar formulation containing 0.09% CsA that is designed to improve drug delivery and penetration to ocular tissues. Cequa® was approved by the FDA in 2018 for the treatment of DED [339]. The micellar formulation is composed of poly-oxygenated hydrogenated castor oil and octoxynol-40, which could form thermally stable micelles simultaneously by hydrogen bonding. The micelles have a particle size of 12–20 nm and a strong encapsulation ability to increase the CsA concentration tenfold [149]. In addition, Restasis®(CsA), Eysuvis® (loteprednol etabonate), Lacrisek® (vitamin A palmitate and vitamin E), Cyclokat®(CsA) and Artelac Rebalance® (vitamin B12) are also used for the therapy of DED [22, 23].
Ikervis® was introduced in 2015 for the treatment of severe keratitis [340]. Xelpros® can be used to treat glaucoma or ocular hypertension [341]. Verkazia® and Besivance® can be used for vernal keratoconjunctivitis and allergic conjunctivitis/keratitis, respectively [341, 342].
Ozurdex® contains a PLGA polymer matrix that provides long-term release of dexamethasone for up to 6 months. It was approved by the FDA in June 2009 for the treatment of macular edema [343, 344]. Bromsite® [345] and Eysuvis® [346], which were based on Durasite technology and mucus penetrating particle technology respectively, extended the residence time of drugs and improved treatment efficiency.
In addition, as shown in Table 3, many nano-based ocular drug delivery systems are currently in clinical testing stage, which further promote the delivery and development of ophthalmic drugs. Although the approval of nanocarriers has progressed slowly over the past two decades, more nanocarriers, including ocular nanomedicines, are expected to be available on the market in the near future.
To treat cataracts, a recent Phase II clinical trial (NCT03001466) involving in evaluating the therapeutic effect of a urea-loaded nanoparticulate system were conducted. Polymeric nanoparticles composed of Pluronic® F-127 copolymers were used to enhance urea efficacy. In this clinical trial, patients in each group received either urea nanoparticles or balanced salt solution, with one drop of eye solution, five times a day for 8 weeks, and the scores of differences in 6-month visual acuity were measured [347].
INVELTYS are delivered as mucus penetrating particles for the treatment of postoperative inflammation and pain following eye surgery. The primary results of the clinical trial showed that INVELTYS, administered twice daily for 2 weeks, safely and effectively resolved postoperative ocular inflammation and subject-rated ocular pain after cataract surgery. The observed outcomes could be attributed to mucus penetrating particles that enable the drug to penetrate the tear film efficiently, facilitating drug release into targeting tissues [348].
Besides, in a recent Phase II clinical trial (NCT02466399), 80 participants with high IOP and open-angle glaucoma were recruited. The differences in intraocular pressure were measured after 3 months of treatment to compare the efficacy and safety of liposome latanoprost (POLAT-001) and latanoprost eye drops [349].
Recently, a multi-center open-labeled study (NCT02371746) is underway to evaluate the efficacy and safety of ENV 515 (travoprost) for treating ocular hypertension and glaucoma. AR-13503 (NCT03835884) and AR-1105 (NCT03739593) designed using PRINT technology as intravitreal implants for the treating AMD and DR are also in clinical trials [22].
Recent patents on ocular disease therapy
The application and approval of a patent is the final confirmation of the commercial interest in a particular product. In the past years, researchers and pharmaceutical companies have made great progress in develo** ocular drug delivery and have obtained multiple patents. Table 4 lists some representative patents in nano-based ocular drug delivery systems.
To treat cataracts, a patent (CN105726484B) disclosed a composition of tetrandrine liquid crystal nanoparticle eye-drops. The eye-drops were composed of matrix material, stabilizer, penetrating agent and cationic materials etc. Importantly, this invention has the advantages of strong drug loading capacity; good biocompatibility, high biological viscosity, higher stability and the capacity to improve the patient's compliance [ Not applicable. Adeno-associated virus Atomic force microscopy Age-related macular degeneration Amphotericin B Antisense oligonucleotide Anti-VEGF antibodies Blood-aqueous barrier Betamethasone phosphate Bevacizumab Blood-retinal barrier Brimonidine tartrate Ciprofloxacin-loaded nanoemulsion Choroidal neovascularization Cyclosporine A Chitosan oligosaccharide-valylvaline-stearic acid Chitosan-coated polylactide-glycolic acid nanoparticles Dry eye disease Dexamethasone-loaded nanowafer Dendrimer gel hydrogel particles Dynamic light scattering Diabetic retinopathy Dendrimer-triamcinolone acetonide Extracellular vesicle Exosome Food and drug administration Freeze-fracture transmission electron microscopy Fungal keratitis Hyaluronic acid Liposomes coated with hyaluronic acid Hydrogen-castor oil 40/octyl alcohol 40 Homology-directed repair Intraocular pressure Intravitreal injection Melatonin Microemulsions Methylglyoxal Microneedles Moxifloxacin–pamoate Exosomes derived from mesenchymal stromal cells Nanostructured microemulsions system NaMESys carrying sorafenib Copolymer EPC Aflibercept loaded nEPCs Nanoemulsions Non-homologous end joining mechanisms Nanoparticles Nanosuspension Negative staining transmission electron microscopy Oil-in-water Ocular drug delivery systems Polycaprolactone Polydispersion index Polyethylene glycol Polylactic acid Polylactide-coglycolide, Thioketal-containing polyurethane Polyvinyl alcohol Exosomes derived from regulatory Treg cell Reactive oxygen -scavenging hydrogel Redox-responsive quasi-mesoporous magnetic nanospheres Scanning electron microscopy Short hairpin RNA Small interfering RNA Self-nano emulsifying drug delivery systems Self-plug-type microneedle Triamcinolone acetonide Transmission electron microscopy Tocopherol polyethylene glycol 1000 succinate Vascular endothelial growth factor Water-in-oil Zeta potential Ma Y, Bao J, Zhang Y, et al. Mammalian near-infrared image vision through injectable and self-powered retinal nanoantennae. Cell. 2019;177(2):243-255.e15. Gote V, Ansong M, Pal D. Prodrugs and nanomicelles to overcome ocular barriers for drug penetration. Expert Opin Drug Metab Toxicol. 2020;16(10):885–906. Khiev D, Mohamed ZA, Vichare R, et al. Emerging nano-formulations and nanomedicines applications for ocular drug delivery. Nanomaterials (Basel). 2021;11(1):173. Kels BD, Grzybowski A, Grant-Kels JM. Human ocular anatomy. Clin Dermatol. 2015;33(2):140–6. Nayak K, Misra M. Triamcinolone acetonide-loaded PEGylated microemulsion for the posterior segment of eye. ACS Omega. 2020;5(14):7928–39. Urtti A. Challenges and obstacles of ocular pharmacokinetics and drug delivery. Adv Drug Deliv Rev. 2006;58(11):1131–5. Tsai CH, Wang PY, Lin IC, Huang H, Liu GS, Tseng CL. Ocular drug delivery: role of degradable polymeric nanocarriers for ophthalmic application. Int J Mol Sci. 2018;19(9):2830. McCluskey P, Powell RJ. The eye in systemic inflammatory diseases. Lancet. 2004;364(9451):2125–33. Vision impairment and blindness. https://www.who.int/news-room/fact-sheets/detail/blindness-and-visual-impairment Accessed 19 July 2022. Brown L, Leck AK, Gichangi M, Burton MJ, Denning DW. The global incidence and diagnosis of fungal keratitis. Lancet Infect Dis. 2021;21(3):e49–57. Wielders LHP, Schouten JSAG, Winkens B, et al. European multicenter trial of the prevention of cystoid macular edema after cataract surgery in nondiabetics: ESCRS PREMED study report 1. J Cataract Refract Surg. 2018;44(4):429–39. Kang JM, Tanna AP. Glaucoma. Med Clin North Am. 2021;105(3):493–510. Rosenfeld PJ, Brown DM, Heier JS, et al. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med. 2006;355(14):1419–31. Stitt AW, Curtis TM, Chen M, et al. The progress in understanding and treatment of diabetic retinopathy. Prog Retin Eye Res. 2016;51:156–86. Cabrera FJ, Wang DC, Reddy K, Acharya G, Shin CS. Challenges and opportunities for drug delivery to the posterior of the eye. Drug Discov Today. 2019;24(8):1679–84. Jumelle C, Gholizadeh S, Annabi N, Dana R. Advances and limitations of drug delivery systems formulated as eye drops. J Control Release. 2020;321:1–22. Ahmed S, Amin MM, Sayed S. Ocular drug delivery: a comprehensive review. AAPS PharmSciTech. 2023;24(2):66. Al-Kinani AA, Zidan G, Elsaid N, Seyfoddin A, Alani AWG, Alany RG. Ophthalmic gels: past, present and future. Adv Drug Deliv Rev. 2018;126:113–26. Silva B, São Braz B, Delgado E, Gonçalves L. Colloidal nanosystems with mucoadhesive properties designed for ocular topical delivery. Int J Pharm. 2021;606:120873. Gholizadeh S, Wang Z, Chen X, Dana R, Annabi N. Advanced nanodelivery platforms for topical ophthalmic drug delivery. Drug Discov Today. 2021;26(6):1437–49. Akhter MH, Ahmad I, Alshahrani MY, et al. Drug delivery challenges and current progress in nanocarrier-based ocular therapeutic system. Gels. 2022;8(2):82. Gorantla S, Rapalli VK, Waghule T, et al. Nanocarriers for ocular drug delivery: current status and translational opportunity. RSC Adv. 2020;10(46):27835–55. Onugwu AL, Nwagwu CS, Onugwu OS, et al. Nanotechnology based drug delivery systems for the treatment of anterior segment eye diseases. J Control Release. 2023;354:465–88. Kang-Mieler JJ, Rudeen KM, Liu W, Mieler WF. Advances in ocular drug delivery systems. Eye (Lond). 2020;34(8):1371–9. Vaneev A, Tikhomirova V, Chesnokova N, et al. Nanotechnology for topical drug delivery to the anterior segment of the eye. Int J Mol Sci. 2021;22(22):12368. Gupta A, Kafetzis KN, Tagalakis AD, Yu-Wai-Man C. RNA therapeutics in ophthalmology—translation to clinical trials. Exp Eye Res. 2021;205:108482. Adrianto MF, Annuryanti F, Wilson CG, Sheshala R, Thakur RRS. In vitro dissolution testing models of ocular implants for posterior segment drug delivery. Drug Deliv Transl Res. 2022;12(6):1355–75. Kumaran K, Karthika K, Padmapreetha J. Comparative review on conventional and advanced ocular drug delivery formulations. Int J Pharm Pharm Sci. 2010;2(4):1–5. Patel A, Cholkar K, Agrahari V, Mitra AK. Ocular drug delivery systems: an overview. World J Pharmacol. 2013;2(2):47–64. Bravo-Osuna I, Andrés-Guerrero V, Arranz-Romera A, Esteban-Pérez S, Molina-Martínez IT, Herrero-Vanrell R. Microspheres as intraocular therapeutic tools in chronic diseases of the optic nerve and retina. Adv Drug Deliv Rev. 2018;126:127–44. Huang H, Yang XR, Li HL, Lu HS, Oswald J, Liu YM, et al. iRGD decorated liposomes: a novel actively penetrating topical ocular drug delivery strategy. Nano Res. 2020;13(11):3105–9. Morrison PW, Khutoryanskiy VV. Advances in ophthalmic drug delivery. Ther Deliv. 2014;5(12):1297–315. Pflugfelder SC, Stern ME. Biological functions of tear film. Exp Eye Res. 2020;197:108115. Imperiale JC, Acosta GB, Sosnik A. Polymer-based carriers for ophthalmic drug delivery. J Control Release. 2018;285:106–41. Wels M, Roels D, Raemdonck K, De Smedt SC, Sauvage F. Challenges and strategies for the delivery of biologics to the cornea. J Control Release. 2021;333:560–78. Durairaj C. Ocular pharmacokinetics. Handb Exp Pharmacol. 2017;242:31–55. Bachu RD, Chowdhury P, Al-Saedi ZHF, Karla PK, Boddu SHS. Ocular drug delivery barriers-role of nanocarriers in the treatment of anterior segment ocular diseases. Pharmaceutics. 2018;10(1):28. Agrahari V, Mandal A, Agrahari V, et al. A comprehensive insight on ocular pharmacokinetics. Drug Deliv Transl Res. 2016;6(6):735–54. Kim YC, Chiang B, Wu X, Prausnitz MR. Ocular delivery of macromolecules. J Control Release. 2014;190:172–81. Eghrari AO, Riazuddin SA, Gottsch JD. Overview of the cornea: structure, function, and development. Prog Mol Biol Transl Sci. 2015;134:7–23. Gaudana R, Ananthula HK, Parenky A, Mitra AK. Ocular drug delivery. AAPS J. 2010;12(3):348–60. Janagam DR, Wu L, Lowe TL. Nanoparticles for drug delivery to the anterior segment of the eye. Adv Drug Deliv Rev. 2017;122:31–64. Zhang T, **ang CD, Gale D, Carreiro S, Wu EY, Zhang EY. Drug transporter and cytochrome P450 mRNA expression in human ocular barriers: implications for ocular drug disposition. Drug Metab Dispos. 2008;36(7):1300–7. Kölln C, Reichl S. mRNA expression of metabolic enzymes in human cornea, corneal cell lines, and hemicornea constructs. J Ocul Pharmacol Ther. 2012;28(3):271–7. Karla PK, Earla R, Boddu SH, Johnston TP, Pal D, Mitra A. Molecular expression and functional evidence of a drug efflux pump (BCRP) in human corneal epithelial cells. Curr Eye Res. 2009;34(1):1–9. Ahmed S, Amin MM, El-Korany SM, Sayed S. Corneal targeted fenticonazole nitrate-loaded novasomes for the management of ocular candidiasis: Preparation, in vitro characterization, ex vivo and in vivo assessments. Drug Deliv. 2022;29(1):2428–41. Loftsson T, Stefánsson E. Cyclodextrins and topical drug delivery to the anterior and posterior segments of the eye. Int J Pharm. 2017;531(2):413–23. Huang D, Chen YS, Rupenthal ID. Overcoming ocular drug delivery barriers through the use of physical forces. Adv Drug Deliv Rev. 2018;126:96–112. Barar J, Javadzadeh AR, Omidi Y. Ocular novel drug delivery: impacts of membranes and barriers. Expert Opin Drug Deliv. 2008;5(5):567–81. Bock F, Maruyama K, Regenfuss B, et al. Novel anti(lymph)angiogenic treatment strategies for corneal and ocular surface diseases. Prog Retin Eye Res. 2013;34:89–124. Shivhare R, Pathak A, Shrivastava N, Singh C, Tiwari G, Goyal R. An update review on novel advancedocular drug delivery system. World J Pharm Pharm Sci. 2012;1:545–68. Watsky MA, Jablonski MM, Edelhauser HF. Comparison of conjunctival and corneal surface areas in rabbit and human. Curr Eye Res. 1988;7(5):483–6. Ramsay E, Ruponen M, Picardat T, et al. Impact of chemical structure on conjunctival drug permeability: adopting porcine conjunctiva and cassette dosing for construction of in silico model. J Pharm Sci. 2017;106(9):2463–71. Ahmed I, Gokhale RD, Shah MV, Patton TF. Physicochemical determinants of drug diffusion across the conjunctiva, sclera, and cornea. J Pharm Sci. 1987;76(8):583–6. Gote V, Sikder S, Sicotte J, Pal D. Ocular drug delivery: present innovations and future challenges. J Pharmacol Exp Ther. 2019;370(3):602–24. Rada JA, Shelton S, Norton TT. The sclera and myopia. Exp Eye Res. 2006;82(2):185–200. Sun S, Li J, Li X, et al. Episcleral drug film for better-targeted ocular drug delivery and controlled release using multilayered poly-ε-caprolactone (PCL). Acta Biomater. 2016;37:143–54. Mofidfar M, Abdi B, Ahadian S, et al. Drug delivery to the anterior segment of the eye: a review of current and future treatment strategies. Int J Pharm. 2021;607:120924. Coca-Prados M. The blood-aqueous barrier in health and disease. J Glaucoma. 2014;23(8 Suppl 1):S36–8. Dubald M, Bourgeois S, Andrieu V, Fessi H. Ophthalmic drug delivery systems for antibiotherapy-a review. Pharmaceutics. 2018;10(1):10. Singh M, Bharadwaj S, Lee KE, Kang SG. Therapeutic nanoemulsions in ophthalmic drug administration: concept in formulations and characterization techniques for ocular drug delivery. J Control Release. 2020;328:895–916. Tisi A, Feligioni M, Passacantando M, Ciancaglini M, Maccarone R. The impact of oxidative stress on blood-retinal barrier physiology in age-related macular degeneration. Cells. 2021;10(1):64. Díaz-Coránguez M, Ramos C, Antonetti DA. The inner blood-retinal barrier: cellular basis and development. Vision Res. 2017;139:123–37. Duvvuri S, Majumdar S, Mitra AK. Drug delivery to the retina: challenges and opportunities. Expert Opin Biol Ther. 2003;3(1):45–56. Bochot A, Couvreur P, Fattal E. Intravitreal administration of antisense oligonucleotides: potential of liposomal delivery. Prog Retin Eye Res. 2000;19(2):131–47. Ge Y, Zhang A, Sun R, et al. Penetratin-modified lutein nanoemulsion in-situ gel for the treatment of age-related macular degeneration. Expert Opin Drug Deliv. 2020;17(4):603–19. Weinreb RN, Aung T, Medeiros FA. The pathophysiology and treatment of glaucoma: a review. JAMA. 2014;311(18):1901–11. Tham YC, Li X, Wong TY, Quigley HA, Aung T, Cheng CY. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121(11):2081–90. Gagnon MM, Boisjoly HM, Brunette I, Charest M, Amyot M. Corneal endothelial cell density in glaucoma. Cornea. 1997;16(3):314–8. Li X, Zhang Z, Ye L, et al. Acute ocular hypertension disrupts barrier integrity and pump function in rat corneal endothelial cells. Sci Rep. 2017;7(1):6951. Renner M, Stute G, Alzureiqi M, et al. Optic nerve degeneration after retinal ischemia/reperfusion in a rodent model. Front Cell Neurosci. 2017;11:254. Cardigos J, Ferreira Q, Crisóstomo S, et al. Nanotechnology-ocular devices for glaucoma treatment: a literature review. Curr Eye Res. 2019;44(2):111–7. Subrizi A, Del Amo EM, Korzhikov-Vlakh V, Tennikova T, Ruponen M, Urtti A. Design principles of ocular drug delivery systems: importance of drug payload, release rate, and material properties. Drug Discov Today. 2019;24(8):1446–57. Quigley HA. 21st century glaucoma care. Eye (Lond). 2019;33(2):254–60. Wong WL, Su X, Li X, et al. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040: a systematic review and meta-analysis. Lancet Glob Health. 2014;2(2):e106–16. Thomas CJ, Mirza RG, Gill MK. Age-related macular degeneration. Med Clin North Am. 2021;105(3):473–91. Gopinath B, Wong TY. Age-related macular degeneration. Lancet. 2018;392(10153):1147–59. Bakri SJ, Thorne JE, Ho AC, et al. Safety and efficacy of anti-vascular endothelial growth factor therapies for neovascular age-related macular degeneration: a report by the American academy of ophthalmology. Ophthalmology. 2019;126(1):55–63. Ogurtsova K, da Rocha Fernandes JD, Huang Y, et al. IDF Diabetes Atlas: global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Res Clin Pract. 2017;128:40–50. Cheung N, Mitchell P, Wong TY. Diabetic retinopathy. Lancet. 2010;376(9735):124–36. Tan TE, Wong TY. Diabetic retinopathy: Looking forward to 2030. Front Endocrinol (Lausanne). 2023;13:1077669. Ajlan RS, Silva PS, Sun JK. Vascular endothelial growth factor and diabetic retinal disease. Semin Ophthalmol. 2016;31(1–2):40–8. Madjedi K, Pereira A, Ballios BG, et al. Switching between anti-VEGF agents in the management of refractory diabetic macular edema: a systematic review. Surv Ophthalmol. 2022;67(5):1364–72. Liu Y, Wu N. Progress of nanotechnology in diabetic retinopathy treatment. Int J Nanomedicine. 2021;16:1391–403. Pflugfelder SC, de Paiva CS. The pathophysiology of dry eye disease: what we know and future directions for research. Ophthalmology. 2017;124(11S):S4–13. Craig JP, Nichols KK, Akpek EK, et al. TFOS DEWS II definition and classification report. Ocul Surf. 2017;15(3):276–83. Roda M, Corazza I, Bacchi Reggiani ML, et al. dry eye disease and tear cytokine levels-a meta-analysis. Int J Mol Sci. 2020;21(9):3111. Asiedu K, Dzasimatu SK, Kyei S. Impact of dry eye on psychosomatic symptoms and quality of life in a healthy youthful clinical sample. Eye Contact Lens. 2018;44(Suppl 2):S404–9. Na KS, Han K, Park YG, Na C, Joo CK. Depression, stress, quality of life, and dry eye disease in Korean women: a population-based study. Cornea. 2015;34(7):733–8. Perez VL, Stern ME, Pflugfelder SC. Inflammatory basis for dry eye disease flares. Exp Eye Res. 2020;201:108294. Jones L, Downie LE, Korb D, et al. TFOS DEWS II management and therapy report. Ocul Surf. 2017;15(3):575–628. Wang L, Zhou MB, Zhang H. The emerging role of topical ocular drugs to target the posterior eye. Ophthalmol Ther. 2021;10(3):465–94. Yang Y, Lockwood A. Topical ocular drug delivery systems: Innovations for an unmet need. Exp Eye Res. 2022;218:109006. Shen J, Lu GW, Hughes P. Targeted ocular drug delivery with pharmacokinetic/pharmacodynamic considerations. Pharm Res. 2018;35(11):217. Maulvi FA, Shetty KH, Desai DT, Shah DO, Willcox MDP. Recent advances in ophthalmic preparations: ocular barriers, dosage forms and routes of administration. Int J Pharm. 2021;608:121105. Gause S, Hsu KH, Shafor C, Dixon P, Powell KC, Chauhan A. Mechanistic modeling of ophthalmic drug delivery to the anterior chamber by eye drops and contact lenses. Adv Colloid Interface Sci. 2016;233:139–54. Grassiri B, Zambito Y, Bernkop-Schnürch A. Strategies to prolong the residence time of drug delivery systems on ocular surface. Adv Colloid Interface Sci. 2021;288:102342. O’Brien Laramy MN, Nagapudi K. Long-acting ocular drug delivery technologies with clinical precedent. Expert Opin Drug Deliv. 2022;19(10):1285–301. Raghava S, Hammond M, Kompella UB. Periocular routes for retinal drug delivery. Expert Opin Drug Deliv. 2004;1(1):99–114. Le NT, Kroeger ZA, Lin WV, Khanani AM, Weng CY. Novel treatments for diabetic macular edema and proliferative diabetic retinopathy. Curr Diab Rep. 2021;21(10):43. Barocas VH, Balachandran RK. Sustained transscleral drug delivery. Expert Opin Drug Deliv. 2008;5(1):1–10. Chiang B, Jung JH, Prausnitz MR. The suprachoroidal space as a route of administration to the posterior segment of the eye. Adv Drug Deliv Rev. 2018;126:58–66. Nayak K, Misra M. A review on recent drug delivery systems for posterior segment of eye. Biomed Pharmacother. 2018;107:1564–82. Liebmann JM, Barton K, Weinreb RN, et al. Evolving guidelines for intracameral injection. J Glaucoma. 2020;29(Suppl 1):S1–7. Gaballa SA, Kompella UB, Elgarhy O, et al. Corticosteroids in ophthalmology: drug delivery innovations, pharmacology, clinical applications, and future perspectives. Drug Deliv Transl Res. 2021;11(3):866–93. Lane SS, Osher RH, Masket S, Belani S. Evaluation of the safety of prophylactic intracameral moxifloxacin in cataract surgery. J Cataract Refract Surg. 2008;34(9):1451–9. Braga-Mele R, Chang DF, Henderson BA, et al. Intracameral antibiotics: safety, efficacy, and preparation. J Cataract Refract Surg. 2014;40(12):2134–42. Labetoulle M, Findl O, Malecaze F, et al. Evaluation of the efficacy and safety of a standardised intracameral combination of mydriatics and anaesthetics for cataract surgery. Br J Ophthalmol. 2016;100(7):976–85. Behndig A, Cochener B, Güell JL, et al. Endophthalmitis prophylaxis in cataract surgery: overview of current practice patterns in 9 European countries. J Cataract Refract Surg. 2013;39(9):1421–31. Grzybowski A, Brona P, Zeman L, Stewart MW. Commonly used intracameral antibiotics for endophthalmitis prophylaxis: a literature review. Surv Ophthalmol. 2021;66(1):98–108. Keating GM. Intracameral cefuroxime. Drugs. 2013;73(2):179–86. Ho JW, Afshari NA. Advances in cataract surgery: preserving the corneal endothelium. Curr Opin Ophthalmol. 2015;26(1):22–7. Vazirani J, Basu S. Role of topical, subconjunctival, intracameral, and irrigative antibiotics in cataract surgery. Curr Opin Ophthalmol. 2013;24(1):60–5. Del Amo EM, Rimpelä AK, Heikkinen E, et al. Pharmacokinetic aspects of retinal drug delivery. Prog Retin Eye Res. 2017;57:134–85. Jonas JB, Spandau UH, Schlichtenbrede F. Short-term complications of intravitreal injections of triamcinolone and bevacizumab. Eye (Lond). 2008;22(4):590–1. Ilochonwu BC, Urtti A, Hennink WE, Vermonden T. Intravitreal hydrogels for sustained release of therapeutic proteins. J Control Release. 2020;326:419–41. Tang Z, Fan X, Chen Y, Gu P. Ocular Nanomedicine. Adv Sci (Weinh). 2022;9(15):e2003699. Gross A, Cestari DM. Optic neuropathy following retrobulbar injection: a review. Semin Ophthalmol. 2014;29(5–6):434–9. Alhassan MB, Kyari F, Ejere HO. 2015 Peribulbar versus retrobulbar anaesthesia for cataract surgery. Cochrane Database Syst Rev. 2015;7:CD004083. Hayashi K, Hayashi H. Intravitreal versus retrobulbar injections of triamcinolone for macular edema associated with branch retinal vein occlusion. Am J Ophthalmol. 2005;139(6):972–82. Safi M, Ang MJ, Patel P, Silkiss RZ. Rhino-orbital-cerebral mucormycosis (ROCM) and associated cerebritis treated with adjuvant retrobulbar amphotericin B. Am J Ophthalmol Case Rep. 2020;19:100771. Cosgrove R, Rossow T, Cosgrove M, Siegel M. Suspected systemic uptake of chlorpromazine after retrobulbar injection. Am J Ophthalmol Case Rep. 2020;19:100801. Urtti A, Salminen L. Minimizing systemic absorption of topically administered ophthalmic drugs. Surv Ophthalmol. 1993;37(6):435–56. Duncan TE. Side effects of topical ocular timolol. Am J Ophthalmol. 1983;95(4):562–3. Anderson JA. Systemic absorption of topical ocularly applied epinephrine and dipivefrin. Arch Ophthalmol. 1980;98(2):350–3. Inoue K. Managing adverse effects of glaucoma medications. Clin Ophthalmol. 2014;8:903–13. Janoria KG, Gunda S, Boddu SH, Mitra AK. Novel approaches to retinal drug delivery. Expert Opin Drug Deliv. 2007;4(4):371–88. Han H, Li S, Xu M, et al. Polymer- and lipid-based nanocarriers for ocular drug delivery: current status and future perspectives. Adv Drug Deliv Rev. 2023;196:114770. Srinivasarao DA, Lohiya G, Katti DS. Fundamentals, challenges, and nanomedicine-based solutions for ocular diseases. Wiley Interdiscip Rev Nanomed Nanobiotechnol. 2019;11(4):e1548. Grimaudo MA, Pescina S, Padula C, et al. Topical application of polymeric nanomicelles in ophthalmology: a review on research efforts for the noninvasive delivery of ocular therapeutics. Expert Opin Drug Deliv. 2019;16(4):397–413. Vaishya RD, Khurana V, Patel S, Mitra AK. Controlled ocular drug delivery with nanomicelles. Wiley Interdiscip Rev Nanomed Nanobiotechnol. 2014;6(5):422–37. Hu Q, Rijcken CJ, van Gaal E, et al. Tailoring the physicochemical properties of core-crosslinked polymeric micelles for pharmaceutical applications. J Control Release. 2016;244(Pt B):314–25. Bourzac K. Nanotechnology: carrying drugs. Nature. 2012;491(7425):S58–60. Trivedi R, Kompella UB. Nanomicellar formulations for sustained drug delivery: strategies and underlying principles. Nanomedicine (Lond). 2010;5(3):485–505. Torchilin VP. Structure and design of polymeric surfactant-based drug delivery systems. J Control Release. 2001;73(2–3):137–72. Rangel-Yagui CO, Pessoa A Jr, Tavares LC. Micellar solubilization of drugs. J Pharm Pharm Sci. 2005;8(2):147–65. Wang Y, Jiang L, Shen Q, Shen J, Han Y, Zhang H. Investigation on the self-assembled behaviors of C18 unsaturated fatty acids in arginine aqueous solution. RSC Adv. 2017;7(66):41561–72. Fameau AL, Arnould A, Lehmann M, von Klitzing R. Photoresponsive self-assemblies based on fatty acids. Chem Commun. 2015;51(14):2907–10. Ghezzi M, Pescina S, Delledonne A, et al. Improvement of imiquimod solubilization and skin retention via TPGS micelles: exploiting the co-solubilizing effect of oleic acid. Pharmaceutics. 2021;13(9):1476. Tampucci S, Guazzelli L, Burgalassi S, et al. pH-responsive nanostructures based on surface active fatty acid-protic ionic liquids for imiquimod delivery in skin cancer topical therapy. Pharmaceutics. 2020;12(11):1078. Ghezzi M, Ferraboschi I, Delledonne A, et al. Cyclosporine-loaded micelles for ocular delivery: investigating the penetration mechanisms. J Control Release. 2022;349:744–55. Xu X, Sun L, Zhou L, Cheng Y, Cao F. Functional chitosan oligosaccharide nanomicelles for topical ocular drug delivery of dexamethasone. Carbohydr Polym. 2020;227:115356. Zhao X, Seah I, Xue K, et al. Antiangiogenic nanomicelles for the topical delivery of aflibercept to treat retinal neovascular disease. Adv Mater. 2022;34(25):e2108360. Peng C, Kuang L, Zhao J, Ross AE, Wang Z, Ciolino JB. Bibliometric and visualized analysis of ocular drug delivery from 2001 to 2020. J Control Release. 2022;345:625–45. Xu J, Zheng S, Hu X, et al. Advances in the research of bioinks based on natural collagen, polysaccharide and their derivatives for skin 3D bioprinting. Polymers (Basel). 2020;12(6):1237. Akhter S, Anwar M, Siddiqui MA, et al. Improving the topical ocular pharmacokinetics of an immunosuppressant agent with mucoadhesive nanoemulsions: formulation development, in-vitro and in-vivo studies. Colloids Surf B Biointerfaces. 2016;148:19–29. Yetisgin AA, Cetinel S, Zuvin M, Kosar A, Kutlu O. Therapeutic nanoparticles and their targeted delivery applications. Molecules. 2020;25(9):2193. Sánchez-López E, Espina M, Doktorovova S, Souto EB, García ML. Lipid nanoparticles (SLN, NLC): overcoming the anatomical and physiological barriers of the eye—Part I—Barriers and determining factors in ocular delivery. Eur J Pharm Biopharm. 2017;110:70–5. Meng T, Kulkarni V, Simmers R, Brar V, Xu Q. Therapeutic implications of nanomedicine for ocular drug delivery. Drug Discov Today. 2019;24(8):1524–38. Jiang C, Cano-Vega MA, Yue F, et al. Dibenzazepine-loaded nanoparticles induce local browning of white adipose tissue to counteract obesity. Mol Ther. 2022;30(1):502. Jiang C, Kuang L, Merkel MP, et al. Biodegradable polymeric microsphere-based drug delivery for inductive browning of fat. Front Endocrinol (Lausanne). 2015;6:169. Pandit J, Sultana Y, Aqil M. Chitosan coated nanoparticles for efficient delivery of bevacizumab in the posterior ocular tissues via subconjunctival administration. Carbohydr Polym. 2021;267:118217. Kim SN, Min CH, Kim YK, et al. Iontophoretic ocular delivery of latanoprost-loaded nanoparticles via skin-attached electrodes. Acta Biomater. 2022;144:32–41. Nguyen DD, Luo LJ, Lai JY. Effects of shell thickness of hollow poly(lactic acid) nanoparticles on sustained drug delivery for pharmacological treatment of glaucoma. Acta Biomater. 2020;111:302–15. Schnichels S, Hurst J, de Vries JW, et al. Improved treatment options for glaucoma with brimonidine-loaded lipid DNA nanoparticles. ACS Appl Mater Interfaces. 2021;13(8):9445–56. Chen Liangbo, Feng Wu, Pang Yan, Yan Dan, Zhang Siyi, Chen Fangjie, Nianxuan Wu, Gong Danni, Liu **yao, Yao Fu, Fan **anqun. Therapeutic nanocoating of ocular surface. Nano Today. 2021;41:101309. Li M, Xu Z, Zhang L, et al. Targeted noninvasive treatment of choroidal neovascularization by hybrid cell-membrane-cloaked biomimetic nanoparticles. ACS Nano. 2021;15(6):9808–19. Peltonen L, Hirvonen J. Drug nanocrystals—versatile option for formulation of poorly soluble materials. Int J Pharm. 2018;537(1–2):73–83. Al-Kassas R, Bansal M, Shaw J. Nanosizing techniques for improving bioavailability of drugs. J Control Release. 2017;260:202–12. Zhang J, Jiao J, Niu M, et al. Ten years of knowledge of nano-carrier based drug delivery systems in ophthalmology: current evidence, challenges, and future prospective. Int J Nanomed. 2021;16:6497–530. Tai L, Liu C, Jiang K, et al. A novel penetratin-modified complex for noninvasive intraocular delivery of antisense oligonucleotides. Int J Pharm. 2017;529(1–2):347–56. Josyula A, Omiadze R, Parikh K, et al. An ion-paired moxifloxacin nanosuspension eye drop provides improved prevention and treatment of ocular infection. Bioeng Transl Med. 2021;6(3):e10238. García-Millán E, Quintáns-Carballo M, Otero-Espinar FJ. Improved release of triamcinolone acetonide from medicated soft contact lenses loaded with drug nanosuspensions. Int J Pharm. 2017;525(1):226–36. Yan R, Xu L, Wang Q, Wu Z, Zhang H, Gan L. Cyclosporine A nanosuspensions for ophthalmic delivery: a comparative study between cationic nanoparticles and drug-core mucus penetrating nanoparticles. Mol Pharm. 2021;18(12):4290–8. Wu Y, Vora LK, Mishra D, et al. Nanosuspension-loaded dissolving bilayer microneedles for hydrophobic drug delivery to the posterior segment of the eye. Biomater Adv. 2022;137:212767. Jacob S, Nair AB, Shah J. Emerging role of nanosuspensions in drug delivery systems. Biomater Res. 2020;24:3. Rimple, Newton MJ. Impact of ocular compatible lipoids and castor oil in fabrication of brimonidine tartrate nanoemulsions by 33 full factorial design. Recent Pat Inflamm Allergy Drug Discov. 2018;12(2):169–83. Qamar Z, Qizilbash FF, Iqubal MK, et al. Nano-based drug delivery system: recent strategies for the treatment of ocular disease and future perspective. Recent Pat Drug Deliv Formul. 2019;13(4):246–54. Singh Y, Meher JG, Raval K, et al. Nanoemulsion: concepts, development and applications in drug delivery. J Control Release. 2017;252:28–49. Lallemand F, Daull P, Benita S, Buggage R, Garrigue JS. Successfully improving ocular drug delivery using the cationic nanoemulsion, novasorb. J Drug Deliv. 2012;2012:604204. Gupta A, Eral HB, Hatton TA, Doyle PS. Nanoemulsions: formation, properties and applications. Soft Matter. 2016;12(11):2826–41. Daull P, Lallemand F, Garrigue JS. Benefits of cetalkonium chloride cationic oil-in-water nanoemulsions for topical ophthalmic drug delivery. J Pharm Pharmacol. 2014;66(4):531–41. Ammar HO, Salama HA, Ghorab M, Mahmoud AA. Nanoemulsion as a potential ophthalmic delivery system for dorzolamide hydrochloride. AAPS PharmSciTech. 2009;10(3):808–19. Jurišić Dukovski B, Juretić M, Bračko D, et al. Functional ibuprofen-loaded cationic nanoemulsion: development and optimization for dry eye disease treatment. Int J Pharm. 2020;576:118979. Tayel SA, El-Nabarawi MA, Tadros MI, Abd-Elsalam WH. Promising ion-sensitive in situ ocular nanoemulsion gels of terbinafine hydrochloride: design, in vitro characterization and in vivo estimation of the ocular irritation and drug pharmacokinetics in the aqueous humor of rabbits. Int J Pharm. 2013;443(1–2):293–305. Mahboobian MM, Mohammadi M, Mansouri Z. Development of thermosensitive in situ gel nanoemulsions for ocular delivery of acyclovir. J Drug Deliv Sci Technol. 2020;55:101400. Bhalerao H, Koteshwara KB, Chandran S. Design, optimisation and evaluation of in situ gelling nanoemulsion formulations of brinzolamide. Drug Deliv Transl Res. 2020;10(2):529–47. Youssef AAA, Cai C, Dudhipala N, Majumdar S. Design of topical ocular ciprofloxacin nanoemulsion for the management of bacterial keratitis. Pharmaceuticals (Basel). 2021;14(3):210. Ismail A, Nasr M, Sammour O. Nanoemulsion as a feasible and biocompatible carrier for ocular delivery of travoprost: improved pharmacokinetic/pharmacodynamic properties. Int J Pharm. 2020;583:119402. Üstündag-Okur N, Gökçe EH, Eğrilmez S, Özer Ö, Ertan G. Novel ofloxacin-loaded microemulsion formulations for ocular delivery. J Ocul Pharmacol Ther. 2014;30(4):319–32. Kale SN, Deore SL. Emulsion micro emulsion and nano emulsion: a review. Syst Rev Pharm. 2016;8:39–47. Cunha Júnior AdS, Fialho SL, Carneiro LB, Oréfice F. Microemulsions as drug delivery systems for topical ocular administration. Arquivos Brasileiros de Oftalmologia. 2003;66:385–91. Üstündağ Okur N, Er S, Çağlar E, Ekmen T, Sala F. Formulation of microemulsions for dermal delivery of Cephalexin. Acta Pharm Sci. 2017;55(4):27. Mahran A, Ismail S, Allam AA. Development of triamcinolone acetonide-loaded microemulsion as a prospective ophthalmic delivery system for treatment of uveitis: in vitro and in vivo evaluation. Pharmaceutics. 2021;13(4):444. Santonocito M, Zappulla C, Viola S, et al. Assessment of a new nanostructured microemulsion system for ocular delivery of sorafenib to posterior segment of the eye. Int J Mol Sci. 2021;22(9):4404. Rupenthal ID, Agarwal P, Uy B, et al. Preparation and characterisation of a cyclodextrin-complexed mānuka honey microemulsion for eyelid application. Pharmaceutics. 2022;14(7):1493. Deepak Amar, Goyal AK, Rath G. Nanofiber in transmucosal drug delivery. J Drug Deliv Sci Technol. 2018;43(2017):379–87. Razavi MS, Ebrahimnejad P, Fatahi Y, D’Emanuele A, Dinarvand R. Recent developments of nanostructures for the ocular delivery of natural compounds. Front Chem. 2022;10:850757. Hu X, Liu S, Zhou G, Huang Y, **e Z, **g X. Electrospinning of polymeric nanofibers for drug delivery applications. J Control Release. 2014;185:12–21. Zupančič Š, Sinha-Ray S, Sinha-Ray S, Kristl J, Yarin AL. Long-term sustained ciprofloxacin release from pmma and hydrophilic polymer blended nanofibers. Mol Pharm. 2016;13(1):295–305. Goyal R, Macri LK, Kaplan HM, Kohn J. Nanoparticles and nanofibers for topical drug delivery. J Control Release. 2016;240:77–92. Da Silva GR, Lima TH, Fernandes-Cunha GM, et al. Ocular biocompatibility of dexamethasone acetate loaded poly(ɛ-caprolactone) nanofibers. Eur J Pharm Biopharm. 2019;142:20–30. Carracedo-Rodríguez G, Martínez-Águila A, Rodriguez-Pomar C, Bodas-Romero J, Sanchez-Naves J, Pintor J. Effect of nutritional supplement based on melatonin on the intraocular pressure in normotensive subjects. Int Ophthalmol. 2020;40(2):419–22. Ferreira de Melo IM, Martins Ferreira CG, da Silva Lima, Souza EH, et al. Melatonin regulates the expression of inflammatory cytokines, VEGF and apoptosis in diabetic retinopathy in rats. Chem Biol Interact. 2020;327:109183. Harpsøe NG, Andersen LP, Gögenur I, Rosenberg J. Clinical pharmacokinetics of melatonin: a systematic review. Eur J Clin Pharmacol. 2015;71(8):901–9. Andersen LP, Werner MU, Rosenkilde MM, et al. Pharmacokinetics of oral and intravenous melatonin in healthy volunteers. BMC Pharmacol Toxicol. 2016;17:8. Romeo A, Kazsoki A, Omer S, et al. Formulation and characterization of electrospun nanofibers for melatonin ocular delivery. Pharmaceutics. 2023;15(4):1296. Rohde F, Walther M, Wächter J, Knetzger N, Lotz C, Windbergs M. In-situ tear fluid dissolving nanofibers enable prolonged viscosity-enhanced dual drug delivery to the eye. Int J Pharm. 2022;616:121513. Tawfik EA, Alshamsan A, Abul Kalam M, et al. In vitro and in vivo biological assessment of dual drug-loaded coaxial nanofibers for the treatment of corneal abrasion. Int J Pharm. 2021;604:120732. Esentürk I, Erdal MS, Güngör S. Electrospinning method to produce drug-loaded nanofibers for topical/transdermal drug delivery applications. J Fac Pharm Istanb Univ. 2016;46:49–64. Farokhi M, Mottaghitalab F, Reis RL, Ramakrishna S, Kundu SC. Functionalized silk fibroin nanofibers as drug carriers: advantages and challenges. J Control Release. 2020;321:324–47. Sridhar R, Lakshminarayanan R, Madhaiyan K, Amutha Barathi V, Lim KH, Ramakrishna S. Electrosprayed nanoparticles and electrospun nanofibers based on natural materials: applications in tissue regeneration, drug delivery and pharmaceuticals. Chem Soc Rev. 2015;44(3):790–814. Yaylaci S, Dinç E, Aydın B, Tekinay AB, Guler MO. Peptide nanofiber system for sustained delivery of anti-vegf proteins to the eye vitreous. Pharmaceutics. 2023;15(4):1264. Shi X, Zhou T, Huang S, et al. An electrospun scaffold functionalized with a ROS-scavenging hydrogel stimulates ocular wound healing. Acta Biomater. 2023;158:266–80. Wei S, Yin R, Tang T, et al. Gas-permeable, irritation-free, transparent hydrogel contact lens devices with metal-coated nanofiber mesh for eye interfacing. ACS Nano. 2019;13(7):7920–9. Abbasi E, Aval SF, Akbarzadeh A, et al. Dendrimers: synthesis, applications, and properties. Nanoscale Res Lett. 2014;9(1):247. Kambhampati SP, Kannan RM. Dendrimer nanoparticles for ocular drug delivery. J Ocul Pharmacol Ther. 2013;29(2):151–65. Spataro G, Malecaze F, Turrin CO, et al. Designing dendrimers for ocular drug delivery. Eur J Med Chem. 2010;45(1):326–34. Shaikh A, Kesharwani P, Gajbhiye V. Dendrimer as a momentous tool in tissue engineering and regenerative medicine. J Control Release. 2022;346:328–54. Romanowski EG, Yates KA, Paull JRA, Heery GP, Shanks RMQ. Topical astodrimer sodium, a non-toxic polyanionic dendrimer, demonstrates antiviral activity in an experimental ocular adenovirus infection model. Molecules. 2021;26(11):3419. Kambhampati SP, Bhutto IA, Wu T, et al. Systemic dendrimer nanotherapies for targeted suppression of choroidal inflammation and neovascularization in age-related macular degeneration. J Control Release. 2021;335:527–40. Wang J, Li B, Huang D, et al. Nano-in-nano dendrimer gel particles for efficient topical delivery of antiglaucoma drugs into the eye. Chem Eng J. 2021;425:130498. Ge X, Wei M, He S, Yuan WE. Advances of non-ionic surfactant vesicles (niosomes) and their application in drug delivery. Pharmaceutics. 2019;11(2):55. Keam SJ, Scott LJ, Curran MP. Verteporfin: a review of its use in the management of subfoveal choroidal neovascularisation. Drugs. 2003;63(22):2521–54. Tavakoli S, Peynshaert K, Lajunen T, et al. Ocular barriers to retinal delivery of intravitreal liposomes: impact of vitreoretinal interface. J Control Release. 2020;328:952–61. Kaur IP, Garg A, Singla AK, Aggarwal D. Vesicular systems in ocular drug delivery: an overview. Int J Pharm. 2004;269(1):1–14. Lajunen T, Nurmi R, Kontturi L, et al. Light activated liposomes: functionality and prospects in ocular drug delivery. J Control Release. 2016;244(Pt B):157–66. Chen X, Wu J, Lin X, et al. Tacrolimus loaded cationic liposomes for dry eye treatment. Front Pharmacol. 2022;13:838168. Sahoo SK, Dilnawaz F, Krishnakumar S. Nanotechnology in ocular drug delivery. Drug Discov Today. 2008;13(3–4):144–51. Chen S, Hanning S, Falconer J, Locke M, Wen J. Recent advances in non-ionic surfactant vesicles (niosomes): Fabrication, characterization, pharmaceutical and cosmetic applications. Eur J Pharm Biopharm. 2019;144:18–39. Gan L, Wang J, Jiang M, et al. Recent advances in topical ophthalmic drug delivery with lipid-based nanocarriers. Drug Discov Today. 2013;18(5–6):290–7. Verma A, Tiwari A, Saraf S, Panda PK, Jain A, Jain SK. Emerging potential of niosomes in ocular delivery. Expert Opin Drug Deliv. 2021;18(1):55–71. Farha AK, Gan RY, Li HB, et al. The anticancer potential of the dietary polyphenol rutin: current status, challenges, and perspectives. Crit Rev Food Sci Nutr. 2022;62(3):832–59. Wichayapreechar P, Anuchapreeda S, Phongpradist R, Rungseevijitprapa W, Ampasavate C. Dermal targeting of Centella asiatica extract using hyaluronic acid surface modified niosomes. J Liposome Res. 2020;30(2):197–207. Kattar A, Quelle-Regaldie A, Sánchez L, Concheiro A, Alvarez-Lorenzo C. Formulation and characterization of epalrestat-loaded polysorbate 60 cationic niosomes for ocular delivery. Pharmaceutics. 2023;15(4):1247. Allam A, Elsabahy M, El Badry M, Eleraky NE. Betaxolol-loaded niosomes integrated within pH-sensitive in situ forming gel for management of glaucoma. Int J Pharm. 2021;598:120380. Fathalla D, Fouad EA, Soliman GM. Latanoprost niosomes as a sustained release ocular delivery system for the management of glaucoma. Drug Dev Ind Pharm. 2020;46(5):806–13. Coursey TG, Henriksson JT, Marcano DC, et al. Dexamethasone nanowafer as an effective therapy for dry eye disease. J Control Release. 2015;213:168–74. Marcano DC, Shin CS, Lee B, et al. Synergistic cysteamine delivery nanowafer as an efficacious treatment modality for corneal cystinosis. Mol Pharm. 2016;13(10):3468–77. Yuan X, Marcano DC, Shin CS, et al. Ocular drug delivery nanowafer with enhanced therapeutic efficacy. ACS Nano. 2015;9(2):1749–58. Dourado LFN, da Silva CN, Gonçalves RS, et al. Improvement of PnPP-19 peptide bioavailability for glaucoma therapy: design and application of nanowafers based on PVA. J Drug Deliv Sci Technol. 2022;74:103501. Rykowska I, Nowak I, Nowak R. Soft contact lenses as drug delivery systems: a review. Molecules. 2021;26(18):5577. Peral A, Martinez-Aguila A, Pastrana C, Huete-Toral F, Carpena-Torres C, Carracedo G. Contact lenses as drug delivery system for glaucoma: a review. Appl Sci. 2020;10(15):5151. Filipe HP, Henriques J, Reis P, Silva PC, Quadrado MJ, Serro AP. Contact lenses as drug controlled release systems: a narrative review. Rev Bras Oftalmol. 2016;75:241–7. Choi SW, Kim J. Therapeutic contact lenses with polymeric vehicles for ocular drug delivery: a review. Materials (Basel). 2018;11(7):1125. Hsu KH, Carbia BE, Plummer C, Chauhan A. Dual drug delivery from vitamin E loaded contact lenses for glaucoma therapy. Eur J Pharm Biopharm. 2015;94:312–21. Soeken TA, Ross AE, Kohane DS, et al. Dexamethasone-eluting contact lens for the prevention of postphotorefractive keratectomy scar in a New Zealand white rabbit model. Cornea. 2021;40(9):1175–80. Maulvi FA, Soni TG, Shah DO. A review on therapeutic contact lenses for ocular drug delivery. Drug Deliv. 2016;23(8):3017–26. Shayani Rad M, Sabeti Z, Mohajeri SA, Fazly Bazzaz BS. Preparation, characterization, and evaluation of zinc oxide nanoparticles suspension as an antimicrobial media for daily use soft contact lenses. Curr Eye Res. 2020;45(8):931–9. Bin Sahadan MY, Tong WY, Tan WN, et al. Phomopsidione nanoparticles coated contact lenses reduce microbial keratitis causing pathogens. Exp Eye Res. 2019;178:10–4. Jiao Z, Huo Q, Lin X, et al. Drug-free contact lens based on quaternized chitosan and tannic acid for bacterial keratitis therapy and corneal repair. Carbohydr Polym. 2022;286:119314. Ding X, Ben-Shlomo G, Que L. Soft contact lens with embedded microtubes for sustained and self-adaptive drug delivery for glaucoma treatment. ACS Appl Mater Interfaces. 2020;12(41):45789–95. Cooper RC, Yang H. Hydrogel-based ocular drug delivery systems: emerging fabrication strategies, applications, and bench-to-bedside manufacturing considerations. J Control Release. 2019;306:29–39. Irimia T, Dinu-Pîrvu CE, Ghica MV, et al. Chitosan-based in situ gels for ocular delivery of therapeutics: a state-of-the-art review. Mar Drugs. 2018;16(10):373. Sacco P, Furlani F, De Marzo G, Marsich E, Paoletti S, Donati I. Concepts for develo** physical gels of chitosan and of chitosan derivatives. Gels. 2018;4(3):67. Zhang Z, Ai S, Yang Z, Li X. Peptide-based supramolecular hydrogels for local drug delivery. Adv Drug Deliv Rev. 2021;174:482–503. Arranz-Romera A, Esteban-Pérez S, Garcia-Herranz D, Aragón-Navas A, Bravo-Osuna I, Herrero-Vanrell R. Combination therapy and co-delivery strategies to optimize treatment of posterior segment neurodegenerative diseases. Drug Discov Today. 2019;24(8):1644–53. Lin S, Ge C, Wang D, et al. Overcoming the anatomical and physiological barriers in topical eye surface medication using a peptide-decorated polymeric micelle. ACS Appl Mater Interfaces. 2019;11(43):39603–12. Fang G, Wang Q, Yang X, Qian Y, Zhang G, Tang B. γ-Cyclodextrin-based polypseudorotaxane hydrogels for ophthalmic delivery of flurbiprofen to treat anterior uveitis. Carbohydr Polym. 2022;277:118889. Jung JH, Kim SS, Chung H, Hejri A, Prausnitz MR. Six-month sustained delivery of anti-VEGF from in-situ forming hydrogel in the suprachoroidal space. J Control Release. 2022;352:472–84. Gao H, Chen M, Liu Y, et al. Injectable anti-inflammatory supramolecular nanofiber hydrogel to promote anti-VEGF therapy in age-related macular degeneration treatment. Adv Mater. 2023;35(2):e2204994. Lee K, Goudie MJ, Tebon P, et al. Non-transdermal microneedles for advanced drug delivery. Adv Drug Deliv Rev. 2020;165–166:41–59. Zhu J, Zhou X, Kim HJ, et al. Gelatin methacryloyl microneedle patches for minimally invasive extraction of skin interstitial fluid. Small. 2020;16(16):e1905910. Jiang J, Moore JS, Edelhauser HF, Prausnitz MR. Intrascleral drug delivery to the eye using hollow microneedles. Pharm Res. 2009;26(2):395–403. Gupta P, Yadav KS. Applications of microneedles in delivering drugs for various ocular diseases. Life Sci. 2019;237:116907. Shi H, Zhou J, Wang Y, et al. A rapid corneal healing microneedle for efficient ocular drug delivery. Small. 2022;18(4):e2104657. Cui M, Zheng M, Wiraja C, et al. Ocular delivery of predatory bacteria with cryomicroneedles against eye infection. Adv Sci (Weinh). 2021;8(21):e2102327. Lee K, Park S, Jo DH, et al. Self-plugging microneedle (SPM) for intravitreal drug delivery. Adv Healthc Mater. 2022;11(12):e2102599. Tawfik M, Chen F, Goldberg JL, Sabel BA. Nanomedicine and drug delivery to the retina: current status and implications for gene therapy. Naunyn Schmiedebergs Arch Pharmacol. 2022;395(12):1477–507. Musarella MA. Gene map** of ocular diseases. Surv Ophthalmol. 1992;36(4):285–312. Cheng KJ, Hsieh CM, Nepali K, Liou JP. Ocular disease therapeutics: design and delivery of drugs for diseases of the eye. J Med Chem. 2020;63(19):10533–93. Mendell JR, Al-Zaidy SA, Rodino-Klapac LR, et al. Current clinical applications of in vivo gene therapy with AAVs. Mol Ther. 2021;29(2):464–88. Dunbar CE, High KA, Joung JK, Kohn DB, Ozawa K, Sadelain M. Gene therapy comes of age. Science. 2018;359(6372):eaan4672. Amador C, Shah R, Ghiam S, Kramerov AA, Ljubimov AV. Gene therapy in the anterior eye segment. Curr Gene Ther. 2022;22(2):104–31. Ren W, Duan S, Dai C, **e C, Jiang L, Shi Y. Nanotechnology lighting the way for gene therapy in ophthalmopathy: from opportunities toward applications. Molecules. 2023;28(8):3500. Colella P, Cotugno G, Auricchio A. Ocular gene therapy: current progress and future prospects. Trends Mol Med. 2009;15(1):23–31. Naso MF, Tomkowicz B, Perry WL 3rd, Strohl WR. Adeno-associated virus (AAV) as a vector for gene therapy. BioDrugs. 2017;31(4):317–34. Bastola P, Song L, Gilger BC, Hirsch ML. Adeno-associated virus mediated gene therapy for corneal diseases. Pharmaceutics. 2020;12(8):767. Tarallo V, Bogdanovich S, Hirano Y, et al. Inhibition of choroidal and corneal pathologic neovascularization by Plgf1-de gene transfer. Invest Ophthalmol Vis Sci. 2012;53(13):7989–96. Lu Y, Tai PWL, Ai J, et al. Transcriptome profiling of neovascularized corneas reveals miR-204 as a multi-target biotherapy deliverable by rAAVs. Mol Ther Nucleic Acids. 2018;10:349–60. Kaemmerer WF. How will the field of gene therapy survive its success? Bioeng Transl Med. 2018;3(2):166–77. Jiang J, Zhang X, Tang Y, Li S, Chen J. Progress on ocular siRNA gene-silencing therapy and drug delivery systems. Fundam Clin Pharmacol. 2021;35(1):4–24. Del Amo EM, Urtti A. Current and future ophthalmic drug delivery systems. A shift to the posterior segment. Drug Discov Today. 2008;13(3–4):135–43. Ma Y, Lin H, Wang P, et al. A miRNA-based gene therapy nanodrug synergistically enhances pro-inflammatory antitumor immunity against melanoma. Acta Biomater. 2023;155:538–53. Ribeiro MCS, de Miranda MC, Cunha PDS, et al. Neuroprotective effect of siRNA entrapped in hyaluronic acid-coated lipoplexes by intravitreal administration. Pharmaceutics. 2021;13(6):845. Kumar S, Fry LE, Wang JH, et al. RNA-targeting strategies as a platform for ocular gene therapy. Prog Retin Eye Res. 2023;92:101110. Russell SR, Drack AV, Cideciyan AV, et al. Intravitreal antisense oligonucleotide sepofarsen in Leber congenital amaurosis type 10: a phase 1b/2 trial. Nat Med. 2022;28(5):1014–21. Supe S, Upadhya A, Singh K. Role of small interfering RNA (siRNA) in targeting ocular neovascularization: a review. Exp Eye Res. 2021;202:108329. Wang J, Zhao P, Chen Z, Wang H, Wang Y, Lin Q. Non-viral gene therapy using RNA interference with PDGFR-α mediated epithelial-mesenchymal transformation for proliferative vitreoretinopathy. Mater Today Bio. 2023;20:100632. Dhurandhar D, Sahoo NK, Mariappan I, Narayanan R. Gene therapy in retinal diseases: a review. Indian J Ophthalmol. 2021;69(9):2257–65. Sander JD, Joung JK. CRISPR-Cas systems for editing, regulating and targeting genomes. Nat Biotechnol. 2014;32:347–55. Guo N, Liu JB, Li W, Ma YS, Fu D. The power and the promise of CRISPR/Cas9 genome editing for clinical application with gene therapy. J Adv Res. 2022;40:135–52. Gumerson JD, Alsufyani A, Yu W, et al. Restoration of RPGR expression in vivo using CRISPR/Cas9 gene editing. Gene Ther. 2022;29(1–2):81–93. Chung SH, Sin TN, Dang B, et al. CRISPR-based VEGF suppression using paired guide RNAs for treatment of choroidal neovascularization. Mol Ther Nucleic Acids. 2022;28:613–22. Banskota S, Raguram A, Suh S, et al. Engineered virus-like particles for efficient in vivo delivery of therapeutic proteins. Cell. 2022;185(2):250-265.e16. Manukonda R, Attem J, Yenuganti VR, Kaliki S, Vemuganti GK. Exosomes in the visual system: new avenues in ocular diseases. Tumour Biol. 2022;44(1):129–52. Gurung S, Perocheau D, Touramanidou L, Baruteau J. The exosome journey: from biogenesis to uptake and intracellular signalling. Cell Commun Signal. 2021;19(1):47. Feng X, Peng Z, Yuan L, et al. Research progress of exosomes in pathogenesis, diagnosis, and treatment of ocular diseases. Front Bioeng Biotechnol. 2023;11:1100310. Wortzel I, Dror S, Kenific CM, Lyden D. Exosome-mediated metastasis: communication from a distance. Dev Cell. 2019;49(3):347–60. Kalluri R, LeBleu VS. The biology, function, and biomedical applications of exosomes. Science. 2020;367(6478):eaau6977. Dong X, Lei Y, Yu Z, et al. Exosome-mediated delivery of an anti-angiogenic peptide inhibits pathological retinal angiogenesis. Theranostics. 2021;11(11):5107–26. Tian Y, Zhang F, Qiu Y, et al. Reduction of choroidal neovascularization via cleavable VEGF antibodies conjugated to exosomes derived from regulatory T cells. Nat Biomed Eng. 2021;5(9):968–82. Zhou T, He C, Lai P, et al. miR-204-containing exosomes ameliorate GVHD-associated dry eye disease. Sci Adv. 2022;8(2):eabj9617. Herrmann IK, Wood MJA, Fuhrmann G. Extracellular vesicles as a next-generation drug delivery platform. Nat Nanotechnol. 2021;16(7):748–59. Piffoux M, Silva AKA, Wilhelm C, Gazeau F, Tareste D. Modification of extracellular vesicles by fusion with liposomes for the design of personalized biogenic drug delivery systems. ACS Nano. 2018;12(7):6830–42. Kojima R, Bojar D, Rizzi G, et al. Designer exosomes produced by implanted cells intracerebrally deliver therapeutic cargo for Parkinson’s disease treatment. Nat Commun. 2018;9(1):1305. Siqueira Jørgensen SD, Al Sawaf M, Graeser K, Mu H, Müllertz A, Rades T. The ability of two in vitro lipolysis models reflecting the human and rat gastro-intestinal conditions to predict the in vivo performance of SNEDDS dosing regimens. Eur J Pharm Biopharm. 2018;124:116–24. Pouton CW. Lipid formulations for oral administration of drugs: non-emulsifying, self-emulsifying and “self-microemulsifying” drug delivery systems. Eur J Pharm Sci. 2000;11(Suppl 2):S93–8. Ujhelyi Z, Vecsernyés M, Fehér P, et al. Physico-chemical characterization of self-emulsifying drug delivery systems. Drug Discov Today Technol. 2018;27:81–6. Li Z, Xu D, Yuan Y, et al. Advances of spontaneous emulsification and its important applications in enhanced oil recovery process. Adv Colloid Interface Sci. 2020;277:102119. Buya AB, Beloqui A, Memvanga PB, Préat V. Self-Nano-emulsifying drug-delivery systems: from the development to the current applications and challenges in oral drug delivery. Pharmaceutics. 2020;12(12):1194. López-Cano JJ, González-Cela-Casamayor MA, Andrés-Guerrero V, et al. Development of an osmoprotective microemulsion as a therapeutic platform for ocular surface protection. Int J Pharm. 2022;623:121948. Kontogiannidou E, Meikopoulos T, Gika H, et al. In vitro evaluation of self-nano-emulsifying drug delivery systems (SNEDDS) containing room temperature ionic liquids (RTILs) for the oral delivery of amphotericin B. Pharmaceutics. 2020;12(8):699. Whitesides GM. Nanoscience, nanotechnology, and chemistry. Small. 2005;1(2):172–9. Zhang T, Wei C, Wu X, et al. Characterization and evaluation of rapamycin-loaded nano-micelle ophthalmic solution. J Funct Biomater. 2023;14(1):49. Barenholz Y. Doxil®–the first FDA-approved nano-drug: lessons learned. J Control Release. 2012;160(2):117–34. Lai SK, Wang YY, Hanes J. Mucus-penetrating nanoparticles for drug and gene delivery to mucosal tissues. Adv Drug Deliv Rev. 2009;61(2):158–71. Toropainen E, Fraser-Miller SJ, Novakovic D, et al. Biopharmaceutics of topical ophthalmic suspensions: importance of viscosity and particle size in ocular absorption of indomethacin. Pharmaceutics. 2021;13(4):452. Younes NF, Abdel-Halim SA, Elassasy AI. Corneal targeted Sertaconazole nitrate loaded cubosomes: Preparation, statistical optimization, in vitro characterization, ex vivo permeation and in vivo studies. Int J Pharm. 2018;553(1–2):386–97. Bali V, Ali M, Ali J. Study of surfactant combinations and development of a novel nanoemulsion for minimising variations in bioavailability of ezetimibe. Colloids Surf B Biointerfaces. 2010;76(2):410–20. Tamilvanan S, Benita S. The potential of lipid emulsion for ocular delivery of lipophilic drugs. Eur J Pharm Biopharm. 2004;58(2):357–68. Apaolaza PS, Delgado D, del Pozo-Rodríguez A, Gascón AR, Solinís MÁ. A novel gene therapy vector based on hyaluronic acid and solid lipid nanoparticles for ocular diseases. Int J Pharm. 2014;465(1–2):413–26. Fangueiro JF, Andreani T, Egea MA, et al. Design of cationic lipid nanoparticles for ocular delivery: development, characterization and cytotoxicity. Int J Pharm. 2014;461(1–2):64–73. Fahmy AM, Hassan M, El-Setouhy DA, Tayel SA, Al-Mahallawi AM. Voriconazole ternary micellar systems for the treatment of ocular mycosis: statistical optimization and in vivo evaluation. J Pharm Sci. 2021;110(5):2130–8. Balguri SP, Adelli GR, Janga KY, Bhagav P, Majumdar S. Ocular disposition of ciprofloxacin from topical, PEGylated nanostructured lipid carriers: Effect of molecular weight and density of poly (ethylene) glycol. Int J Pharm. 2017;529(1–2):32–43. Nayak K, Misra M. Triamcinolone acetonide-Loaded PEGylated microemulsion for the posterior segment of eye. ACS Omega. 2020;5(14):7928–39. Lakhani P, Patil A, Wu KW, et al. Optimization, stabilization, and characterization of amphotericin B loaded nanostructured lipid carriers for ocular drug delivery. Int J Pharm. 2019;572:118771. Craig JP, Simmons PA, Patel S, Tomlinson A. Refractive index and osmolality of human tears. Optom Vis Sci. 1995;72(10):718–24. Patel N, Nakrani H, Raval M, Sheth N. Development of loteprednol etabonate-loaded cationic nanoemulsified in-situ ophthalmic gel for sustained delivery and enhanced ocular bioavailability. Drug Deliv. 2016;23(9):3712–23. Fialho SL, da Silva-Cunha A. New vehicle based on a microemulsion for topical ocular administration of dexamethasone. Clin Exp Ophthalmol. 2004;32(6):626–32. López-Alemany A, Montés-Micó R, García-Valldecabres M. Ocular physiology and artificial tears. J Am Optom Assoc. 1999;70(7):455–60. Moiseev RV, Steele F, Khutoryanskiy VV. Polyaphron formulations stabilised with different water-soluble polymers for ocular drug delivery. Pharmaceutics. 2022;14(5):926. Radomska-Soukharev A, Wojciechowska J. Microemulsions as potential ocular drug delivery systems: phase diagrams and physical properties depending on ingredients. Acta Pol Pharm. 2005;62(6):465–71. Doshi U, Xu J. Effect of viscosity, surface tension and mucoadhesion on ocular residence time of lubricant eye drops. Invest Ophthalmol Vis Sci. 2009;50(13):4641–4641. Luo Q, Zhao J, Zhang X, Pan W. Nanostructured lipid carrier (NLC) coated with Chitosan Oligosaccharides and its potential use in ocular drug delivery system. Int J Pharm. 2011;403(1–2):185–91. Stahl U, Willcox M, Stapleton F. Osmolality and tear film dynamics. Clin Exp Optom. 2012;95(1):3–11. Murube J. Tear osmolarity. Ocul Surf. 2006;4(2):62–73. Varela-Fernández R, Díaz-Tomé V, Luaces-Rodríguez A, et al. Drug delivery to the posterior segment of the eye: biopharmaceutic and pharmacokinetic considerations. Pharmaceutics. 2020;12(3):269. Shetty R, Naidu JR, Nair AP, et al. Distinct ocular surface soluble factor profile in human corneal dystrophies. Ocul Surf. 2020;18(2):237–48. Romeo A, Musumeci T, Carbone C, et al. Ferulic acid-loaded polymeric nanoparticles for potential ocular delivery. Pharmaceutics. 2021;13(5):687. Carnevale C, Riva I, Roberti G, et al. Confocal microscopy and anterior segment optical coherence tomography imaging of the ocular surface and bleb morphology in medically and surgically treated glaucoma patients: a review. Pharmaceuticals (Basel). 2021;14(6):581. Khalil IA, Ali IH, El-Sherbiny IM. Noninvasive biodegradable nanoparticles-in-nanofibers single-dose ocular insert: in vitro, ex vivo and in vivo evaluation. Nanomedicine (Lond). 2019;14(1):33–55. Leonardi A, Bucolo C, Romano GL, et al. Influence of different surfactants on the technological properties and in vivo ocular tolerability of lipid nanoparticles. Int J Pharm. 2014;470(1–2):133–40. Ammar HO, Haider M, Ibrahim M, El Hoffy NM. In vitro and in vivo investigation for optimization of niosomal ability for sustainment and bioavailability enhancement of diltiazem after nasal administration. Drug Deliv. 2017;24(1):414–21. Tavakoli M, Mahboobian MM, Nouri F, Mohammadi M. Studying the ophthalmic toxicity potential of developed ketoconazole loaded nanoemulsion in situ gel formulation for ophthalmic administration. Toxicol Mech Methods. 2021;31(8):572–80. Mahboobian MM, Seyfoddin A, Aboofazeli R, Foroutan SM, Rupenthal ID. Brinzolamide-loaded nanoemulsions: ex vivo transcorneal permeation, cell viability and ocular irritation tests. Pharm Dev Technol. 2019;24(5):600–6. Ames P, Galor A. Cyclosporine ophthalmic emulsions for the treatment of dry eye: a review of the clinical evidence. Clin Investig (Lond). 2015;5(3):267–85. Boujnah Y, Mouchel R, El-Chehab H, Dot C, Burillon C, Kocaba V. Étude prospective, monocentrique, non contrôlée de l’efficacité, de la tolérance et de l’adhésion au traitement par ciclosporine 0,1 % au cours des sécheresses oculaires sévères [Prospective, monocentric, uncontrolled study of efficacy, tolerance and adherence of cyclosporin 0.1 % for severe dry eye syndrome]. J Fr Ophtalmol. 2018;41(2):129–35. Mandal A, Gote V, Pal D, Ogundele A, Mitra AK. Ocular Pharmacokinetics of a topical ophthalmic nanomicellar solution of cyclosporine (Cequa®) for dry eye disease. Pharm Res. 2019;36(2):36. Henostroza M, Melo K, Yukuyama MN, Löbenberg R, Bou-Chacra NA. Cationic rifampicin nanoemulsion for the treatment of ocular tuberculosis. Colloids Surf, A. 2020;597:124755. Kagkelaris K, Panayiotakopoulos G, Georgakopoulos CD. Nanotechnology-based formulations to amplify intraocular bioavailability. Ther Adv Ophthalmol. 2022;14:25158414221112356. Eroglu YI. A comparative review of Haute Autorité de Santé and National Institute for Health and Care Excellence health technology assessments of Ikervis® to treat severe keratitis in adult patients with dry eye disease which has not improved despite treatment with tear substitutes. J Mark Access Health Policy. 2017;5(1):1336043. Boyer DS, Yoon YH, Belfort R Jr, et al. Three-year, randomized, sham-controlled trial of dexamethasone intravitreal implant in patients with diabetic macular edema. Ophthalmology. 2014;121(10):1904–14. Wentz SM, Price F, Harris A, Siesky B, Ciulla T. Efficacy and safety of bromfenac 0.075% formulated in DuraSite for pain and inflammation in cataract surgery. Expert Opin Pharmacother. 2019;20(14):1703–9. Rodrigues GA, Lutz D, Shen J, et al. Topical drug delivery to the posterior segment of the eye: addressing the challenge of preclinical to clinical translation. Pharm Res. 2018;35(12):245. Ahn SJ, Hong HK, Na YM, et al. Use of rabbit eyes in pharmacokinetic studies of intraocular drugs. J Vis Exp. 2016;113:53878. U.S. National Library of Medicine, A randomized controlled trial comparing urea loaded nanoparticles to placebo: a new concept for cataract management, NCT03001466, 2016. Kim T, Sall K, Holland EJ, Brazzell RK, Coultas S, Gupta PK. Safety and efficacy of twice daily administration of KPI-121 1% for ocular inflammation and pain following cataract surgery. Clin Ophthalmol. 2018;13:69–86. U.S. National Library of Medicine, POLAT-001 compared to latanoprost ophthalmic solution in patients with ocular hypertension and open-angle glaucoma, NCT02466399, 2020. Wang LR, Wang Y, Wang SLW, **g**g JC, ** C. Timolol maleate cubic liquid crystal nanoparticle eye drops and preparation method thereof. C.N. Patent CN 1,06,619,573 A, 2016. Lee JY, Shin YJ, Sang-Rok R. ophthalmic nanoemulsion composition containing cyclosporine and method for preparing same, PH12015502587B1, 2016. Wang SJ, Cha KH, Kang H, Sun BK. Cyclosporine-containing non-irritative nanoemulsion ophthalmic composition, US 9,320,801 B2, 2016. XU S, Zhu Y, Fan Q, Ou S, Liu X. nanosuspension of tobramycin and dexamethasone and preparation method thereof, CN105708844, 2016. Weiss, S.L. Treatment of glaucoma and/or retinal diseases. WO 2017152129A2, 9 August 2017. Yates CR, Smith JS, Miller DD, Toutounchian JJ. Method for regulating retinal endothelial cell viability, in, US 9,566,255, 2017. Chen H, Enlow EM, Popov A. Pharmaceutical nanoparticles showing improved mucosal transport. A.U. Patent AU 2,013,256,092 B2, 2017. Campora G. Nanoparticle ophthalmic composition for the treatment of ocular disorders or diseases. U.S. Patent US 20,190,070,242 A1, 2018. Dongwoo L, Hyunju B, Younggwan K. Non-irritant ophthalmic composition containing cyclosporin, and convenient preparation method, US 15/747,618, 2018. Yates CR, Smith JS, Miller DD, Toutounchian JJ. Method for regulating retinal endothelial cell viability, in, US 10,010,516, 2018. Lopes FP, Jose E. Compositions of jasmonate compounds and methods of use. US 20,180,000,958 A1, 2018. Arumugham R, Upadhyay AK. Ophthalmic compositions and methods of use. U.S. Patent US 20,190,008,920 A1, 2018. Venkatraman S, Natarajan JV, Howden T, Boey F. inventors; Nanyang Technological University, Singapore Health Services Pte Ltd, assignee. Stable liposomal formulations for ocular drug delivery. United States patent US 9,956,195. 2018 May 1. Barman SP, Liu M, Barman K, Ward KL, Hackett B. inventors; Integral Biosystems LLC, assignee. Methods and biocompatible compositions to achieve sustained drug release in the eye. United States patent US 9,931,306. 2018 Apr 3. Fu J, Campochiaro PA, Hanes JS. inventors; Johns Hopkins University, assignee. Non-linear multiblock copolymer-drug conjugates for the delivery of active agents. United States patent application US 16/182,261. 2019 Mar 7. Davis ME, Davishan ME, Han H. Nanoparticles stabilized by nitrophenylboronic acid composition. JP 2,019,108,372A, 2019. Lee HC. Drug delivery implant for treating eye diseases, and preparation method therefore. WO 2,019,160,306A1, 2019. Liposome Corticosteroid for the Locally Injecting in Inflammation Lesion or Region. CN 109906075A, 18 June 2019. Aquilue JS, Gris MDCL, Gan˜an MID. ´ An oil-in-water nanoemulsion composition of clobetasol, in: WO2018233878A1, 2019. Rasappa Arumugham AU. Ophthalmic compositions and methods of use, in: WO2020047197A1, 2020. Junyeop L, Jae SY, Sang-rok R. Eye composition containing a cyclosporine and a method of preparing the same. KR20200000395A, 2 January 2020. Chul-hwan K, Hyun-seop N, Hye-min K, Da-hye S. A surfactant-free type ophthalmic nano-emulsion composition, and the manufacturing method thereof. KR 20200053205A, 18 May 2020. Qing D. Nanocrystalline eye drop, preparation method and application thereof. CN 110664757A, 28 May 2020. Jain S, Kompella UB, Musunuri S. Preservative free ocular compositions and methods for using the same for treating dry eye disease and other eye disorders, in: US10751337B2, 2020. Not applicable. This work was supported by the National Natural Science Foundation of China (82271041, 82201136), the Disciplinary Crossing Cultivation Program of Shanghai Jiao Tong University (YG2022QN055), the Basic Research Programs of Shanghai Ninth People’s Hospital, Shanghai Jiao Tong University School of Medicine (JYZZ152), Shanghai Key Clinical Specialty and Shanghai Eye Disease Research Center (2022ZZ01003). SL and LC contributed equally to this work. SL and LC drafted the manuscript and created all the figures. SL, LC and YF discussed the concepts of the manuscript. All authors read and approved the final manuscript. Not applicable. Not applicable. All authors declare that they had no competing interests. Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data. Li, S., Chen, L. & Fu, Y. Nanotechnology-based ocular drug delivery systems: recent advances and future prospects.
J Nanobiotechnol 21, 232 (2023). https://doi.org/10.1186/s12951-023-01992-2 Received: Accepted: Published: DOI: https://doi.org/10.1186/s12951-023-01992-2Availability of data and materials
Abbreviations
References
Acknowledgements
Funding
Author information
Authors and Affiliations
Contributions
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Consent for publication
Competing interests
Additional information
Publisher's Note
Rights and permissions
About this article
Cite this article
Keywords