Abstract
This study aimed to compare tumor lesion detectability and diagnostic accuracy of whole-body magnetic resonance imaging (WB-MRI) and radioiodine-labeled meta-iodo-benzylguanidine (mIBG) imaging techniques in patients with metastatic pheochromocytoma and paraganglioma (PPGL). This retrospective study included 13 patients had pheochromocytoma and 5 had paraganglioma, who were all suspected of having metastatic tumors. Each patient underwent WB-MRI and 123I-mIBG as a pretreatment screening for 131I-mIBG therapy. Two expert reviewers evaluated WB-MRI, 123I-mIBG images, and post-therapy 131I-mIBG images for the presence of metastatic lesions in the lungs, bones, liver, lymph nodes, and other organs. Diagnostic measures for detecting metastatic lesions, including sensitivity, specificity, accuracy, positive predictive value (PPV), negative predictive value (NPV), and receiver operating characteristics (ROC)—area under the curve (AUC), were calculated for each imaging technique. We analyzed WB-MRI images for detecting metastatic lesions, which demonstrated sensitivity, specificity, accuracy, PPV, NPV, and AUC of 82%, 97%, 90%, 96%, 86%, and 0.92, respectively. These values were 83%, 95%, 89%, 94%, 86%, and 0.90 in 123I-mIBG images and 85%, 92%, 89%, 91%, 87%, and 0.91 in post-therapy 131I-mIBG images, respectively. Our results reveal the comparable diagnostic accuracy of WB-MRI to one of the mIBG images.
Similar content being viewed by others
Introduction
Pheochromocytoma and paraganglioma (PPGL) are rare chromaffin cell-derived tumors that originate from the adrenal medulla or extra-adrenal paraganglia1. These tumor cells express the cell membrane norepinephrine transporter (NET), also known as uptake-1, and secrete catecholamine. Meta-iodo-benzylguanidine (mIBG) is a structural analog of norepinephrine, and it is actively taken up by PPGL cells via NET. Whole-body scans and single-photon emission computed tomography/X-ray computed tomography (SPECT/CT) with 123I-mIBG scintigraphy are widely available and used to assess the spread of mIBG-avid metastases and identify suitability for 131I-mIBG therapy in patients with PPGL2.
Since the 1980s, 131I-mIBG therapy has been widely used as a targeted radionuclide therapy in patients with PPGLs and mIBG-avid lesions. Moreover, post-therapeutic imaging following 131I-mIBG therapy demonstrated enhanced metastatic lesion detectability compared to diagnostic 123I-mIBG scintigraphy3,4. Further, 131I-mIBG serves as a therapeutic and diagnostic agent for PPGL in individuals with mIBG-avid metastases.
The current international guidelines recommend whole-body magnetic resonance imaging (WB-MRI) for detecting the presence of different cancer types5. Its effectiveness in detecting cancers and cancer-predisposition syndromes is well-documented, and it has numerous applications in clinical practice5,6. WB-MRI is recommended as a cancer screening image tool for individuals with a genetic predisposition for PPGL7,8, but its efficacy in detecting metastases in these patients and in comparison with 123I-mIBG and 131I-mIBG imaging techniques remains unknown. This study evaluated lesion detectability and the diagnostic characteristics of WB-MRI compared with 123I-mIBG and 131I-mIBG post-therapy in patients with metastatic PPGL.
Materials and methods
Study participants
The study included 18 patients, with data obtained from19 studies (a single hospital, Kanazawa University Hospital, Japan), who underwent WB-MRI and 123I-mIBG within one month as pretreatment to screen for 131I-mIBG therapy eligibility at Kanazawa University Hospital (Japan), from August 2019 to January 2022. All the patients underwent surgical removal of primary tumor lesions and histologically confirmed PPGL. The average age of the patients was 53.5 years old (average age: 53.5 ± 16.1 years), 12 patients were male (male/female ratio: 12/6), and 13 had pheochromocytoma whereas 5 had paraganglioma. All the patients were suspected of having metastatic tumor spread (Table 1). One patient (#6) was found to have positive mutations in the succinate dehydrogenase subunit B (SDHB) gene, but the status of other patients remains unclear. Family history could not be confirmed for any of the cases. Two patients did not undergo 131I-mIBG therapy due to progressive or stable disease. One patient underwent WB-MRI with 123I-mIBG imaging and 131I-mIBG therapy twice.
Image review and analysis
Two experienced reviewers (with 10 and 12 years of experience in imaging), blinded to the diagnosis, evaluated the presence of metastatic lesions in the lungs, bones, liver, lymph nodes, and other organs on images taken using WB-MRI, 123I-mIBG, and 131I-mIBG. Imaging modalities and acquisition characteristics include WB-MRI, WB-diffusion weighted image, apparent diffusion coefficient map, T1-weighted image, T2-weighted image, short inversion time inversion recovery weighted image; 123I-mIBG images, whole-body scan and SPECT/CT images 24 h after 123I-mIBG injection (PDR Pharma Co., Ltd, 222 MBq/person), post-therapy 131I-mIBG images, whole-body scan and SPECT/CT images 72–96 h after 131I-mIBG injection (POLATOM, Otwock, Poland or PDR Pharma Co., Ltd, 5550–7400 MBq/person). Lesions on images were classified as “positive” when one or more metastatic lesions and as “negative” when no metastatic lesions were identified (Table 2). A third independent expert reviewer (16 years of experience) who considered and combined in the analysis all imaging modalities tested (123I-mIBG image, post-therapy 131I-mIBG image, WB-MRI, plain/contrast-enhanced CT images, 18F-FDG-PET/CT images) and clinical information, established the gold standard.
Diagnostic measures
We calculated the following diagnostic measures to evaluate the presence of metastatic tumor lesions in the different organs considered: sensitivity, specificity, accuracy, positive predictive value (PPV), negative predictive value (NPV), and receiver operating characteristics (ROC)—area under the curve (AUC). AUC was calculated for each of the organs considered (lung, bone, liver, lymph node, and other organs). The diagnostic tests were compared using ROC—AUC and DeLong’s tests. Cohen’s kappa statistics were used to evaluate reviewers’ consistency.
Imaging protocol
A 1.5T MRI system (Philips Healthcare, Best, The Netherlands), equipped with a 20-channel head-neck coil and a 32-channel dS torso coil was used to examine all patients. The WB-MRI protocol developed in this study included several MR sequences, starting with a WB-diffusion-weighted image in a coronal plane. The WB-diffusion-weighted image sequence utilized a repetition time/time to echo of 6800/70 ms, a field of view set at 320 × 480 mm, and a 96 × 140 matrix size. The slice thickness was 5.0 mm, and inversion recovery with short-time inversion recovery (STIR) was used for fat suppression. Additionally, images were acquired with two b-factors of 0 and 800 s/mm2. Other sequences within the WB-MRI scan protocol, such as STIR TSE, T1W TSE, In/Out GRE, and T2W TSE, were acquired in different orientations, each with specific imaging parameters. The coronal WB-diffusion-weighted images were used to reconstruct three-dimensional maximum intensity projection (3D-MIP) images.
Anterior and posterior whole-body planar images and SPECT/CT images were acquired using a dual-head gamma camera (Symbia Intevo Bold; hybrid SPECT/CT scanner, Siemens Medical Solutions USA Inc., Hoffman Estates, IL, USA) after obtaining WB-MRI images. A low-medium energy general-purpose collimator was used for the 123I-mIBG imaging. Whole-body scintigraphy using 123I-mIBG was conducted with a matrix size of 256 × 1024 and a scan speed of 15 cm/min. The energy window was set to 159 keV, with a variance of ± 7.5%, optimized for 123I isotope detection. The SPECT/CT imaging in the 123I-mIBG protocol used a matrix size of 128 × 128, with each pixel measuring 4.8 mm. The imaging process involved 60 views (30 steps) at 20 s/step, with a total of 12.5 min/bed, evenly split across two detectors. Dedicated processing equipment (syngo Acquisition Workplace, Siemens Medical Solutions USA Inc., Hoffman Estates, IL, USA) was used to reconstruct the SPECT images.
Similarly to the 123I-mIBG imaging protocol, a high-energy collimator was used for 131I-mIBG imaging. The protocol for 131I-mIBG whole-body scintigraphy used a matrix size of 256 × 1024 with a scan speed of 20 cm/min. The energy window was specifically configured at 364 keV with a 10% variance. A 128 × 128 matrix size, with a pixel size of 4.8 mm, involving 60 views (30 steps) at 15 s/step, resulting in 7.5 min/bed of imaging, equally divided between two detectors, was used for the SPECT/CT imaging under the 131I-mIBG protocol. The SPECT images were reconstructed using dedicated processing equipment (syngo Acquisition Workplace, Siemens Medical Solutions USA Inc., Hoffman Estates, IL, USA).
Statistical analysis
The diagnostic tests were compared using ROC—AUC and DeLong’s tests. Cohen’s kappa statistics were used to evaluate reviewers’ consistency. Statistical analyses were performed using EZR software (ver.1.60)9 and JMP software (ver. 13.2.0). A P-value of < 0.05 indicated statistically significant.
Ethical approval and consent to participate
This study was conducted with ethical considerations in accordance with the Declaration of Helsinki and the ethical guidelines for biomedical research involving human subjects. The present study was approved by the ethics committee of Kanazawa University (Kanazawa University Medical Ethics Review Committee, Approval No. 2023-086 [114337]). Due to this study’s retrospective nature, written informed consent from each patient was waived by the Kanazawa University Medical Ethics Review Committee.
Results
Detectability of metastatic lesions using WB-MRI and mIBG imaging
We calculated the sensitivity, specificity, accuracy, PPV, NPV, and AUC for detecting metastatic lesions using WB-MRI, 123I-mIBG, and post-therapy 131I-mIBG images (Table 3). The results were 82%, 97%, 90%, 96%, 86%, and 0.92 for WB-MRI, 83%, 95%, 89%, 94%, 86%, and 0.90 for 123I-mIBG images, and 85%, 92%, 89%, 91%, 87%, and 0.91 for post-therapy 131I-mIBG images, respectively. The AUC did not significantly differ across the imaging modalities tested, with P-values of 0.55 and 0.78 for WB-MRI versus 123I mIBG and 131I-mIBG, respectively. The kappa coefficients for WB-MRI, 123I-mIBG, and post-therapy 131I-mIBG images were comparable when we evaluated reviewers’ agreements, with values of 0.87, 0.94, and 0.88, respectively. Therefore, we concluded that WB-MRI images demonstrated lesion detectability comparable to 123I-mIBG and post-therapy 131I-mIBG images in patients with PPGL (Table 3).
Detectability of metastatic lesions in each organ using WB-MRI and mIBG imaging
The AUC for detecting metastatic lesions in the lungs, bones, liver, lymph nodes, and other organs were 0.80, 0.96, 0.88, 0.91, and 0.97 for WB-MRI images, 0.89, 0.80, 0.75, 0.91, and 0.97 for 123I-mIBG images, 0.89, 0.96, 0.77, 0.89, and 0.97 for post-therapy 131I-mIBG images, respectively. The AUCs and the P-values did not significantly differ among the tested imaging modalities. WB-MRI images in each of the body locations considered demonstrated lesion detectability comparable to 123I-mIBG and post-therapy 131I-mIBG images (Table 3). Either 123I/131I-mIBG or WB-MRI images distinctly detected some lesions (Figs. 1, 2). Notably, identifying or distinguishing physiological from abnormal findings in body regions adjacent to organs with high mIBG uptake on 123/131I-mIBG scintigraphy was possible using WB-MRI (Figs. 2, 3). Rib metastasis in patient No. 3 was detectable by both WB-MRI and mIBG images, but the extent of the metastatic lesions was more clearly depicted by WB-MRI images. In patient No. 13, multiple bone metastases (ribs, vertebrae, pelvic bones) were observed, with WB-MRI images providing a more detailed depiction. However, the use of WB-MRI did not allow for discrimination between liver metastases and benign liver lesions in one case (Fig. 4).
A case of multiple bone metastases (patient No. 6). A male patient with multiple bone metastases of pheochromocytoma (left scapula, thoracic, and lumbar vertebra, as indicated by black arrows). 123/131I-mIBG images detected more lesions compared with WB-MRI. Lumbar vertebral metastases were detected clearly by 131I-mIBG images. (a,b) 123I-mIBG scintigrams (anterior and posterior). (c) The MIP of WB-MRI. (d,e) Post-therapy 131I-mIBG scintigram (anterior and posterior). mIBG meta-iodo-benzylguanidine, MIP maximum intensity projection, WB-MRI whole-body magnetic resonance image.
A case of multiple lung metastases with confusing liver accumulation in mIBG images (patient No. 7). A male patient in his 60s with multiple metastases of pheochromocytoma (lung and pelvis). Post-therapy 131I-mIBG image clearly detected multiple lung metastases (black arrows) compared with the 123I-mIBG image and WB-MRI. Conversely, mIBG images were confusing between liver metastases and physiologic accumulation (white arrows). (a) 123I-mIBG scintigram (anterior). (b) The MIP of WB-MRI. (c) Post-therapy 131I-mIBG scintigram (anterior). (d) DWI (axial). (e) 123I-mIBG SPECT/CT (axial). (f) Post-therapy 131I-mIBG SPECT/CT (axial). WB-MRI whole-body magnetic resonance image, MIP maximum intensity projection, DWI diffusion-weighted image, T2WI T2 weighted image, mIBG meta-iodo-benzylguanidine, SPECT/CT single-photon emission computed tomography/computed tomography.
A case of liver metastasis that could only be detected by WB-MRI (patient No. 14). A female patient in her 40s with multiple metastases of paraganglioma (liver, vertebra, pelvis, peritoneum). Liver metastasis could only be detected by WB-MRI (arrows). Conversely, mIBG images could not detect metastasis due to physiologic liver accumulation. (a,b) The MIP of WB-MRI and DWI coronal image (WB-MRI). (c) Post-therapy 131I-mIBG scintigram (anterior). WB-MRI whole-body magnetic resonance image, MIP maximum intensity projection, DWI diffusion-weighted image, mIBG meta-iodo-benzylguanidine.
A case of WB-MRI confusing liver metastases with benign hepatic lesions (patient No. 9). A male patient in his 50s with multiple bone metastases of pheochromocytoma. Liver metastases, in addition to the metastases, were suspected by WB-MRI alone (arrows). Abnormal signal density and structures of DWI and T2WI revealed liver cysts, with no abnormal accumulation on post-therapy 131I-mIBG images. (a) 123I-mIBG scintigram (anterior). (b) The MIP of WB-MRI. (c) Post-therapy 131I-mIBG scintigram (anterior). (d,g) DWI (axial). (e,h) 123I-mIBG SPECT/CT (axial). (f,i) Post-therapy 131I-mIBG SPECT/CT (axial). WB-MRI whole-body magnetic resonance image, MIP maximum intensity projection, DWI diffusion-weighted image, T2WI T2 weighted image, mIBG meta-iodo-benzylguanidine.
Discussion
The diagnostic accuracy of WB-MRI was comparable to the one of mIBG images for all the lesions and organs considered in patients with metastatic PPGL in the study. WB-MRI was considered more valuable than 123I-mIBG scintigraphy because it detects lesions around organs with physiologic mIBG accumulation and allows clinical follow-up without exposing the patients to radiation. Additionally, the kappa coefficient revealed a substantial concordance among reviewers, indicating high reproducibility of the obtained results.
WB-MRI is currently an established screening tool for malignancies10, and international guidelines recommend it for screening patients with malignant tumors5. WB-MRI exhibits high diagnostic performances in identifying several tumor types, with 86% sensitivity for tumors, 80% sensitivity and 75% specificity for lymph node metastases, and 96% sensitivity and 82% specificity for metastatic disease determination11. WB-MRI demonstrated better screening performances for PPGL predisposition to biochemical tests. However, a comprehensive comparison with other imaging modalities was unaddressed. This study revealed that WB-MRI demonstrated a detection rate similar to that of mIBG imaging, which is currently used as a standard tool in Japan to assess tumor progression in patients with metastatic PPGL.
Our study used both WB-MRI and mIBG imaging techniques to assess the detectability of tumor lesions and explore the diagnostic performances specific to each of the five organs included in the analysis. We classified images as “positive” if they detected one or more lesions (Table 2). The detection in each of the organs was inconsistent, with no significant difference in detection performances for lesions with organ metastasis.
WB-MRI’s detectability in the liver demonstrated no significant differences compared to 123I-mIBG or 131I-mIBG scintigraphy. However, WB-MRI holds greater potential for detecting liver metastases than 123I-mIBG and 131I-mIBG scintigraphy due to the physiological accumulation of mIBG in the liver. Congruently, both 123I-mIBG and 131I-mIBG images demonstrated lower sensitivity in detecting liver tumor lesions. These results are consistent with previous studies reporting the superiority of diffusion-weighted whole-body imaging with background body signal suppression (DWIBS) over mIBG scintigraphy for detecting metastatic lesions12. The number of cases with liver metastasis was small which could potentially bias the results, but our study revealed that WB-MRI can be used as a tool to detect liver metastases.
In lung metastases assessment, WB-MRI exhibited low detectability compared to 123I-mIBG and 131I-mIBG images. Petralia et al.13 revealed the detection of false-negative when analyzing lung metastases of < 4 mm and Nicholas et al.14 reported a low detection rate with MRI imaging for pulmonary nodules of < 4 mm. Hence, further technical improvements are required before considering WB-MRI a viable alternative to CT in routine clinical lung assessments. The limited spatial resolution may have hindered WB-MRI detection of diffuse micro-metastases. Resolution concerns could also arise concerning 123I-mIBG and 131I-mIBG scintigraphy, but this was not an issue in our study given the good mIBG accumulation in the included patients.
The high physiological signal intensity had the potential drawback of hindering WB-MRI assessment in case of LN metastases, but it also has some advantages, as it can detect lesions around organs with physiologically high mIBG accumulation. Both WB-MRI and 123I-mIBG scintigraphy require the combination of physiological and pathological findings for proper detection. This study demonstrated that two reviewers revealed almost identical detection capabilities in identifying lesions with minimal or negligible knowledge of physiological features. The detectability and concordance of others did not significantly differ with physiological findings, including pleural dissemination, retroperitoneal and pelvic dissemination, pleural invasion, local recurrence of retroperitoneal paraganglioma, posterior mediastinum, and peritoneal dissemination in 2, 1, 1, 1, 1, and 2 cases, respectively.
Previous reports have revealed the superior diagnostic performance of post-therapy 131I-mIBG images in PPGL and neuroblastoma compared to 123I-mIBG images3,15. However, the diagnostic performance of both modalities, including whole-body and individual organ assessments, revealed comparable results in this study. The kappa coefficients of the reviewers for WB-MRI, 123I-mIBG, and post-therapy 131I-mIBG images exhibited similar concordance levels. This similarity in diagnostic performance may be associated with the specific criteria selected, where a lesion was considered “positive” if it was detectable across multiple lesions (Table 2).
This study included patients with mIBG-avid metastases in the therapy, but notably, several factors, including genetic information and tumor heterogeneity, influenced the varying detection rate of 123I-mIBG scintigraphy. Previous studies reported the diagnostic performance of 123I-mIBG in primary or metastatic PPGL, indicating sensitivity of 28–100% and specificity of 70–100%2,16.
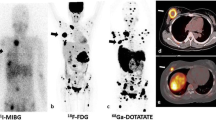
Koopmans et al. reported that both 111In-pentetreotide and anatomical imaging (CT/MRI) showed a sensitivity of 93% in the detection of head and neck paraganglioma (HNPGL), with that of 123I-mIBG imaging being only 44%, suggesting that 111In-pentetreotide is a more suitable functional imaging tool for assessing HNPGL disease, particularly when there is high clinical suspicion and negative 123I-mIBG scintigraphy17. Fluorodeoxyglucose labeled with fluorine-18 (18F-FDG) is used to detect various tumors, and 18F-FDG PET has demonstrated high sensitivity (83%) for metastatic diseases of pheochromocytoma (PCC) and paraganglioma (PGL) in patients with mutations in the succinate dehydrogenase subunit B (SDHB) gene18, making it valuable for localizing metastatic PPGLs that are negative for mIBG19. It images glucose metabolism in tumors and has been reported to have no correlation with the uptake and storage of catecholamines19. However, 18F-FDG has limited specificity for qualitative diagnosis due to uptake in various tumors18,20. 3,4-dihydroxy-6-[18F]fluoro-L-phenylalanine (18F-DOPA) PET exhibits high sensitivity and specificity for detecting non-metastatic PCCs (both 100%)21, but sensitivity decreases in metastatic PCC and PGL diseases associated with SDHB mutations when compared to CT/MRI (20–45%)18,22. The loss of the norepinephrine transporter in dedifferentiated metastatic lesions may contribute to this reduced sensitivity18. Kroiss et al. reported the superiority of 18F-DOPA PET/CT over 123I-mIBG scintigraphy in ten patients with extra-adrenal PGL23. While 18F-DOPA PET and diagnostic CT detected all HNPGL, 18F-DOPA PET occasionally failed to detect bone metastases found by diagnostic CT, leading to an overall reduced sensitivity of 69.2% for malignant HNPGLs. Janssen et al. reported that the superiority of 68Ga-DOTA(0)-Tyr(3)-octreotate (68Ga-DOTATATE) PET/CT over 18F-FDG and 18F-FDOPA PET/CT in the localizing sporadic metastatic PPGLs24. Recently, studies have shown the advantages of 18F-meta-fluorobenzylguanidine (18F-mFBG) PET/CT over 68Ga-DOTATATE PET/CT in patients with metastatic PPGLs25,26. It is suggested that a combination of functional and anatomical imaging is necessary to improve tumor detection. Therefore, a combination of imaging evaluations, including mIBG scintigraphy, somatostatin receptor imaging, and PET tracer imaging, is necessary to prepare for nuclear medicine treatment in a clinical setting. This indicates that results may differ when mIBG-negative patients are included.
Future studies focusing on the mIBG-negative patient group are required to further consolidate data on detection rates. Conducting follow-up observations in mIBG-negative patients using radiation-free imaging techniques may be possible if a high detection rate similar to the one of WB-MRI could be achieved.
This study is not without limitations. First, the number of patients included was limited, but this reflects the rarity of PPGL as a disease. Hence, minor differences observed among the imaging modalities under evaluation may not have reached statistical significance. Second, not all the metastatic lesions that demonstrated positive findings in WB-MRI and mIBG images underwent pathological diagnosis. This may introduce the possibility of false-positive findings. Third, the assessment did not account for the precise number of metastases because this study focused on the presence and extent of metastases, and any abnormal mIBG accumulation was considered “positive”.
Conclusion
This study revealed that WB-MRI and mIBG images demonstrated comparable diagnostic accuracy. However, we observed that WB-MRI holds some advantages as a technique for detecting lesions that are in proximity to organs characterized by physiological mIBG accumulation. Furthermore, WB-MRI offers a radiation-free alternative for follow-up examinations in patients with PPGL. WB-MRI may play a significant role in the long-term follow-up and treatment of patients with PPGL. Further research in the field is required to corroborate our findings and open new clinical management avenues for these patients, considering the retrospective study design.
Data availability
The data of this study are available from the corresponding author (HM) upon reasonable request.
Abbreviations
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance image
- SPECT/CT:
-
Single-photon emission computed tomography/X-ray computed tomography
- PPGL:
-
Paraganglioma
- mIBG:
-
Meta-Iodo-benzylguanidine
- WB-MRI:
-
Whole-body magnetic resonance image
- DWIBS:
-
Diffusion-weighted whole-body imaging with background body signal suppression
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
- ROC:
-
Receiver operating characteristics
- AUC:
-
Area under the curve
- FDG-PET/CT:
-
Fluorodeoxyglucose positron emission tomography/computed tomography
- NET:
-
Norepinephrine transporter
- SDHB:
-
Succinate dehydrogenase subunit B
- HNPGL:
-
Head and neck paraganglioma
- PCC:
-
Pheochromocytoma
- PGL:
-
Paraganglioma
- 18F-DOPA:
-
3,4-Dihydroxy-6-[18F]fluoro-L-phenylalanine
- 68Ga-DOTATATE:
-
68Ga-DOTA(0)-Tyr(3)-octreotate
- 18F-mFBG:
-
18F-meta-fluorobenzylguanidine
References
Lenders, J. W. M. & Eisenhofer, G. Update on modern management of pheochromocytoma and paraganglioma. Endocrinol. Metab. 32(2), 152–161 (2017).
Wiseman, G. A. et al. Usefulness of 123I-MIBG scintigraphy in the evaluation of patients with known or suspected primary or metastatic pheochromocytoma or paraganglioma: Results from a prospective multicenter trial. J. Nucl. Med. 50(9), 1448–1454 (2009).
Fukuoka, M. et al. Comparison of diagnostic value of I-123 MIBG and high-dose I-131 MIBG scintigraphy including incremental value of SPECT/CT over planar image in patients with malignant pheochromocytoma/paraganglioma and neuroblastoma. Clin. Nucl. Med. 36(1), 1–7 (2011).
Jain, A., Baracco, R. & Kapur, G. Pheochromocytoma and paraganglioma—An update on diagnosis, evaluation, and management. Pediatr. Nephrol. 35(4), 581–594 (2020).
Summers, P. et al. Whole-body magnetic resonance imaging: Technique, guidelines and key applications. Ecancermedicalscience 15(7), 1164 (2021).
Lenders, J. W. M. et al. Pheochromocytoma and paraganglioma: An endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 99(6), 1915–1942 (2014).
Gottumukkala, R. V., Gee, M. S., Hampilos, P. J. & Greer, M. C. Current and emerging roles of whole-body MRI in evaluation of pediatric cancer patients. Radiographics 39(2), 516–34 (2019).
Grasparil, A. D. et al. Whole-body MRI surveillance of cancer predisposition syndromes: Current best practice guidelines for use, performance, and interpretation. Am. J. Roentgenol. 215(4), 1002–1011 (2020).
Kanda, Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant. 48(3), 452–458 (2013).
Pasoglou, V. et al. The role of imaging in screening special feature: Review article whole body MRI and oncology: Recent major advances. Br. J. Radiol. 91, 20170664 (2018).
Schmidt, G. P. et al. High-resolution whole-body magnetic resonance image tumor staging with the use of parallel imaging versus dual-modality positron emission tomography-computed tomography: Experience on a 32-channel system. Investig. Radiol. 40(12), 743–753 (2005).
Takano, A. et al. Detection of metastatic lesions from malignant pheochromocytoma and paraganglioma with diffusion-weighted magnetic resonance imaging: Comparison with 18F-FDG positron emission tomography and 123I-MIBG scintigraphy. Ann. Nucl. Med. 22(5), 395–401 (2008).
Petralia, G. et al. Whole-body diffusion-weighted imaging: Is it all we need for detecting metastases in melanoma patients? Eur. Radiol. 23(12), 3466–3476 (2013).
Burris, N. S. et al. Detection of small pulmonary nodules with ultrashort echo time sequences in oncology patients by using a PET/MR system. Radiology 278(1), 239–246 (2016).
Yang, J. et al. I-131 MIBG post-therapy scan is more sensitive than I-123 MIBG pretherapy scan in the evaluation of metastatic neuroblastoma. Nucl. Med. Commun. 33(11), 1134–1137 (2012).
Granberg, D., Juhlin, C. C. & Falhammar, H. Metastatic pheochromocytomas and abdominal paragangliomas. J. Clin. Endocrinol. Metab. 106(5), e1937–e1952 (2021).
Koopmans, K. P. et al. 111In-octreotide is superior to 123I-metaiodobenzylguanidine for scintigraphic detection of head and neck paragangliomas. J. Nucl. Med. 49, 1232–1237 (2008).
Timmers, H. J. et al. Comparison of 18F-fluoro-L-DOPA, 18F-fluoro-deoxyglucose, and 18F-fluorodopamine PET and 123I-MIBG scintigraphy in the localization of pheochromocytoma and paraganglioma. J. Clin. Endocrinol. Metab. 94(12), 4757–4767 (2009).
Sisson, J. C. & Shulkin, B. L. Nuclear medicine imaging of pheochromocytoma and neuroblastoma. Q. J. Nucl. Med. 43(3), 217–223 (1999).
Shulkin, B. L. et al. Neuroblastoma: Positron emission tomography with 2-[fluorine-18]-fluoro-2-deoxy-D-glucose compared with metaiodobenzylguanidine scintigraphy. Radiology 199(3), 743–750 (1996).
Hoegerle, S. et al. Pheochromocytomas: Detection with 18F DOPA whole body PET—Initial results. Radiology 222(2), 507–512. https://doi.org/10.1148/radiol.2222010622 (2002).
Treglia, G. et al. Diagnostic performance of 18F-dihydroxyphenylalanine positron emission tomography in patients with paraganglioma: A meta-analysis. Eur. J. Nucl. Med. Mol. Imaging 39(7), 1144–1153 (2012).
Kroiss, A. S. et al. Compared to 123I-MIBG SPECT/CT, 18F-DOPA PET/CT provides accurate tumor extent in patients with extra-adrenal paraganglioma. Ann. Nucl. Med. 31(5), 357–365 (2017).
Janssen, I. et al. PET/CT comparing (68)Ga-DOTATATE and other radiopharmaceuticals and in comparison with CT/MRI for the localization of sporadic metastatic pheochromocytoma and paraganglioma. Eur. J. Nucl. Med. Mol. Imaging 43(10), 1784–1791 (2016).
Suurd, D. P. D. et al. [18F]mFBG PET/CT imaging outperforms MRI and [68 Ga]Ga-DOTA-TOC PET/CT in identifying recurrence pheochromocytoma. Eur. J. Nucl. Med. Mol. Imaging 50(5), 1538–1540 (2023).
Wang, P. et al. 18 F-MFBG PET/CT is an effective alternative of 68 Ga-DOTATATE PET/CT in the evaluation of metastatic pheochromocytoma and paraganglioma. Clin. Nucl. Med. 48(1), 43–48 (2023).
Acknowledgements
The authors would like to thank Takahiro Konishi and Masako Ohno (Department of Radiological Technology, Kanazawa University Hospital, Kanazawa, Ishikawa, Japan) for their technical support.
Author information
Authors and Affiliations
Contributions
H.M. wrote the main manuscript, and all authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mori, H., Wakabayashi, H., Saito, S. et al. Evaluating the diagnostic efficacy of whole-body MRI versus 123I-mIBG/131I-mIBG imaging in metastatic pheochromocytoma and paraganglioma. Sci Rep 14, 13828 (2024). https://doi.org/10.1038/s41598-024-64607-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-64607-2
- Springer Nature Limited