Abstract
Thyroid surgery often results in ischemia–reperfusion injury (IRI) to the parathyroid glands, yet the mechanisms underlying this and how to ameliorate IRI remain incompletely explored. Our study identifies a polyphenolic herbal extract—gallic acid (GA)—with antioxidative properties against IRI. Through flow cytometry and CCK8 assays, we investigate the protective effects of GA pretreatment on a parathyroid IRI model and decode its potential mechanisms via RNA-seq and bioinformatics analysis. Results reveal increased apoptosis, pronounced G1 phase arrest, and significantly reduced cell proliferation in the hypoxia/reoxygenation group compared to the hypoxia group, which GA pretreatment mitigates. RNA-seq and bioinformatics analysis indicate GA’s modulation of various signaling pathways, including IL-17, AMPK, MAPK, transient receptor potential channels, cAMP, and Rap1. In summary, GA pretreatment demonstrates potential in protecting parathyroid cells from IRI by influencing various genes and signaling pathways. These findings offer a promising therapeutic strategy for hypoparathyroidism treatment.
Similar content being viewed by others
Introduction
Hypoparathyroidism is characterized by reduced blood calcium and elevated blood phosphorus due to inadequate parathyroid hormone secretion1. The occurrence of hypoparathyroidism is associated with an increased risk of develo** cardiovascular disease and, in severe cases, can contribute to the development of heart failure2. Moreover, hypoparathyroidism can lead to renal insufficiency and kidney stone formation3. Primary causes of hypoparathyroidism include truncation or damage to the blood vessels that supply the parathyroid branches during total thyroidectomy and inadvertent removal of parathyroid glands4,5. However, with advancements in surgical techniques and implementation of preoperative or intraoperative parathyroid positioning6, the occurrence of improper parathyroid removal has become exceedingly rare. Nevertheless, the origin and branching of the vessels supplying the parathyroid glands are often intricate and present huge variability7. Consequently, even when parathyroid glands are intact in situ, vascular damage may occur from clam** or thermal injury during surgical procedures, which can lead to ischemia–reperfusion injury (IRI) of the glands.
IRI tends to occur in highly perfused organs and can result in conditions such as acute kidney injury, myocardial infarction, ischemic stroke and liver failure8. The abrupt interruption of blood flow induces ischemia, causing damage to metabolically robust tissues. Subsequent restoration of blood flow can elicit additional cellular damage, primarily through oxygen radical-mediated injury and inflammatory cascade responses, resulting in damage to vascular endothelial cells and organ function9. Therefore, it is critical to improve the understanding of IRI and to develop novel therapeutic strategies. One approach is through the regulation of genes8. Several previous studies have shown that BNIP3, HIF-1a and the Hippo pathway are all capable of being mechanisms to ameliorate IRI10,11,12,13.
Using pharmacological agents to alleviate IRI has emerged as a promising clinical treatment approach. Gallic acid (GA), also known as 3,4,5-trihydroxybenzoic acid, is a plant-derived polyphenolic compound with low molecular weight14. A previous study showed that GA exerts antioxidant properties by inhibiting cell apoptosis and suppressing the progression of inflammatory processes14. In addition, numerous studies have consistently demonstrated the protective role of GA in organs that are likely to suffer from IRI, such as the heart, brain and kidney. GA can ameliorate left ventricular dysfunction and hypertrophy, which are associated with diabetes, and reduce the ischemia–reperfusion-induced myocardial infarction area15,16. It can also mitigate oxidative stress injury caused by renal ischemia-reperfusion17, elevate antioxidant levels in brain tissue and reduce cerebral infarction attributed to cerebral IRI18. After pretreating patients with cyclophosphamide, GA can diminish inflammatory and oxidative stress injury to the kidneys in IRI induced by cyclophosphamide19. Collectively, these findings indicated that GA can mitigate IRI.
Notably, to the best of our knowledge, the potential benefits of GA pretreatment in parathyroid IRI have not been thoroughly explored. Therefore, the aim of the present study was to evaluate the protective effect of GA on parathyroid cells following IRI and to investigate the underlying mechanism.
Results
IRI reduces cell proliferation by inducing cell apoptosis and inducing cell cycle arrest
The hypoxia (Hypo) group was generated by culturing primary parathyroid cells in 1% O2 for 3, 6 or 12 h, after which, apoptosis, cell cycle progression and cell proliferation were assessed. The results showed that the early and late apoptotic rate gradually increased (**P < 0.01) with increasing hypoxic incubation time (3 h (8.79 ± 0.13%) vs. 6 h (10.97 ± 0.70%) vs. 12 h (11.55 ± 0.49%)) (Fig. 1A). Furthermore, halted cell cycle transition from G1 phase to S phase was observed (3 h (G1-49.47 ± 1.86%, S-32.5 ± 2.1%, G2/M-21.7 ± 1.35%) vs. 6 h (G1-55.43 ± 1.71%, S-23.97 ± 3.15%, G2/M-22.27 ± 0.91%) vs. 12 h (G1-55.73 ± 0.51%, S-20.07 ± 1.67%, G2/M-23.53 ± 1.21%) , ****P < 0.0001, **P < 0.01, *P < 0.05) (Fig. 1B), as well as reduced cell proliferation (3 h vs. 6 h vs. 12 h, at 24 h (3 h-0.78 ± 0.03, 6 h-0.74 ± 0.03, 12 h-0.73 ± 0.04), 48 h (3 h-1.09 ± 0.09, 6 h-0.88 ± 0.11, 12 h-0.75 ± 0.10), 72 h (3 h-1.52 ± 0.09, 6 h-1.34 ± 0.06, 12 h-1.13 ± 0.06) and 96 h (3 h-1.94 ± 0.09, 6 h-1.65 ± 0.05, 12 h-1.53 ± 0.05), ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05) (Fig. 1C–F). Notably, no significant difference in terms of apoptosis and proportion of cells in G1 phase was observed between cells cultured for 6 and 12 h, which suggested that the hypoxia-induced apoptosis of parathyroid cells may have plateaued at 6 h.
Changes in (A) early and late apoptosis, (B) cell cycle progression and (C) proliferative alterations in parathyroid cells during a 24-h period following incubation in 1% oxygen for 3, 6 or 12 h, (D) proliferative alterations in parathyroid cells during a 48-h period following incubation in 1% oxygen for 3, 6 or 12 h, (E) proliferative alterations in parathyroid cells during a 72-h period following incubation in 1% oxygen for 3, 6 or 12 h, (F) proliferative alterations in parathyroid cells during a 96-h period following incubation in 1% oxygen for 3, 6 or 12 h. ****P < 0.0001, **P < 0.01, *P < 0.05.
Subsequently, an IRI model was established by resupplying 21% O2 to parathyroid cells that were cultured with 1% O2 for 3, 6 or 12 h for another 3, 6 or 12 h, respectively. The results demonstrated a gradual increase (**P < 0.01) in apoptosis (3 h-3 h (11.45 ± 1.47%) vs. 6 h-6 h (20.88 ± 2.40%) vs. 12 h-12 h (21.52 ± 2.85%)) (Fig. 2A) and cell cycle arrest in G1 phase (3 h-3 h (G1-62.00 ± 1.04%, S-29.50 ± 2.26%, G2/M-7.42 ± 2.57%) vs. 6 h-6 h (G1-65.4 ± 0.70%, S-27.17 ± 2.22%, G2/M-6.86 ± 2.01%) vs. 12 h-12 h (G1-70.4 ± 2.65%, S-22.3 ± 4.42%, G2/M-6.39 ± 3.01%), **P < 0.01) (Fig. 2B), as well as reduced cell proliferation (3 h-3 h vs. 6 h-6 h vs. 12 h-12 h, at 24 h (3 h-3 h-0.92 ± 0.09, 6 h-6 h-0.88 ± 0.14, 12 h-12 h-0.82 ± 0.08), 48 h (3 h-3 h-1.32 ± 0.10, 6 h-6 h-1.05 ± 0.10, 12 h-12 h-0.88 ± 0.09), 72 h (3 h-3 h-1.51 ± 0.09, 6 h-6 h-1.21 ± 0.10, 12 h-12 h-1.05 ± 0.09) and 96 h (3 h-3 h-1.67 ± 0.13, 6 h-6 h-1.52 ± 0.11, 12 h-12 h-1.33 ± 0.09), ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05) (Fig. 2C–F). However, no significant difference in apoptotic rate was observed between the 6 h-6 h and 12 h-12 h groups.
Changes in (A) early and late apoptosis, (B) cell cycle progression and (C) proliferative alterations in parathyroid cells during a 24-h period following incubation in 1% oxygen for 3, 6 or 12 h, followed by incubation with 21% O2 for 3, 6 or 12 h, respectively, (D) proliferative alterations in parathyroid cells during a 48-h period following incubation in 1% oxygen for 3, 6 or 12 h, followed by incubation with 21% O2 for 3, 6 or 12 h, respectively, (E) proliferative alterations in parathyroid cells during a 72-h period following incubation in 1% oxygen for 3, 6 or 12 h, followed by incubation with 21% O2 for 3, 6 or 12 h, respectively, (F) proliferative alterations in parathyroid cells during a 96-h period following incubation in 1% oxygen for 3, 6 or 12 h, followed by incubation with 21% O2 for 3, 6 or 12 h, respectively. ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05.
The present results revealed that apoptosis was more pronounced in the IRI groups compared with that in the Hypo groups (3 h-3 h vs. 3 h, 6 h-6 h vs. 6 h, 12 h-12 h, ****P < 0.0001, **P < 0.01) (Fig. 3A), as was the cell cycle arrest in G1 phase (3 h-3 h vs. 3 h, 6 h-6 h vs. 6 h, 12 h-12 h, ****P < 0.0001) (Fig. 3B-D). In addition, the reduction in cell proliferation was more pronounced after 72 h in the IRI group compared with that in the Hypo group (***P < 0.001, **P < 0.01, *P < 0.05) (Fig. 3E,G), although not statistically significant (Fig. 3F). These findings indicated that IRI could induce further damage to parathyroid cells compared with hypoxia and identified the time-point of 6 h-6 h for further experiments.
Comparisons of (A) early and late apoptotic rate, (B) proportion of cells in G1 phase, (C) proportion of cells in S phase and (D) proportion of cells in G2/m phase, and (E) proliferative alterations in parathyroid cells from 24 to 96 h between the IRI group and the Hypo group at 3 h-3 h/3 h, (F) proliferative alterations in parathyroid cells from 24 to 96 h between the IRI group and the Hypo group at 6 h-6 h/6 h, (G) proliferative alterations in parathyroid cells from 24 to 96 h between the IRI group and the Hypo group at 12 h-12 h/12 h. The original flow cytometry plots for the data shown in A are in Figs. 1A and 2A, and those for the data shown in B–D are in Figs. 1B and 2B. ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05. Hypo hypoxia; IRI ischemia–reperfusion injury.
GA partially alleviates IRI-induced damage
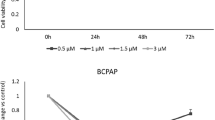
Based on the aforementioned results, the 6 h-6 h time point was used to investigate whether GA could protect cells from IRI. Parathyroid cells were pretreated with six concentrations of GA for 24 h before being exposed to a hypoxic environment. The results showed that the apoptotic rate gradually decreased (0 μM-24.2 ± 1.54%, 150 μM-14.44 ± 0.58%, 300 μM-11.43 ± 0.70%, 600 μM-10.69 ± 0.23%, 1200 μM-8.34 ± 0.10%, 2400 μM-8.69 ± 0.19%, ****P < 0.0001, **P < 0.01, *P < 0.05) with increasing drug concentrations (Fig. 4A), and the proportion of cells at G1 phase gradually decreased (0 μM-76.5 ± 1.31%, 150 μM-72.43 ± 1.40%, 300 μM-61.23 ± 1.25%, 600 μM-59.00 ± 1.74%, 1200 μM-8.34 ± 0.10%, 2400 μM-8.69 ± 0.19%, ****P < 0.0001, *P < 0.05), whereas the proportion of cells that entered S phase gradually increased (Fig. 4B). Furthermore, cell proliferation exhibited an ascending trend (at 48 h (0 μM-1.01 ± 0.07, 150 μM-1.00 ± 0.08, 300 μM-1.15 ± 0.05, 600 μM-1.38 ± 0.07, 1200 μM-1.43 ± 0.08, 2400 μM-1.42 ± 0.05), 72 h (0 μM-1.21 ± 0.05, 150 μM-1.24 ± 0.09, 300 μM-1.27 ± 0.06, 600 μM-1.47 ± 0.08, 1200 μM-1.60 ± 0.02, 2400 μM-1.68 ± 0.06) and 96 h (0 μM-1.46 ± 0.06, 150 μM-1.47 ± 0.08, 300 μM-1.61 ± 0.04, 600 μM-1.78 ± 0.04, 1200 μM-2.01 ± 0.10, 2400 μM-2.10 ± 0.08), ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05)in response to increasing concentrations of GA (Fig. 4D–F). Comparing the cells treated with different concentrations of GA, cells treated with 1200 μM exhibited the most significant changes and were thus chosen for subsequent experiments. The results revealed that pretreatment with 1200 μM GA significantly inhibited apoptosis (GA vs. IRI, ***P < 0.001) (Fig. 5A), enhanced cell proliferation (GA vs. IRI, at 48 h, 72 h and 96 h,****P < 0.0001) (Fig. 5B) and restored cell cycle progression (GA vs. IRI, ****P < 0.0001, **P < 0.01) (Fig. 5C).
Changes in (A) early and late apoptosis, (B) cell cycle progression, (C) proliferative alterations in parathyroid cells during a 24-h period, (D) proliferative alterations in parathyroid cells during a 48-h period, (E) proliferative alterations in parathyroid cells during a 72-h period, (F) proliferative alterations in parathyroid cells during a 96-h period, pretreated with different concentrations of gallic acid for 24 h before being cultured in a hypoxic environment for 6 h and an oxygenated environment for an additional 6 h. ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05.
Comparisons of (A) apoptosis, (B) proliferation and (C) cell cycle progression between parathyroid cells that were pretreated with GA at 1200 μM for 24 h, or non-treated cells following exposure to 6 h-6 h IRI. The original flow cytometry plots for the data shown in (A) are in Figs. 2A and 4A, and those for the data shown in (C) are in Figs. 2B and 4B. ****P < 0.0001, ***P < 0.001, **P < 0.01. OD optical density; GA gallic acid; IRI ischemia–reperfusion injury.
RNA-seq and bioinformatics analysis show the potential mechanism of GA in IRI
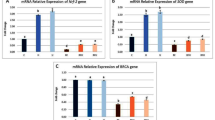
RNA-seq was performed to investigate the mechanism underlying the effects of GA on IRI. The cells were divided into the following groups: negative control (NC) group, consisting of parathyroid primary cells; model (M) group, consisting of cells that underwent IRI (6 h-6 h); treatment (T) group, consisting of cells that were pretreated with 1200 μM GA and underwent IRI (6 h-6 h). The differential expression levels of genes were analyzed, and |log2 (fold change)|> 1 and P < 0.05 were the cutoff for significantly altered genes. The results indicated that 3315 genes were significantly downregulated and 117 genes were significantly upregulated in the treatment group compared with in the model group, and 8170 genes were significantly downregulated and 596 genes were significantly upregulated in the model group compared with in the NC group (Fig. 6A,B,E,F). Further intersection analysis of the downregulated genes in the treatment versus model comparison and the upregulated genes in the model versus NC comparison (Fig. 6C), as well as the upregulated genes in the treatment versus model comparison and the downregulated genes in the model versus NC comparison (Fig. 6D) showed a total of 105 and 13 shared genes, respectively. Subsequently, the significantly enriched KEGG signaling pathways were determined, such as ‘Fat digestion and absorption’, ‘alpha-Linolenic acid metabolism’, ‘IL-17 signaling pathway’, ‘Limoleic acid metabolism’, ‘PPAR signaling pathway’, ‘Inflammatory mediator regulation of TRP channels’, ‘Ras signaling pathway’, ‘p53 signaling pathway’, ‘TNF signaling pathway’, ‘AMPK signaling pathway’, ‘Calcium signaling pathway’, ‘cAMP signaling pathway’, ‘MAPK signaling pathway’, ‘PI3K-Akt signaling pathway’, ‘Chemokine signaling pathway’, ‘ABC transporters Rap1 signaling pathway’, and ‘Regulation of actin cytoskeleton’. A total of 13 genes (Fig. 6G), including PLA2G3, PLA2G2F, HTR4, GYS2, MMP1, MMP9, DUSP5, RRM2, TRPV3, TRPV1, HMGCS2, FOSB and NPC1L1 were upregulated in the M group and downregulated in the T group, and four genes (Fig. 6H), including TIAM1, ABCA6, SUCNR1 and PPBP were downregulated in the M group and upregulated in the T group.
RNA-sequencing analysis of mRNA expression changes. (A and E) Differentially expressed genes in the T group compared with the M group, and (B and F) differentially expressed genes in the M group compared with the NC group. Intersection analysis of (C) downregulated genes in the T vs. M comparison and upregulated genes in the of M vs. NC comparison, and (D) upregulated genes in the T vs. M comparison and the downregulated genes in the M vs. NC comparison. KEGG enrichment analysis of (G) genes with elevated expression in the M group and reduced expression in the T group relative to the NC group, and (H) genes with reduced expression in the M group and elevated expression in the T group relative to the NC group. KEGG Kyoto encyclopedia of genes and genomes; M model; NC, negative control; T treatment.
Discussion
During thyroid surgery, the parathyroid glands are susceptible to damage, which can result in IRI. IRI can further induce hypocalcemia and other clinical symptoms, such as convulsions. In severe cases, it may severely affect vital organs, such as the heart and kidneys. Consequently, careful consideration must be given to minimize the impact of IRI1,8. The present study established an Hypo model using primary parathyroid cells and an ischemia–reperfusion model to explore the effect of GA on IRI. The results showed that when applied prior to the occurrence of ischemia–reperfusion, GA significantly inhibited IRI-induced apoptosis, restored the normal cell cycle and promoted cell proliferation, thereby confirming the protective effect of GA on parathyroid cells.
GA is a low molecular weight tri-phenolic compound that has potent free radical-scavenging properties, and notable anti-inflammatory and anti-oxidative stress effects20. It is well known that IRI triggers oxidative stress injury by producing reactive oxygen species, which further induce apoptosis and the secretion of inflammatory factors21,22. Previous studies20,21,22 have indicated that GA may possess the potential to ameliorate cellular damage caused by ischemia–reperfusion, which was verified in the present study.
To explore the mechanism of GA in IRI, the present study conducted an RNA-seq analysis and a comprehensive literature review, which revealed that GA likely exerts its anti-oxidative stress effect through regulating the expression or function of MMP1, MMP9, DUSP5, GYS2, TRPV3, TRPV1, FOSB, TIAM1, SUCNR1 and PPBP23,24,25,26,27,28,29,30,31,32,33,34,35,36. According to the KEGG signaling pathway enrichment analysis, MMP1, MMP9 and FOSB were found to be enriched in the ‘IL-17 signaling pathway’. When IRI occurs, cytokines, chemokines and MMPs are released to trigger an inflammatory response and activate the IL-17 signaling pathway37, which in turn exacerbates tissue damage. Previous studies have revealed that inhibiting the IL-17 pathway can significantly alleviate IRI in the heart38,39,40. MMP1 and MMP9 belong to the MMP family, and downregulating their expression has been shown to reduce IRI in the heart and brain23,24,25,26. FOSB serves as a component of AP-1 and serves a crucial role in upregulating the activity of inflammatory macrophages during IRI27,28. The present findings indicated that the expression levels of MMP1, MMP9 and FOSB were significantly increased during hypoxia-reoxygenation injury and ameliorated following pretreatment with GA. These results suggested that GA may effectively mitigate ischemia–reperfusion-related inflammation by downregulating the expression of MMP1, MMP9 and FOSB. Previous studies showed that GA can activate the PPAR signaling pathway by downregulating MMP141,42. Additionally, GA can inhibit activation of the TNF signaling pathway, which leads to the downregulation of MMP9 expression43,44. Collectively, these results demonstrated that the protective effects of GA on parathyroid cells undergoing IRI may be via regulating the expression levels of MMP1, MMP9 and FOSB.
The AMPK signaling pathway has a pivotal role in IRI as a central regulatory pathway. As a cellular energy sensor, AMPK is activated in response to substantial depletion of cellular energy. Activation of the AMPK pathway protects cells from IRI by initiating catabolism to restore ATP production, while simultaneously inhibiting anabolism to prevent further ATP depletion during ischemia-reperfusion45. Additionally, the AMPK pathway enhances the antioxidant activity of Nrf2 and reduces oxidative stress45,46. Conversely, the phosphorylation of GYS2 at Ser7 results in inactivation of GYS2 when the AMPK signaling pathway is active29. While the activation of the PI3K/AKT signaling pathway has been shown to mitigate IRI47,48, it paradoxically results in the upregulation of GYS2 expression49. This outcome seems contradictory to the experimental aforementioned findings. The present results demonstrated that GA alleviated IRI in parathyroid cells by downregulating GYS2 and activating the AMPK signaling pathway. However, further studies are required to determine the association among GA, GYS2 and the PI3K/AKT signaling pathway.
DUSP5 is an inducible bispecific kinase with three binding sites (Thr321, Ser346 and Ser376), which serves a crucial role in dephosphorylating ERK, JNK and p38, which are key signaling molecules within the MAPK signaling pathway. This process enables DUSP5 to regulate the function of MAPK30,31. Notably, when the MAPK/ERK and MAPK/p38 signaling pathways are inhibited, damage caused by ischemia–reperfusion is alleviated50,51. Similarly, the present results showed that GA could ameliorate IRI through regulating the DUSP5-mediated MAPK signaling pathway. However, further validation is necessary to determine the precise mechanism underlying this phenotype.
Transient receptor potential (TRP) channels have a pivotal role in mediating the release of cytokines in inflammation and oxidative stress injury32,33. Among these channels, TRPV1 and TRPV3, which are associated with inflammation, are primarily implicated in oxidative stress-induced cellular injury. Furthermore, TRP channels have been implicated in the pathogenesis of IRI in myocardial studies52,53. Similarly, the present study revealed that GA can modulate TRPV1 and TRPV3 of the TRP channels, thereby alleviating IRI.
During the reperfusion phase of IRI, the secretion of pro-inflammatory factors and macrophage-related chemokines is elevated, and can be used as surrogates to predict the extent of tissue damage54,55. Chemokine signaling pathways are instrumental in regulating cell polarization and inflammatory responses56. Deficiency of TIAM1, a key regulatory protein, leads to reduced cellular chemotaxis34. In addition, the expression of PPBP is positively correlated with CXCL8 expression35. Surprisingly, in the present study, GA pretreatment resulted in the upregulation of both TIAM1 and PPBP, in other word, IRI leads to an increase in cell chemokine levels, along with elevated expression of TIAM1 and PPBP. In theory, the application of GA should mitigate the impact of IRI on cells, thereby reducing chemokine levels, as well as the expression of TIAM1 and PPBP. However, our sequencing data indicates an increase in the expression of TIAM1 and PPBP in the T group, which is a discrepancy from the literature analysis. This suggests the existence of potentially distinct regulatory mechanisms that need to be explored in future.
The cAMP signaling pathway facilitates transduction of vasoactive transmitters, regulates vascular barriers and modulates inflammatory responses. It encompasses three principal effector proteins: Protein kinase A (PKA), cyclic-nucleotide-gated ion channels, and exchange proteins directly activated by cAMP/Epacs57. IRI disrupts the vascular barrier, leading to increased vascular permeability and subsequent recruitment of inflammation-associated cells, which eventually promotes the inflammatory response58,59. Previous studies have shown that increasing cAMP/PKA expression during IRI can effectively mitigate IRI60,61. TIAM1 serves a crucial role in elevating activation of the cAMP signaling pathway, thereby promoting stabilization of the vascular endothelial barrier62. By contrast, increased signaling of SUCNR1 leads to a decrease in cAMP expression36. The present results showed that GA upregulated the expression levels of both TIAM1 and SUCNR1, thereby alleviating IRI in parathyroid cells. Notably, the observed change in TIAM1 expression was consistent, whereas the change in SUCNR1 expression was inconsistent with the findings of a previous study36. These discrepancies need to be further examined in future studies.
Activation of the Rap1 signaling pathway promotes cellular anti-inflammatory, antioxidant and anti-apoptotic functions63. Additionally, within the cAMP/Epac signaling axis, Rap1 activation can stabilize the vascular endothelial barrier62. Notably, TIAM1 is implicated in the regulation of the cAMP signaling pathway. The results of the present study demonstrated an association between increased TIAM1 expression and the Rap1 signaling pathway identified by KEGG pathway enrichment analysis. However, further experiments are required to further determine this association. It has been discovered that downregulation of the actin cytoskeleton can attenuate oxidative stress in vascular smooth muscle during ischemia-reperfusion64. Conversely, elevated TIAM1 activity promotes actin cytoskeleton reorganization65. Thus, the TIAM1-dependent actin cytoskeleton signaling axis may not serve as a regulatory pathway for GA in ameliorating IRI. Additionally, TIAM1 is a direct mediator of Rac activation within the RAS signaling pathway that can promote intercellular adhesion66. Cell adhesion resulting from overexpression of vascular cell adhesion molecules is one of the pathogenic factors underlying IRI67. Consequently, inhibiting activation of the RAS signaling pathway can reduce apoptosis and enhance endovascular proliferation68. However, these findings are inconsistent with the experimental results of the present study; therefore, it is worth considering that GA may exert its regulatory role through TIAM1 in the Rap1 signaling pathway.
In conclusion, the present study not only confirmed the damage induced by IRI in parathyroid cells, but also demonstrated the protective role of GA against such damage. The results showed that GA may be considered a novel therapeutic approach to manage parathyroid IRI in the clinic. Furthermore, the preliminary mechanism investigation (Fig. 7) revealed that eight genes (MMP1, MMP9, FOSB, GSY2, DUSP5, TRPV1/3 and TIAM1) that belonged to various signaling pathways may participate in the process. The identification of these genes provides a foundation for subsequent mechanistic studies and may provide information on the potential clinical application of GA under different circumstances.
During ischemia–reperfusion injury in parathyroid cells, the expression levels of FOSB, MMP1, MMP9, GYS2, DUSP5 and TRPV1/3 were upregulated, whereas the expression of TIAM1 was downregulated. This may lead to the activation or inhibition of several corresponding signaling pathways, resulting in apoptosis, cell cycle arrest and defective proliferation of parathyroid cells. Pretreatment with gallic acid can reverse the changes in the expression of the aforementioned genes during ischemia–reperfusion injury, thus alleviating apoptosis, and restoring the normal cell cycle progression and proliferation to a certain extent.
Material and methods

GA. GA (cat. no. S4603) was obtained from Selleck Chemicals and was dissolved in dimethyl sulfoxide (cat. No. D8370, purity > 99.9%, Solarbio) according to the manufacturer’s instructions. The official recommended starting effective concentration of GA for use in PC12 cells is 50 μM. To design the drug concentration gradients, this value was used as a reference, with preliminary experiments assessing concentrations ranging from 0 to 6000 μM (data not shown) in primary parathyroid cells. For the present study, the experimental drug concentrations used were 0, 150, 300, 600, 1200 and 2400 μM.
Primary parathyroid cell culture. The rabbit parathyroid gland primary cells (cat. no. RAB-iCell-g014) were purchased from the iCell Bioscience Inc, Shanghai, and they were cultured using the ICell Primary Epithelial Cell Culture System (cat. no. PriMed-iCell-001) under conditions of 37 °C and 5% CO2 concentration. We monitored the growth and cell structure of primary parathyroid cells on a daily basis. Additionally, we refreshed the complete culture medium every two days to ensure that the cells received the essential nutrients they required.
Cellular models. Rabbit parathyroid primary cell were obtained and were separated into the following groups: The negative control (NC) group, without any specific treatment. The hypoxia (Hypo) group, in which the progenitor cells were cultured in a 1% oxygen environment for 3, 6 or 12 h. The IRI group, in which the progenitor cells were cultured in a 1% oxygen environment for 3, 6 or 12 h, followed by reoxygenation to a normal 21% oxygen environment and continued culturing for 3, 6 or 12 h. In the treatment group, GA pretreatment was administered to the parathyroid primary cells for 24 h prior to ischemia–reperfusion.
Flow cytometric analysis of apoptosis and cell cycle progression. Cells (> 1 × 106 cells/well) were grown in 6-well plates and, after adherence, were treated according to the experimental requirements. The treated cells were then digested with 0.25% trypsin, washed three times in PBS and subjected to flow cytometry using the Annexin V-FITC/PI Apoptosis detection kit (cat. no. 40302ES60; Shanghai Yeasen Biotechnology Co., Ltd.) to detect apoptosis according to the manufacturer’s protocol. For cell cycle analysis, the cells were fixed in 75% cold ethanol for 24 h at 4 °C, after ethanol fixation, centrifuge the cells at room temperature for 5 min (200 × g), carefully remove the upper ethanol layer after centrifugation, add 100 ul of PBS to gently resuspend the cells, and then centrifuge again at room temperature for 5 min (200 × g), carefully aspirate the upper PBS layer after centrifugation. and stained with 100 μl PI containing 50 μl RNaseA at room temperature to detect cell cycle progression. Flow cytometry was performed using a flow cytometer (CytoFLEX S; Beckman Coulter, Inc.) and the results were analyzed and the plots were generated using FlowJo v10 software (FlowJo, LLC).
Cell Counting Kit-8 (CCK-8) cell proliferation assay. Cells were seeded in 96-well plates (4000 cells/well), and were treated according to the experimental requirements. Subsequently, cell proliferation was assessed at 24, 48, 72 and 96 h using a CCK-8 kit (cat. no. 40203ES80; Shanghai Yeasen Biotechnology Co., Ltd.) for 4 h and the OD values at 450 nm were measured in a multifunctional enzyme plate reader. Graphs were plotted using GraphPad Prism v9 (Dotmatics).
RNA-sequencing (RNA-seq) and bioinformatics analysis. Cells were seeded in 10-cm dishes (> 1 × 107 cells/well) were treated according to the experimental requirements. Subsequently, the treated cells were subjected to RNA-seq (resulting in dataset no. GSE240162), which was performed by Hangzhou LC Biotechnology Co. (project no. Is LC-P20220413-037). R v4.0.4 (https://www.r-project.org/) was used to load DESeq269 (http://www.bioconductor.org/packages/release/bioc/html/DESeq2.html)/edgeR70 (http://www.bioconductor.org/packages/release/bioc/html/edgeR.html) for differential expression analysis, and gene expression changes (groups T vs. M and M vs. NC) were considered statistically significant if |log2 (fold change)|> 1 and P < 0.05. For differential expression clustering analysis Log10(FPKM + 1) was used for gene expression presentation, with colors ranging from blue through to white to red indicating low to high expression, respectively. Hiplot71 was used to plot Venn diagrams and SangerBox72 was used for Kyoto Encyclopedia of Genes and Genomes (KEGG) signaling pathway enrichment analysis.
Statistical analysis
Two-way ANOVA followed by Tukey’s multiple-comparisons test was used to analyze the differences among multiple groups when two variables were being assessed. When one variable was being assessed, one-way ANOVA and Tukey’s multiple-comparisons test was performed. All statistical analyses were performed using GraphPad Prism version 9 (GraphPad Software; Dotmatics). All experiments were repeated independently at least three times and the results are shown as the mean ± SD. P < 0.05 was considered to indicate a statistically significant difference.
Data availability
The RNA-seq datasets generated and analyzed during the current study are available in the GEO repository (https://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE240162). The other datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- GA:
-
Gallic acid
- IRI:
-
Ischemia–reperfusion injury
- Hypo:
-
Hypoxia
- TRP:
-
Transient receptor potential
- NC:
-
Negative control
- M:
-
Model
- T:
-
Treament
- PKA:
-
Protein kinase A
References
Mannstadt, M. et al. Hypoparathyroidism. Nat. Rev. Dis. Primers. 31(3), 17055. https://doi.org/10.1038/nrdp.2017.55 (2017).
Yao, L. et al. Complications, symptoms, presurgical predictors in patients with chronic hypoparathyroidism: A systematic review. J. Bone Miner. Res. 37(12), 2642–2653. https://doi.org/10.1002/jbmr.4673 (2022).
Bilezikian, J. P. Hypoparathyroidism. J. Clin. Endocrinol. Metab. 105(6), 1722–1736. https://doi.org/10.1210/clinem/dgaa113 (2020).
Cho, J. N., Park, W. S. & Min, S. Y. Predictors and risk factors of hypoparathyroidism after total thyroidectomy. Int. J. Surg. 34, 47–52. https://doi.org/10.1016/j.ijsu.2016.08.019 (2016).
Jason, D. S. & Balentine, C. J. Intraoperative decision making in parathyroid surgery. Surg. Clin. North Am. 99(4), 681–691. https://doi.org/10.1016/j.suc.2019.04.008 (2019).
Baj, J. et al. Preoperative and intraoperative methods of parathyroid gland localization and the diagnosis of parathyroid adenomas. Molecules. 25(7), 1724. https://doi.org/10.3390/molecules25071724 (2020).
Mohebati, A. & Shaha, A. R. Anatomy of thyroid and parathyroid glands and neurovascular relations. Clin. Anat. 25(1), 19–31. https://doi.org/10.1002/ca.21220 (2012).
Tang, J. & Zhuang, S. Histone acetylation and DNA methylation in ischemia/reperfusion injury. Clin. Sci. (Lond). 133(4), 597–609. https://doi.org/10.1042/CS20180465 (2019).
Anaya-Prado, R., Toledo-Pereyra, L. H., Lentsch, A. B. & Ward, P. A. Ischemia/reperfusion injury. J. Surg. Res. 105(2), 248–258. https://doi.org/10.1006/jsre.2002.6385 (2002).
Fu, Z. J. et al. HIF-1α-BNIP3-mediated mitophagy in tubular cells protects against renal ischemia/reperfusion injury. Redox Biol. 36, 101671. https://doi.org/10.1016/j.redox.2020.101671 (2020).
Zheng, J. et al. HIF-1α in myocardial ischemia-reperfusion injury (Review). Mol. Med. Rep. 23(5), 352. https://doi.org/10.3892/mmr.2021.11991 (2021).
Liu, Y. et al. Activation of YAP attenuates hepatic damage and fibrosis in liver ischemia-reperfusion injury. J. Hepatol. 71(4), 719–730. https://doi.org/10.1016/j.jhep.2019.05.029 (2019).
Nakamura, K. et al. Macrophage heme oxygenase-1-SIRT1-p53 axis regulates sterile inflammation in liver ischemia-reperfusion injury. J. Hepatol. 67(6), 1232–1242. https://doi.org/10.1016/j.jhep.2017.08.010 (2017).
Al Zahrani, N. A., El-Shishtawy, R. M. & Asiri, A. M. Recent developments of gallic acid derivatives and their hybrids in medicinal chemistry: A review. Eur. J. Med. Chem. 15(204), 112609. https://doi.org/10.1016/j.ejmech.2020.112609 (2020).
Ramezani-Aliakbari, F., Badavi, M., Dianat, M., Mard, S. A. & Ahangarpour, A. Effects of gallic acid on hemodynamic parameters and infarct size after ischemia-reperfusion in isolated rat hearts with alloxan-induced diabetes. Biomed. Pharmacother. 96, 612–618. https://doi.org/10.1016/j.biopha.2017.10.014 (2017).
Liu, X. et al. GA increases atrial natriuretic peptide secretion and mechanical dynamics through activation of PKC. Life Sci. 15(181), 45–52. https://doi.org/10.1016/j.lfs (2017).
Canbek, M. et al. The examination of protective effects of gallic acid against damage of oxidative stress during induced-experimental renal ischemia-reperfusion in experiment. Bratisl. Lek. Listy. 115(9), 557–562. https://doi.org/10.4149/bll_2014_108 (2014).
Praveen Kumar, P. et al. A new cerebral ischemic injury model in rats, preventive effect of gallic acid and in silico approaches. Saudi J. Biol. Sci. 28(9), 5204–5213. https://doi.org/10.1016/j.sjbs.2021.05.044 (2021).
Baharmi, S. et al. Pretreatment with gallic acid mitigates cyclophosphamide induced inflammation and oxidative stress in mice. Curr. Mol. Pharmacol. 15(1), 204–212. https://doi.org/10.2174/1874467214666210531162741 (2022).
Nouri, A., Heibati, F. & Heidarian, E. Gallic acid exerts anti-inflammatory, anti-oxidative stress, and nephroprotective effects against paraquat-induced renal injury in male rats. Naunyn Schmiedebergs Arch. Pharmacol. 394(1), 1–9. https://doi.org/10.1007/s00210-020-01931-0 (2021).
Bardallo Raquel, G. et al. Nrf2 and oxidative stress in liver ischemia/reperfusion injury. FEBS J. 289(18), 5463–5479. https://doi.org/10.1111/febs.16336 (2022).
Soares, R. O. S., Losada, D. M., Jordani, M. C., Évora, P. & Castro-E-Silva, O. Ischemia/reperfusion injury revisited: An overview of the latest pharmacological strategies. Int. J. Mol. Sci. 20(20), 5034. https://doi.org/10.3390/ijms20205034 (2019).
Chen, H., Li, D., Saldeen, T. & Mehta, J. L. TGF-beta 1 attenuates myocardial ischemia-reperfusion injury via inhibition of upregulation of MMP-1. Am. J. Physiol. Heart Circ. Physiol. 284(5), H1612–H1617. https://doi.org/10.1152/ajpheart.00992.2002 (2003).
Li, D. et al. LOX-1 inhibition in myocardial ischemia-reperfusion injury: Modulation of MMP-1 and inflammation. Am. J. Physiol. Heart Circ. Physiol. 283(5), H1795–H1801. https://doi.org/10.1152/ajpheart.00382.2002 (2002).
Liu, M. B. et al. Icariside II attenuates cerebral ischemia/reperfusion-induced blood-brain barrier dysfunction in rats via regulating the balance of MMP9/TIMP1. Acta Pharmacol. Sin. 41(12), 1547–1556. https://doi.org/10.1038/s41401-020-0409-3 (2020).
Jiao-Yan, Y. et al. Oxymatrine improves blood-brain barrier integrity after cerebral ischemia-reperfusion injury by downregulating CAV1 and MMP9 expression. Phytomedicine. 84, 153505. https://doi.org/10.1016/j.phymed.2021.153505 (2021).
Huang, C. K. et al. Lgr4 governs a pro-inflammatory program in macrophages to antagonize post-infarction cardiac repair. Circ. Res. 127(8), 953–973. https://doi.org/10.1161/CIRCRESAHA.119.315807 (2020).
Alfonso-Jaume, M. A. et al. Cardiac ischemia-reperfusion injury induces matrix metalloproteinase-2 expression through the AP-1 components FosB and JunB. Am. J. Physiol. Heart Circ. Physiol. 291(4), H1838–H1846. https://doi.org/10.1152/ajpheart.00026.2006 (2006).
Bultot, L. et al. AMP-activated protein kinase phosphorylates and inactivates liver glycogen synthase. Biochem. J. 443(1), 193–203. https://doi.org/10.1042/BJ20112026 (2012).
Chen, H. F., Chuang, H. C. & Tan, T. H. Regulation of dual-specificity phosphatase (DUSP) ubiquitination and protein stability. Int. J. Mol. Sci. 20(11), 2668. https://doi.org/10.3390/ijms20112668 (2019).
Kucharska, A., Rushworth, L. K., Staples, C., Morrice, N. A. & Keyse, S. M. Regulation of the inducible nuclear dual-specificity phosphatase DUSP5 by ERK MAPK. Cell Signal. 21(12), 1794–1805. https://doi.org/10.1016/j.cellsig.2009.07.015 (2009).
Silverman, H. A., Chen, A., Kravatz, N. L., Chavan, S. S. & Chang, E. H. Involvement of neural transient receptor potential channels in peripheral inflammation. Front. Immunol. 23(11), 590261. https://doi.org/10.3389/fimmu.2020.590261 (2020).
Miller, B. A. & Zhang, W. TRP channels as mediators of oxidative stress. Adv. Exp. Med. Biol. 704, 531–544. https://doi.org/10.1007/978-94-007-0265-3_29 (2011).
Gérard, A., van der Kammen, R. A., Janssen, H., Ellenbroek, S. I. & Collard, J. G. The Rac activator Tiam1 controls efficient T-cell trafficking and route of transendothelial migration. Blood. 113(24), 6138–6147. https://doi.org/10.1182/blood-2008-07-167668 (2009).
Qiao, E., Huang, Z. & Wang, W. Exploring potential genes and pathways related to calcific aortic valve disease. Gene. 15(808), 145987. https://doi.org/10.1016/j.gene.2021.145987 (2022).
Högberg, C. et al. Succinate independently stimulates full platelet activation via cAMP and phosphoinositide 3-kinase-β signaling. J. Thromb. Haemost. 9(2), 361–372. https://doi.org/10.1111/j.1538-7836.2010.04158.x (2011).
Barry, S. P. et al. Enhanced IL-17 signalling following myocardial ischaemia/reperfusion injury. Int. J. Cardiol. 163(3), 326–334. https://doi.org/10.1016/j.ijcard.2011.08.849 (2013).
Zhang, A. et al. Necrostatin-1 inhibits Hmgb1-IL-23/IL-17 pathway and attenuates cardiac ischemia reperfusion injury. Transpl. Int. 27(10), 1077–1085. https://doi.org/10.1111/tri.12349 (2014).
Chen, M., Yu, L., Liu, Q., Jiang, H. & Zhou, S. Interleukin-17 inhibition: An important target for attenuating myocardial ischemia and reperfusion injury. Int. J. Cardiol. 1(198), 89–90. https://doi.org/10.1016/j.ijcard.2015.06.152 (2015).
Hu, X., Zhang, K., Chen, Z., Jiang, H. & Xu, W. The HMGB1-IL-17A axis contributes to hypoxia/reoxygenation injury via regulation of cardiomyocyte apoptosis and autophagy. Mol. Med. Rep. 17(1), 336–341. https://doi.org/10.3892/mmr.2017.7839 (2018).
Li, Q., Zhang, H. & Liu, X. Didymin alleviates cerebral ischemia-reperfusion injury by activating the PPAR signaling pathway. Yonsei Med. J. 63(10), 956–965. https://doi.org/10.3349/ymj.2022.0040 (2022).
Kuo, M. Y. et al. Ellagic acid inhibits oxidized low-density lipoprotein (OxLDL)-induced metalloproteinase (MMP) expression by modulating the protein kinase C-α/extracellular signal-regulated kinase/peroxisome proliferator-activated receptor γ/nuclear factor-κB (PKC-α/ERK/PPAR-γ/NF-κB) signaling pathway in endothelial cells. J. Agric. Food Chem. 59(9), 5100–5108. https://doi.org/10.1021/jf1041867 (2011).
Lee, S. J., Park, S. S., Lee, U. S., Kim, W. J. & Moon, S. K. Signaling pathway for TNF-alpha-induced MMP-9 expression: mediation through p38 MAP kinase, and inhibition by anti-cancer molecule magnolol in human urinary bladder cancer 5637 cells. Int. Immunopharmacol. 8(13–14), 1821–1826. https://doi.org/10.1016/j.intimp.2008.08.018 (2008).
Li, W. et al. Astrocyte-derived TNF-α-activated platelets promote cerebral ischemia/reperfusion injury by regulating the RIP1/RIP3/AKT signaling pathway. Mol. Neurobiol. 59(9), 5734–5749. https://doi.org/10.1007/s12035-022-02942-z (2022).
Cai, J. et al. AMPK: The key to ischemia-reperfusion injury. J. Cell Physiol. 237(11), 4079–4096. https://doi.org/10.1002/jcp.30875 (2022).
Tang, C. et al. Palmatine protects against cerebral ischemia/reperfusion injury by activation of the AMPK/Nrf2 pathway. Oxid. Med. Cell Longev. 11(2021), 6660193. https://doi.org/10.1155/2021/6660193 (2021).
Qin, G. W., Lu, P., Peng, L. & Jiang, W. Ginsenoside Rb1 inhibits cardiomyocyte autophagy via PI3K/Akt/mTOR signaling pathway and reduces myocardial ischemia/reperfusion injury. Am. J. Chin. Med. 49(8), 1913–1927. https://doi.org/10.1142/S0192415X21500907 (2021).
Wang, M. et al. Methyl eugenol attenuates liver ischemia reperfusion injury via activating PI3K/Akt signaling. Int. Immunopharmacol. 99, 108023. https://doi.org/10.1016/j.intimp.2021.108023 (2021).
Yan, F., Zhang, J., Zhang, L. & Zheng, X. Mulberry anthocyanin extract regulates glucose metabolism by promotion of glycogen synthesis and reduction of gluconeogenesis in human HepG2 cells. Food Funct. 7(1), 425–433. https://doi.org/10.1039/c5fo00841g (2016).
Xu, D. et al. Orexin-A alleviates astrocytic apoptosis and inflammation via inhibiting OX1R-mediated NF-κB and MAPK signaling pathways in cerebral ischemia/reperfusion injury. Biochim. Biophys. Acta Mol. Basis Dis. 1867(11), 166230. https://doi.org/10.1016/j.bbadis.2021.166230 (2021).
**e, W. et al. HMGB1-triggered inflammation inhibition of notoginseng leaf triterpenes against cerebral ischemia and reperfusion injury via MAPK and NF-κB signaling pathways. Biomolecules. 9(10), 512. https://doi.org/10.3390/biom9100512 (2019).
Hof, T. et al. Transient receptor potential channels in cardiac health and disease. Nat. Rev. Cardiol. 16(6), 344–360. https://doi.org/10.1038/s41569-018-0145-2 (2019).
Earley, S. & Brayden, J. E. Transient receptor potential channels in the vasculature. Physiol. Rev. 95(2), 645–690. https://doi.org/10.1152/physrev.00026.2014 (2015).
Hua, H. T. et al. CXC chemokine expression and synthesis in skeletal muscle during ischemia/reperfusion. J. Vasc. Surg. 42(2), 337–343. https://doi.org/10.1016/j.jvs.2005.04.046 (2005).
Jo, N., Wu, G. S. & Rao, N. A. Upregulation of chemokine expression in the retinal vasculature in ischemia-reperfusion injury. Invest. Ophthalmol. Vis. Sci. 44(9), 4054–4060. https://doi.org/10.1167/iovs.02-1308 (2003).
Mellado, M., Rodríguez-Frade, J. M., Mañes, S. & Martínez-A, C. Chemokine signaling and functional responses: The role of receptor dimerization and TK pathway activation. Annu. Rev. Immunol. 19, 397–421. https://doi.org/10.1146/annurev.immunol.19.1.397 (2001).
Roberts, O. L. & Dart, C. cAMP signalling in the vasculature: the role of Epac (exchange protein directly activated by cAMP). Biochem. Soc. Trans. 42(1), 89–97. https://doi.org/10.1042/BST20130253 (2014).
Abcouwer, S. F. et al. Inflammatory resolution and vascular barrier restoration after retinal ischemia reperfusion injury. J. Neuroinflammation. 18(1), 186. https://doi.org/10.1186/s12974-021-02237-5 (2021).
Cai, C. et al. Empagliflozin attenuates cardiac microvascular ischemia/reperfusion through activating the AMPKα1/ULK1/FUNDC1/mitophagy pathway. Redox Biol. 52, 102288. https://doi.org/10.1016/j.redox.2022.102288 (2022).
**a, Y. et al. Adenosine A2a receptor regulates autophagy flux and apoptosis to alleviate ischemia-reperfusion injury via the cAMP/PKA signaling pathway. Front. Cardiovasc. Med. 29(9), 755619. https://doi.org/10.3389/fcvm.2022.755619 (2022).
Liu, Y. et al. Lidocaine improves cerebral ischemia-reperfusion injury in rats through cAMP/PKA signaling pathway. Exp. Ther. Med. 20(1), 495–499. https://doi.org/10.3892/etm.2020.8688 (2020).
Schlegel, N. & Waschke, J. cAMP with other signaling cues converges on Rac1 to stabilize the endothelial barrier-a signaling pathway compromised in inflammation. Cell Tissue Res. 355(3), 587–596. https://doi.org/10.1007/s00441-013-1755-y (2014).
El-Mokadem, B. M., El-Abhar, H. S., Abdallah, D. M., Awad, A. S. & Soubh, A. A. Epac-1/Rap-1 signaling pathway orchestrates the reno-therapeutic effect of ticagrelor against renal ischemia/reperfusion model. Biomed. Pharmacother. 139, 111488. https://doi.org/10.1016/j.biopha.2021.111488 (2021).
Coucha, M. et al. Nox4 contributes to the hypoxia-mediated regulation of actin cytoskeleton in cerebrovascular smooth muscle. Life Sci. 15(163), 46–54. https://doi.org/10.1016/j.lfs.2016.08.018 (2016).
Connolly, B. A., Rice, J., Feig, L. A. & Buchsbaum, R. J. Tiam1-IRSp53 complex formation directs specificity of rac-mediated actin cytoskeleton regulation. Mol. Cell Biol. 25(11), 4602–4614. https://doi.org/10.1128/MCB.25.11.4602-4614.2005 (2005).
Sander, E. E. et al. Matrix-dependent Tiam1/Rac signaling in epithelial cells promotes either cell-cell adhesion or cell migration and is regulated by phosphatidylinositol 3-kinase. J. Cell Biol. 143(5), 1385–1398. https://doi.org/10.1083/jcb.143.5.1385 (1998).
Bavarsad, K. et al. Protective effects of curcumin against ischemia-reperfusion injury in the liver. Pharmacol. Res. 141, 53–62. https://doi.org/10.1016/j.phrs.2018.12.014 (2019).
Chen, Y. F., Wu, K. J., Siao, L. R. & Tsai, H. Y. Trilinolein, a natural triacylglycerol, protects cerebral ischemia through Inhibition of neuronal apoptosis and ameliorates intimal hyperplasia via attenuation of migration and modulation of matrix metalloproteinase-2 and RAS/MEK/ERK signaling pathway in VSMCs. Int. J. Mol. Sci. 23(21), 12820. https://doi.org/10.3390/ijms232112820 (2022).
Love, M. I., Huber, W. & Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 15(12), 550. https://doi.org/10.1186/s13059-014-0550-8 (2014).
McCarthy, D. J., Chen, Y. & Smyth, G. K. Differential expression analysis of multifactor RNA-Seq experiments with respect to biological variation. Nucleic Acids Res. 40(10), 4288–4297. https://doi.org/10.1093/nar/gks042 (2012).
Li, J. et al. Hiplot: A comprehensive and easy-to-use web service for boosting publication-ready biomedical data visualization. Brief Bioinform. 23(4), bbac261. https://doi.org/10.1093/bib/bbac261 (2022).
Shen, W. et al. Sangerbox: A comprehensive, interaction-friendly clinical bioinformatics analysis platform. iMeta 1(3), e36. https://doi.org/10.1002/imt2.36 (2022).
Funding
This study was supported by funding from the Yunnan Provincial Science and Technology Department Science and Technology Project, The First Affiliated Hospital of Kunming Medical University (Grant No. 202001AY070001-212 and 202301AY070001-009). The Yunnan Provincial Education Department Scientific Research Fund, the Third Affiliated Hospital of Kunming Medical University, Yunnan Cancer Center (Grant No. 2023Y0654), the Scientific Research Foundation of Education Department (Grant No. 2022Y219).
Author information
Authors and Affiliations
Contributions
N.Q.L., H.M.L. and W.H.C. confirm the authenticity of all the raw data. N.Q.L. and H.M.L. participated in the design of the study, and were responsible for collecting and interpreting data, performing the bioinformatics analysis, visualizing the presentation, and drafting and revising the original manuscript. H.Y. collected the data, performed the bioinformatics analysis and drafted the original manuscript. X.K.L. and X.J. participated in data curation, confirmed and analyzed the data. H.M.L., X.K.L., X.J. and W.H.C. provided funding support. Y.T.L., S.Y.T. and Y.H.L. participated in data curation. W.H.C. mainly provided the research conceptualization and funding support, supervised and assisted in designing the study, and participated in the revision of the manuscript. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Liu, N., Liang, H., Hong, Y. et al. Gallic acid pretreatment mitigates parathyroid ischemia–reperfusion injury through signaling pathway modulation. Sci Rep 14, 12971 (2024). https://doi.org/10.1038/s41598-024-63470-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-63470-5
- Springer Nature Limited