Abstract
Besides its metabolic and endocrine effects, growth hormone (GH)-releasing hormone (GHRH) is involved in the modulation of inflammation. Recently synthetized GHRH antagonist MIA-690 and MR-409, GHRH agonist, developed by us have shown potent pharmacological effects in various experimental paradigms. However, whether their administration modify resistance to chronic inflammatory stimuli in colon is still unknown. Ex vivo results demonstrated that MIA-690 and MR-409 inhibited production of pro-inflammatory and oxidative markers induced by lipopolysaccharide on isolated mouse colon specimens. In vivo, both MIA-690 and MR-409 have also been able to decrease the responsiveness to nociceptive stimulus, in hot plate test. Additionally, both peptides also induced a decreased sensitivity to acute and persistent inflammatory stimuli in male mice, in formalin test and dextran sodium sulfate (DSS)-induced colitis model, respectively. MIA-690 and MR-409 attenuate DSS-induced colitis with particular regard to clinical manifestations, histopathological damage and release of pro-inflammatory and oxidative markers in colon specimens. Respect to MR-409, MIA-690 showed higher efficacy in inhibiting prostaglandin (PG)E2, 8-iso-PGF2α and serotonin (5-HT) levels, as well as tumor necrosis factor (TNF)-α, interleukin (IL)-6 and nitric oxide synthase gene expression in colon specimens of DSS-induced colitis. Furthermore, MIA-690 decreased serum insulin-like growth factor (IGF)-1 levels in mice DSS-treated, respect to MR-409. Thus, our findings highlight the protective effects of MIA-690 and MR-409 on inflammation stimuli. The higher antinflammatory and antioxidant activities observed with MIA-690 could be related to decreased serum IGF-1 levels.
Similar content being viewed by others
Introduction
The hypothalamic peptide growth hormone-releasing hormone (GHRH) stimulates the production and secretion of growth hormone (GH) by binding to pituitary type GHRH receptor (GHRH-R)1. GHRH also exerts direct extrapituitary activities2,3, such as cardioprotection4,5, regeneration of pancreatic islets6, wound healing7, as well as survival and antiapoptotic effects8,9. In addition, GHRH acts as an autocrine and/or paracrine growth factor in normal non-neoplastic cells and in cancers through the involvement of GHRH-R and its splice variant type 1 (SV1)1,2,3,10,11,63.
In vivo studies
After 2-week acclimation, mice were treated daily by subcutaneous (s.c.) administration of 0.1 ml solution of GHRH antagonist MIA 690 (5 µg), GHRH agonist MR 409 (5 µg) or vehicle20. All solutions were freshly prepared before use. The concentrations were selected based on previous studies19,20. All treatments were administered at 09:00 a.m., and all in vivo testings were performed between 10:00 a.m. and 12:00 a.m. to minimize circadian variations in sensitivity to pain64. Care was taken to standardize testing conditions65. The experimental room was maintained with minimal background noise and constant temperature (22 ± 2 °C). All materials used for each test were thoroughly cleaned after test completion for each mouse. At the end of each test, the animals were returned to their home cages, and the apparatus was cleaned with 75% ethanol and dried before the next procedure. Antinociceptive and antinflammation testing was performed at 2 and 4 weeks after the first injection. Each test was conducted on the same group of animals (n = 6 for each group of treatment), after a 2-week rest period to avoid any interference on behavioral test performance, as previously reported66.
Hot plate test
Basal responsiveness to nociceptive stimulation was measured by hot-plate apparatus (2biological Instruments, Varese, Italy), set at the temperature of 54.0 ± 0.4 °C, as previously described31. The antinociceptive response was the latency from placement of the mouse on the heated surface until the first overt behavioral sign of nociception, such as (i) licking a hind paw, (ii) vocalization, or (iii) an escape attempt (jum** off the plate). The timer was stopped by a foot-operated pedal and the mouse was immediately removed from the hot-plate immediately after responding or after a maximum of 30 s (cut-off), to prevent tissue damage. In our conditions, the baseline latencies obtained in pre-experimental tests, ranged from 5.1 ± 0.7 to 6.2 ± 0.8 s. The analgesic effect was calculated as a percentage of the maximum possible effect (%M.P.E.) according to the formula: (TL-BL)/(30-BL) × 100, where TL = test latency, BL = baseline latency, 30 = cut-off time in seconds.
Formalin test
A diluted formalin solution was injected subcutaneously under the plantar surface of a hind paw, and pain related behaviors were scored during two successive phases31. The first phase (0–5 min.) reflects direct activation of nociceptors and therefore provides a measure of acute chemical pain. The second phase (20–60 min) mainly reflects persistent pain that is associated with develo** inflammatory response within the injected paw. Each mouse was placed in a transparent Plexiglas box (17.5 × 23.5 × 9.5 cm) positioned above a mirror to allow an unobstructed view of the paw. After a 15-min habituation period, formalin (10 μl of a 3% solution in saline) was injected under the plantar surface of the right hind paw, using a 50 μl Hamilton microsyringe with a 25-gauge needle. The mouse was placed back into the box immediately after the injection and behavioral scoring consisted of either counting the number of nociceptive responses (paw licking, shaking and biting) or measuring how long the animal produced these responses.
DSS-induced colitis
Male mice were randomized into three groups and treated daily for 7 days. Colitis was induced by 2.5% (w/v) DSS (molecular weight 40 kDa; Sigma Aldrich, Steinheim, Germany) added to the drinking water, ad libitum for 7 days31. C57BL/6 (n = 6) mice untreated with DSS were used as positive control.
Colitis DAI analysis
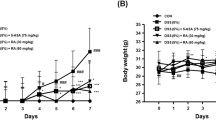
Colitis DAI scoring was calculated as previously described67. DAI score was the combined score of weight loss (0, none; 1, 0–5%; 2, 5–10%; 3, 10–20%; and 4, > 20%), stool consistency change (0, none; 2, loose stool; and 4, diarrhea), and bleeding (0, none; 1, trace; 2, mild hemoccult; 3, obvious hemoccult; and 4, gross bleeding), and then divided by three. The minimal score was 0 and the maximal score was 4. The animals were scored for the DAI at the same time of each day, and DAI score was recorded every day. Animals were treated with anesthetic and analgesic drugs [caprofen 10 mg/kg; meloxicam 10 mg/kg; lidocaine (1–2%) 2–4 mg/kg] when they displayed signs of distress, according to the guidelines suggested by the ‘National Centre for the Replacement, Refinement and Reduction of Animals in Research’ (NC3RS).
Macroscopic and histological evaluation
Mice were sacrificed by CO2 inhalation (100% CO2) at a flow rate of 20% of the chamber volume per min), individual colon was dissected and the colon segment length (from ileocecal junction to the anal verge; mm) measured by a ruler. Tissues were fixed in 10% phosphate-buffered formalin, dehydrated in a series of alcohol solutions of 50%, 70%, 95% and 99% and then in xylene. Samples were then paraffin-embedded and cut in 5 μm-thick sections. Sections were de-waxed (xylene and alcohol in progressively lower concentrations), rehydrated and processed for Hematoxylin and Eosin (H&E) staining (Bio Optica, Milano, Italy) according to the manufacturer protocol.
H&E-stained 5 mm distal colonic sections were coded for blind microscopic assessment of inflammation. Samples were then observed by means of Leica DM 4000 microscope (Leica Cambridge Ltd, Cambridge, UK) equipped with a Leica DFC 320 camera (Leica Cambridge Ltd.) for computerized images.
PGE2 and 8-iso-PGF2α production in isolated colon specimens
PGE2 and 8-iso-PGF2α levels (ng/mg wet tissue) in isolated colon specimens of mice treated with MIA-690 (5 µg) andMR-409 (5 µg) were evaluated by radioimmunoassay (RIA), as previously reported31. Colon specimens dissected from C57BL/6 (n = 6) mice untreated with DSS were used as positive control.
5-HT and high performance liquid chromatography (HPLC) determination
Tissue 5-HT levels were analyzed through an HPLC apparatus consisting of a Jasco (Tokyo, Japan) PU-2080 chromatographic pump and an ESA (Chelmsford, MA, USA) Coulochem III coulometric detector, equipped with microdialysis cell (ESA-5014b) porous graphite working electrode and solid-state palladium reference electrode. The analytical conditions for identification and quantification were selected according to a previous study. Briefly, the analytical cell was set at -0.150 V, for detector 1 and at + 0.300 V for detector 2, with a range of 100 nA. The chromatograms were monitored at the analytical detector 2. Integration was performed by Jasco Borwin Chromatography software, version 1.5. The chromatographic separation was performed by isocratic elution on Phenomenex Kinetex reverse phase column (C18, 150 mm × 4.6 mm i.d., 2.6 µm). As regards separation of 5-HT, the mobile phase was (10:90 v/v) acetonitrile and 75 mM pH 3.00 phosphate buffer containing octanesulfonic acid 1.8 mM, EDTA 30 µm and triethylamine 0.015% v/v. Flow rate was 0.6 ml/min and the samples were manually injected through a 20 µl loop. Analyte peaks were identified by comparison with the retention time of pure standard. Analyte concentrations in the samples were calculated by linear regression curve (y = bx + m) obtained with standard. The standard stock solution of 5-HT at 2 mg/ml was prepared in bidistilled water containing 0.004% EDTA and 0.001% sodium bisulfite. The stock solutions were stored at 4 °C. Work solutions (1.25–20.00 ng/ml) were obtained by progressively diluting the stock solutions in the mobile phase.
KA and HPLC-Fluorimetric Determination
The KA quantitative determination in the tissue was carried out a reversed phase HPLC-fluorimeter in agreement with the method employed by Pocivavsek and colleagues. Analyses were performed by using a liquid chromatograph (MOD. 1525, Waters Corporation, Milford MA, USA) equipped with a fluorimetric detector (MOD, 2475, Waters Corporation), a C18 reversed-phase column (Acclaim 120,3 µm, 2.1 × 100 mm, Dionex Corporation Sunnyvale, CA, USA), and an on-line degasser (Biotech 4-CH degasi compact, LabService, Anzola, Italy). The separation was conducted in isocratic conditions and the mobile phase consisted of 250 mM zinc acetate, 50 mM sodium acetate, and 3% aceto nitrile (pH adjusted to 6.2 with glacial acetic acid), using a flow rate of 1.0 mL/min. In the eluate, the KA was identified and measured fluorimetrically (excitation: 344 nm; emission: 120 nm).
RNA extraction, reverse transcription and real-time reverse transcription polymerase chain reaction (real-time RT PCR)
Colon tissue was rapidly removed, dissected and stored in RNAlater solution (Ambion, Austin, TX) at -20 °C until further processed as previously described. Gene expression of TNF-α, IL-6 and iNOS was determined by quantitative real-time PCR using TaqMan probe-based chemistry (Applied Biosystems, Foster City, CA, USA). PCR primers and TaqMan probes were obtained from Applied Biosystems (Assays-on-Demand Gene Expression Products, Mm00443258_m1 for TNF-α gene, Mm00446190_m1 for IL-6 gene, Mm00440502_m1 for iNOS gene, Mm00607939_s1 for β-actin gene. β-actin was used as the housekee** gene. Gene expression data were calculated as previously reported63.
IGF-1 Analysis
Blood sample (1 ml) collection was performed through cardiac puncture in mice. Serum, obtained by centrifugation of total blood at 450 g at 4 °C for 15 min, was stored at − 80 °C until analysis. IGF-I were measured using mouse IGF-I ELISA Kit (Abcam, cod: ab100695), following the manufacturers’ instructions. Results were assessed by colorimetric detection at 450 nm absorbance using LT-4000 microplate reader (Euroclone).
Statistical analysis
Statistical analysis was performed using GraphPad Prism version 5.01 for Windows (GraphPad Software, San Diego, CA, USA). All data were collected from each of the animals used in the experimental procedure and means ± SEM were determined for each experimental group and analyzed by two-way analysis of variance (ANOVA) followed by Bonferroni post-hoc test. F values are referring to repeated measure 2-way ANOVA. As for gene expression analysis, 1.00 (calibrator sample) was considered the theoretical mean for the comparison. Statistical significance was accepted at p < 0.05. As regards gene expression analysis, the comparative 2-ΔΔCt method was used to quantify the relative abundance of mRNA and then to determine the relative changes in individual gene expression (relative quantification)63. Number of animals randomized for each experimental group was calculated on the basis of the ‘Resource Equation’ N = (E + T)/T (10 ≤ E ≤ 20)68, according to the guidelines suggested by the ‘National Centre for the Replacement, Refinement and Reduction of Animals in Research’ (NC3RS) and reported on the following web site: https://www.nc3rs.org.uk/experimental-designstatistics.
References
Kiaris, H., Chatzistamou, I., Papavassiliou, A. G. & Schally, A. V. Growth hormone releasing hormone: Not only a neurohormone. Trends Endocrinol. Metab. 22, 311–317 (2011).
Schally, A. V. et al. Actions and potential therapeutic applications of growth hormone-releasing hormone agonists. Endocrinology 160, 1600–1612 (2019).
Granata, R. Peripheral activities of growth hormone-releasing hormone. J. Endocrinol. Invest. 39, 721–727 (2016).
Kanashiro-Takeuchi, R. M. et al. Cardioprotective effects of growth hormone-releasing hormone agonist after myocardial infarction. Proc. Natl. Acad. Sci. USA 107, 2604–2609 (2010).
Gesmundo, I. et al. Growth hormone-releasing hormone attenuates cardiac hypertrophy and improves heart function in pressure overload-induced heart failure. Proc. Natl. Acad. Sci. USA 114, 12033–12038 (2017).
Zhang, X. et al. Beneficial effects of growth hormone-releasing hormone agonists on rat INS-1 cells and on streptozotocin-induced NOD/SCID mice. Proc. Natl. Acad. Sci USA 112, 13651–13656 (2015).
Cui, T. et al. Agonistic analogs of growth hormone releasing hormone (GHRH) promote wound healing by stimulating the proliferation and survival of human dermal fibroblasts through ERK and AKT pathways. Oncotarget 7, 52661–52672 (2016).
Gallo, D. et al. GH-releasing hormone promotes survival and prevents TNFα-induced apoptosis and atrophy in C2C12 myotubes. Endocrinology 156, 3239–3252 (2015).
Granata, R. et al. Growth hormone-releasing hormone promotes survival of cardiac myocytes in vitro and protects against ischaemia-reperfusion injury in rat heart. Cardiovasc. Res. 83, 303–312 (2009).
Kiaris, H., Schally, A. V., Varga, J. L., Groot, K. & Armatis, P. Growth hormone-releasing hormone: an autocrine growth factor for small cell lung carcinoma. Proc. Natl. Acad. Sci. USA 96, 14894–14898 (1999).
Barabutis, N. & Schally, A. V. Growth hormone-releasing hormone: extrapituitary effects in physiology and pathology. Cell Cycle 9, 4110–4116 (2010).
**ong, X. et al. Splice variant of growth hormone-releasing hormone receptor drives esophageal squamous cell carcinoma conferring a therapeutic target. Proc. Natl. Acad. Sci. USA 117, 6726–6732 (2020).
Zarandi, M. et al. Synthesis and biological activities of highly potent antagonists of growth hormone-releasing hormone. Proc. Natl. Acad. Sci. USA 91, 12298–12302 (1994).
Izdebski, J. et al. Synthesis and biological evaluation of superactive agonists of growth hormone-releasing hormone. Proc. Natl. Acad. Sci. USA 92, 4872–4876 (1995).
Varga, J. L. et al. Increased activity of antagonists of growth hormone-releasing hormone substituted at positions 8, 9, and 10. Proc. Natl. Acad. Sci. USA 101, 1708–1713 (2004).
Schally, A. V., Varga, J. L. & Engel, J. B. Antagonists of growth-hormone-releasing hormone: an emerging new therapy for cancer. Nat. Clin. Pract. Endocrinol. Metab. 4, 33–43 (2008).
Cai, R. et al. Synthesis of new potent agonistic analogs of growth hormone-releasing hormone (GHRH) and evaluation of their endocrine and cardiac activities. Peptides 52, 104–112 (2014).
Zarandi, M. et al. Synthesis and structure-activity studies on novel analogs of human growth hormone releasing hormone (GHRH) with enhanced inhibitory activities on tumor growth. Peptides 89, 60–70 (2017).
Schally, A. V. et al. Agonists of growth hormone-releasing hormone (GHRH) inhibit human experimental cancers in vivo by down-regulating receptors for GHRH. Proc. Natl. Acad. Sci. USA 115, 12028–12033 (2018).
Villanova, T. et al. Antagonists of growth hormone-releasing hormone (GHRH) inhibit the growth of human malignant pleural mesothelioma. Proc. Natl. Acad. Sci. USA 116, 2226–2231 (2019).
Barabutis, N., Akhter, M. S., Uddin, M. A., Kubra, K. T. & Schally, A. V. GHRH antagonists protect against hydrogen peroxide-induced breakdown of brain microvascular endothelium integrity. Horm. Metab. Res. 52, 336–339 (2020).
Barabutis, N. & Schally, A. V. Antioxidant activity of growth hormone-releasing hormone antagonists in LNCaP human prostate cancer line. Proc. Natl. Acad. Sci. USA 105, 20470–20475 (2008).
Barabutis, N., Schally, A. V. & Siejka, A. P53, GHRH, inflammation and cancer. EBioMedicine 37, 557–562 (2018).
Yong, J. Q. et al. Antagonist of GH-releasing hormone receptors alleviates experimental ocular inflammation. Proc. Natl. Acad. Sci. USA 111, 18303–18308 (2014).
Jaszberenyi, M. et al. Beneficial effects of novel antagonists of GHRH in different models of Alzheimer’s disease. Aging (Albany NY) 4, 755–767 (2012).
Recinella, L. et al. Antinflammatory, antioxidant, and behavioral effects induced by administration of growth hormone-releasing hormone analogs in mice. Sci. Rep. 10, 4850 (2020).
Thounaojam, M. C. et al. Protective effects of agonists of growth hormone-releasing hormone (GHRH) in early experimental diabetic retinopathy. Proc. Natl. Acad. Sci. USA 114, 13248–13253 (2017).
Lathe, R. Hormones and the hippocampus. J. Endocrinol. 169, 205–231 (2001).
Olsen, J. et al. Intimate associations between the endogenous opiate systems and the growth hormone-releasing hormone system in the human hypothalamus. Neuroscience 258, 238–245 (2014).
Codd, E. E., Yellin, T. & Walker, R. F. Binding of growth hormone-releasing hormones and enkephalin-derived growth hormone-releasing peptides to mu and delta opioid receptors in forebrain of rat. Neuropharmacology 27, 1019–1025 (1988).
Leone, S. et al. Increased pain and inflammatory sensitivity in growth hormone-releasing hormone (GHRH) knockout mice. Prostaglandins Other Lipid Mediat. 144, 106362 (2019).
Corsi, M. M. et al. The effect of somatostatin on experimental inflammation in rats. Anesth. Analg. 85, 1112–1115 (1997).
Chrubasik, J. et al. Somatostatin, a potent analgesic. Lancet 2, 1208–1209 (1984).
Perez, R. et al. Antagonists of growth hormone-releasing hormone suppress in vivo tumor growth and gene expression in triple negative breast cancers. Oncotarget 3, 988–997 (2012).
Popovics, P., Cai, R., Sha, W., Rick, F. G. & Schally, A. V. Growth hormone-releasing hormone antagonists reduce prostatic enlargement and inflammation in carrageenan-induced chronic prostatitis. Prostate 78, 970–980 (2018).
Liang, W. C. et al. Signaling mechanisms of growth hormone-releasing hormone receptor in LPS-induced acute ocular inflammation. Proc. Natl. Acad. Sci. USA 117, 6067–6074 (2020).
Talhouk, R. S., Saadé, N. E., Mouneimne, G., Masaad, C. A. & Safieh-Garabedian, B. Growth hormone releasing hormone reverses endotoxin-induced localized inflammatory hyperalgesia without reducing the upregulated cytokines, nerve growth factor and gelatinase activity. Prog. Neuropsychopharmacol. Biol. Psychiatry. 28, 625–631 (2004).
Ren, J. L. et al. Growth hormone-releasing hormone receptor mediates cytokine production in ciliary and iris epithelial cells during LPS-induced ocular inflammation. Exp. Eye Res. 181, 277–284 (2019).
Coates, M. D. et al. Molecular defects in mucosal serotonin content and decreased serotonin reuptake transporter in ulcerative colitis and irritable bowel syndrome. Gastroenterology 126, 1657–1664 (2004).
Minderhoud, I. M., Oldenburg, B., Schipper, M. E. I., ter Linde, J. J. M. & Samsom, M. Serotonin synthesis and uptake in symptomatic patients with Crohn’s disease in remission. Clin. Gastroenterol. Hepatol. 5, 714–720 (2007).
Stoyanova, I. I. & Gulubova, M. V. Mast cells and inflammatory mediators in chronic ulcerative colitis. Acta Histochem. 104, 185–192 (2002).
Bearcroft, C. P., Perrett, D. & Farthing, M. J. G. Postprandial plasma 5-hydroxytryptamine in diarrhoea predominant irritable bowel syndrome: a pilot study. Gut 42, 42–46 (1998).
Spiller, R. C. et al. Increased rectal mucosal enteroendocrine cells, T lymphocytes, and increased gut permeability following acute Campylobacter enteritis and in post-dysenteric irritable bowel syndrome. Gut 47, 804–811 (2000).
Chen, M. et al. Serotonin-exacerbated DSS-induced colitis is associated with increase in MMP-3 and MMP-9 expression in the mouse colon. Mediators Inflamm. 2016, 5359768 (2016).
Raab, Y., Hällgren, R. & Gerdin, B. Enhanced intestinal synthesis of interleukin-6 is related to the disease severity and activity in ulcerative colitis. Digestion 55, 44–49 (1994).
Schürmann, G., Betzler, M., Post, S., Herfarth, C. & Meuer, S. Soluble interleukin-2 receptor, interleukin-6 and interleukin-1 beta in patients with Crohn’s disease and ulcerative colitis: preoperative levels and postoperative changes of serum concentrations. Digestion 51, 51–59 (1992).
Wang, S., Zhou, T., Zhai, J. P., Wang, L. H. & Chen, J. Effects of Modified Sanhuang Decoction enema on serum tumor necrosis factor-α and colonic mucosa interleukin-1β, interleukin-6 levels in ulcerative colitis rats. Chin. J. Integr. Med. 20, 865–869 (2014).
Lee, M. J. et al. Interleukin-6 induces S100A9 expression in colonic epithelial cells through STAT3 activation in experimental ulcerative colitis. PLoS ONE 7, e38801 (2012).
Mudter, J. & Neurath, M. F. Il-6 signaling in inflammatory bowel disease: pathophysiological role and clinical relevance. Inflamm. Bowel Dis. 13, 1016–1023 (2007).
Mourkioti, F. & Rosenthal, N. IGF-1, inflammation and stem cells: interactions during muscle regeneration. Trends Immunol. 26, 535–542 (2005).
Sanchez-Lopez, E. et al. Targeting colorectal cancer via its microenvironment by inhibiting IGF-1 receptor-insulin receptor substrate and STAT3 signaling. Oncogene 35, 2634–2644 (2016).
Pollak, M. N., Schernhammer, E. S. & Hankinson, S. E. Insulin-like growth factors and neoplasia. Nat. Rev. Cancer. 4, 505–518 (2004).
Clayton, P. E., Banerjee, I., Murray, P. G. & Renehan, A. G. Growth hormone, the insulin-like growth factor axis, insulin and cancer risk. Nat. Rev. Endocrinol. 7, 11–24 (2011).
Vigneri, P. G. et al. The insulin/IGF system in colorectal cancer development and resistance to therapy. Front. Oncol. 5, 230 (2015).
Spadaro, O. et al. IGF1 shapes macrophage activation in response to immunometabolic challenge. Cell Rep. 19, 225–234 (2017).
Cui, T. & Schally, A. V. Growth hormone-releasing hormone (GHRH) and its agonists inhibit hepatic and tumoral secretion of IGF-1. Oncotarget. 9, 28745–28756 (2018).
Qin, Y. J. et al. Antagonist of GH-releasing hormone receptors alleviates experimental ocular inflammation. Proc. Natl. Acad. Sci. USA 111, 18303–18308 (2014).
Kanashiro-Takeuchi, R. M. et al. Cardioprotective effects of growth hormone-releasing hormone agonist after myocardial infarction. Proc. Natl. Acad. Sci. USA 107, 2604–2609 (2010).
Kanashiro-Takeuchi, R. M. et al. Activation of growth hormone releasing hormone (GHRH) receptor stimulates cardiac reverse remodeling after myocardial infarction (MI). Proc. Natl. Acad. Sci. USA 109, 559–563 (2012).
Recinella, L. et al. Protective effects induced by two polyphenolic liquid complexes from olive (Olea europaea, mainly Cultivar Coratina) pressing juice in rat isolated tissues challenged with LPS. Molecules 24, 3002 (2019).
Leone, S. et al. Increased locomotor and thermogenic activity in mice with targeted ablation of the GHRH gene. Growth Horm. IGF Res. 25, 80–84 (2015).
Recinella, L. et al. Effects of isolated GH deficiency on adipose tissue, feeding and adipokines in mice. Growth Horm. IGF Res. 23, 237–242 (2013).
Livak, K. J. & Schmittgen, T. D. Analysis of relative gene expression data using real- time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25, 402–408 (2001).
Konecka, A. M. & Sroczynska, I. Circadian rhythm of pain in male mice. Gen. Pharmacol. 31, 809–810 (1998).
Wilson, S. G. & Mogil, J. S. Measuring pain in the (knockout) mouse: big challenges in a small mammal. Behav. Brain Res. 125, 65–73 (2001).
Leone, S. et al. Behavioural phenoty** of male growth hormone-releasing hormone (GHRH) knockout mice. Growth Horm. IGF Res. 24, 192–197 (2014).
Yu, C. et al. American ginseng attenuates azoxymethane/dextran sodium sulfate-induced colon carcinogenesis in mice. J. Ginseng Res. 39, 14–21 (2015).
Charan, J. & Kantharia, N. D. How to calculate sample size in animal studies?. J. Pharmacol. Pharmacother. 4, 303–306 (2013).
Acknowledgements
This work was supported by grants from the Italian Ministry of Education, University and Research (MIUR) (FFABR 2017 to S. Leone) and by funds of University “G. d’Annunzio” of Chieti-Pescara, Italy (FAR 2020 to L. Recinella, FAR 2019 to L. Brunetti and FAR 2019 to S. Leone). Work in Miami was supported by the Medical Research Service of the Department of Veterans Affairs and by the University of Miami Miller School of Medicine.
Author information
Authors and Affiliations
Contributions
L.R., A.C., L.B., A.V.S. and S.L. conceived and coordinated the study and wrote the paper. R.C., W.S., and A.V.S. contributed new reagents. L.R., A.C., V.D.V., S.V., G.O., C.F., I.G., R.G., R.L. and S.L. performed the experiments and analyzed the data. All authors reviewed the results and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
A.V.S. and R.C. work has been funded by Medical Research Service of the Department of Veterans Affairs and by the University of Miami Miller School of Medicine. A.V.S. and R.C. are listed as co-inventors on patents for GHRH agonists and GHRH antagonists, assigned to the University of Miami, Miami, FL, and the Veterans Affairs Medical Center, Miami, FL. L.R., A.C., V.D.V., S.V., G.O., C.F., I.G., R.G., W.S., R.L., L.B. and S.L. declare no conflicts of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Recinella, L., Chiavaroli, A., Di Valerio, V. et al. Protective effects of growth hormone-releasing hormone analogs in DSS-induced colitis in mice. Sci Rep 11, 2530 (2021). https://doi.org/10.1038/s41598-021-81778-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-81778-4
- Springer Nature Limited