Abstract
Introduction
We investigated the efficiency of high mobility group box-1 protein (HMGB-1) in differentiation of asymptomatic knee prosthesis, and periprosthetic joint infection and aseptic loosening causing painful knee prosthesis.
Materials and Methods
The data of patients who consulted our clinic for checking after total knee arthroplasty surgery were recorded prospectively. Blood levels of CRP, ESR, WBC, and HMGB-1 were recorded. Patients whose examination and routine tests were within normal limits comprised group I, asymptomatic total knee arthroplasty (ATKA). Painful patients with abnormal test results underwent three phase bone scintigraphy for further investigation Patients with periprosthetic joint infection (PJI) and aseptic loosening (AL) according to scintigraphy comprised group II and group III, respectively. The mean values of HMGB-1 and cut-off values according to the groups and their correlations with other inflammatory parameters were determined.
Results
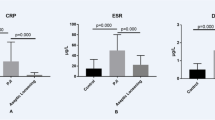
Seventy-three patients were included in the study. Significant differences were observed in three groups, in terms of CRP, ESR, WBC, and HMGB-1. The cut-off value of HMGB-1 was determined as 15.16 ng/ml between ATKA and PJI, 16.92 ng/ml between ATKA and AL, and 27.87 ng/ml between PJI and AL, respectively. Accordingly, the sensitivity, and specificity of HMGB-1 in differentiation of ATKA and PJI were 91%, 88%, and in differentiation of ATKA and AL were 91%, 96%, and in differentiation of PJI and AL were 81%, 73%, respectively.
Conclusion
HMGB-1 may be utilized as an additional blood test in the differential diagnosis of problematic knee prosthesis patients.




Similar content being viewed by others
References
Postler, A., Lützner, C., Beyer, F., Tille, E., & Lützner, J. (2018). Analysis of total knee arthroplasty revision causes. BMC Musculoskeletal Disorders, 19(1), 55. https://doi.org/10.1186/s12891-018-1977-y
Sharkey, P. F., Lichstein, P. M., Shen, C., Tokarski, A. T., & Parvizi, J. (2014). Why are total knee arthroplasties failing today–has anything changed after 10 years? The Journal of arthroplasty, 29(9), 1774–1778. https://doi.org/10.1016/j.arth.2013.07.024
Thiele, K., Perka, C., Matziolis, G., Mayr, H. O., Sostheim, M., & Hube, R. (2015). Current failure mechanisms after knee arthroplasty have changed: Polyethylene wear is less common in revision surgery. The Journal of Bone and Joint Surgery American, 97(9), 715–720. https://doi.org/10.2106/jbjs.M.01534
Dyrhovden, G. S., Lygre, S. H. L., Badawy, M., Gøthesen, Ø., & Furnes, O. (2017). Have the causes of revision for total and unicompartmental knee arthroplasties changed during the past two decades? Clinical orthopaedics and Related Research, 475(7), 1874–1886. https://doi.org/10.1007/s11999-017-5316-7
Lombardi, A. V., Jr., Berend, K. R., & Adams, J. B. (2014). Why knee replacements fail in 2013: Patient, surgeon, or implant? The Bone & Joint Journal, 96-b(11 Supple A), 101–104. https://doi.org/10.1302/0301-620x.96b11.34350
Claassen, L., Ettinger, M., Plaass, C., Daniilidis, K., Calliess, T., & Ezechieli, M. (2014). Diagnostic value of bone scintigraphy for aseptic loosening after total knee arthroplasty. Technology and Health Care: Official Journal of the European Society for Engineering and Medicine, 22(5), 767–773. https://doi.org/10.3233/thc-140850
Gehrke, T., Alijanipour, P., & Parvizi, J. (2015). The management of an infected total knee arthroplasty. The Bone & Joint Journal, 97-b(10 Suppl A), 20–29. https://doi.org/10.1302/0301-620x.97b10.36475
Niccoli, G., Mercurio, D., & Cortese, F. (2017). Bone scan in painful knee arthroplasty: Obsolete or actual examination? Acta Bio-medica: Atenei Parmensis, 88(2s), 68–77. https://doi.org/10.23750/abm.v88i2-S.6516
Li, C., Renz, N., Trampuz, A., & Ojeda-Thies, C. (2020). Twenty common errors in the diagnosis and treatment of periprosthetic joint infection. International Orthopaedics, 44(1), 3–14. https://doi.org/10.1007/s00264-019-04426-7
Palestro, C. J., & Love, C. (2017). Role of nuclear medicine for diagnosing infection of recently implanted lower extremity arthroplasties. Seminars in Nuclear Medicine, 47(6), 630–638. https://doi.org/10.1053/j.semnuclmed.2017.07.008
Renz, N., Müller, M., Perka, C., & Trampuz, A. (2016). Implant-associated infections - diagnostics. Der Chirurg; Zeitschrift fur alle Gebiete der operativen Medizen, 87(10), 813–821. https://doi.org/10.1007/s00104-016-0234-x
Abdel Karim, M., Andrawis, J., Bengoa, F., Bracho, C., Compagnoni, R., Cross, M., Danoff, J., Della Valle, C. J., Foguet, P., Fraguas, T., Gehrke, T., Goswami, K., Guerra, E., Ha, Y. C., Klaber, I., Komnos, G., Lachiewicz, P., Lausmann, C., Levine, B., … Zahar, A. (2019). Hip and knee section, diagnosis, algorithm: Proceedings of international consensus on orthopedic infections. The Journal of Arthroplasty, 34(2s), S339–S350. https://doi.org/10.1016/j.arth.2018.09.018
Yamada, S., & Maruyama, I. (2007). HMGB1, a novel inflammatory cytokine. Clinica Chimica Acta; International Journal of Clinical Chemistry, 375(1–2), 36–42. https://doi.org/10.1016/j.cca.2006.07.019
Kargı, A., Demirpençe, Ö., Gündüz, Ş, Göktaş, S., Alikanoǧlu, A. S., & Yıldırım, M. (2016). Serum levels of HMGB1 have a diagnostic role in metastatic renal cell cancer. Cancer Biomarkers: Section A of Disease Markers, 17(1), 17–20. https://doi.org/10.3233/cbm-160611
Venereau, E., De Leo, F., Mezzapelle, R., Careccia, G., Musco, G., & Bianchi, M. E. (2016). HMGB1 as biomarker and drug target. Pharmacological Research, 111, 534–544. https://doi.org/10.1016/j.phrs.2016.06.031
Sundén-Cullberg, J., Norrby-Teglund, A., Rouhiainen, A., Rauvala, H., Herman, G., Tracey, K. J., Lee, M. L., Andersson, J., Tokics, L., & Treutiger, C. J. (2005). Persistent elevation of high mobility group box-1 protein (HMGB1) in patients with severe sepsis and septic shock. Critical Care Medicine, 33(3), 564–573. https://doi.org/10.1097/01.ccm.0000155991.88802.4d
Roof, M. A., Kreinces, J. B., Schwarzkopf, R., Rozell, J. C., & Aggarwal, V. K. (2022). Are there avoidable causes of early revision total knee arthroplasty? Knee Surgery & Related Research, 34(1), 29. https://doi.org/10.1186/s43019-022-00157-z
Evangelopoulos, D. S., Ahmad, S. S., Krismer, A. M., Albers, C. E., Hoppe, S., Kleer, B., Kohl, S., & Ateschrang, A. (2019). Periprosthetic infection: Major cause of early failure of primary and revision total knee arthroplasty. The Journal of Knee Surgery, 32(10), 941–946. https://doi.org/10.1055/s-0038-1672203
Della Valle, C., Parvizi, J., Bauer, T. W., DiCesare, P. E., Evans, R. P., Segreti, J., Spangehl, M., Watters, W. C., 3rd., Keith, M., Turkelson, C. M., Wies, J. L., Sluka, P., & Hitchcock, K. (2011). American academy of orthopaedic surgeons clinical practice guideline on: The diagnosis of periprosthetic joint infections of the hip and knee. The Journal of Bone and Joint Surgery American, 93(14), 1355–1357. https://doi.org/10.2106/JBJS.9314ebo
Frangiamore, S. J., Siqueira, M. B., Saleh, A., Daly, T., Higuera, C. A., & Barsoum, W. K. (2016). Synovial cytokines and the MSIS criteria are not useful for determining infection resolution after periprosthetic joint infection explantation. Clinical Orthopaedics and Related Research, 474(7), 1630–1639. https://doi.org/10.1007/s11999-016-4710-x
Parvizi, J., Adeli, B., Zmistowski, B., Restrepo, C., & Greenwald, A. S. (2012). Management of periprosthetic joint infection: the current knowledge: AAOS exhibit selection. The Journal of Bone and Joint Surgery American, 94(14), e104. https://doi.org/10.2106/jbjs.K.01417
Jacovides, C. L., Parvizi, J., Adeli, B., & Jung, K. A. (2011). Molecular markers for diagnosis of periprosthetic joint infection. The Journal of Arthroplasty, 26(6 Suppl), 99-103.e101. https://doi.org/10.1016/j.arth.2011.03.025
Diaz-Ledezma, C., Higuera, C. A., & Parvizi, J. (2013). Success after treatment of periprosthetic joint infection: A Delphi-based international multidisciplinary consensus. Clinical Orthopaedics and Related Research, 471(7), 2374–2382. https://doi.org/10.1007/s11999-013-2866-1
Gollwitzer, H., Dombrowski, Y., Prodinger, P. M., Peric, M., Summer, B., Hapfelmeier, A., Saldamli, B., Pankow, F., von Eisenhart-Rothe, R., Imhoff, A. B., Schauber, J., Thomas, P., Burgkart, R., & Banke, I. J. (2013). Antimicrobial peptides and proinflammatory cytokines in periprosthetic joint infection. The Journal of Bone and Joint Surgery American, 95(7), 644–651. https://doi.org/10.2106/jbjs.L.00205
Nilsdotter-Augustinsson, A., Briheim, G., Herder, A., Ljunghusen, O., Wahlström, O., & Ohman, L. (2007). Inflammatory response in 85 patients with loosened hip prostheses: A prospective study comparing inflammatory markers in patients with aseptic and septic prosthetic loosening. Acta Orthopaedica, 78(5), 629–639. https://doi.org/10.1080/17453670710014329
Ong, J., Tang, A., Rozell, J. C., Babb, J. S., Schwarzkopf, R., & Lin, D. (2022). Factors predicting hip joint aspiration yield or “dry taps” in patients with total hip arthroplasty. Journal of Orthopaedic Surgery and Research, 17(1), 42. https://doi.org/10.1186/s13018-022-02942-8
Hassebrock, J. D., Fox, M. G., Spangehl, M. J., Neville, M. R., & Schwartz, A. J. (2019). What is the role of repeat aspiration in the diagnosis of periprosthetic hip infection? The Journal of arthroplasty, 34(1), 126–131. https://doi.org/10.1016/j.arth.2018.09.001
Love, C., Marwin, S. E., Tomas, M. B., Krauss, E. S., Tronco, G. G., Bhargava, K. K., Nichols, K. J., & Palestro, C. J. (2004). Diagnosing infection in the failed joint replacement: A comparison of coincidence detection 18F-FDG and 111In-labeled leukocyte/99mTc-sulfur colloid marrow imaging. Journal of Nuclear Medicine: Official publication, Society of Nuclear Medicine, 45(11), 1864–1871.
Lima, A. L., Oliveira, P. R., Carvalho, V. C., Saconi, E. S., Cabrita, H. B., & Rodrigues, M. B. (2013). Periprosthetic joint infections. Interdisciplinary Perspectives on Infectious Diseases, 2013, 542796. https://doi.org/10.1155/2013/542796
Stumpe, K. D., Nötzli, H. P., Zanetti, M., Kamel, E. M., Hany, T. F., Görres, G. W., von Schulthess, G. K., & Hodler, J. (2004). FDG PET for differentiation of infection and aseptic loosening in total hip replacements: Comparison with conventional radiography and three-phase bone scintigraphy. Radiology, 231(2), 333–341. https://doi.org/10.1148/radiol.2312021596
Rosenthall, L., Lepanto, L., & Raymond, F. (1987). Radiophosphate uptake in asymptomatic knee arthroplasty. Journal of Nuclear Medicine: Official publication, Society of Nuclear Medicine, 28(10), 1546–1549.
Hofmann, A. A., Wyatt, R. W., Daniels, A. U., Armstrong, L., Alazraki, N., & Taylor, A., Jr. (1990). Bone scans after total knee arthroplasty in asymptomatic patients. Cemented versus cementless. Clinical Orthopaedics and Related Research, 251, 183–188.
Scaffidi, P., Misteli, T., & Bianchi, M. E. (2002). Release of chromatin protein HMGB1 by necrotic cells triggers inflammation. Nature, 418(6894), 191–195. https://doi.org/10.1038/nature00858
O’Connor, K. A., Hansen, M. K., Rachal Pugh, C., Deak, M. M., Biedenkapp, J. C., Milligan, E. D., Johnson, J. D., Wang, H., Maier, S. F., Tracey, K. J., & Watkins, L. R. (2003). Further characterization of high mobility group box 1 (HMGB1) as a proinflammatory cytokine: Central nervous system effects. Cytokine, 24(6), 254–265. https://doi.org/10.1016/j.cyto.2003.08.001
Giannoudis, P. V., Mallina, R., Harwood, P., Perry, S., Sante, E. D., & Pape, H. C. (2010). Pattern of release and relationship between HMGB-1 and IL-6 following blunt trauma. Injury, 41(12), 1323–1327. https://doi.org/10.1016/j.injury.2010.09.012
Zhou, Z., Han, J. Y., **, C. X., **e, J. X., Feng, X., Wang, C. Y., Mei, L., & **ong, W. C. (2008). HMGB1 regulates RANKL-induced osteoclastogenesis in a manner dependent on RAGE. Journal of Bone and Mineral Research: The Official Journal of the American Society for Bone and Mineral Research, 23(7), 1084–1096. https://doi.org/10.1359/jbmr.080234
Steinbeck, M. J., Jablonowski, L. J., Parvizi, J., & Freeman, T. A. (2014). The role of oxidative stress in aseptic loosening of total hip arthroplasties. The Journal of arthroplasty, 29(4), 843–849. https://doi.org/10.1016/j.arth.2013.09.001
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval for this study was obtained from “Sanko University- Clinical Studies Ethics Committee (Approval number: 202018-01)”.
Informed Consent
All participants were informed about the study and signed written informed consent before enrollment.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rızvanoglu, İ.H., Sakarya, B., Benlier, N. et al. HMGB-1 Levels in Painful Knee Arthroplasty: Is it Possible to Distingue Periprosthetic Joint Infection and Aseptic Loosening?. JOIO 57, 1023–1031 (2023). https://doi.org/10.1007/s43465-023-00903-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-023-00903-9