Abstract
Purpose
Percutaneous minimally invasive spinal surgery is performed to manage vertebral compression fractures. The novel modular spine block (MSB) is a spinal fixator designed to provide cementless intravertebral fixation. This study tested the rate of new bone formation in a porcine model following MSB fixation.
Methods
A total of 24 MSBs were implanted in four pigs that served as porcine animal models: solid MSB designated as MSB-0, perforated MSB as MSB-1, hollow MSB as MSB-2, porous 3D-printed MSB as MSB-3. Commercially available intravertebral expandable pillars (IVEP) were also implanted, to serve as a comparison with the MSBs. All pigs underwent X-ray imaging, computed tomography (CT), micro-CT, and histomorphometry. The bone volume fraction (bone volume/tissue volume, BV/TV), bone surface density (bone surface area/tissue volume, BS/TV), trabecular bone thickness (TBT), trabecular bone number (TBN), and trabecular bone separation (TBS) were evaluated.
Results
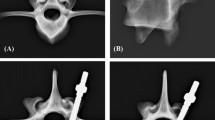
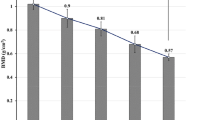
All fixators were securely implanted without any major complications. Adequate alignment of the implants was confirmed radiologically. Marked bone growth was observed on micro-CT and histomorphometry. The average results of BV/TV, BS/TV, TBT, and TBN were the highest in the MSB-2 cases, whereas the values of TBS were the lowest. No statistically significant differences were found between the various intravertebral fixators used.
Conclusions
These findings suggest that MSBs have a similar positive effect on osseointegration as other commercially available cementless intravertebral device. Since these data were obtained from porcine models, further clinical research is required to confirm the reproducibility of these data in humans.





Similar content being viewed by others
Data Availability
All authors make sure that all data and materials as well as software application or custom code support their published claims and comply with field standards.
Code Availability
All authors make sure that all data and materials as well as software application or custom code support their published claims and comply with field standards.
References
Chapman, J., Smith, J. S., Kopjar, B., Vaccaro, A. R., Arnold, P., Shaffrey, C. I., & Fehlings, M. G. (2013). The AO Spine North America Geriatric Odontoid Fracture Mortality Study: A retrospective review of mortality outcomes for operative versus nonoperative treatment of 322 patients with long-term follow-up. Spine (Phila Pa 1976), 38(13), 1098–1104.
Chotigavanich, C., Sanpakit, S., Wantthanaapisith, T., Thanapipatsiri, S., & Chotigavanich, C. (2009). The surgical treatment of the osteoporotic vertebral compression fracture in the elderly patients with the spinal instrumentation. Journal of the Medical Association of Thailand, 92(Suppl5), S109-115.
Reinhold, M., Knop, C., Beisse, R., Audigé, L., Kandziora, F., Pizanis, A., Pranzl, R., Gercek, E., Schultheiss, M., Weckbach, A., Bühren, V., & Blauth, M. (2010). Operative treatment of 733 patients with acute thoracolumbar spinal injuries: Comprehensive results from the second, prospective, Internet-based multicenter study of the Spine Study Group of the German Association of Trauma Surgery. European Spine Journal, 19(10), 1657–1676.
Pourtaheri, S., Luo, W., Cui, C., & Garfin, S. (2018). Vertebral augmentation is superior to nonoperative care at reducing lower back pain for symptomatic osteoporotic compression fractures: A meta-analysis. Clinical Spine Surgery: A Spine Publication, 31(8), 339–344.
Wang, H., Sribastav, S. S., Ye, F., Yang, C., Wang, J., Liu, H., & Zheng, Z. (2015). Comparison of percutaneous vertebroplasty and balloon kyphoplasty for the treatment of single level vertebral compression fractures: A meta-analysis of the literature. Pain Physician, 18(3), 209–222.
Flors, L., Lonjedo, E., Leiva-Salinas, C., Martí-Bonmatí, L., Martínez-Rodrigo, J. J., López-Pérez, E., Figueres, G., & Raoli, I. (2009). Vesselplasty: A new technical approach to treat symptomatic vertebral compression fractures. AJR: American Journal of Roentgenology, 193(1), 218–226.
Eschler, A., Ender, S. A., Ulmar, B., Herlyn, P., Mittlmeier, T., & Gradl, G. (2014). Cementless fixation of osteoporotic VCFs using titanium mesh implants (OsseoFix): Preliminary results. BioMed Research International, 2014, 853897.
Jacobson, R. E. (2020). The use of SpineJack intravertebral implant for the correction of recurrent vertebral fracture after kyphoplasty. Cureus, 12(4), e7599.
Belkoff, S. M., & Molloy, S. (2003). Temperature measurement during polymerization of polymethylmethacrylate cement used for vertebroplasty. Spine (Phila Pa 1976), 28(14), 1555–1559.
Fribourg, D., Tang, C., Sra, P., Delamarter, R., & Bae, H. (2004). Incidence of subsequent vertebral fracture after kyphoplasty. Spine (Phila Pa 1976), 29(20), 2270–2276.
Hsieh, J. Y., Wu, C. D., Wang, T. M., Chen, H. Y., Farn, C. J., & Chen, P. Q. (2013). Reduction of the domino effect in osteoporotic vertebral compression fractures through short-segment fixation with intravertebral expandable pillars compared to percutaneous kyphoplasty: A case control study. BMC Musculoskeletal Disorders, 14, 75.
Hsieh, J. Y., Chen, P. Q., & Wang, J. H. (2018). Minimally invasive open reduction and internal fixation for osteoporotic vertebral compression fractures: Technical report and mid-term outcomes. Open Journal of Orthopedics, 8(9), 337–350.
Hsieh, J. Y. (2021). Minimally invasive management of osteoporotic vertebral compression fractures. In P. Q. Chen, R. M. Lin, & K. S. Tsai (Eds.), Osteoporosis of the spine. Asian perspectives (pp. 615–634). World Scientific.
Castellani, C., Lindtner, R. A., Hausbrandt, P., Tschegg, E., Stanzl-Tschegg, S. E., Zanoni, G., Beck, S., & Weinberg, A. M. (2011). Bone-implant interface strength and osseointegration: Biodegradable magnesium alloy versus standard titanium control. Acta Biomaterialia, 7(1), 432–440.
Li, G., Qian, H., Guo, S., Wang, D., Sun, C., Du, Y., Cheng, J., & Jiang, H. (2019). Assessment of aging characteristics of female condylar trabecular structure by cone-beam computed tomography. Oral Radiology, 35(1), 16–22.
Ghofrani, H., Nunn, T., Robertson, C., Mahar, A., Lee, Y., & Garfin, S. (2010). An evaluation of fracture stabilization comparing kyphoplasty and titanium mesh repair techniques for vertebral compression fractures: Is bone cement necessary? Spine (Phila Pa 1976), 35(16), E768–E773.
Upasani, V. V., Robertson, C., Lee, D., Tomlinson, T., & Mahar, A. T. (2010). Biomechanical comparison of kyphoplasty versus a titanium mesh implant with cement for stabilization of vertebral compression fractures. Spine (Phila Pa 1976), 35(19), 1783–1788.
Ender, S. A., Gradl, G., Ender, M., Langner, S., Merk, H. R., & Kayser, R. (2014). Osseofix® system for percutaneous stabilization of osteoporotic and tumorous vertebral compression fractures—Clinical and radiological results after 12 months. Rofo, 186(4), 380–387.
Lee, J., & Song, K. S. (2020). Transpedicular intravertebral cage augmentation in a patient with neurologic deficits after severely collapsed kummel disease: Minimum 2-year follow-up. World Neurosurgery, 135, 146–155.
Graillon, T., Farah, K., Rakotozanany, P., Blondel, B., Adetchessi, T., Dufour, H., & Fuentes, S. (2016). Anterior approach with expandable cage implantation in management of unstable thoracolumbar fractures: Results of a series of 93 patients. Neuro-Chirurgie, 62(2), 78–85.
Müller, R., Van Campenhout, H., Van Damme, B., Van Der Perre, G., Dequeker, J., Hildebrand, T., & Rüegsegger, P. (1998). Morphometric analysis of human bone biopsies: A quantitative structural comparison of histological sections and micro-computed tomography. Bone, 23(1), 59–66.
de Oliveira, R. C., Leles, C. R., Lindh, C., & Ribeiro-Rotta, R. F. (2012). Bone tissue microarchitectural characteristics at dental implant sites. Part 1: Identification of clinical-related parameters. Clinical Oral Implants Research, 23(8), 981–986.
Keller, J. C., Schneider, G. B., Stanford, C. M., & Kellogg, B. (2003). Effects of implant microtopography on osteoblast cell attachment. Implant Dentistry, 12(2), 175–181.
Parkinson, I. H., Badiei, A., Stauber, M., Codrington, J., Muller, R., & Fazzalari, N. L. (2012). Vertebral body bone strength: The contribution of individual trabecular element morphology. Osteoporosis International, 23(7), 1957–1965.
Vasconcellos, L. M., Leite, D. O., Oliveira, F. N., Carvalho, Y. R., & Cairo, C. A. (2010). Evaluation of bone ingrowth into porous titanium implant: Histomorphometric analysis in rabbits. Brazilian Oral Research, 24(4), 399–405.
Karageorgiou, V., & Kaplan, D. (2005). Porosity of 3D biomaterial scaffolds and osteogenesis. Biomaterials, 26(27), 5474–5491.
Hartmann, F., Griese, M., Dietz, S. O., Kuhn, S., Rommens, P. M., & Gercek, E. (2015). Two-year results of vertebral body stenting for the treatment of traumatic incomplete burst fractures. Minimally Invasive Therapy and Allied Technologies, 24(3), 161–166.
Acknowledgements
This study was approved by National Taiwan University Hospital. The authors wish to thank all the members who participated in this study.
Author information
Authors and Affiliations
Contributions
Y-YH designed the study. J-YH participated in the conception, acquisition, analysis and interpretation of the data, drafting, and final preparation of the manuscript. J-HW and P-QC revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors, their immediate families, and any research foundations with which they are affiliated have not received any financial payments or other benefits from any commercial entity related to the subject of this article.
Ethical Approval
The experimental protocol and surgical procedures were conducted with the approval of the Institutional Animal Care and Use Committee of Pig model Animal Technology Co., Ltd. (Approval No. PIG-107012).
Consent to Participate
Not applicable.
Consent for Publication
All authors will either grant the Publisher an exclusive license to publish the article.
Supplementary Information
Below is the link to the electronic supplementary material.
40846_2022_698_MOESM1_ESM.jpg
Supplementary file1 (JPG 179 kb)—Supplemental Figure 1—Procedure of MSB fixation (from left to right): transpedicular insertion of the first MSB segment, guided by a template plug, expansion by a thin tamper, expansion by a thick tamper, and second MSB segment fixation.
Rights and permissions
About this article
Cite this article
Hsieh, JY., Wang, JH., Chen, PQ. et al. Comparison of Osseointegration in Different Intravertebral Fixators. J. Med. Biol. Eng. 42, 196–203 (2022). https://doi.org/10.1007/s40846-022-00698-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40846-022-00698-4