Abstract
Purpose of Review
The management of insomnia is shrouded with clinical dilemmas resulting in dissatisfaction both for clinicians and patients. Pharmacotherapy, which forms the more popular part of the armamentarium, is fraught with warnings of various adverse effects, though its effectiveness in treatment is undoubtable. Behavioural therapies, which form the other important part of the treatment options, are considered to be underutilised, despite apparent safety with regard to adverse effects. The current manuscript intends to summarize the effectiveness of various behavioural therapies in the management of insomnia.
Recent Findings
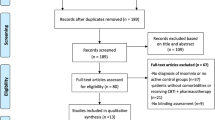
A review was conducted on the various meta-analyses published on the said topic. The total number of studies recruited for this review was 31, most of which were on multicomponent cognitive behavioural therapy for insomnia (CBTi) (N = 26). The studies on CBTi were more diverse in their approach and depicted good evidence base as effective management modality. Multi-component CBTi was also safe in special populations and effective in dealing with cognitive symptoms of insomnia. Individual components of CBTi like mindfulness therapy, sleep hygiene and sleep restriction therapies had relatively modest efficacy.
Summary
CBTi forms a safe and effective behavioural therapy for the management of insomnia. It has a good evidence base and can be a prudent treatment option for insomnia. Further research is required to substantiate the evidence base for other behavioural therapies.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Lovato N, Lack L. Insomnia and mortality: a meta-analysis. Sleep Med Rev. 2019;43:71–83.
Weissman MM, Greenwald S, Niño-Murcia G, Dement WC. The morbidity of insomnia uncomplicated by psychiatric disorders. Gen Hosp Psych. 1997;19:245–50.
Basu A, Joshi T, Pal A, Gupta R. Management of chronic insomnia using hypnotics: a friend or a foe? Sleep Biol Rhythm. 2022;201(20):39–46.
Guina J, Merrill B. Benzodiazepines I: up** the care on downers: the evidence of risks, benefits and alternatives. J Clin Med. 2018;7:17.
Pal A, Joshi T, Basu A, Gupta R. Management of chronic insomnia using cognitive behavior therapy for insomnia (CBT-I) during COVID-19 pandemic: Does One Shoe Fit All? Sleep Vigil. 2022;6:51–60.
Edinger JD, Arnedt JT, Bertisch SM, et al. Behavioral and psychological treatments for chronic insomnia disorder in adults: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2021;17:255–62.
Hauk L. Treatment of chronic insomnia in adults: ACP guideline. Am Fam Physician. 2017;95:669–70.
Riemann D, Baglioni C, Bassetti C, et al. European guideline for the diagnosis and treatment of insomnia. J Sleep Res. 2017;26:675–700.
Vincent N, Lionberg C. Treatment preference and patient satisfaction in chronic insomnia. Sleep. 2001;24:411–7.
• van Straten A, van der Zweerde T, Kleiboer A, Cuijpers P, Morin CM, Lancee J. Cognitive and behavioral therapies in the treatment of insomnia: a meta-analysis. Sleep Med Rev. 2018;38:3–16. This study is a large-scale meta-analysis of 87 RCTs evaluating the role of CBTi on nighttime sleep.
Trauer JM, Qian MY, Doyle JS, Rajaratnam SMW, Cunnington D. Cognitive behavioral therapy for chronic insomnia: a systematic review and meta-analysis. Ann Intern Med. 2015;163:191–204.
Wang YY, Yang Y, Rao WW, Zhang SF, Zeng LN, Zheng W, Ng CH, Ungvari GS, Zhang L, **ang YT. Cognitive behavioural therapy monotherapy for insomnia: a meta-analysis of randomized controlled trials. Asian J Psychiatr. 2020; https://doi.org/10.1016/j.ajp.2019.10.008.
Edinger JD, Arnedt JT, Bertisch SM, et al. Behavioral and psychological treatments for chronic insomnia disorder in adults: an American Academy of Sleep Medicine systematic review, meta-analysis, and GRADE assessment. J Clin Sleep Med. 2021;17:263–98.
• Thakral M, Von Korff M, SM MC, Morin CM, Vitiello MV. Changes in dysfunctional beliefs about sleep after cognitive behavioral therapy for insomnia: a systematic literature review and meta-analysis. Sleep Med Rev. 2020; https://doi.org/10.1016/j.smrv.2019.101230. Meta-analysis evaluating the role of CBTi on sleep-related cognition.
Ballesio A, Bacaro V, Vacca M, Chirico A, Lucidi F, Riemann D, Baglioni C, Lombardo C. Does cognitive behaviour therapy for insomnia reduce repetitive negative thinking and sleep-related worry beliefs? A systematic review and meta-analysis: Sleep Med Rev.; 2021. https://doi.org/10.1016/j.smrv.2020.101378.
Parsons CE, Zachariae R, Landberger C, Young KS. How does cognitive behavioural therapy for insomnia work? A systematic review and meta-analysis of mediators of change. Clin Psychol Rev.; 2021. https://doi.org/10.1016/j.cpr.2021.102027.
Benz F, Knoop T, Ballesio A, Bacaro V, Johann AF, Rücker G, Feige B, Riemann D, Baglioni C. The efficacy of cognitive and behavior therapies for insomnia on daytime symptoms: a systematic review and network meta-analysis. Clin Psychol Rev. 2020; https://doi.org/10.1016/j.cpr.2020.101873.
van der Zweerde T, Bisdounis L, Kyle SD, Lancee J, van Straten A. Cognitive behavioral therapy for insomnia: a meta-analysis of long-term effects in controlled studies. Sleep Med Rev. 2019; https://doi.org/10.1016/j.smrv.2019.08.002.
Seyffert M, Lagisetty P, Landgraf J, Chopra V, Pfeiffer PN, Conte ML, Rogers MAM. Internet-delivered cognitive behavioral therapy to treat insomnia: a systematic review and meta-analysis. PLoS One. 2016; https://doi.org/10.1371/journal.pone.0149139.
Zachariae R, Lyby MS, Ritterband LM, O’Toole MS. Efficacy of internet-delivered cognitive-behavioral therapy for insomnia – a systematic review and meta-analysis of randomized controlled trials. Sleep Med Rev. 2016;30:1–10.
Hasan F, Tu YK, Yang CM, James Gordon C, Wu D, Lee HC, Yuliana LT, Herawati L, Chen TJ, Chiu HY. Comparative efficacy of digital cognitive behavioral therapy for insomnia: a systematic review and network meta-analysis. Sleep Med Rev. 2022; https://doi.org/10.1016/j.smrv.2021.101567.
Soh HL, Ho RC, Ho CS, Tam WW. Efficacy of digital cognitive behavioural therapy for insomnia: a meta-analysis of randomised controlled trials. Sleep Med. 2020;75:315–25.
Ye YY, Chen NK, Chen J, Liu J, Lin L, Liu YZ, Lang Y, Li XJ, Yang XJ, Jiang XJ. Internet-based cognitive-behavioural therapy for insomnia (ICBT-i): a meta-analysis of randomised controlled trials. BMJ Open. 2016; https://doi.org/10.1136/bmjopen-2015-010707.
Cheng SK, Dizon J. Computerised cognitive behavioural therapy for insomnia: a systematic review and meta-analysis. Psychother Psychosom. 2012;81:206–16.
Sharafkhaneh A, Salari N, Khazaie S, Ghasemi H, Darvishi N, Hosseinian-Far A, Mohammadi M, Khazaie H. Telemedicine and insomnia: a comprehensive systematic review and meta-analysis. Sleep Med. 2022;90:117–30.
Koffel EA, Koffel JB, Gehrman PR. A meta-analysis of group cognitive behavioral therapy for insomnia. Sleep Med Rev. 2015;19:6–16.
Ho FYY, Chung KF, Yeung WF, Ng TH, Kwan KS, Yung KP, Cheng SK. Self-help cognitive-behavioral therapy for insomnia: a meta-analysis of randomized controlled trials. Sleep Med Rev. 2015;19:17–28.
• Gao Y, Ge L, Liu M, et al. Comparative efficacy and acceptability of cognitive behavioral therapy delivery formats for insomnia in adults: a systematic review and network meta-analysis. Sleep Med Rev. 2022;64:101648. Meta-analysis comparing various modes of delivery of CBTi.
Ma ZR, Shi LJ, Deng MH. Efficacy of cognitive behavioral therapy in children and adolescents with insomnia: a systematic review and meta-analysis. Brazilian J Med Biol Res. 2018; https://doi.org/10.1590/1414-431X20187070.
Åslund L, Arnberg F, Kanstrup M, Lekander M. Cognitive and behavioral interventions to improve sleep in school-age children and adolescents: a systematic review and meta-analysis. J Clin Sleep Med. 2018;14:1937–47.
Blake MJ, Sheeber LB, Youssef GJ, Raniti MB, Allen NB. Systematic review and meta-analysis of adolescent cognitive–behavioral sleep interventions. Clin Child Fam Psychol Rev. 2017;20:227–49.
Irwin MR, Cole JC, Nicassio PM. Comparative meta-analysis of behavioral interventions for insomnia and their efficacy in middle-aged adults and in older adults 55+ years of age. Heal Psychol. 2006;25:3–14.
Montgomery P, Dennis JA. Cognitive behavioural interventions for sleep problems in adults aged 60+. Cochrane Database Syst Rev. 2003;1:CD003161. https://doi.org/10.1002/14651858.CD003161
Gong H, Ni CX, Liu YZ, Zhang Y, Su WJ, Lian YJ, Peng W, Jiang CL. Mindfulness meditation for insomnia: a meta-analysis of randomized controlled trials. J Psychosom Res. 2016;89:1–6.
Wang YY, Wang F, Zheng W, Zhang L, Ng CH, Ungvari GS, **ang YT. Mindfulness-based interventions for insomnia: a meta-analysis of randomized controlled trials. Behav Sleep Med. 2020;18:1–9.
Chen TL, Chang SC, Hsieh HF, Huang CY, Chuang JH, Wang HH. Effects of mindfulness-based stress reduction on sleep quality and mental health for insomnia patients: a meta-analysis. J Psychosom Res. 2020; https://doi.org/10.1016/j.jpsychores.2020.110144.
Chung KF, Lee CT, Yeung WF, Chan MS, Chung EWY, Lin WL. Sleep hygiene education as a treatment of insomnia: a systematic review and meta-analysis. Fam Pract. 2018;35:365–75.
Maurer LF, Schneider J, Miller CB, Espie CA, Kyle SD. The clinical effects of sleep restriction therapy for insomnia: a meta-analysis of randomised controlled trials. Sleep Med Rev. 2021; https://doi.org/10.1016/j.smrv.2021.101493.
van Straten A, Cuijpers P. Self-help therapy for insomnia: a meta-analysis. Sleep Med Rev. 2009;13:61–71.
Matthews EE, Arnedt JT, McCarthy MS, Cuddihy LJ, Aloia MS. Adherence to cognitive behavioral therapy for insomnia: a systematic review. Sleep Med Rev. 2013;17:453–64.
Mellor A, Kavaliotis E, Mascaro L, Drummond SPA. Approaches to the assessment of adherence to CBT-I, predictors of adherence, and the association of adherence to outcomes: a systematic review. Sleep Med Rev. 2022; https://doi.org/10.1016/J.SMRV.2022.101620.
Horsch C, Lancee J, Beun RJ, Neerincx MA, Brinkman WP. Adherence to technology-mediated insomnia treatment: a meta-analysis, interviews, and focus groups. J Med Internet Res. 2015;17:e214.
Berk M, Parker G. The elephant on the couch: side-effects of psychotherapy. Aust N Z J Psychiatry. 2009;43:787–94. https://doi.org/10.1080/00048670903107559.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
AP and AB have no conflict of interest to declare. RG has received grants from Indian Council of Medical Research, National Health Mission, Uttarakhand and Uttarakhand Council for Science and Technology and royalties from Elsevier RELX India, Springer Nature, Singapore and Apple Academic Press, USA, but none pertaining to this manuscript.
Human and Animal Rights and Informed Consent
Not required.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pal, A., Basu, A. & Gupta, R. Behavioural Treatment Considerations for Insomnia: a Review of Meta-analyses. Curr Sleep Medicine Rep 9, 257–264 (2023). https://doi.org/10.1007/s40675-023-00264-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40675-023-00264-7