Abstract
Purpose
Controversies exist in the effect of body weight loss and fluctuation on cardiovascular disease (CVD) and mortality. This study aims to assess the effect of weight variability on CVD and all-cause and cardiovascular mortality in the Tehran Lipid and Glucose Study (TLGS) cohort.
Method
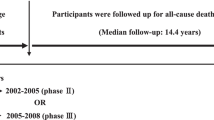
Participants aged ≥ 40 year at the baseline period with at least 3 BMI measurements were included in this study. After excluding individuals with cancer, CVD, end-stage renal disease, systemic use of glucocorticoids, pregnancy, and missing covariates at the baseline, a total of 3461 participants were enrolled and followed for 18 years. BMI variability was defined using root mean squared error (RMSE) and average successive variability (ASV). In the RMSE method, BMI variability was calculated using the best-fitting model for BMI trend of each subject. Multivariate Cox proportional hazard models were applied to assess BMI variability’s effect on CVD and mortality.
Results
Among the 3461 participants in this study, the group with the highest weight variability had an increased risk of death for all-cause (HR 1.65; 95% CI 1.21–2.25), non-cardiovascular (HR 1.77; 95% CI 1.24–2.53), and non-cancer (HR 1.77; 95% CI 1.25–2.50) mortality. However, BMI variability showed to be protective against CVD (HR 0.76; 95% CI 0.6–0.97). These findings were significant in males, non-smokers, participants with age ≤ 60 year, BMI < 30, negative BMI slope, and both diabetic and non-diabetic subjects.
Conclusion
High BMI variability is associated with increased risk of all-cause, non-CVD, and non-cancer mortality, although protective for the CVD event. Appropriate strategies for body weight maintenance after weight loss could be adopted to avoid weight variability, particularly in non-obese subjects.



Similar content being viewed by others
References
Danaei G, Robins JM, Young J, Hu FB, Manson JE, Hernán MA (2016) Estimated effect of weight loss on risk of coronary heart disease and mortality in middle-aged or older women: sensitivity analysis for unmeasured confounding by undiagnosed disease. Epidemiology 27(2):302
Mulligan AA, Lentjes MA, Luben RN, Wareham NJ, Khaw K-T (2018) Weight change and 15 year mortality: results from the European Prospective Investigation into Cancer in Norfolk (EPIC-Norfolk) cohort study. Eur J Epidemiol 33(1):37–53
Doehner W, Erdmann E, Cairns R, Clark AL, Dormandy JA, Ferrannini E et al (2012) Inverse relation of body weight and weight change with mortality and morbidity in patients with type 2 diabetes and cardiovascular co-morbidity: an analysis of the PROactive study population. Int J Cardiol 162(1):20–26
Chen Y, Yang X, Wang J, Li Y, Ying D, Yuan H (2018) Weight loss increases all-cause mortality in overweight or obese patients with diabetes: a meta-analysis. Medicine. https://doi.org/10.1097/MD.0000000000012075
Chaston TB, Dixon J (2008) Factors associated with percent change in visceral versus subcutaneous abdominal fat during weight loss: findings from a systematic review. Int J Obes 32(4):619–628
Clark AL, Fonarow GC, Horwich TB (2014) Obesity and the obesity paradox in heart failure. Prog Cardiovasc Dis 56(4):409–414
Costanzo P, Cleland JG, Pellicori P, Clark AL, Hepburn D, Kilpatrick ES et al (2015) The obesity paradox in type 2 diabetes mellitus: relationship of body mass index to prognosis: a cohort study. Ann Intern Med 162(9):610–618
Casazza K, Fontaine KR, Astrup A, Birch LL, Brown AW, Bohan Brown MM et al (2013) Myths, presumptions, and facts about obesity. N Engl J Med 368(5):446–454
Ochner CN, Barrios DM, Lee CD, Pi-Sunyer FX (2013) Biological mechanisms that promote weight regain following weight loss in obese humans. Physiol Behav 120:106–113
Wing RR, Phelan S (2005) Long-term weight loss maintenance—. Am J Clin Nutr 82(1):222S-S225
Stevens VL, Jacobs EJ, Sun J, Patel AV, McCullough ML, Teras LR et al (2012) Weight cycling and mortality in a large prospective US study. Am J Epidemiol 175(8):785–792
Katan MB (2009) Weight-loss diets for the prevention and treatment of obesity. N Engl J Med 360(9):923
Diaz VA, Mainous AG, Everett CJ (2005) The association between weight fluctuation and mortality: results from a population-based cohort study. J Community Health 30(3):153–165
Field AE, Malspeis S, Willett WC (2009) Weight cycling and mortality among middle-aged or older women. Arch Intern Med 169(9):881–886
Iribarren C, Sharp DS, Burchfiel CM, Petrovitch H (1995) Association of weight loss and weight fluctuation with mortality among Japanese American men. N Engl J Med 333(11):686–692
Lissner L, Odell PM, D’Agostino RB, Stokes J III, Kreger BE, Belanger AJ et al (1991) Variability of body weight and health outcomes in the Framingham population. N Engl J Med 324(26):1839–1844
Lissner L, Andres R, Muller D, Shimokata H (1990) Body weight variability in men: metabolic rate, health and longevity. Int J Obes 14(4):373–383
Rzehak P, Meisinger C, Woelke G, Brasche S, Strube G, Heinrich J (2007) Weight change, weight cycling and mortality in the ERFORT Male Cohort Study. Eur J Epidemiol 22(10):665–673
Blair SN, Shaten J, Brownell K, Collins G, Lissner L (1993) Body weight change, all-cause mortality, and cause-specific mortality in the multiple risk factor intervention trial. Ann Intern Med 119(7_Part_2):749–57
Dyer AR, Stamler J, Greenland P (2000) Associations of weight change and weight variability with cardiovascular and all-cause mortality in the Chicago Western Electric Company Study. Am J Epidemiol 152(4):324–333
Hamm P, Shekelle RB, Stamler J (1989) Large fluctuations in body weight during young adulthood and twenty-fwe-year risk of coronary death in men. Am J Epidemiol 129(2):312–318
Folsom A, French S, Zheng W, Baxter J, Jeffery R (1996) Weight variability and mortality: the Iowa Women’s Health Study. Int J Obes Relat Metab Disord 20(8):704–709
Wannamethee SG, Shaper AG, Walker M (2002) Weight change, weight fluctuation, and mortality. Arch Intern Med 162(22):2575–2580
Bangalore S, Fayyad R, DeMicco DA, Colhoun HM, Waters DD (2018) Body weight variability and cardiovascular outcomes in patients with type 2 diabetes mellitus. Circ Cardiovasc Qual Outcomes 11(11):e004724
Cai Z, Wu W, Chen Z, Fang W, Li W, Chen G et al (2021) Long-term body mass index variability, weight change slope, and risk of cardiovascular outcomes: 7-year prospective study in Chinese hypertensive subjects. Obes Facts 14(5):442–449
Sponholtz TR, Heuvel ERvd, Xanthakis V, Vasan RS (2019) Association of variability in body mass index and metabolic health with cardiometabolic disease risk. J Am Heart Assoc 8(7):e010793
Jeong S, Choi S, Chang J, Kim K, Kim SM, Hwang SY et al (2021) Association of weight fluctuation with cardiovascular disease risk among initially obese adults. Sci Rep 11(1):10152
Oh TJ, Moon JH, Choi SH, Lim S, Park KS, Cho NH et al (2019) Body-weight fluctuation and incident diabetes mellitus, cardiovascular disease, and mortality: a 16-year prospective cohort study. J Clin Endocrinol Metab 104(3):639–646
Cologne J, Takahashi I, French B, Nanri A, Misumi M, Sadakane A et al (2019) Association of weight fluctuation with mortality in Japanese adults. JAMA Netw Open 2(3):e190731-e
Azizi F, Ghanbarian A, Momenan AA, Hadaegh F, Mirmiran P, Hedayati M et al (2009) Prevention of non-communicable disease in a population in nutrition transition: Tehran Lipid and Glucose Study phase II. Trials 10:5
Choi D, Choi S, Park SM (2019) Impact of weight variability on mortality among Korean men and women: a population based study. Sci Rep 9(1):1–8
Goni L, García-Granero M, Milagro FI, Cuervo M, Martínez JA (2018) Phenotype and genotype predictors of BMI variability among European adults. Nutr Diabetes 8(1):27
Lycett D, Munafò M, Johnstone E, Murphy M, Aveyard P (2011) Associations between weight change over 8 years and baseline body mass index in a cohort of continuing and quitting smokers. Addiction 106(1):188–196
Serdula MK, Mokdad AH, Williamson DF, Galuska DA, Mendlein JM, Heath GW (1999) Prevalence of attempting weight loss and strategies for controlling weight. JAMA 282(14):1353–1358
Narkiewicz K (2005) Obesity and hypertension—the issue is more complex than we thought. Nephrol Dial Transplant 21(2):264–267
Nam GE, Kim W, Han K, Lee C-w, Kwon Y, Han B et al (2020) Body weight variability and the risk of cardiovascular outcomes and mortality in patients with type 2 diabetes: a Nationwide Cohort Study. Diabetes Care 43(9):2234–41
MacLean PS, Higgins J, Giles E, Sherk V, Jackman M (2015) The role for adipose tissue in weight regain after weight loss. Obes Rev 16:45–54
Yatsuya H, Tamakoshi K, Yoshida T, Hori Y, Zhang H, Ishikawa M et al (2003) Association between weight fluctuation and fasting insulin concentration in Japanese men. Int J Obes Relat Metab Disord 27(4):478–483
Li X, Jiang L, Yang M, Wu YW, Sun JZ (2018) Impact of weight cycling on CTRP3 expression, adipose tissue inflammation and insulin sensitivity in C57BL/6J mice. Exp Ther Med 16(3):2052–2059
Tamakoshi K, Yatsuya H, Kondo T, Ishikawa M, Zhang H, Murata C et al (2003) Long-term body weight variability is associated with elevated C-reactive protein independent of current body mass index among Japanese men. Int J Obes 27(9):1059–1065
Olson MB, Kelsey SF, Bittner V, Reis SE, Reichek N, Handberg EM et al (2000) Weight cycling and high-density lipoprotein cholesterol in women: evidence of an adverse effect: a report from the NHLBI-sponsored WISE study. J Am Coll Cardiol 36(5):1565–1571
Karschin J, Lagerpusch M, Enderle J, Eggeling B, Müller MJ, Bosy-Westphal A (2015) Endocrine determinants of changes in insulin sensitivity and insulin secretion during a weight cycle in healthy men. PLoS One 10(2):e0117865
Anderson EK, Gutierrez DA, Kennedy A, Hasty AH (2013) Weight cycling increases T-cell accumulation in adipose tissue and impairs systemic glucose tolerance. Diabetes 62(9):3180–3188
Hanatani S, Izumiya Y, Onoue Y, Tanaka T, Yamamoto M, Ishida T et al (2018) Non-invasive testing for sarcopenia predicts future cardiovascular events in patients with chronic kidney disease. Int J Cardiol 268:216–221
Shade ED, Ulrich CM, Wener MH, Wood B, Yasui Y, Lacroix K et al (2004) Frequent intentional weight loss is associated with lower natural killer cell cytotoxicity in postmenopausal women: possible long-term immune effects. J Am Diet Assoc 104(6):903–912
Nguyen ND, Center JR, Eisman JA, Nguyen TV (2007) Bone loss, weight loss, and weight fluctuation predict mortality risk in elderly men and women. J Bone Miner Res 22(8):1147–1154
Zou H, Yin P, Liu L, Liu W, Zhang Z, Yang Y et al (2019) Body-weight fluctuation was associated with increased risk for cardiovascular disease, all-cause and cardiovascular mortality: a systematic review and meta-analysis. Front Endocrinol. https://doi.org/10.3389/fendo.2019.00728
Park HW, Kim KH, Song IG, Kwon TG, Kim WH, Bae JH (2017) Body mass index, carotid plaque, and clinical outcomes in patients with coronary artery disease. Coron Artery Dis 28(4):278–286
Fildes A, Charlton J, Rudisill C, Littlejohns P, Prevost AT, Gulliford MC (2015) Probability of an obese person attaining normal body weight: cohort study using electronic health records. Am J Public Health 105(9):e54–e59
Cheng FW, Gao X, Jensen GL (2015) Weight change and all-cause mortality in older adults: a meta-analysis. J Nutr Gerontol Geriatr 34(4):343–368
Svetkey LP, Clark JM, Funk K, Corsino L, Batch BC, Hollis JF et al (2014) Greater weight loss with increasing age in the weight loss maintenance trial. Obesity (Silver Spring) 22(1):39–44
Lee JS, Visser M, Tylavsky FA, Kritchevsky SB, Schwartz AV, Sahyoun N et al (2010) Weight loss and regain and effects on body composition: the health, aging, and body composition study. J Gerontol A Biol Sci Med Sci 65(1):78–83
Shufelt CL, Pacheco C, Tweet MS, Miller VM (2018) Sex-specific physiology and cardiovascular disease. Adv Exp Med Biol 1065:433–454
American Diabetes Association (2015) 6. Obesity management for the treatment of type 2 diabetes. Diabetes Care 39(Supplement_1):S47–S51
Harrington M, Gibson S, Cottrell RC (2009) A review and meta-analysis of the effect of weight loss on all-cause mortality risk. Nutr Res Rev 22(1):93–108
Wing RR, Reboussin D, Lewis CE (2013) Intensive lifestyle intervention in type 2 diabetes. N Engl J Med 369(24):2358–2359
Strelitz J, Lawlor ER, Wu Y, Estlin A, Nandakumar G, Ahern AL et al (2022) Association between weight change and incidence of cardiovascular disease events and mortality among adults with type 2 diabetes: a systematic review of observational studies and behavioural intervention trials. Diabetologia 65(3):424–439
Rhee EJ (2017) Weight cycling and its cardiometabolic impact. J Obes Metab Syndr 26(4):237–242
Saito Y, Takahashi O, Arioka H, Kobayashi D (2017) Associations between body fat variability and later onset of cardiovascular disease risk factors. PLoS One 12(4):e0175057
Lee JS, Kawakubo K, Kobayashi Y, Mori K, Kasihara H, Tamura M (2001) Effects of ten year body weight variability on cardiovascular risk factors in Japanese middle-aged men and women. Int J Obes Relat Metab Disord 25(7):1063–1067
Ceriello A, Lucisano G, Prattichizzo F, Eliasson B, Franzén S, Svensson A-M et al (2021) Variability in body weight and the risk of cardiovascular complications in type 2 diabetes: results from the Swedish National Diabetes Register. Cardiovasc Diabetol 20(1):173
Kolber MR, Scrimshaw C (2014) Family history of cardiovascular disease. Can Fam Physician 60(11):1016
Brown R, Kuk J (2015) Consequences of obesity and weight loss: a devil’s advocate position. Obes Rev 16(1):77–87
Hong N, Yoon H-j, Lee Y-h, Kim HR, Lee BW, Rhee Y et al (2016) Serum PTHrP predicts weight loss in cancer patients independent of hypercalcemia, inflammation, and tumor burden. J Clin Endocrinol Metab 101(3):1207–14
Santos I, Sniehotta FF, Marques MM, Carraça EV, Teixeira PJ (2017) Prevalence of personal weight control attempts in adults: a systematic review and meta-analysis. Obes Rev 18(1):32–50
Acknowledgements
The authors express our appreciation to TLGS participants and the research team members for their contribution to the study.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the ethics committee of the Research Institute for Endocrine Sciences (RIES), Shahid Beheshti University of Medical Sciences, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Research involving human participants
All procedures followed were in accordance with the ethical standards of the ethics committee of the Research Institute for Endocrine Sciences (RIES), Shahid Beheshti University of Medical Sciences (IR.SBMU.ENDOCRINE.REC. 1398.103), and with the Helsinki Declaration of 1964 and later versions.
Informed consent
Informed consent was obtained from all participants for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mehran, L., Honarvar, M., Masoumi, S. et al. Weight fluctuation, mortality, and cardiovascular disease in adults in 18 years of follow-up: Tehran Lipid and Glucose Study. J Endocrinol Invest 46, 37–49 (2023). https://doi.org/10.1007/s40618-022-01881-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-022-01881-9