Abstract
At the onset of pregnancy, people with preexisting conditions face additional challenges in carrying their pregnancy to term, as the safety of the develo** fetus and pregnant person is a significant factor of concern. Nanoparticle (NP)-based therapies have displayed success against various conditions and diseases in non-pregnant patients, but the use of NPs in maternal–fetal health applications needs to be better established. Local vaginal delivery of NPs is a promising administration route with the potential to yield high cargo retention in the vagina and improved therapeutic efficacy compared to systemic administration that results in rapid NP clearance by the hepatic first-pass effect. In this study, we investigated the biodistribution and short-term toxicity of poly(ethylene glycol)-poly(lactic-co-glycolic acid) (PEG-PLGA) NPs in pregnant mice following vaginal delivery. The NPs were either loaded with DiD fluorophores for tracking cargo distribution (termed DiD-PEG-PLGA NPs) or included Cy5-tagged PLGA in the formulation for tracking polymer distribution (termed Cy5-PEG-PLGA NPs). DiD-PEG-PLGA NPs were administered at gestational day (E)14.5 or 17.5, and cargo biodistribution was analyzed 24 h later by fluorescence imaging of whole excised tissues and histological sections. No gestational differences in DiD distribution were observed, so Cy5-PEG-PLGA NPs were administered at only E17.5 to evaluate polymer distribution in the reproductive organs of pregnant mice. Cy5-PEG-PLGA NPs distributed to the vagina, placentas, and embryos, whereas DiD cargo was only observed in the vagina. NPs did not impact maternal, fetal, or placental weight, suggesting they display no short-term effects on maternal or fetal growth. The results from this study encourage future investigation into the use of vaginally delivered NP therapies for conditions affecting the vagina during pregnancy.
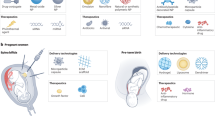
Graphical Abstract








Similar content being viewed by others
Availability of data and materials
The datasets generated during the current study are available from the corresponding authors on reasonable request.
References
Ci LQ, Huang ZG, Lv FM, Wang J, Feng LL, Sun F, Cao SJ, Liu ZP, Liu Y, Wei G, Lu WY. Enhanced delivery of imatinib into vaginal mucosa via a new positively charged nanocrystal-loaded in situ hydrogel formulation for treatment of cervical cancer. Pharmaceutics. 2019;11(1). https://doi.org/10.3390/pharmaceutics11010015.
Chen J, Gu W, Yang L, Chen C, Shao R, Xu K, Xu ZP. Nanotechnology in the management of cervical cancer. Rev Med Virol. 2015;25:72–83. https://doi.org/10.1002/rmv.
Cunha-Reis C, Machado A, Barreiros L, Araújo F, Nunes R, Seabra V, Ferreira D, Segundo MA, Sarmento B, das Neves J. Nanoparticles-in-film for the combined vaginal delivery of anti-HIV microbicide drugs. J Control Release. 2016;243:43–53. https://doi.org/10.1016/j.jconrel.2016.09.020.
Chaowanachan T, Krogstad E, Ball C, Woodrow KA. Drug synergy of tenofovir and nanoparticle-based antiretrovirals for HIV prophylaxis. PLoS One. 2013;8(4). https://doi.org/10.1371/journal.pone.0061416.
Friend DR. Drug delivery for the treatment of endometriosis and uterine fibroids. Drug Deliv Transl Res. 2017;7(6):829–39. https://doi.org/10.1007/s13346-017-0423-2.
Chaudhury K, Babu K N, Singh AK, Das S, Kumar A, Seal S. Mitigation of endometriosis using regenerative cerium oxide nanoparticles. Nanomed Nanotech Biol Med. 2013;9(3):439–448. https://doi.org/10.1016/j.nano.2012.08.001.
Bradshaw CS, Sobel JD. Current treatment of bacterial vaginosis-limitations and need for innovation. J Infect Dis. 2016;214(Suppl 1):S14–20. https://doi.org/10.1093/infdis/jiw159.
Machado A, Cerca N. Influence of biofilm formation by gardnerella vaginalis and other anaerobes on bacterial vaginosis. J Infect Dis. 2015;212(12):1856–61. https://doi.org/10.1093/infdis/jiv338.
Irvin-Choy NS, Nelson KM, Gleghorn JP, Day ES. Design of nanomaterials for applications in maternal/fetal medicine. J Mater Chem B. 2020;8:6548–61. https://doi.org/10.1039/d0tb00612b.
Hoshyar N, Gray S, Han H, Bao G. The effect of nanoparticle size on in vivo pharmacokinetics and cellular interaction. Nanomedicine. 2016;11(6):673–92. https://doi.org/10.2217/nnm.16.5.
Alexis F, Pridgen E, Molnar LK, Farokhzad OC. Factors affecting the clearance and biodistribution of polymeric nanoparticles. Mol Pharm. 2008;5(4):505–15. https://doi.org/10.1021/mp800051m.
Chenthamara D, Subramaniam S, Ramakrishnan SG, Krishnaswamy S, Essa MM, Lin FH, Qoronfleh MW. Therapeutic efficacy of nanoparticles and routes of administration. Biomater Res. 2019;23(1):1–29. https://doi.org/10.1186/s40824-019-0166-x.
Nelson KM, Irvin-Choy ND, Hoffman MK, Gleghorn JP, Day ES. Diseases and conditions that impact maternal and fetal health and the potential for nanomedicine therapies. Adv Drug Deliv Rev. 2020. https://doi.org/10.1016/j.addr.2020.09.013.
Figueroa-Espada CG, Mitchell MJ, Riley RS, Hofbauer S. Exploiting the placenta for nanoparticle-mediated drug delivery during pregnancy. Adv Drug Deliv Rev. 2020;160:244–61. https://doi.org/10.1016/j.addr.2020.09.006.
Young RE, Nelson KM, Hofbauer SI, Vijayakumar T, Alameh M-G, Weissman D, Papachristou C, Gleghorn JP, Riley RS. Lipid nanoparticle composition drives MRNA delivery to the placenta. BioRxiv Prepr Serv Biol. 2022. https://doi.org/10.1101/2022.12.22.521490.
Yang H, Du L, Tian X, Fan Z, Sun C, Liu Y, Keelan JA, Nie G. Effects of nanoparticle size and gestational age on maternal biodistribution and toxicity of gold nanoparticles in pregnant mice. Toxicol Lett. 2014;230(1):10–8. https://doi.org/10.1016/j.toxlet.2014.07.030.
Yang H, Sun C, Fan Z, Tian X, Yan L, Du L, Liu Y, Chen C, Liang XJ, Anderson GJ, Keelan JA, Zhao Y, Nie G. Effects of gestational age and surface modification on materno-fetal transfer of nanoparticles in murine pregnancy. Sci Rep. 2012;2:1–8. https://doi.org/10.1016/j.nano.2021.102412.
Irvin-Choy NS, Nelson KM, Dang MN, Gleghorn JP, Day ES. Gold nanoparticle biodistribution in pregnant mice following intravenous administration varies with gestational age. Nanomed Nanotechnol Biol Med. 2021;36(August):22–24. https://doi.org/10.1016/j.nano.2021.102412.
Owens DE, Peppas NA. Opsonization, biodistribution, and pharmacokinetics of polymeric nanoparticles. Int J Pharm. 2006;307(1):93–102. https://doi.org/10.1016/j.ijpharm.2005.10.010.
Blanco E, Shen H, Ferrari M, Author NB. Principles of nanoparticle design for overcoming biological barriers to drug delivery. Nat Biotechnol. 2016;33(9):941–51. https://doi.org/10.1038/nbt.3330.
Katz DF, Dunmire EN. Cervical mucus. Adv Drug Deliv Rev. 1993;11(3):385–401. https://doi.org/10.1016/0169-409X(93)90017-X.
Becher N, Waldorf KA, Hein M, Uldbjerg N. The cervical mucus plug: structured review of the literature. Acta Obstet Gynecol Scand. 2009;88(5):502–13. https://doi.org/10.1080/00016340902852898.
Cu Y, Booth CJ, Saltzman MW. In vivo distribution of surface modified PLGA nanoparticles following intravaginal delivery. J Control Release. 2011;156(2):258–64. https://doi.org/10.1016/j.jconrel.2011.06.036.
Zierden HC, Josyula A, Shapiro RL, Hsueh H, Ensign LM, Sciences M. Avoiding a sticky situation: bypassing the mucus barrier for improved local drug delivery. Trends Mol Med. 2022;27(5):436–50. https://doi.org/10.1016/j.molmed.2020.12.001.
Maisel K, Reddy M, Xu Q, Chattopadhyay S, Cone R, Ensign LM, Hanes J. Nanoparticles coated with high molecular weight PEG penetrate mucus and provide uniform vaginal and colorectal distribution in vivo. Nanomedicine. 2016;11(11):1337–43.
Ensign LM, Henning A, Schneider CS, Maisel K, Wang Y, Porosoff MD, Cone R, Hanes J. Ex vivo characterization of particle transport in mucus secretions coating freshly excised mucosal tissues. Mol Pharm. 2013;10(6):2176–82. https://doi.org/10.1021/mp400087y.Ex.
Khutoryanskiy VV. Beyond PEGylation: alternative surface-modification of nanoparticles with mucus-inert biomaterials. Adv Drug Deliv Rev. 2018;124:140–9. https://doi.org/10.1016/j.addr.2017.07.015.
Edwards VL, McComb E, Gleghorn JP, Forney L, Bavoil PM, Ravel J. Three-dimensional models of the cervicovaginal epithelia to study host-microbiome interactions and sexually transmitted infections. Pathog Dis. 2022;80(1):1–13. https://doi.org/10.1093/femspd/ftac026.
Harris JC, Sterin EH, Day ES. Membrane-wrapped nanoparticles for enhanced chemotherapy of acute myeloid leukemia. ACS Biomater Sci Eng. 2022;8(10):4439–48. https://doi.org/10.1021/acsbiomaterials.2c00832.
Valcourt DM, Dang MN, Scully MA, Day ES. Nanoparticle-mediated co-delivery of notch-1 antibodies and ABT-737 as a potent treatment strategy for triple-negative breast cancer. ACS Nano. 2020;14(3):3378–88. https://doi.org/10.1021/acsnano.9b09263.
Khanal S, Adhikari U, Rijal N, Bhattarai S, Sankar J, Bhattarai N. PH-responsive PLGA nanoparticle for controlled payload delivery of diclofenac sodium. J Funct Biomater. 2016;7(3):21. https://doi.org/10.3390/jfb7030021.
Poley M, Shammai Y, Kaduri M, Koren L, Adir O, Shklover J. Chemotherapeutic nanoparticles accumulate in the female reproductive system during ovulation affecting fertility and anticancer activity. 2020. https://doi.org/10.1021/acsnano.1c07237.
Hayward CE, Lean S, Sibley CP, Jones RL, Wareing M, Greenwood SL, Dilworth MR. Placental adaptation: what can we learn from birthweight:placental weight ratio? Front Physiol. 2016;7(FEB):1–13. https://doi.org/10.3389/fphys.2016.00028.
Coan PM, Angiolini E, Sandovici I, Burton GJ, Constância M, Fowden AL. Adaptations in placental nutrient transfer capacity to meet fetal growth demands depend on placental size in mice. J Physiol. 2008;586(18):4567–76. https://doi.org/10.1113/jphysiol.2008.156133.
Lai SK, Wang Y-Y, Hida K, Cone R, Hanes J. Nanoparticles reveal that human cervicovaginal mucus is riddled with pores larger than viruses. Proc Natl Acad Sci. 2010;107(2):598–603. https://doi.org/10.1073/pnas.0911748107.
Sugiyama M, Machida N, Yasunaga A, Terai N, Fukasawa H, Ono HK, Kobayashi R, Nishiyama K, Hashimoto O, Kurusu S, Yoshioka K. Vaginal mucus in mice: developmental and gene expression features of epithelial mucous cells during pregnancy†. Biol Reprod. 2021;105(5):1272–82. https://doi.org/10.1093/biolre/ioab157.
Acknowledgements
The authors thank Shannon Modla for assistance acquiring TEM images and Maneesha Sahni for assistance with Cy5-PEG-PLGA NP synthesis.
Funding
This work was supported by the National Institutes of Health under grant numbers R35GM119659 (ESD), U54GM104941 (ESD, JPG), U19AI158930 (JPG) and T32GM133395 and F31HD105398 (KMN). NIC received support from the University Graduate Scholars Program. TEM access was supported by grants from the NIH-NIGMS P20 GM103446, the NSF (IIA-1301765) and the State of Delaware. The content of this article is solely the responsibility of the authors and does not necessarily reflect the views of the funding agencies.
Author information
Authors and Affiliations
Contributions
All authors contributed to study conception and design. Material preparation, data collection, and analysis were performed by N’Dea Irvin-Choy and Katherine Nelson, co-first authors of this manuscript. The first draft of the manuscript was written by N’Dea Irvin-Choy and Katherine Nelson and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Funding acquisition and project supervision were performed by Emily Day and Jason Gleghorn, the co-corresponding authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Animal studies
All institutional and national guidelines for the care and use of laboratory animals were followed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Irvin-Choy, N.S., Nelson, K.M., Gleghorn, J.P. et al. Delivery and short-term maternal and fetal safety of vaginally administered PEG-PLGA nanoparticles. Drug Deliv. and Transl. Res. 13, 3003–3013 (2023). https://doi.org/10.1007/s13346-023-01369-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-023-01369-w