Abstract
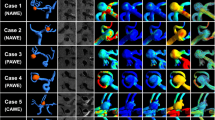
Aneurysm wall remodeling (AWR) is an important pathological characteristic in aneurysm wall, which was characterized by abnormal histological structure and inflammation infiltration. In the present study, the aim is to determine the relationships of morphological-hemodynamic characteristics, inflammation, and AWR in intracranial aneurysms (IAs), as well as the pathological basis of morphological-hemodynamic predictors to achieve IA development. For this end, 113 unruptured IAs were prospectively collected from 110 cases. In addition, patient-specific computational fluid dynamics and geometry were adopted to determine hemodynamic and morphological parameters. Moreover, Hematoxylin-Eosin staining was performed to identify the AWR. By performing immunofluorescence, the inflammatory markers were detected. Masson staining was conducted to characterize the characteristics of atherosclerosis in aneurysm wall. To demonstrate the parameters regarding the AWR, a multivariate logistic analysis was conducted. Besides, correlation analyses were conducted to verify the relationship between morphological-hemodynamic and pathological characteristics. For 113 unruptured IAs, no difference was identified in baseline information. AWR was demonstrated in 92 (81.4%) IAs. To be specific, the aneurysm size (odds ratio (OR), 2.63; confidence interval (CI), 1.04–6.67; P = 0.041), size ratio (SR; OR, 1.95; CI, 1.38–2.76; P < 0.001), normalized wall shear stress average (NWSSA; OR, 0.05; CI, 0.01–0.15; P = 0.007), and relative resident time (RRT; OR, 1.28; CI, 1.07–1.53; P = 0.007) were proved as the factors of AWR. As revealed from the results of immunofluorescence, aneurysm size, SR, NWSSA, and RRT were significantly correlated with the level of inflammation in IA tissues. Furthermore, Masson staining revealed that atherosclerosis area in IA tissues and NWSSA was correlated with RRT. In this study, SR, NWSSA, and RRT were demonstrated as the risk factors of AWR. The mentioned parameters could also reflect the characteristics of inflammation and atherosclerosis in aneurysm wall as well. This study revealed that biomechanical stress and inflammation in aneurysm wall are correlated, which might suggest the pathological evidence of morphological-hemodynamic predictors for IA development.




Similar content being viewed by others
Availability of Data and Material
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
Abbreviations
- IA:
-
Intracranial aneurysm
- UIA:
-
Unruptured intracranial aneurysm
- STA:
-
Superficial temporal artery
- CTA:
-
Computational tomographic angiography
- CFD:
-
Computational fluid dynamics
- S:
-
Aneurysm size
- N:
-
Neck diameter
- H:
-
Perpendicular height
- VA:
-
Vessel angle
- AA:
-
Aneurysm angle
- AR:
-
Aspect ratio
- SR:
-
Size ratio
- NSI:
-
Nonsphericity index
- UI:
-
Undulation index
- WSS:
-
Wall shear stress
- WSSA:
-
Wall shear stress average
- WSSM:
-
Wall shear stress maximum
- PA:
-
Pressure average
- WSSA:
-
Wall shear stress gradient
- NWSSA:
-
Normalized wall shear stress average
- NWSSM:
-
Normalized wall shear stress maximum
- NPA:
-
Normalized pressure average
- LSAR:
-
Low shear area rate
- RRT:
-
Relative resident time
- OSI:
-
Oscillatory shear index
- VA:
-
Vessel angle
- AA:
-
Aneurysm angle
- NFKB1:
-
Nuclear factor-kappa-B 1
- IL-2:
-
Interleukin-2
- MMP-2:
-
Matrix metalloproteinase-2
- MMP-9:
-
Matrix metalloproteinase-9
References
Lawton MT, Vates GE. Subarachnoid hemorrhage. N Engl J Med. 2017;377:257–66.
Li MH, Chen SW, Li YD, Chen YC, Cheng YS, Hu DJ, et al. Prevalence of unruptured cerebral aneurysms in chinese adults aged 35 to 75 years: a cross-sectional study. Ann Intern Med. 2013;159:514–21.
Diagbouga M, Morel S, Bijlenga P, Kwak B. Role of hemodynamics in initiation/growth of intracranial aneurysms. Eur J Clin Investig. 2018;48:e12992.
Frösen J, Tulamo R, Paetau A, Laaksamo E, Korja M, Laakso A, et al. Saccular intracranial aneurysm: pathology and mechanisms. Acta Neuropathol. 2012;123:773–86.
Hosaka K, Hoh B. Inflammation and cerebral aneurysms. Transl Stroke Res. 2014;5:190–8.
Meng H, Tutino VM, **ang J, Siddiqui A. High WSS or low WSS? Complex interactions of hemodynamics with intracranial aneurysm initiation, growth, and rupture: toward a unifying hypothesis. AJNR Am J Neuroradiol. 2014;35:1254–62.
Signorelli F, Sela S, Gesualdo L, Chevrel S, Tollet F, Pailler-Mattei C, et al. Hemodynamic stress, inflammation, and intracranial aneurysm development and rupture: a systematic review. World Neurosurg. 2018;115:234–44.
Tulamo R, Frösen J, Hernesniemi J, Niemelä M. Inflammatory changes in the aneurysm wall: a review. J Neurointerventional Surg. 2018;10:i58–67.
Varble N, Kono K, Rajabzadeh-Oghaz H, Meng H. Rupture resemblance models may correlate to growth rates of intracranial aneurysms: preliminary results. World Neurosurg. 2018;110:e794–805.
**ang J, Natarajan S, Tremmel M, Ma D, Mocco J, Hopkins L, et al. Hemodynamic-morphologic discriminants for intracranial aneurysm rupture. Stroke. 2011;42:144–52.
**ang J, Yu J, Snyder K, Levy E, Siddiqui A, Meng H. Hemodynamic-morphological discriminant models for intracranial aneurysm rupture remain stable with increasing sample size. J Neurointerventional Surg. 2016;8:104–10.
Jiang P, Liu Q, Wu J, Chen X, Li M, Li Z, et al. A novel scoring system for rupture risk stratification of intracranial aneurysms: a hemodynamic and morphological study. Front Neurosci. 2018;12:596.
Liu Q, Jiang P, Wu J, Li M, Gao B, Zhang Y, et al. Intracranial aneurysm rupture score may correlate to the risk of rebleeding before treatment of ruptured intracranial aneurysms. Neurolog Sci : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology. 2019;40:1683–93.
Frösen J, Piippo A, Paetau A, Kangasniemi M, Niemelä M, Hernesniemi J, et al. Remodeling of saccular cerebral artery aneurysm wall is associated with rupture: histological analysis of 24 unruptured and 42 ruptured cases. Stroke. 2004;35:2287–93.
Edjlali M, Gentric J, Régent-Rodriguez C, Trystram D, Hassen W, Lion S, et al. Does aneurysmal wall enhancement on vessel wall mri help to distinguish stable from unstable intracranial aneurysms? Stroke. 2014;45:3704–6.
Gariel F, Ben Hassen W, Boulouis G, Bourcier R, Trystram D, Legrand L, et al. Increased wall enhancement during follow-up as a predictor of subsequent aneurysmal growth. Stroke. 2020;51:1868–72.
Koseki H, Miyata H, Shimo S, Ohno N, Mifune K, Shimano K, et al. Two diverse hemodynamic forces, a mechanical stretch and a high wall shear stress, determine intracranial aneurysm formation. Transl Stroke Res. 2020;11:80–92.
Jiang P, Wu J, Chen X, Ning B, Liu Q, Li Z, et al. Quantitative proteomics analysis of differentially expressed proteins in ruptured and unruptured cerebral aneurysms by iTRAQ. J Proteome. 2018;182:45–52.
Humphrey JD, Schwartz MA, Tellides G, Milewicz DM. Role of mechanotransduction in vascular biology: focus on thoracic aortic aneurysms and dissections. Circ Res. 2015;116:1448–61.
Zhang C, Zhou T, Chen Z, Yan M, Li B, Lv H, et al. Coupling of integrin alpha5 to annexin a2 by flow drives endothelial activation. Circ Res. 2020;127:1074–90.
Tegeler CH, Crutchfield K, Katsnelson M, Kim J, Tang R, Passmore Griffin L, et al. Transcranial doppler velocities in a large, healthy population. J Neuroimaging. 2013;23:466–72.
Greving JP, Wermer MJ, Brown RD Jr, Morita A, Juvela S, Yonekura M, et al. Development of the phases score for prediction of risk of rupture of intracranial aneurysms: a pooled analysis of six prospective cohort studies. Lancet Neurol. 2014;13:59–66.
Cras TY, Bos D, Ikram MA, Vergouwen MDI, Dippel DWJ, Voortman T, et al. Determinants of the presence and size of intracranial aneurysms in the general population: the Rotterdam study. Stroke. 2020;51:2103–10.
Nakajima H, Mochizuki N. Flow pattern-dependent endothelial cell responses through transcriptional regulation. Cell Cycle. 2017;16:1893–901.
Xu X, Yang Y, Wang G, Yin Y, Han S, Zheng D, et al. Low shear stress regulates vascular endothelial cell pyroptosis through mir-181b-5p/stat-3 axis. J Cell Physiol. 2020.
Yang H, Zhu L, Chao Y, Gu Y, Kong X, Chen M, et al. Hyaluronidase2 (hyal2) modulates low shear stress-induced glycocalyx impairment via the lkb1/ampk/nadph oxidase-dependent pathway. J Cell Physiol. 2018;233:9701–15.
Zhu L, Wang F, Yang H, Zhang J, Chen S. Low shear stress damages endothelial function through stat1 in endothelial cells (ECs). J Physiol Biochem. 2020;76:147–57.
Quan K, Song J, Yang Z, Wang D, An Q, Huang L, et al. Validation of wall enhancement as a new imaging biomarker of unruptured cerebral aneurysm. Stroke. 2019;50:1570–3.
Lv N, Karmonik C, Chen S, Wang X, Fang Y, Huang Q, et al. Wall enhancement, hemodynamics, and morphology in unruptured intracranial aneurysms with high rupture risk. Transl Stroke Res. 2020;11:882–9.
Duchene J, Cayla C, Vessillier S, Scotland R, Yamashiro K, Lecomte F, et al. Laminar shear stress regulates endothelial kinin b1 receptor expression and function: potential implication in atherogenesis. Arterioscler Thromb Vasc Biol. 2009;29:1757–63.
Albarran-Juarez J, Iring A, Wang S, Joseph S, Grimm M, Strilic B, et al. Piezo1 and gq/g11 promote endothelial inflammation depending on flow pattern and integrin activation. J Exp Med. 2018;215:2655–72.
Acknowledgements
We thank Jia Liu for providing technical support of computational fluid dynamic analysis.
Funding
This study was supported by the “National Natural Science Foundation of China” (Grant No. 82071296, 81671129, and 81471210) and “Major special projects in the 13th five-year plan” (Grant No. 2016YFC1301800).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics Approval
The work was approved by the Institutional Review Board of Tiantan Hospital (KY2017-076-01).
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, Q., Zhang, Y., Yang, J. et al. The Relationship of Morphological-Hemodynamic Characteristics, Inflammation, and Remodeling of Aneurysm Wall in Unruptured Intracranial Aneurysms. Transl. Stroke Res. 13, 88–99 (2022). https://doi.org/10.1007/s12975-021-00917-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-021-00917-1