Abstract
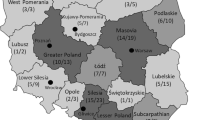
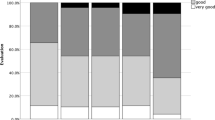
This study aimed to investigate the educational environment of radiotherapy technology and medical physics specialists (RTMP) in Japan. We conducted a nationwide questionnaire survey in radiotherapy institutions between June and August 2022. Participants were asked questions regarding the educational system, perspectives on updating RTMP’s skills and qualifications, and perspectives on higher education for RTMP at radiotherapy institutions. The results were then analyzed in detail according to three factors: whether the hospital was designed for cancer care, whether it was a Japanese Society for Radiation Oncology (JASTRO)-accredited hospital, and whether it was an intensity-modulated radiation therapy charged hospital. Responses were obtained from 579 (69%) nationwide radiation therapy institutions. For non-qualified RTMP, 10% of the institutions had their own educational systems, only 17% of institutions provided on-the-job training, and 84% of institutions encouraged participation in educational lectures and workshops in academic societies. However, for qualified RTMP, 3.0% of institutions had their own educational systems, only 8.9% of the institutions provided on-the-job training, and 83% encouraged participation in academic conferences and workshops. Less than 1% of the facilities offered salary increases for certification, whereas 8.2% offered consideration for occupational promotion. Regarding the educational environment, JASTRO-accredited hospitals were better than general hospitals. Few institutions have their own educational systems for qualified and non-qualified RTMP, but they encourage them to attend educational seminars and conferences. It is desirable to provide systematic education and training by academic and professional organizations to maintain the skills of individuals.




Similar content being viewed by others
References
EBCTCG (Early Breast Cancer Trialists’ Collaborative Group), McGale P, Taylor C, et al. Effect of radiotherapy after mastectomy and axillary surgery on 10-year recurrence and 20-year breast cancer mortality: meta-analysis of individual patient data for 8135 women in 22 randomised trials. Lancet. 2014;383:2127–35.
Vinod SK, Hau E. Radiotherapy treatment for lung cancer: current status and future directions. Respirology. 2020;25(Supplement 2):61–71.
Iwata H, Demizu Y, Fujii O, et al. Long-term outcome of proton therapy and carbon-ion therapy for large (T2a–T2bN0M0) non-small-cell lung cancer. J Thorac Oncol. 2013;8:726–35.
Kamada T, Tsujii H, Blakely EA, et al. Carbon ion radiotherapy in Japan: an assessment of 20 years of clinical experience. Lancet Oncol. 2015;16:e93–100.
Akino Y, Tohyama N, Akita K, et al. Modalities and techniques used for stereotactic radiotherapy, intensity-modulated radiotherapy, and image-guided radiotherapy: a 2018 survey by the Japan Society of Medical Physics. Phys Med. 2019;64:182–7.
Feain IJ, Court L, Palta JR, et al. Innovations in radiotherapy technology. Clin Oncol (R Coll Radiol). 2017;29:120–8.
Numasaki H, Teshima T, Okuda Y, et al. Japanese structure survey of radiation oncology in 2013. J Radiat Res. 2020;61:799–816.
Numasaki H, Nakada Y, Okuda Y, et al. Japanese structure survey of radiation oncology in 2015. J Radiat Res. 2022;63:230–46.
Numasaki H, Teshima T, Nishimura T, et al. Japanese structure survey of radiation oncology in 2010. J Radiat Res. 2019;60:80–97.
Eriksen JG, Beavis AW, Coffey MA, et al. The updated ESTRO core curricula 2011 for clinicians, medical physicists and RTTs in radiotherapy/radiation oncology. Radiother Oncol. 2012;103:103–8.
Dunscombe P, Grau C, Defourny N, et al. Guidelines for equipment and staffing of radiotherapy facilities in the European countries: final results of the ESTRO-HERO survey. Radiother Oncol. 2014;112:165–77.
Bentzen SM, Heeren G, Cottier B, et al. Towards evidence-based guidelines for radiotherapy infrastructure and staffing needs in Europe: the ESTRO QUARTS project. Radiother Oncol. 2005;75:355–65.
Slotman BJ, Cottier B, Bentzen SM, et al. Overview of national guidelines for infrastructure and staffing of radiotherapy. ESTRO-QUARTS: work package 1. Radiother Oncol. 2005;75:349–54.
Di Tella M, Tesio V, Bertholet J, et al. Professional quality of life and burnout among medical physicists working in radiation oncology: the role of alexithymia and empathy. Phys Imaging Radiat Oncol. 2020;15:38–43.
Kadoya N, Karasawa K, Sumida I, et al. Educational outcomes of a medical physicist program over the past 10 years in Japan. J Radiat Res. 2017;58:669–74.
Terashita T, Tamura N, Kisa K, et al. Problem-based learning for radiological technologists: a comparison of student attitudes toward plain radiography. BMC Med Educ. 2016;16:236.
Herman MG, Mills MD, Gillin MT. Reimbursement versus effort in medical physics practice in radiation oncology. J Appl Clin Med Phys. 2003;4:179–87.
Coffey M, Leech M, ESTRO Radiation TherapisT Committee. The European Society of Radiotherapy and Oncology (ESTRO) European Higher Education Area levels 7 and 8 postgraduate benchmarking document for Radiation TherapisTs (RTTs). Tech Innov Patient Support Radiat Oncol. 2018;8:22–40.
Kisling KD, Ger RB, Netherton TJ, et al. A snapshot of medical physics practice patterns. J Appl Clin Med Phys. 2018;19:306–15.
Acknowledgements
We would like to express our deepest gratitude to all radiotherapy institutions in Japan that cooperated with us in this survey.
Funding
This work was supported by a grant from the Ministry of Health, Labor, and Welfare [MHLW grant number 21EA1010].
Author information
Authors and Affiliations
Contributions
NH summarized the data and created the manuscript. MO, MN, and YI summarized the data. NT, KS, and HO created the questionnaire items and analyzed the data. HO supervised the study. All authors discussed the results of this survey.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
This study was approved by the Institutional Ethical Review Board of the National Cancer Center Hospital (2021–476) for collecting data through a national questionnaire.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Hayashi, N., Okumura, M., Nakamura, M. et al. Current status of the educational environment to acquire and maintain the professional skills of radiotherapy technology and medical physics specialists in Japan: a nationwide survey. Radiol Phys Technol 16, 431–442 (2023). https://doi.org/10.1007/s12194-023-00739-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12194-023-00739-w