Abstract
Background
Hypoxemia is the main modifiable factor preventing lungs from being transplanted from organ donors after brain death. One major contributor to impaired oxygenation in patients with brain injury is atelectasis. Apnea testing, an integral component of brain death declaration, promotes atelectasis and can worsen hypoxemia. In this study, we tested whether performing a recruitment maneuver (RM) after apnea testing could mitigate hypoxemia and atelectasis.
Methods
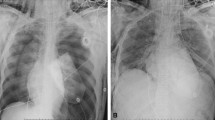
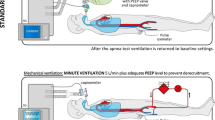
During the study period, an RM (positive end-expiratory pressure of 15 cm H2O for 15 s then 30 cm H2O for 30 s) was performed immediately after apnea testing. We measured partial pressure of oxygen, arterial (PaO2) before and after RM. The primary outcomes were oxygenation (PaO2 to fraction of inspired oxygen [FiO2] ratio) and the severity of radiographic atelectasis (proportion of lung without aeration on computed tomography scans after brain death, quantified using an image analysis algorithm) in those who became organ donors. Outcomes in RM patients were compared with control patients undergoing apnea testing without RM in the previous 2 years.
Results
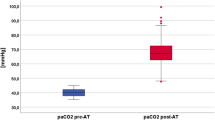
Recruitment maneuver was performed in 54 patients after apnea testing, with a median immediate increase in PaO2 of 63 mm Hg (interquartile range 0–109, p = 0.07). Eighteen RM cases resulted in hypotension, but none were life-threatening. Of this cohort, 37 patients became organ donors, compared with 37 donors who had apnea testing without RM. The PaO2:FiO2 ratio was higher in the RM group (355 ± 129 vs. 288 ± 127, p = 0.03), and fewer had hypoxemia (PaO2:FiO2 ratio < 300 mm Hg, 22% vs. 57%; p = 0.04) at the start of donor management. The RM group showed less radiographic atelectasis (median 6% vs. 13%, p = 0.045). Although there was no difference in lungs transplanted (35% vs. 24%, p = 0.44), both better oxygenation and less atelectasis were associated with a higher likelihood of lungs being transplanted.
Conclusions
Recruitment maneuver after apnea testing reduces hypoxemia and atelectasis in organ donors after brain death. This effect may translate into more lungs being transplanted.


Similar content being viewed by others
References
Greer DM, Shemie SD, Lewis A, et al. Determination of brain death/death by neurologic criteria: the World Brain Death Project. JAMA. 2020;324(11):1078–97.
Wijdicks EF. In search of a safe apnea test in brain death: Is the procedure really more dangerous than we think? Arch Neurol. 1995;52(4):338–9.
Gorton LE, Dhar R, Woodworth L, et al. Pneumothorax as a complication of apnea testing for brain death. Neurocrit Care. 2016;25(2):282–7.
Yee AH, Mandrekar J, Rabinstein AA, Wijdicks EF. Predictors of apnea test failure during brain death determination. Neurocrit Care. 2010;12(3):352–5.
Copeland H, Hayanga JWA, Neyrinck A, et al. Donor heart and lung procurement: a consensus statement. J Heart Lung Transplant. 2020;39(6):501–17.
Ware LB, Landeck M, Koyama T, et al. A randomized trial of the effects of nebulized albuterol on pulmonary edema in brain-dead organ donors. Am J Transplant. 2014;14:621–8.
Dhar R, Stahlschmidt E, Paramesh A, Marklin G. A randomized controlled trial of naloxone for optimization of hypoxemia in lung donors after brain death. Transplantation. 2019;103(7):1433–8.
Valapour M, Lehr CJ, Skeans MA, et al. OPTN/SRTR 2016 annual data report: lung. Am J Transplant. 2018;18(Suppl 1):363–433.
Paries M, Boccheciampe N, Raux M, et al. Benefit of a single recruitment maneuver after an apnea test for the diagnosis of brain death. Crit Care. 2012;16(4):R116.
Chang SH, Kreisel D, Marklin GF, et al. Lung focused resuscitation at a specialized donor care facility improves lung procurement rates. Ann Thorac Surg. 2018;6:66.
Wijdicks EFM, Varelas PN, Gronseth GS, Greer DM. Evidence-based guideline update: determining brain death in adults: report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2010;74:1911–8.
Hofmanninger J, Prayer F, Pan J, et al. Automatic lung segmentation in routine imaging is primarily a data diversity problem, not a methodology problem. Eur Radiol Exp. 2020;4(1):50.
Sato Y, Nakajima S, Shiraga N, et al. Three-dimensional multi-scale line filter for segmentation and visualization of curvilinear structures in medical images. Med Image Anal. 1998;2(2):143–68.
McCormick M, Liu X, Jomier J, Marion C, Ibanez L. ITK: enabling reproducible research and open science. Front Neuroinform. 2014;8:13.
Marklin GF, O’Sullivan C, Dhar R. Ventilation in the prone position improves oxygenation and results in more lungs being transplanted from organ donors with hypoxemia and atelectasis. J Heart Lung Transplant. 2021;40(2):120–7.
Migdady I, Rae-Grant A, Greer DM. Brain death evaluation during the pandemic. Neurology. 2020;95(15):693–4.
Radaideh Y, Garg R, Abdalla AA, et al. Challenges in brain death determination and Apnea testing for patients with COVID-19. J Stroke Cerebrovasc Dis. 2020;29(12): 105419.
Ahlawat A, Carandang R, Heard SO, Muehlschlegel S. The modified Apnea test during brain death determination: an alternative in patients with hypoxia. J Intensive Care Med. 2016;31(1):66–9.
Puri V, Hachem RR, Frye CC, et al. Unintended consequences of changes to lung allocation policy. Am J Transplant. 2019;19(8):2164–7.
Funding
This study was funded by a grant from Mid-America Transplant Foundation Clinical Innovation Fund. RD also received unrelated funding from the National Institutes of Health (K23NS099440, R01NS121218).
Author information
Authors and Affiliations
Contributions
RD and JP conceived of the study. RD conducted the primary analyses. Data were collected by PB, JP, and FL. Study data were reviewed by BA. RD drafted the manuscript, tables, and figures. All authors reviewed and edited the manuscript and approved the final version.
Corresponding author
Ethics declarations
Conflicts of interest
RD reports consulting fees from Marinus Pharma and Mid-America Transplant.
Ethical Approval/Informed Consent
All research was conducted under approval of the institutional ethics review board, deemed as exempt from consent given this was a study involving only deceased patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dhar, R., Braun, P., Kumar, A. et al. A Recruitment Maneuver After Apnea Testing Improves Oxygenation and Reduces Atelectasis in Organ Donors After Brain Death. Neurocrit Care (2024). https://doi.org/10.1007/s12028-024-01975-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12028-024-01975-7