Abstract
Purpose
Accumulating evidence suggests that serum uric acid (SUA) plays a beneficial role in bone health in the general population through antioxidant mechanisms. However, there is controversy over the association between SUA and bone in patients with type 2 diabetes mellitus (T2DM). We aimed to investigate the association of serum UA with BMDs and future fracture risks and its potential influencing factors in those patients.
Method
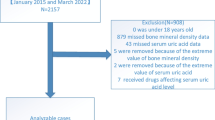
This was a cross-sectional study of 485 patients. BMDs at femoral neck (FN), Troch and the lumbar spine (LS) were measured by DXA. The 10-year probability of fracture risk was assessed using the fracture risk assessment tool (FRAX). SUA level and other biochemical indexes were measured.
Results
There were lower SUA concentrations in patients with osteoporosis/osteopenia compared with those in the normal group, which only existed in non-elderly men and elderly women with T2DM. After adjustment for potential confounders, SUA was positively associated with BMD and negatively with 10-year probability of fracture risk only in non-elderly men and elderly women with T2DM. Multiple stepwise regression analysis showed that SUA was an independent determinant of BMD and 10-year probability of fracture risk, which also occurred in the above patients.
Conclusion
These results implied that relatively high SUA is a protective factor for bone in T2DM patients, but the osteoprotective effect of SUA was mediated by age and gender, and persisted only in non-elderly men and elderly women. Large intervention studies are needed to further confirm the outcomes and provide possible explanations.

Similar content being viewed by others
Data availability
The data used to support the findings of this study are available from the authors upon request.
References
K. Siggeirsdottir, T. Aspelund, B.Y. Jonsson, B. Mogensen, L.J. Launer, T.B. Harris, G. Sigurdsson, V. Gudnason, Effect of vertebral fractures on function, quality of life and hospitalisation the AGES-Reykjavik study. Age Ageing 41(3), 351–357 (2012). https://doi.org/10.1093/ageing/afs003
C.J. Crandall, V.O. Yildiz, J. Wactawski-Wende, K.C. Johnson, Z. Chen, S.B. Going, N.C. Wright, J.A. Cauley, Postmenopausal weight change and incidence of fracture: post hoc findings from Women’s Health Initiative Observational Study and Clinical Trials. BMJ 350, h25 (2015). https://doi.org/10.1136/bmj.h25
H. Nimitphong, N. Siwasaranond, C. Sritara, S. Saetung, L.O. Chailurkit, N. Chirakalwasan, B. Ongphiphadhanakul, S. Reutrakul, The differences in the relationship between obstructive sleep apnea severity and trabecular bone score in men and women with type 2 diabetes. J. Clin. Transl. Endocrinol. 16, 100193 (2019). https://doi.org/10.1016/j.jcte.2019.100193
S.A. Abdulameer, S.A. Sulaiman, M.A. Hassali, K. Subramaniam, M.N. Sahib, Osteoporosis and type 2 diabetes mellitus: what do we know, and what we can do? Patient Prefer Adherence 6, 435–448 (2012). https://doi.org/10.2147/PPA.S32745
L. Billings, Y. Hsu, R. Ackerman, J. Dupuis, B. Voight, L. Rasmussen-Torvik, S. Hercberg, M. Lathrop, D. Barnes, C. Langenberg et al. Impact of common variation in bone-related genes on type 2 diabetes and related traits. Diabetes 61(8), 2176–2186 (2012). https://doi.org/10.2337/db11-1515
S. Wen, D. Wang, H. Yu, M. Liu, Q. Chen, R. Bao, L. Liu, Y. Zhang, T. Wang, The time-feature of uric acid excretion in hyperuricemia mice induced by potassium oxonate and adenine. Int. J. Mol. Sci. 21(15), (2020). https://doi.org/10.3390/ijms21155178.
D. Yan, J. Wang, X. Hou, Y. Bao, Z. Zhang, C. Hu, W. Jia, Association of serum uric acid levels with osteoporosis and bone turnover markers in a Chinese population. Acta Pharmacol. Sin. 39(4), 626–632 (2018). https://doi.org/10.1038/aps.2017.165
X. Lin, C. Zhao, A. Qin, D. Hong, W. Liu, K. Huang, J. Mo, H. Yu, S. Wu, S. Fan, Association between serum uric acid and bone health in general population: a large and multicentre study. Oncotarget 6(34), 35395–35403 (2015). https://doi.org/10.18632/oncotarget.6173
W. Han, X. Bai, N. Wang, L. Han, X. Sun, X. Chen, Association between lumbar bone mineral density and serum uric acid in postmenopausal women: a cross-sectional study of healthy Chinese population. Arch. Osteoporos. 12(1), 50 (2017). https://doi.org/10.1007/s11657-017-0345-0
S. Ishii, M. Miyao, Y. Mizuno, M. Tanaka-Ishikawa, M. Akishita, Y. Ouchi, Association between serum uric acid and lumbar spine bone mineral density in peri- and postmenopausal Japanese women. Osteoporos. Int 25(3), 1099–1105 (2014). https://doi.org/10.1007/s00198-013-2571-7
J. Hwang, J.H. Hwang, S. Ryu, J.K. Ahn, Higher serum uric acid is associated with higher lumbar spine bone mineral density in male health-screening examinees: a cross-sectional study. J. Bone Min. Metab. 37(1), 142–151 (2019). https://doi.org/10.1007/s00774-018-0905-4
M.E. Kuyumcu, Y. Yesil, Z.A. Ozturk, E. Cinar, C. Kizilarslanoglu, M. Halil, Z. Ulger, N.K. Yesil, M. Cankurtaran, S. Ariogul, The association between homocysteine (hcy) and serum natural antioxidants in elderly bone mineral densitometry (BMD. Arch. Gerontol. Geriatr. 55, 739–743 (2012). https://doi.org/10.1016/j.archger.2012.05.004
T. Muka, E.A. de Jonge, J.C. Kiefte-de Jong, A.G. Uitterlinden, A. Hofman, A. Dehghan, M.C. Zillikens, O.H. Franco, F: Rivadeneira, The influence of serum uric acid on bone mineral density, hip geometry, and fracture risk: the Rotterdam study. J. Clin. Endocrinol. Metab. 101(3), 1113–1122 (2016). https://doi.org/10.1210/jc.2015-2446
D. Zhang, I.A. Bobulescu, N.M. Maalouf, B. Adams-Huet, J. Poindexter, S. Park, F. Wei, C. Chen, O.W. Moe, K. Sakhaee, Relationship between serum uric Acid and bone mineral density in the general population and in rats with experimental hyperuricemia. J. Bone Min. Res 30(6), 992–999 (2015). https://doi.org/10.1002/jbmr.2430
N. Veronese, F. Bolzetta, M. De Rui, S. Maggi, M. Noale, S. Zambon, M.C. Corti, E.D. Toffanello, G. Baggio, E. Perissinotto et al. Serum uric acid and incident osteoporotic fractures in old people: the PRO.V.A study. Bone 79, 183–189 (2015). https://doi.org/10.1016/j.bone.2015.06.005
Y.Y. Sautin, R.J. Johnson, Uric acid: the oxidant-antioxidant paradox. Nucleosides Nucleotides Nucleic Acids 27(6), 608–619 (2008). https://doi.org/10.1080/15257770802138558
M. Kanbay, T. Jensen, Y. Solak, M. Le, C. Roncal-Jimenez, C. Rivard, M.A. Lanaspa, T. Nakagawa, R.J. Johnson, Uric acid in metabolic syndrome: from an innocent bystander to a central player. Eur. J. Intern Med 29, 3–8 (2016). https://doi.org/10.1016/j.ejim.2015.11.026
W. Baldwin, S. McRae, G. Marek, D. Wymer, V. Pannu, C. Baylis, R. Johnson, Y. Sautin, Hyperuricemia as a mediator of the proinflammatory endocrine imbalance in the adipose tissue in a murine model of the metabolic syndrome. Diabetes 60(4), 1258–1269 (2011). https://doi.org/10.2337/db10-0916
W.G. Lima, M.E. Martins-Santos, V.E. Chaves, Uric acid as a modulator of glucose and lipid metabolism. Biochimie 116, 17–23 (2015). https://doi.org/10.1016/j.biochi.2015.06.025
Y. Ma, H. Cao, Z. Li, J. Fang, X. Wei, P. Cheng, R. Jiao, X. Liu, Y. Li, Y. **ng, et al. A novel multi-epitope vaccine based on urate transporter 1 alleviates streptozotocin-induced diabetes by producing anti-URAT1 antibody and an immunomodulatory effect in C57BL/6J mice. Int J Mol Sci. 18(10) (2017). https://doi.org/10.3390/ijms18102137.
P. Yan, Z. Zhang, Q. Wan, J. Zhu, H. Li, C. Gao, H. Ma, Y. Xu, Association of serum uric acid with bone mineral density and clinical fractures in Chinese type 2 diabetes mellitus patients: a cross-sectional study. Clin. Chim. Acta 486, 76–85 (2018). https://doi.org/10.1016/j.cca.2018.07.033
J.G. Jones, Hepatic glucose and lipid metabolism. Diabetologia 59(6), 1098–1103 (2016). https://doi.org/10.1007/s00125-016-3940-5
H. Johansson, J.A. Kanis, A. Oden, O. Johnell, E. McCloskey, BMD, clinical risk factors and their combination for hip fracture prevention. Osteoporos. Int 20(10), 1675–1682 (2009). https://doi.org/10.1007/s00198-009-0845-x
R. Eastell, C.J. Rosen, D.M. Black, A.M. Cheung, M.H. Murad, D. Shoback, Pharmacological management of osteoporosis in postmenopausal women: an endocrine society* clinical practice guideline. J. Clin. Endocrinol. Metab. 104(5), 1595–1622 (2019). https://doi.org/10.1210/jc.2019-00221
N.E. Lane, N. Parimi, L.Y. Lui, B.L. Wise, W. Yao, Y.A. Lay, P.M. Cawthon, E. Orwoll, Osteoporotic fractures in men study G: association of serum uric acid and incident nonspine fractures in elderly men: the Osteoporotic Fractures in Men (MrOS) study. J. Bone Min. Res 29(7), 1701–1707 (2014). https://doi.org/10.1002/jbmr.2164
A. Zengin, A. Prentice, K.A. Ward, Ethnic differences in bone health. Front. Endocrinol. 6, 24 (2015). https://doi.org/10.3389/fendo.2015.00024
M. Musumeci, G. Vadala, G. Tringali, E. Insirello, A.M. Roccazzello, J. Simpore, S. Musumeci, Genetic and environmental factors in human osteoporosis from Sub-Saharan to Mediterranean areas. J. Bone Min. Metab. 27(4), 424–434 (2009). https://doi.org/10.1007/s00774-009-0041-2
W.D. Leslie, Clinical review: ethnic differences in bone mass–clinical implications. J. Clin. Endocrinol. Metab. 97(12), 4329–4340 (2012). https://doi.org/10.1210/jc.2012-2863
S. Lei, Y. Chen, D. **ong, L. Li, H. Deng, Ethnic difference in osteoporosis-related phenotypes and its potential underlying genetic determination. J. Musculoskelet. Neuronal Interact. 6(1), 36–46 (2006)
J. Anderson, W. Pollitzer, Ethnic and genetic differences in susceptibility to osteoporotic fractures. Adv. Nutr. Res. 9, 129–149 (1994). https://doi.org/10.1007/978-1-4757-9092-4_8
J. Makovey, M. Macara, J.S. Chen, C.S. Hayward, L. March, M.J. Seibel, P.N. Sambrook, Serum uric acid plays a protective role for bone loss in peri- and postmenopausal women: a longitudinal study. Bone 52(1), 400–406 (2013). https://doi.org/10.1016/j.bone.2012.10.025
G. Glantzounis, E. Tsimoyiannis, A. Kappas, D. Galaris, Uric acid and oxidative stress. Curr. Pharm. Des. 11(32), 4145–4151 (2005). https://doi.org/10.2174/138161205774913255
D.D. Zhao, P.L. Jiao, J.J. Yu, X.J. Wang, L. Zhao, Y. Xuan, L.H. Sun, B. Tao, W.Q. Wang, G. Ning et al. Higher serum uric acid is associated with higher bone mineral density in chinese men with type 2 diabetes mellitus. Int J. Endocrinol. 2016, 2528956 (2016). https://doi.org/10.1155/2016/2528956
M. Xu, J. Su, J. Hao, N. Zhong, Z. Zhang, R. Cui, F. Li, C. Sheng, G. Zhang, H. Sheng et al. Positive association between serum uric acid and bone mineral density in Chinese type 2 diabetes mellitus stratified by gender and BMI. J. Bone Min. Metab. 36(5), 609–619 (2018). https://doi.org/10.1007/s00774-017-0877-9
K. Yang, H. Miao, R. Zhao, X. Wu, B. Liu, S. Zheng, D. Huang, Z. **, Association between serum uric acid and bone mineral density in patients with type 2 diabetes: a 6-year longitudinal study in China. Medicine 100(17), e25733 (2021). https://doi.org/10.1097/MD.0000000000025733
K.S. Ruth, F.R. Day, J. Tyrrell, D.J. Thompson, A.R. Wood, A. Mahajan, R.N. Beaumont, L. Wittemans, S. Martin, A.S. Busch et al. Using human genetics to understand the disease impacts of testosterone in men and women. Nat. Med. 26(2), 252–258 (2020). https://doi.org/10.1038/s41591-020-0751-5
L. Chan, B.W. O’Malley, Mechanism of action of the sex steroid hormones (first of three parts). N. Engl. J. Med. 294(24), 1322–1328 (1976). https://doi.org/10.1056/nejm197606102942405
S. Harman, E. Metter, J. Tobin, J. Pearson, M. Blackman, Longitudinal effects of aging on serum total and free testosterone levels in healthy men. Baltimore Longitudinal Study of Aging. J. Clin. Endocrinol. Metabol. 86(2), 724–731 (2001). https://doi.org/10.1210/jcem.86.2.7219
E.L. Rhoden, E.P. Ribeiro, C. Teloken, C.A. Souto, Diabetes mellitus is associated with subnormal serum levels of free testosterone in men. BJU Int. 96(6), 867–870 (2005). https://doi.org/10.1111/j.1464-410X.2005.05728.x
L.Y. **, Z.D. Lv, K. Wang, L. Qian, X.X. Song, X.F. Li, H.X. Shen, Estradiol alleviates intervertebral disc degeneration through modulating the antioxidant enzymes and inhibiting autophagy in the model of menopause rats. Oxid. Med. Cell Longev. 2018, 7890291 (2018). https://doi.org/10.1155/2018/7890291
L. Chen, G. Wang, Q. Wang, Q. Liu, Q. Sun, L. Chen, N-acetylcysteine prevents orchiectomy-induced osteoporosis by inhibiting oxidative stress and osteocyte senescence. Am. J. Transl. Res. 11(7), 4337–4347 (2019)
J.R. Perry, M.N. Weedon, C. Langenberg, A.U. Jackson, V. Lyssenko, T. Sparso, G. Thorleifsson, H. Grallert, L. Ferrucci, M. Maggio et al. Genetic evidence that raised sex hormone binding globulin (SHBG) levels reduce the risk of type 2 diabetes. Hum. Mol. Genet 19(3), 535–544 (2010). https://doi.org/10.1093/hmg/ddp522
Author contributions
J.X. and Y.-M.Z. contributed to study design, interpretation of data for the work, literature search; N.X. contributed to the data collection, analysis and writing of the manuscript. Y.W., Y.C., Y.-N.G., R.-X.L. contributed to the data collection, J.X. and Y.-M.Z. contributed equally as co-corresponding authors of this paper.
Funding
This work was support by the Taishan Scholar Construction Project Special Funding (Grant number.TS201712092), Shandong Provincial Natural Science Foundation (Grant number. ZR2020MH111), National Natural Science Foundation of China (Grant number. 82100937), and Shandong Provincial Natural Science Foundation (Grant number. ZR2021QH132).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Institutional Review Board of Shandong Provincial Hospital affiliated with Shandong First Medical University (SWYX: NO.2022-451).
Informed consent
All participants signed an informed consent.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xu, N., Wang, Y., Chen, Y. et al. The associations between uric acid with BMDs and risk of the 10-year probability of fractures in Chinese patients with T2DM stratified by age and gender. Endocrine 80, 520–528 (2023). https://doi.org/10.1007/s12020-023-03353-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-023-03353-3