Abstract
Human mesenchymal stem cells are a promising cell source for the treatment of stroke. Their primary mechanism of action occurs via neuroprotective effects by trophic factors, anti-inflammatory effects, and immunomodulation. However, the regeneration of damaged neuronal networks by cell transplantation remains challenging. We hypothesized that cells induced to neural lineages would fit the niche, replace the lesion, and be more effective in improving symptoms compared with stem cells themselves. We investigated the characteristics of induced neural cells from human dental pulp tissue and compared the transplantation effects between these induced neural cells and uninduced dental pulp stem cells. Induced neural cells or dental pulp stem cells were intracerebrally transplanted 5 days after cerebral infarction induced by permanent middle cerebral artery occlusion in immunodeficient mice. Effects on functional recovery were also assessed through behavior testing. We used immunohistochemistry and neuron tracing to analyze the differentiation, axonal extension, and connectivity of transplanted cells to the host’s neural circuit. Transplantation of induced neural cells from human dental pulp ameliorated functional recovery after cerebral infarction compared with dental pulp stem cells. The induced neural cells comprised both neurons and glia and expressed functional voltage, and they were more related to neurogenesis in terms of transcriptomics. Induced neural cells had a higher viability than did dental pulp stem cells in hypoxic culture. We showed that induced neural cells from dental pulp tissue offer a novel therapeutic approach for recovery after cerebral infarction.
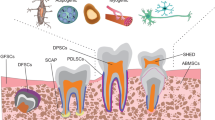
Graphic Abstract







Similar content being viewed by others
Data Availability
Data supporting the findings of this study are available from the corresponding author upon reasonable request. Microarray data discussed in this publication have been deposited in NCBI’s Gene Expression Omnibus (GEO, http://www.ncbi.nlm.nih.gov/geo/) and are accessible through GEO Series accession number GSE174260.
References
Virani, S. S., Alonso, A., Benjamin, E. J., Bittencourt, M. S., Callaway, C. W., & Carson, A. P. (2020). Heart disease and stroke statistics-2020 update: A report from the American Heart Association. Circulation, 141(9), e139–e596. https://doi.org/10.1161/CIR.0000000000000757
Hess, D. C., Wechsler, L. R., Clark, W. M., Savitz, S. I., Ford, G. A., Chiu, D., & Mays, R. W. (2017). Safety and efficacy of multipotent adult progenitor cells in acute ischaemic stroke (masters): A randomised, double-blind, placebo-controlled, phase 2 trial. Lancet Neurology, 16(5), 360–368. https://doi.org/10.1016/S1474-4422(17)30046-7
Steinberg, G. K., Kondziolka, D., Wechsler, L. R., Lunsford, L. D., Coburn, M. L., Billigen, J. B., & Schwartz, N. E. (2016). Clinical outcomes of transplanted modified bone marrow-derived mesenchymal stem cells in stroke: A phase 1/2a study. Stroke, 47(7), 1817–1824. https://doi.org/10.1161/STROKEAHA.116.012995
Grade, S., & Götz, M. (2017). Neuronal replacement therapy: Previous achievements and challenges ahead. npj Regenerative Medicine, 2, 29. https://doi.org/10.1038/s41536-017-0033-0
Kikuchi, T., Morizane, A., Doi, D., Magotani, H., Onoe, H., Hayashi, T., & Takahashi, J. (2017). Human iPS cell-derived dopaminergic neurons function in a primate Parkinson’s disease model. Nature, 548(7669), 592–596. https://doi.org/10.1038/nature23664
Kawaguchi, S., Soma, Y., Nakajima, K., Kanazawa, H., Tohyama, S., Tabei, R., & Fujita, J. (2021). Intramyocardial transplantation of human iPS cell-derived cardiac spheroids improves cardiac function in heart failure animals. JACC: Basic to Translational Science, 6(3), 239–254. https://doi.org/10.1016/j.jacbts.2020.11.017
Kalladka, D., Sinden, J., Pollock, K., Haig, C., McLean, J., Smith, W., & Muir, K. W. (2016). Human neural stem cells in patients with chronic ischaemic stroke (PISCES): A phase 1, first-in-man study. Lancet, 388(10046), 787–796. https://doi.org/10.1016/s0140-6736(16)30513-x
Oki, K., Tatarishvili, J., Wood, J., Koch, P., Wattananit, S., Mine, Y., & Kokaia, Z. (2012). Human-induced pluripotent stem cells form functional neurons and improve recovery after grafting in stroke-damaged brain. Stem Cells, 30(6), 1120–1133. https://doi.org/10.1002/stem.1104
Cui, L. L., Golubczyk, D., Tolppanen, A. M., Boltze, J., & Jolkkonen, J. (2019). Cell therapy for ischemic stroke: Are differences in preclinical and clinical study design responsible for the translational loss of efficacy? Annals of Neurology, 86(1), 5–16. https://doi.org/10.1002/ana.25493
Mayor, R., & Theveneau, E. (2013). The neural crest. Development, 140(11), 2247–2251. https://doi.org/10.1242/dev.091751
Gronthos, S., Mankani, M., Brahim, J., Robey, P. G., & Shi, S. (2000). Postnatal human dental pulp stem cells (dpscs) in vitro and in vivo. Proceedings of the National Academy of Sciences of the United States of America, 97(25), 13625–13630. https://doi.org/10.1073/pnas.240309797
Yalvac, M. E., Ramazanoglu, M., Rizvanov, A. A., Sahin, F., Bayrak, O. F., Salli, U., & Kose, G. T. (2010). Isolation and characterization of stem cells derived from human third molar tooth germs of young adults: Implications in neo-vascularization, osteo-, adipo- and neurogenesis. Pharmacogenomics Journal, 10(2), 105–113. https://doi.org/10.1038/tpj.2009.40
Alge, D. L., Zhou, D., Adams, L. L., Wyss, B. K., Shadday, M. D., Woods, E. J., & Goebel, W. S. (2010). Donor-matched comparison of dental pulp stem cells and bone marrow-derived mesenchymal stem cells in a rat model. Journal of Tissue Engineering and Regenerative Medicine, 4(1), 73–81. https://doi.org/10.1002/term.220
Nito, C., Sowa, K., Nakajima, M., Sakamoto, Y., Suda, S., Nishiyama, Y., & Kimura, K. (2018). Transplantation of human dental pulp stem cells ameliorates brain damage following acute cerebral ischemia. Biomedicine & Pharmacotherapy, 108, 1005–1014. https://doi.org/10.1016/j.biopha.2018.09.084
Raza, S. S., Wagner, A. P., Hussain, Y. S., & Khan, M. A. (2018). Mechanisms underlying dental-derived stem cell-mediated neurorestoration in neurodegenerative disorders. Stem Cell Research and Therapy, 9(1), 245. https://doi.org/10.1186/s13287-018-1005-z
Song, M., Lee, J. H., Bae, J., Bu, Y., & Kim, E. C. (2017). Human dental pulp stem cells are more effective than human bone marrow-derived mesenchymal stem cells in cerebral ischemic injury. Cell Transplantation, 26(6), 1001–1016. https://doi.org/10.3727/096368916X694391
Leong, W. K., Henshall, T. L., Arthur, A., Kremer, K. L., Lewis, M. D., Helps, S. C., & Koblar, S. A. (2012). Human adult dental pulp stem cells enhance poststroke functional recovery through non-neural replacement mechanisms. Stem Cells Translational Medicine, 1(3), 177–187. https://doi.org/10.5966/sctm.2011-0039
Karaöz, E. (2011). Human dental pulp stem cells demonstrate better neural and epithelial stem cell properties than bone marrow-derived mesenchymal stem cells. Histochemistry and Cell Biology, 136(4), 455–473. https://doi.org/10.1007/s00418-011-0858-3
Kumar, A., Kumar, V., Rattan, V., Jha, V., & Bhattacharyya, S. (2017). Secretome cues modulate the neurogenic potential of bone marrow and dental stem cells. Molecular Neurobiology, 54(6), 4672–4682. https://doi.org/10.1007/s12035-016-0011-3
Takahashi, H., Ishikawa, H., & Tanaka, A. (2017). Regenerative medicine for Parkinson’s disease using differentiated nerve cells derived from human buccal fat pad stem cells. Human Cell, 30(2), 60–71. https://doi.org/10.1007/s13577-017-0160-3
Yuan, S. H., Martin, J., Elia, J., Flippin, J., Paramban, R. I., Hefferan, M. P., & Carson, C. T. (2011). Cell-surface marker signatures for the isolation of neural stem cells, glia and neurons derived from human pluripotent stem cells. PLoS ONE, 6(3), e17540. https://doi.org/10.1371/journal.pone.0017540
Schneider, C. A., Rasband, W. S., & Eliceiri, K. W. (2012). Nih image to ImageJ: 25 years of image analysis. Nature Methods, 9(7), 671–675. https://doi.org/10.1038/nmeth.2089
Prentice, J. S., Homann, J., Simmons, K. D., Tkačik, G., Balasubramanian, V., & Nelson, P. C. (2011). Fast, scalable, bayesian spike identification for multi-electrode arrays. PLoS ONE, 6(7), e19884. https://doi.org/10.1371/journal.pone.0019884
Sherman, B. T., & Lempicki, R. A. (2009). Systematic and integrative analysis of large gene lists using David bioinformatics resources. Nature Protocols, 4(1), 44–57. https://doi.org/10.1038/nprot.2008.211
Taguchi, A., Kasahara, Y., Nakagomi, T., Stern, D. M., Fukunaga, M., Ishikawa, M., & Matsuyama, T. (2010). A reproducible and simple model of permanent cerebral ischemia in cb-17 and scid mice. Journal of Experimental Stroke and Translational Medicine, 3(1), 28–33. https://doi.org/10.6030/1939-067x-3.1.28
Roome, R. B., & Vanderluit, J. L. (2015). Paw-dragging: A novel, sensitive analysis of the mouse cylinder test. Journal of Visualized Experiments: JoVE, 98(98), e52701. https://doi.org/10.3791/52701
Mei, T., Kim, A., Vong, L. B., Marushima, A., Puentes, S., Matsumaru, Y., & Nagasaki, Y. (2019). Encapsulation of tissue plasminogen activator in ph-sensitive self-assembled antioxidant nanoparticles for ischemic stroke treatment—Synergistic effect of thrombolysis and antioxidant. Biomaterials, 215, 119209. https://doi.org/10.1016/j.biomaterials.2019.05.020
Brundin, P., Karlsson, J., Emgård, M., Schierle, G. S., Hansson, O., Petersén, A., & Castilho, R. F. (2000). Improving the survival of grafted dopaminergic neurons: A review over current approaches. Cell Transplantation, 9(2), 179–195. https://doi.org/10.1177/096368970000900205
Sakai, K., Yamamoto, A., Matsubara, K., Nakamura, S., Naruse, M., Yamagata, M., & Ueda, M. (2012). Human dental pulp-derived stem cells promote locomotor recovery after complete transection of the rat spinal cord by multiple neuro-regenerative mechanisms. Journal of Clinical Investigation, 122(1), 80–90. https://doi.org/10.1172/jci59251
Nuti, N., Corallo, C., Chan, B. M. F., Ferrari, M., & Gerami-Naini, B. (2016). Multipotent differentiation of human dental pulp stem cells: A literature review. Stem Cell Reviews and Reports, 12(5), 511–523. https://doi.org/10.1007/s12015-016-9661-9
Kandasamy, M., Lehner, B., Kraus, S., Sander, P. R., Marschallinger, J., Rivera, F. J., & Aigner, L. (2014). TGF-beta signalling in the adult neurogenic niche promotes stem cell quiescence as well as generation of new neurons. Journal of Cellular and Molecular Medicine, 18(7), 1444–1459. https://doi.org/10.1111/jcmm.12298
Close, J. L., Gumuscu, B., & Reh, T. A. (2005). Retinal neurons regulate proliferation of postnatal progenitors and Müller glia in the rat retina via tgf beta signaling. Development, 132(13), 3015–3026. https://doi.org/10.1242/dev.01882
Pineda, J. R., Daynac, M., Chicheportiche, A., Cebrian-Silla, A., Sii Felice, K., Garcia-Verdugo, J. M., & Mouthon, M. A. (2013). Vascular-derived TGF-β increases in the stem cell niche and perturbs neurogenesis during aging and following irradiation in the adult mouse brain. EMBO Molecular Medicine, 5(4), 548–562. https://doi.org/10.1002/emmm.201202197
Wachs, F. P., Winner, B., Couillard-Despres, S., Schiller, T., Aigner, R., Winkler, J., & Aigner, L. (2006). Transforming growth factor-beta1 is a negative modulator of adult neurogenesis. Journal of Neuropathology and Experimental Neurology, 65(4), 358–370. https://doi.org/10.1097/01.jnen.0000218444.53405.f0
Ghashghaei, H. T., Weimer, J. M., Schmid, R. S., Yokota, Y., McCarthy, K. D., Popko, B., & Anton, E. S. (2007). Reinduction of erbb2 in astrocytes promotes radial glial progenitor identity in adult cerebral cortex. Genes and Development, 21(24), 3258–3271. https://doi.org/10.1101/gad.1580407
Patten, B. A., Peyrin, J. M., Weinmaster, G., & Corfas, G. (2003). Sequential signaling through notch1 and erbb receptors mediates radial glia differentiation. Journal of Neuroscience, 23(14), 6132–6140. https://doi.org/10.1523/JNEUROSCI.23-14-06132.2003
**nou, H., Sawada, M., Kawase, K., Kaneko, N., Herranz-Pérez, V., Miyamoto, T., & Sawamoto, K. (2018). Radial glial fibers promote neuronal migration and functional recovery after neonatal brain injury. Cell Stem Cell, 22(1), 128-137.e9. https://doi.org/10.1016/j.stem.2017.11.005
Herculano-Houzel, S. (2014). The glia/neuron ratio: How it varies uniformly across brain structures and species and what that means for brain physiology and evolution. Glia, 62(9), 1377–1391. https://doi.org/10.1002/glia.22683
Zhang, Q., & Haydon, P. G. (2005). Roles for gliotransmission in the nervous system. Journal of Neural Transmission, 112(1), 121–125. https://doi.org/10.1007/s00702-004-0119-x
Ye, Y., Zeng, Y. M., Wan, M. R., & Lu, X. F. (2011). Induction of human bone marrow mesenchymal stem cells differentiation into neural-like cells using cerebrospinal fluid. Cell Biochemistry and Biophysics, 59(3), 179–184. https://doi.org/10.1007/s12013-010-9130-z
Ponnaiyan, D., & Jegadeesan, V. (2014). Comparison of phenotype and differentiation marker gene expression profiles in human dental pulp and bone marrow mesenchymal stem cells. European Journal of Dentistry, 8(3), 307–313. https://doi.org/10.4103/1305-7456.137631
Yamashita, T., Kawai, H., Tian, F., Ohta, Y., & Abe, K. (2011). Tumorigenic development of induced pluripotent stem cells in ischemic mouse brain. Cell Transplantation, 20(6), 883–891. https://doi.org/10.3727/096368910x539092
Acknowledgements
We thank Dr. Murakoshi and Dr. Okabe from the Department of Cardiology, University of Tsukuba for a data acquirement of the multielectrode array, Ms. Tsukada and Ms. Miyakawa from Graduate School of Comprehensive Human Sciences, University of Tsukuba for their technical support.
Funding
This work was supported by Grant-in-Aid for Scientific Research (C) for Yuji Matsumaru (No. 19K09450), Scientific Research (B) for Aiki Marushima (no. 20H03787), and Grant-in-Aid for JSPS Fellows for Hideaki Matsumura (no. 20J12956) from the Japan Society for the Promotion of Science (JSPS), supported by Translational Research Program (University of Tsukuba, A18-36) for the Japan Agency for Medical Research and Development for Aiki Marushima.
Author information
Authors and Affiliations
Contributions
HM, AM, HI conceived and designed the experiments. HM, HI, JT, AO, MW, and ST performed the experiments and analyzed the data. Hideaki Matsumura wrote the manuscript. AM, HI, HB, AM, YM, and EI investigated and supervised the experiment. All authors read and approved the final version of the manuscript. All authors revised and approved the manuscript that must be published and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work is appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Ethical Approval
The Ethics Committee of the University of Tsukuba Hospital approved this study (Approval Number: H30-181). The Institutional Animal Care and Use Committee of the University of Tsukuba approved all experimental mouse studies (Approval Number: 18-108).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file2 (MOV 5442 kb)
Rights and permissions
About this article
Cite this article
Matsumura, H., Marushima, A., Ishikawa, H. et al. Induced Neural Cells from Human Dental Pulp Ameliorate Functional Recovery in a Murine Model of Cerebral Infarction. Stem Cell Rev and Rep 18, 595–608 (2022). https://doi.org/10.1007/s12015-021-10223-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-021-10223-w