Abstract
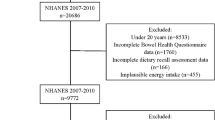
Iron may be involved in the etiology of inflammatory bowel disease (IBD) and chronic diarrhea by modulating gut microbiota and immune responses, but data from epidemiological studies in adults examining this relationship are limited. Thus, the aim of this study was to evaluate the association between iron intake and serum iron levels with IBD and chronic diarrhea in adults. Data from the National Health and Nutritional Examination Surveys (NHANES) between 2007 and 2010 for adults ≥ 20 years were obtained. Chronic diarrheal symptoms were determined by using the 2007–2010 NHANES questionnaire which included questions pertaining to bowel health. The presence of IBD was analyzed from the NHANES data, directly querying the presence or absence of ulcerative colitis (UC) and Crohn’s disease (CD). A total of 9605 participants were initially included in this study. Multivariable logistic regression analysis was used and stratified by gender. Compared with quartile 1 (the lowest quartile), the multivariate-adjusted ORs (95% CI) for risk of having chronic diarrheal symptoms were 1.01 (0.86–1.18), 1.29 (1.07–1.56) and 1.25 (1.02–1.54) across quartiles 2 to 4 of iron intake. This significant association remained among men, but not among women in subgroup analyses. No significant association between either iron intake or serum iron level and the risk of IBD was observed. Generally, there was a positive association between iron intake and chronic diarrheal symptoms in adults that was modified by sex.

Similar content being viewed by others
Data Availability
The data of this study will be made available on reasonable request.
References
Kappelman MD, Rifas-Shiman SL, Kleinman K, Ollendorf D, Bousvaros A, Grand RJ, Finkelstein JA (2007) The prevalence and geographic distribution of Crohn’s disease and ulcerative colitis in the United States. Clin Gastroenterol Hepatol 5(12):1424–1429. https://doi.org/10.1016/j.cgh.2007.07.012
Ganz ML, Sugarman R, Wang R, Hansen BB, Håkan-Bloch J (2016) The economic and health-related impact of Crohn’s disease in the United States: evidence from a nationally representative survey. Inflamm Bowel Dis 22(5):1032–1041. https://doi.org/10.1097/MIB.0000000000000742
Barros LL, Farias AQ, Rezaie A (2019) Gastrointestinal motility and absorptive disorders in patients with inflammatory bowel diseases: prevalence, diagnosis and treatment. World J Gastroenterol 25(31):4414–4426. https://doi.org/10.3748/wjg.v25.i31.4414
Baumgart DC, Carding SR (2007) Inflammatory bowel disease: cause and immunobiology. Lancet 369(9573):1627–1640. https://doi.org/10.1016/S0140-6736(07)60750-8
Kaplan GG, Ng SC (2017) Understanding and preventing the global increase of inflammatory bowel disease. Gastroenterology 152(2):313–321. https://doi.org/10.1053/j.gastro.2016.10.020
Owczarek D, Rodacki T, Domagała-Rodacka R, Cibor D, Mach T (2016) Diet and nutritional factors in inflammatory bowel diseases. World J Gastroenterol 22(3):895–905. https://doi.org/10.3748/wjg.v22.i3.895
Mohammadi E, Qujeq D, Taheri H, Hajian-Tilaki K (2017) Evaluation of serum trace element levels and superoxide dismutase activity in patients with inflammatory bowel disease: translating basic research into clinical application. Biol Trace Elem Res 177(2):235–240. https://doi.org/10.1007/s12011-016-0891-0
Opstelten JL, Leenders M, Dik VK, Chan SS, van Schaik FD, Khaw KT, Luben R, Hallmans G, Karling P, Lindgren S, Grip O, Key TJ, Crowe FL, Boeing H, Bergmann MM, Overvad K, Palli D, Masala G, Racine A, Carbonnel F, Boutron-Ruault MC, Tjønneland A, Olsen A, Andersen V, Kaaks R, Katzke VA, Tumino R, Trichopoulou A, Siersema PD, Bueno-de-Mesquita HB, Hart AR, Oldenburg B (2016) Dairy products, dietary calcium, and risk of inflammatory bowel disease: results from a european prospective cohort investigation. Inflamm Bowel Dis 22(6): 1403-1411. https://doi.org/10.1097/MIB.0000000000000798
Zhang L, Shao F, Li L (2020) Association of copper and zinc intake with inflammatory bowel disease and fecal incontinence symptoms: evidence from the national health and nutrition examination survey. Biol Trace Elem Res. https://doi.org/10.1007/s12011-020-02390-7
Cairo G, Bernuzzi F, Recalcati S (2006) A precious metal: Iron, an essential nutrient for all cells. Genes Nutr 1(1):25–39. https://doi.org/10.1007/BF02829934
Simcox JA, McClain DA (2013) Iron and diabetes risk. Cell Metab 17(3):329–341. https://doi.org/10.1016/j.cmet.2013.02.007
Gujja P, Rosing DR, Tripodi DJ, Shizukuda Y (2010) Iron overload cardiomyopathy: better understanding of an increasing disorder. J Am Coll Cardiol 56(13):1001–1012. https://doi.org/10.1016/j.jacc.2010.03.083
Paganini D, Zimmermann MB (2017) The effects of iron fortification and supplementation on the gut microbiome and diarrhea in infants and children: a review. Am J Clin Nutr 106(Suppl 6):1688S–1693S. https://doi.org/10.3945/ajcn.117.156067
Paganini D, Uyoga MA, Zimmermann MB (2016) Iron fortification of foods for infants and children in low-income countries: effects on the gut microbiome, gut inflammation, and diarrhea. Nutrients 8(8). https://doi.org/10.3390/nu8080494
Stochel-Gaudyn A, Fyderek K, Kościelniak P (2019) Serum trace elements profile in the pediatric inflammatory bowel disease progress evaluation. J Trace Elem Med Biol 55:121–126. https://doi.org/10.1016/j.jtemb.2019.06.016
de Silva PS, Yang X, Korzenik JR, Goldman RH, Arheart KL, Caban-Martinez AJ (2017) Association of urinary phenolic compounds, inflammatory bowel disease and chronic diarrheal symptoms: evidence from the National Health and Nutrition Examination Survey. Environ Pollut 229:621–626. https://doi.org/10.1016/j.envpol.2017.06.023
Whelton PK, Carey RM, Aronow WS, Casey DJ, Collins KJ, Dennison HC, DePalma SM, Gidding S, Jamerson KA, Jones DW, MacLaughlin EJ, Muntner P, Ovbiagele B, Smith SJ, Spencer CC, Stafford RS, Taler SJ, Thomas RJ, Williams KS, Williamson JD, Wright JJ (2018) 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 138(17):e426–e483. https://doi.org/10.1161/CIR.0000000000000597
Ballou S, Singh P, Rangan V, Iturrino J, Nee J, Lembo A (2019) Obesity is associated with significantly increased risk for diarrhoea after controlling for demographic, dietary and medical factors: a cross-sectional analysis of the 2009-2010 National Health and Nutrition Examination Survey. Aliment Pharmacol Ther 50(9):1019–1024. https://doi.org/10.1111/apt.15500
Gera T, Sachdev HP (2002) Effect of iron supplementation on incidence of infectious illness in children: systematic review. BMJ 325(7373):1142. https://doi.org/10.1136/bmj.325.7373.1142
Soofi S, Cousens S, Iqbal SP, Akhund T, Khan J, Ahmed I, Zaidi AK, Bhutta ZA (2013) Effect of provision of daily zinc and iron with several micronutrients on growth and morbidity among young children in Pakistan: a cluster-randomized trial. Lancet 382(9886):29–40. https://doi.org/10.1016/S0140-6736(13)60437-7
Richard SA, Zavaleta N, Caulfield LE, Black RE, Witzig RS, Shankar AH (2006) Zinc and iron supplementation and malaria, diarrhea, and respiratory infections in children in the Peruvian Amazon. Am J Trop Med Hyg 75(1):126–132. https://doi.org/10.4269/ajtmh.2006.75.1.0750126
Dewey KG, Domellöf M, Cohen RJ, Landa RL, Hernell O, Lönnerdal B (2002) Iron supplementation affects growth and morbidity of breast-fed infants: results of a randomized trial in Sweden and Honduras. J Nutr 132(11):3249–3255. https://doi.org/10.1093/jn/132.11.3249
Kortman GA, Boleij A, Swinkels DW, Tjalsma H (2012) Iron availability increases the pathogenic potential of Salmonella typhimurium and other enteric pathogens at the intestinal epithelial interface. Plos One 7(1):e29968. https://doi.org/10.1371/journal.pone.0029968
Emerit J, Beaumont C, Trivin F (2001) Iron metabolism, free radicals, and oxidative injury. Biomed Pharmacother 55(6):333–339. https://doi.org/10.1016/s0753-3322(01)00068-3
Lovell RM, Ford AC (2012) Effect of gender on prevalence of irritable bowel syndrome in the community: systematic review and meta-analysis. Am J Gastroenterol 107(7):991–1000. https://doi.org/10.1038/ajg.2012.131
Singh P, Mitsuhashi S, Ballou S, Rangan V, Sommers T, Cheng V, Iturrino-Moreda J, Friedlander D, Nee J, Lembo A (2018) Demographic and dietary associations of chronic diarrhea in a representative sample of adults in the United States. Am J Gastroenterol 113(4):593–600. https://doi.org/10.1038/ajg.2018.24
Acknowledgments
The authors thank the National Center for Health Statistics of the Centers for Disease Control and Prevention for sharing the data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
NHANES was approved by the National Center for Health Statistics Research Ethics Review Board.
Code Availability
The code of this study will be made available on reasonable request.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, F., Yang, D. & Wang, Z. Associations Between Iron Intake and Serum Iron with Inflammatory Bowel Disease and Chronic Diarrheal Symptoms in Adults: the National Health and Nutrition Examination Survey, 2007–2010. Biol Trace Elem Res 199, 4084–4091 (2021). https://doi.org/10.1007/s12011-020-02550-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-020-02550-9