Abstract
Purpose
Illness beliefs impact disease self-management; however, little is known about the impact of patients’ beliefs about one illness on the management of another illness. We sought to understand how cancer beliefs impact diet self-management for cancer survivors with diabetes and whether a change in beliefs leads to a change in dietary adherence.
Methods
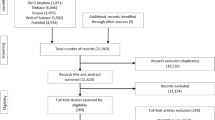
Seventy-eight participants with diabetes and recently diagnosed early-stage breast, prostate, lung, or colon cancer were recruited. Participants were surveyed at enrollment and after 12 months about their cancer and diabetes illness beliefs and dietary adherence. Associations between beliefs about cancer and diabetes to diet adherence at baseline and at 12 months were assessed. Change in diet adherence was examined in relation to beliefs about each illness.
Results
The mean age was 62 years, and 23 (32%) identified as black non-Hispanic, 22 (31%) as white non-Hispanic, and 14 (19%) as Hispanic. Participants with more threatening beliefs about both cancer and diabetes at baseline had worse adherence to a diabetes diet than those with less threatening beliefs. However, at 12 months, those with more threatening cancer beliefs had better dietary adherence than participants with less threatening beliefs. Diabetes beliefs were not associated with diet adherence at 12 months.
Conclusions
While threatening illness beliefs may initially result in worse diet adherence, over time these beliefs may result in increased activation for better self-care and improved diet adherence.
Implications for Cancer Survivors
Understanding how cancer beliefs impact diet self-management for diabetes may provide co** strategies to improve cancer survivors’ management of comorbidities.


Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Miller KD, et al. Cancer treatment and survivorship statistics, 2019. CA Cancer J Clin. 2019;69(5):363–85.
Ritchie CS, Kvale E, Fisch MJ. Multimorbidity: an issue of growing importance for oncologists. J Oncol Pract. 2011;7(6):371–4.
Edwards BK, et al. Annual report to the nation on the status of cancer, 1975–2010, featuring prevalence of comorbidity and impact on survival among persons with lung, colorectal, breast, or prostate cancer. Cancer. 2014;120(9):1290–314.
Berglund A, et al. Comorbidity, treatment and mortality: a population based cohort study of prostate cancer in PCBaSe Sweden. J Urol. 2011;185(3):833–9.
Roy S, et al. Comparison of comorbid conditions between cancer survivors and age-matched patients without cancer. J Clin Med Res. 2018;10(12):911–9.
Xu Y, et al. Factors influencing diabetes self-management in Chinese people with type 2 diabetes. Res Nurs Health. 2008;31(6):613–25.
Petrie KJ, Weinman J. Why illness perceptions matter. Clin Med (Lond). 2006;6(6):536–9.
Harvey JN, Lawson VL. The importance of health belief models in determining self-care behaviour in diabetes. Diabet Med. 2009;26(1):5–13.
Luo X, et al. Factors influencing self-management in Chinese adults with type 2 diabetes: a systematic review and meta-analysis. Int J Environ Res Public Health. 2015;12(9):11304–27.
Wang JQ, Tak-Ying Shiu A. Diabetes self-efficacy and self-care behaviour of Chinese patients living in Shanghai. J Clin Nurs. 2004;13(6):771–2.
James J, et al. Exploratory study of impact of cancer-related posttraumatic stress symptoms on diabetes self-management among cancer survivors. Psychooncology. 2018;27(2):648–53.
Broadbent E, et al. The brief illness perception questionnaire. J Psychosom Res. 2006;60(6):631–7.
Zanders MM, et al. Impact of cancer on adherence to glucose-lowering drug treatment in individuals with diabetes. Diabetologia. 2015;58(5):951–60.
Sami W, et al. Effect of diet on type 2 diabetes mellitus: a review. Int J Health Sci (Qassim). 2017;11(2):65–71.
Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care activities measure: results from 7 studies and a revised scale. Diabetes Care. 2000;23(7):943–50.
Paxton AE, et al. Starting the conversation: performance of a brief dietary assessment and intervention tool for health professionals. Am J Prev Med. 2011;40(1):67–71.
Cardoso G, et al. Depression and anxiety symptoms following cancer diagnosis: a cross-sectional study. Psychol Health Med. 2016;21(5):562–70.
Linden W, et al. Anxiety and depression after cancer diagnosis: prevalence rates by cancer type, gender, and age. J Affect Disord. 2012;141(2–3):343–51.
Kivimäki M (2018) The Routledge international handbook of psychosocial epidemiology, Routledge/Taylor & Francis Group,: London ; New York. p. 1 online resource
Dauchy S, Dolbeault S, Reich M. Depression in cancer patients. EJC Suppl. 2013;11(2):205–15.
Bussell VA, Naus MJ. A longitudinal investigation of co** and posttraumatic growth in breast cancer survivors. J Psychosoc Oncol. 2010;28(1):61–78.
Czerw A, Religioni U, Deptala A. Assessment of pain, acceptance of illness, adjustment to life with cancer and co** strategies in breast cancer patients. Breast Cancer. 2016;23(4):654–61.
Chew BH, Shariff-Ghazali S, Fernandez A. Psychological aspects of diabetes care: effecting behavioral change in patients. World J Diabetes. 2014;5(6):796–808.
Stuckey HL, et al. Personal accounts of the negative and adaptive psychosocial experiences of people with diabetes in the second diabetes attitudes, wishes and needs (DAWN2) study. Diabetes Care. 2014;37(9):2466–74.
Huang M, et al. Self-management behavior in patients with type 2 diabetes: a cross-sectional survey in western urban China. PLoS ONE. 2014;9(4):e95138.
Gross JJ. Emotion regulation: affective, cognitive, and social consequences. Psychophysiology. 2002;39(3):281–91.
Acknowledgements
We wish to acknowledge Jody-Ann McLeggon, Sarah Prieto, Margaret Yoon, Alexandra Rosenberg, and Janey James for their help with patient recruitment, interviews, and study management. We would also like to thank the participants for their time.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article. This study was supported by the National Cancer Institute (1K07CA166462 to JJL).
Author information
Authors and Affiliations
Contributions
All authors contributed to the manuscript topic and design. KAM and CS performed all analyses and developed the initial abstract and manuscript draft. CS, RZ, and KP conducted the literature review and wrote and revised the final manuscript text. JJL was responsible for the initial hypotheses and supervised the manuscript’s development. YTH provided expertise on diabetes mellitus in cancer survivors and made substantial revisions to the manuscript. JPW guided statistical analyses and made substantial contributions to both the tables and text. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Authors Kimberly A. Muellers, Chloe Soukas, Rebecca Zeidman, Karisma Panaleon, Yael T. Harris, and Jenny J. Lin declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Author Juan Wisnivesky received consulting honorarium from Banook, PPD, Sanofi, Atea, and Prospero and grants from Regenron, Axella, Sanofi and Arnolds Consultant.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Muellers, K.A., Soukas, C., Zeidman, R. et al. Cancer beliefs and diet self-management among cancer survivors with comorbid diabetes. J Cancer Surviv 18, 900–906 (2024). https://doi.org/10.1007/s11764-023-01340-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-023-01340-1