Abstract
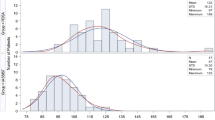
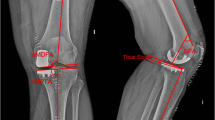
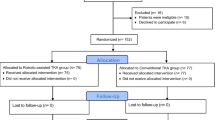
The aim of this study was to compare the short term clinical and radiological outcomes of imageless robotic and conventional total knee arthroplasty (TKA) and to estimate the accuracy of the two techniques by analysing the outliers after TKA. We have evaluated 200 consecutive knees (158 patients), 100 knees undergoing robotic TKA, and 100 knees treated with conventional TKA. Demographic parameters like age, gender, body mass index, diagnosis and range of motion were obtained. Knee society score (KSS) and Knee society functional score (KSS-F) were used for clinical evaluation. Mechanical alignment (Hip-knee-ankle angle), proximal tibial angle (MPTA), distal femoral angle (LDFA) and tibial slope were analysed for radiological results and outliers were compared between both groups. Outliers were defined when the measured angle exceeded ± 3° from the neutral alignment in each radiological measurement on the final follow-up radiograph.The minimum follow-up was 6 months (range, 6 to 18 months). The preoperative mean HKA angle was 169.7 ± 11.3° in robotic group and 169.3 ± 7.3° in conventional group. There was significant improvement in HKA, LDFA, MPTA and tibial slope compared to the preoperative values in both the groups (p < 0.01). The number of HKA, LDFA and tibial slope outliers were 31, 29 and 37, respectively, in the conventional group compared to 13, 23 and 17 in the robotic group (p < 0.01). There was a significant improvement in the KSS and KSS-F functional scores postoperatively in both the groups (p < 0.01). However, there was no significant difference in the functional scores between the groups postoperatively (p = 0.08). This study showed excellent improvement with both imageless robotic and conventional TKA, with similar clinical outcomes between both groups. However, radiologically robotic TKA showed better accuracy and consistency with fewer outliers compared with conventional TKA.


Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
Change history
15 June 2024
A Correction to this paper has been published: https://doi.org/10.1007/s11701-024-02004-7
References
Vos T, Lim SS, Abbafati C, Abbas KM, Abbasi M, Abbasifard M, Abbasi-Kangevari M, Abbastabar H, Abd-Allah F, Abdelalim A, Abdollahi M (2020) Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the global burden of disease study 2019. Lancet 396(10258):1204–1222. https://doi.org/10.1016/S0140-6736(20)30925-9
Price AJ, Alvand A, Troelsen A, Katz JN, Hooper G, Gray A, Carr A, Beard D (2018) Knee replacement. Lancet 392(10158):1672–1682. https://doi.org/10.1016/S0140-6736(18)32344-4
Kazarian GS, Haddad FS, Donaldson MJ, Wignadasan W, Nunley RM, Barrack RL (2022) Implant malalignment may be a risk factor for poor patient-reported outcomes measures (PROMs) following total knee arthroplasty (TKA). J Arthroplast 37(6):S129–S133. https://doi.org/10.1016/j.arth.2022.02.087
Wu M, Charalambous L, Penrose C, Belay E, Seyler TM (2021) Imageless robotic knee arthroplasty. Oper Tech Orthop 31(4):100906. https://doi.org/10.1016/j.oto.2021.100906
Walgrave S, Oussedik S (2023) Comparative assessment of current robotic-assisted systems in primary total knee arthroplasty. Bone Jt Open 4(1):13–18. https://doi.org/10.1302/2633-1462.41.BJO-2022-0070.R1
Ewald FC (1989) The knee society total knee arthroplasty roentgenographic evaluation and scoring system. Clin Orthop Relat Res 248:9–12
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res 248:13–14
Jeffery R, Morris R, Denham R (1991) Coronal alignment after total knee replacement. J Bone Jt Surg Br. https://doi.org/10.1302/0301-620X.73B5.1894655
Doan GW, Courtis RP, Wyss JG, Green EW, Clary CW (2022) Image-free robotic-assisted total knee arthroplasty improves implant alignment accuracy: a cadaveric study. J Arthroplast 37(4):795–801. https://doi.org/10.1016/j.arth.2021.12.035
Ruangsomboon P, Ruangsomboon O, Pornrattanamaneewong C, Narkbunnam R, Chareancholvanich K (2023) Clinical and radiological outcomes of robotic-assisted versus conventional total knee arthroplasty: a systematic review and meta-analysis of randomized controlled trials. ActaO 94:60–79. https://doi.org/10.2340/17453674.2023.9411
Riantho A, Butarbutar JCP, Fidiasrianto K et al (2023) Radiographic outcomes of robot-assisted versus conventional total knee arthroplasty: a systematic review and meta-analysis of randomized clinical trials. JBJS Open Access. https://doi.org/10.2106/JBJS.OA.23.00010
Cho KJ, Seon JK, Jang WY, Park CG, Song EK (2019) Robotic versus conventional primary total knee arthroplasty: clinical and radiological long-term results with a minimum follow-up of ten years. Int Orthop (SICOT) 43(6):1345–1354. https://doi.org/10.1007/s00264-018-4231-1
Deckey DG, Rosenow CS, Verhey JT, Brinkman JC, Mayfield CK, Clarke HD, Bingham JS (2021) Robotic- assisted total knee arthroplasty improves accuracy and precision compared to conventional techniques. Bone Jt J. 103(6 Supple A):74–80
Song EK, Seon JK, Park SJ, Jung WB, Park HW, Lee GW (2011) Simultaneous bilateral total knee arthroplasty with robotic and conventional techniques: a prospective, randomized study. Knee Surg Sports Traumatol Arthrosc 19(7):1069–1076. https://doi.org/10.1007/s00167-011-1400-9
Rajasekaran RB, Palanisami DR, Natesan R, Rajasekaran S (2020) Minimal under-correction gives better outcomes following total knee arthroplasty in severe varus knees—myth or reality?—analysis of one hundred sixty two knees with varus greater than fifteen degrees. Int Orthop 44:715–723
Boddu SP, Moore ML, Rodgers BM, Brinkman JC, Verhey JT, Bingham JS (2023) (2023) A bibliometric analysis of the top 100 most influential studies on robotic arthroplasty. Arthroplast Today 22:101153. https://doi.org/10.1016/j.artd.2023.101153
Abdel MP, Ollivier M, Parratte S, Trousdale RT, Berry DJ, Pagnano MW (2018) Effect of postoperative mechanical axis alignment on survival and functional outcomes of modern total knee arthroplasties with cement: a concise follow-up at 20 years. J Bone Jt Surg 100(6):472–478. https://doi.org/10.2106/JBJS.16.01587
Kim YH, Yoon SH, Park JW (2020) Does robotic-assisted TKA result in better outcome scores or long-term survivorship than conventional TKA? A randomized Controlled Trial. Clin Orthop Relat Res 478(2):266–275. https://doi.org/10.1097/CORR.0000000000000916
Lee YM, Kim GW, Lee CY, Song EK, Seon JK (2023) No difference in clinical outcomes and survivorship for robotic, navigational, and conventional primary total knee arthroplasty with a minimum follow-up of 10 years. Clin Orthop Surg 15(1):82. https://doi.org/10.4055/cios21138
Ofa SA, Ross BJ, Flick TR, Patel AH, Sherman WF (2020) Robotic total knee arthroplasty vs conventional total knee arthroplasty: a nationwide database study. Arthroplast Today 6(4):1001-1008.e3. https://doi.org/10.1016/j.artd.2020.09.014
Canfield M, Savoy L, Cote MP, Halawi MJ (2020) Patient-reported outcome measures in total joint arthroplasty: defining the optimal collection window. Arthroplast Today 6(1):62–67. https://doi.org/10.1016/j.artd.2019.10.003
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Soundarrajan Dhanasekaran, Bahru Atnafu Shiferaw and Rithika Singh. The first draft of the manuscript was written by Shanmuganathan Rajasekaran, Soundarrajan Dhanasekaran and Rithika Singh. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Institutional Ethics Committee (IRB Approval No: 7/11/2022).
Consent for participate
Informed consent was obtained from all individual participants included in the study.
Consent for publish
The authors affirm that human research participants provided informed consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rajasekaran, S., Soundarrajan, D., Singh, R. et al. Comparison of imageless robotic assisted total knee arthroplasty and conventional total knee arthroplasty: early clinical and radiological outcomes of 200 knees. J Robotic Surg 18, 151 (2024). https://doi.org/10.1007/s11701-024-01905-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11701-024-01905-x