Abstract
Purpose
Steatohepatitic hepatocellular carcinoma (SH-HCC) is characterized by intratumoral fat with > 50% inflammatory changes. However, intratumoral fat (with or without inflammation) can also be found in not-otherwise specified HCC (NOS-HCC). We compared the imaging features and outcome of resected HCC containing fat on pathology including SH-HCC (> 50% steatohepatitic component), NOS-HCC with < 50% steatohepatitic component (SH-NOS-HCC), and fatty NOS-HCC (no steatohepatitic component).
Material and methods
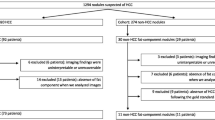
From September 2012 to June 2021, 94 patients underwent hepatic resection for fat-containing HCC on pathology. Imaging features and categories were assessed using LIRADS v2018. Fat quantification was performed on chemical-shift MRI. Recurrence-free and overall survival were estimated.
Results
Twenty-one patients (26%) had nonalcoholic steatohepatitis (NASH). The median intra-tumoral fat fraction was 8%, with differences between SH-HCC and SH-NOS-HCC (9.5% vs. 5% p = 0.03). There was no difference in major LI-RADS features between all groups; most tumors were classified as LR-4/5. A mosaic architecture on MRI was rare (7%) in SH-HCC, a fat in mass on CT was more frequently depicted (48%) in SH-HCC. A combination of NASH with no mosaic architecture on MRI or NASH with fat in mass on CT yielded excellent specificity for diagnosing SH-HCC (97.6% and 97.7%, respectively). The median recurrence-free and overall survival were 58 and 87 months, with no difference between groups (p = 0.18 and p = 0.69).
Conclusion
In patients with NASH, an SH-HCC may be suspected in L4/LR-5 observations with no mosaic architecture at MRI or with fat in mass on CT. Oncological outcomes appear similar between fat-containing HCC subtypes.






Similar content being viewed by others
References
Cancer (IARC) TIA for R on Global Cancer Observatory. https://gco.iarc.fr/. Accessed 18 Apr 2022
WHO Classification of Tumours. Digestive System Tumours. Fifth Edition—WHO. Accessed 20 Apr 2020
Calderaro J, Couchy G, Imbeaud S et al (2017) Histological subtypes of hepatocellular carcinoma are related to gene mutations and molecular tumour classification. J Hepatol 67:727–738. https://doi.org/10.1016/j.jhep.2017.05.014
Ziol M, Poté N, Amaddeo G et al (2018) Macrotrabecular-massive hepatocellular carcinoma: a distinctive histological subtype with clinical relevance. Hepatology 68:103–112. https://doi.org/10.1002/hep.29762
Salomao M, Yu WM, Brown RS, Emond JC (2010) Steatohepatitic hepatocellular carcinoma (SH-HCC). Am J Surg Pathol 34:7
Shafizadeh N, Kakar S (2013) Hepatocellular carcinoma. Surg Pathol Clin 6:367–384. https://doi.org/10.1016/j.path.2013.03.007
Shibahara J, Ando S, Sakamoto Y et al (2014) Hepatocellular carcinoma with steatohepatitic features: a clinicopathological study of Japanese patients. Histopathology 64:951–962. https://doi.org/10.1111/his.12343
Salomao M, Remotti H, Vaughan R et al (2012) The steatohepatitic variant of hepatocellular carcinoma and its association with underlying steatohepatitis. Hum Pathol 43:737–746. https://doi.org/10.1016/j.humpath.2011.07.005
Taniai M, Hashimoto E, Tobari M et al (2018) Clinicopathological investigation of steatohepatitic hepatocellular carcinoma: a multicenter study using immunohistochemical analysis of adenoma-related markers: clinicopathological investigation of steatohepatitic hepatocellular carcinoma. Hepatol Res 48:947–955. https://doi.org/10.1111/hepr.13203
Jain D, Nayak NC, Kumaran V, Saigal S (2013) Steatohepatitic hepatocellular carcinoma, a morphologic indicator of associated metabolic risk factors: a study from India. Arch Pathol Lab Med 137:961–966. https://doi.org/10.5858/arpa.2012-0048-OA
Olofson AM, Gonzalo DH, Chang M, Liu X (2018) Steatohepatitic variant of hepatocellular carcinoma: a focused review. Gastroenterol Res 11:391–396. https://doi.org/10.14740/gr1110
Ando S, Shibahara J, Hayashi A, Fukayama M (2015) β-catenin alteration is rare in hepatocellular carcinoma with steatohepatitic features: immunohistochemical and mutational study. Virchows Arch 467:535–542. https://doi.org/10.1007/s00428-015-1836-2
Lee JS, Yoo JE, Kim H et al (2017) Tumor stroma with senescence-associated secretory phenotype in steatohepatitic hepatocellular carcinoma. PLoS ONE 12:e0171922. https://doi.org/10.1371/journal.pone.0171922
Fujiwara N, Nakagawa H, Enooku K et al (2018) CPT2 downregulation adapts HCC to lipid-rich environment and promotes carcinogenesis via acylcarnitine accumulation in obesity. Gut 67:1493–1504. https://doi.org/10.1136/gutjnl-2017-315193
Cannella R, Dioguardi Burgio M, Beaufrère A et al (2021) Imaging features of histological subtypes of hepatocellular carcinoma: implication for LI-RADS. JHEP Rep 3:100380. https://doi.org/10.1016/j.jhepr.2021.100380
Inui S, Kondo H, Tanahashi Y et al (2021) Steatohepatitic hepatocellular carcinoma: imaging findings with clinicopathological correlation. Clin Radiol 76:160.e15-160.e25. https://doi.org/10.1016/j.crad.2020.09.011
Mulé S (2023) MRI features associated with HCC histologic subtypes: a western American and European bicenter study. Eur Radiol 33:1342
Yamaoka K, Saitoh S, Kinowaki K et al (2022) Clinicopathological assessment of steatohepatitic hepatocellular carcinoma. Clin Res Hepatol Gastroenterol 46:101799. https://doi.org/10.1016/j.clinre.2021.101799
Park JH, Park YN, Kim M-J et al (2023) Steatotic hepatocellular carcinoma: association of MRI findings to underlying liver disease and clinicopathological characteristics. Liver Int 43:1332–1344. https://doi.org/10.1111/liv.15589
Kambadakone AR, Fung A, Gupta RT et al (2018) LI-RADS technical requirements for CT, MRI, and contrast-enhanced ultrasound. Abdom Radiol 43:56–74. https://doi.org/10.1007/s00261-017-1325-y
CT/MRI LI-RADS v2018. https://www.acr.org/Clinical-Resources/Reporting-and-Data-Systems/LI-RADS/CT-MRI-LI-RADS-v2018. Accessed 18 Apr 2022
Chiang H-J, Lin L-H, Li C-W et al (2014) Magnetic resonance fat quantification in living donor liver transplantation. Transplant Proc 46:666–668. https://doi.org/10.1016/j.transproceed.2013.11.050
Kim HJ, Cho HJ, Kim B et al (2019) Accuracy and precision of proton density fat fraction measurement across field strengths and scan intervals: a phantom and human study. J Magn Reson Imaging JMRI 50:305–314. https://doi.org/10.1002/jmri.26575
Idilman IS, Tuzun A, Savas B et al (2015) Quantification of liver, pancreas, kidney, and vertebral body MRI-PDFF in non-alcoholic fatty liver disease. Abdom Imaging 40:1512–1519. https://doi.org/10.1007/s00261-015-0385-0
Hui SCN, So H-K, Chan DFY et al (2018) Validation of water-fat MRI and proton MRS in assessment of hepatic fat and the heterogeneous distribution of hepatic fat and iron in subjects with non-alcoholic fatty liver disease. Eur J Radiol 107:7–13. https://doi.org/10.1016/j.ejrad.2018.08.008
Hussain HK, Chenevert TL, Londy FJ et al (2005) Hepatic fat fraction: MR imaging for quantitative measurement and display—early experience. Radiology 237:1048–1055. https://doi.org/10.1148/radiol.2373041639
Trapani L, Beaufrère A, Hobeika C et al (2023) Pathological overview of steatohepatitic hepatocellular carcinoma in a surgical series. Histopathology 83:526–537. https://doi.org/10.1111/his.14941
Kleiner DE, Brunt EM, Natta MV et al (2005) Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 41:1313–1321. https://doi.org/10.1002/hep.20701
Bedossa P, Poitou C, Veyrie N et al (2012) Histopathological algorithm and scoring system for evaluation of liver lesions in morbidly obese patients. Hepatology 56:1751–1759. https://doi.org/10.1002/hep.25889
Aykutlu U, Argon A, Orman M et al (2021) Steatotic and steatohepatitic hepatocellular carcinomas: features in a series with predominantly viral etiology. Am J Surg Pathol 45:1252–1263. https://doi.org/10.1097/PAS.0000000000001714
Kupczyk PA, Kurt D, Endler C et al (2023) MRI proton density fat fraction for estimation of tumor grade in steatotic hepatocellular carcinoma. Eur Radiol 33:8974–8985. https://doi.org/10.1007/s00330-023-09864-x
Liu X, Ni X, Li Y et al (2022) Diagnostic performance of LI-RADS version 2018 for primary liver cancer in patients with liver cirrhosis on enhanced MRI. Front Oncol 12:934045. https://doi.org/10.3389/fonc.2022.934045
Kim Y-Y, An C, Kim S, Kim M-J (2018) Diagnostic accuracy of prospective application of the Liver Imaging Reporting and Data System (LI-RADS) in gadoxetate-enhanced MRI. Eur Radiol 28:2038–2046. https://doi.org/10.1007/s00330-017-5188-y
An C, Park S, Chung YE et al (2017) Curative resection of single primary hepatic malignancy: liver imaging reporting and data system category LR-M portends a worse prognosis. Am J Roentgenol 209:576–583. https://doi.org/10.2214/AJR.16.17478
Auer TA, Halskov S, Fehrenbach U et al (2023) Gd-EOB MRI for HCC subtype differentiation in a western population according to the 5th edition of the World Health Organization classification. Eur Radiol 33:6902–6915. https://doi.org/10.1007/s00330-023-09669-y
Chen K, Xu Y, Dong Y et al (2023) Contrast-enhanced imaging features and clinicopathological investigation of steatohepatitic hepatocellular carcinoma. Diagnostics 13:1337. https://doi.org/10.3390/diagnostics13071337
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Alexandre Faure, Marco Dioguardi Burgio, Roberto Cannella. The first draft of the manuscript was written by Alexandre Faure, Marco Dioguardi Burgio and Maxime Ronot and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.”
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval/consent to publish
This study was performed in line with the principles of the Declaration of Helsinki. Local IRB (CERIM) approved this retrospective study and waiver of written informed consent was obtained due to de retrospective approach.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Faure, A., Dioguardi Burgio, M., Cannella, R. et al. Imaging and prognostic characterization of fat-containing hepatocellular carcinoma subtypes. Radiol med 129, 687–701 (2024). https://doi.org/10.1007/s11547-024-01807-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-024-01807-w