Abstract
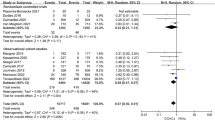
The optimal INR target in patients with mechanical heart valves is unclear. Higher INR targets are often used in Western compared with East Asian countries. The objective of this systematic review and meta-analysis was to summarize the evidence for the efficacy and safety of lower versus higher INR targets in Western and East Asian left-sided mechanical heart valve patients. We searched Western databases including Cochrane CENTRAL, Medline, and Embase as well as Chinese databases including SinoMed, CNKI, and Wanfang Data in addition to grey literature for Randomized Controlled Trials (RCTs) and observational studies. We pooled risk ratios (RRs) using random-effects model. Low and high INR targets were defined by the individual studies. We identified nine RCTs, including six Western (n = 5496) and three East Asian (n = 209) trials, and 17 observational studies, including two Western (n = 3199) and 15 East Asian (n = 5485) studies. In the RCTs, lower compared with higher targets were associated with similar rates of thromboembolism (2.4 vs. 2.3%; RR: 1.14, 95% CI 0.82, 1.60, I2 = 0%) and lower rates of both total bleeding (21.9 vs. 40.9%, RR: 0.46, 95% CI 0.28, 0.78, I2 = 88%) and major bleeding. RCT data showed no statistical heterogeneity by region. These effects were consistent in the observational data. We downgraded the quality of evidence due to serious risk of bias and imprecision. In patients with left-sided contemporary mechanical heart valves, low quality evidence suggests lower INR targets are associated with similar rates of thromboembolism and moderate quality evidence suggests lower rates of bleeding.




Similar content being viewed by others
References
Yacoub MH, Takkenberg JJ (2005) Will heart valve tissue engineering change the world? Nat Clin Pract Cardiovasc Med 2(2):60–61
Hammermeister K, Sethi GK, Henderson WG, Grover FL, Oprian C, Rahimtoola SH (2000) Outcomes 15 years after valve replacement with a mechanical versus a bioprosthetic valve: final report of the veterans affairs randomized trial. J Am Coll Cardiol 36(4):1152–1158
Koertke H, Minami K, Boethig D, Breymann T, Seifert D, Wagner O, Atmacha N, Krian A, Ennker J, Taborski U, Klovekorn WP (2003) INR self-management permits lower anticoagulation levels after mechanical heart valve replacement. Circulation 108(10_suppl_1):75
Matiasz R, Rigolin VH (2018) 2017 focused update for management of patients with valvular heart disease: summary of new recommendations. J Am Heart Assoc 7(1):e007596
Whitlock RP, Sun JC, Fremes SE, Rubens FD, Teoh KH (2012) Antithrombotic and thrombolytic therapy for valvular disease: antithrombotic therapy and prevention of thrombosis: American college of chest physicians evidence-based clinical practice guidelines. Chest 141(2):e576S-600S
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP III, Guyton RA, O’Gara PT, Ruiz CE, Skubas NJ, Sorajja P, Sundt TM III (2014) 2014 AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American college of cardiology/American heart association task force on practice guidelines. Circulation 129(23):2440–2492
Baumgartner H, Falk V, Bax JJ, De Bonis M, Hamm C, Holm PJ, Iung B, Lancellotti P, Lansac E, Rodriguez Munoz D, Rosenhek R (2017) 2017 ESC/EACTS guidelines for the management of valvular heart disease. Eur Heart J 38(36):2739–2791
Kim HK, Tantry US, Smith SC Jr, Jeong MH, Park SJ, Kim MH, Lim DS, Shin ES, Park DW, Huo Y, Chen SL (2020) The East Asian paradox: an updated position statement on the challenges to the current antithrombotic strategy in patients with cardiovascular disease. Thromb Haemost. https://doi.org/10.1055/s-0040-1718729
Gupta S, Belley-Cote EP, Sarkaria A, Pandey A, Spence J, McClure G, Panchal P, Jaffer IH, An K, Eikelboom J, Whitlock RP (2018) International normalized ratio targets for left-sided mechanical valve replacement. Thromb Haemost 118(05):906–913
Pandey AK, Xu K, Zhang L, Gupta S, Eikelboom J, Cook O, McIntyre WF, Lopes RD, Crowther M, Belley-Côté EP, Whitlock RP (2020) Lower versus standard INR targets in atrial fibrillation: a systematic review and meta-analysis of randomized controlled trials. Thromb Haemost 120(03):484–494
Gupta S, Whitlock R, Belley-Cote E, Spence J, Jaffer I, Eikelboom J, McClure G (2016) INR targets for mechanical aortic and mitral valves: a systematic review and meta-analysis. PROSPERO 2016 CRD42016048334 Available from: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42016048334
Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia. Available at: www.covidence.org. Accessed 20 Nov 2019
Higgins JPT, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JAC, Cochrane Bias Methods Group, Cochrane Statistical Methods Group (2011) The cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Tool to Assess Risk of Bias in Cohort Studies [Internet]. MAGIC Evidence Ecosystem Foundation. http://help.magicapp.org/knowledgebase/articles/327941-tool-to-assess-risk-of-bias-in-cohort-studies. Accessed 13 Jul 2021
Manager R (2014) (RevMan) [Computer program]. Version 5.3. Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(03):177–188
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, Schünemann HJ, GRADE Working Group (2008) GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ 336(7650):924–926
Acar J, Iung B, Boissel JP, Samama MM, Michel PL, Teppe JP, Pony JC, Le Breton H, Thomas D, Isnard R, de Gevigney G (1996) AREVA: multicenter randomized comparison of low-dose versus standard-dose anticoagulation in patients with mechanical prosthetic heart valves. Circulation 94(9):2107–2112
Hering D, Piper C, Bergemann R, Hillenbach C, Dahm M, Huth C, Horstkotte D (2005) Thromboembolic and bleeding complications following St. Jude Medical valve replacement: results of the German experience with low-intensity anticoagulation study. Chest 127(1):53–59
Koertke H, Zittermann A, Wagner O, Secer S, Sciangula A, Saggau W, Sack FU, Ennker J, Cremer J, Musumeci F (2015) Telemedicine-guided, very low-dose international normalized ratio self-control in patients with mechanical heart valve implants. Eur Heart J 36(21):1297–1305
Pengo V, Palareti G, Cucchini U, Molinatti M, Del Bono R, Baudo F, Ghirarduzzi A, Pegoraro C, Iliceto S (2007) Low-intensity oral anticoagulant plus low-dose aspirin during the first six months versus standard-intensity oral anticoagulant therapy after mechanical heart valve replacement: a pilot study of low-intensity warfarin and aspirin in cardiac prostheses (LIWACAP). Clin Appl Thromb Hemost 13(3):241–248
Puskas J, Gerdisch M, Nichols D, Quinn R, Anderson C, Rhenman B, Fermin L, McGrath M, Kong B, Hughes C, Sethi G (2014) Reduced anticoagulation after mechanical aortic valve replacement: interim results from the prospective randomized on-X valve anticoagulation clinical trial randomized food and drug administration investigational device exemption trial. J Thorac Cardiovasc Surg 147(4):1202–1211
Torella M, Torella D, Chiodini P, Franciulli M, Romano G, De Santo L, De Feo M, Amarelli C, Sasso FC, Salvatore T, Ellison GM (2010) Lowering the intensity of oral anticoagulant therapy in patients with bileaflet mechanical aortic valve replacement: results from the “LOWERING-IT” trial. Am Heart J 160(1):171–178
Gao S (2017) Clinical observation of different doses of warfarin on anticoagulation for patients with cardiac valvular replacement. Chin J Mod Drug Appl 11(3):99–100
Wang S, Wang Z (2007) The clinical research of low-intensity anti-coagulation after the mechanical valve replacement in Yunnan [master’s thesis]. Kunming Medical College, Yunnan
Xu Q, Tong L, Cai Z (2002) A pilot study on low-intensity anticoagulation of HVR patients in northwest China [master’s thesis]. Fourth Military Medical University, Shaanxi
Bové T, Van Belleghem Y, François K, Caes F, De Pauw M, Taeymans Y, Van Nooten GJ (2017) Low target-INR anticoagulation is safe in selected aortic valve patients with the medtronic open pivot mechanical prosthesis: long-term results of a propensity-matched comparison with standard anticoagulation. Interact Cardiovasc Thorac Surg 24(6):862–868
Poli D, Antonucci E, Pengo V, Migliaccio L, Testa S, Lodigiani C, Coffetti N, Facchinetti R, Serricchio G, Falco P, Mangione C (2018) Mechanical prosthetic heart valves: quality of anticoagulation and thromboembolic risk. The observational multicenter PLECTRUM study. Int J Cardiol 267:68–73
Chen J, Shiying L, Yiquan D (2018) Significance of monitoring the levels of D-dimer and thrombus precursor protein during warfarin anticoagulation in patients undergoing mechanical heart valve replacement. Int J Lab Med 39(12):1511–1513
Chen LP, Taichang Q (2017) Comparative study of two different anticoagulant intensities after cardiac valve replacement [dissertation]. Shanxi Medical University, Shaanxi
Chen S, Shu DC, Wang Z (2017) Efficacy of low intensity warfarin antieoagulation therapy in elderly patients after heart valve replacement. Chin J Geriatr Heart Brain Vessel Dis 19(1):35–37
Han C, Wangfu Z (2008) The initial research of the impact of the low-level anticoagulation in patients through the mitral valve replacement surgery [master’s thesis]. Shanghai Jiaotong University, Shanghai
Meng X, Li JZ, Liu Y, Zhang HB (2004) The uniform standard intensity of oral anticoagulant therapy for the patients with mechanical heart valve prostheses. Chin J Cardiol 32(7):618–621
Mu C, Xue C, Zhang Y, Zhang W (2015) Anticoagulation intensity with warfarin for patients after heart valve replacement. Chin J Postgrad Med 38(4):258–262
**ong P, **ngyun L (2014) The effect of mechanical valve replacement in the treatment of heart valve disease. Chin J Trauma Disabil Med 22(23):59–60
Wang YL, Zhang W, Li XF (2011) The expression and clinical significance of plasma D-dimer in patients after mechanical heart valve replacement. Shaanxi Med J 40(7):797–799
Wang ZW, Yu HT, Yang XH (2007) Lower intense anti-coagulation therapy after replacement of prosthetic mechanical aortic valve. Chin J Exp Surg 24(5):602–603
Wu XY, Zhang MT, Zhang J, Shen J, Hou J (2013) Clinical observation of long-term anticoagulation status after mechanical heart valve replacement. Chin Foreign Med Treat 20:96–98
Xu B, Yi D (2013) The correlation between the intensity of anticoagulant therapy and incidence of complication in patients after mechanical heart valve replacement [master’s thesis]. Fourth Military Medical University
Yang SQ (2014) Expression of D-dimer in different anticoagulation intensity of mechanical heart valve replacement surgery and its clinical significance. Chin J Prac Med 41(4):43–45
Zhang J, Zhang W, Wan J (2014) Application and monitoring of anticoagulation after heart valve replacement. Chin J Postgrad Med 37(8):8–10
Zhang XF, **ao Y, Cheng Y, Chen X, Jia B, Liang L, Han SM (2014) Warfarin after mechanical heart valve replacement: clinical analysis of low-intensity anticoagulation therapy. Chin J Clin Thorac Cardiovasc Surg 21(2):270–271
Zhao M (2017) Clinical analysis of low-intensity anticoagulation after artificial mechanical heart valve replacement in Inner Mongolia [master’s thesis]
Zhang H, Dong Y, Ao X, Zhu D, Dong L (2020) Optimal oral anticoagulant therapy in Chinese patients with mechanical heart valves. Eur J Pharm Sci 144:105202
ClinicalTrials.gov [Internet]. Bethesda (MD): National Library of Medicine (US). 2018 Aug 17. Identifier NCT03636295, Low INR to minimize bleeding with mechanical valves trial (LIMIT), [cited 2021 Jan 6]. https://clinicaltrials.gov/ct2/show/NCT03636295. Accessed 13 Nov 2019
Acknowledgements
Mr. Pandey has nothing to disclose. Dr. Xu has nothing to disclose. Dr. Zhang has nothing to disclose. Dr. Gupta has nothing to disclose. Dr. Crowther reports grants and other from Bayer, personal fees from Pfizer, personal fees from CSL Behring, personal fees from Servier Canada, personal fees from Diagnostica Stago, personal fees from Asahi Kasei, outside the submitted work. Dr. Belley-Cote reports grants from Bayer, grants from Roche, outside the submitted work; Dr. Whitlock reports grants from Bayer, grants from Roche, grants from Boeringer-Ingelheim, other from Boeringer-Ingelheim, other from AtriCure, other from PhaseBio, outside the submitted work. Dr. Eikelboom reports honoraria and grant support from Astra Zeneca, Bayer, Boehringer Ingelheim, Bristol-Myers-Squibb/Pfizer, Daiichi Sankyo, Glaxo Smith Kline, Janssen, sanofi aventis and Eli Lilly as well as a personnel award from the Heart and Stroke Foundation. Dr. Lopes reports personal fees from Bayer, personal fees from Boehringer Ingleheim, grants and personal fees from Bristol-Myers Squibb, personal fees from Daiichi Sankyo, grants and personal fees from Glaxo Smith Kline, grants and personal fees from Medtronic, personal fees from Merck, grants and personal fees from Pfizer, personal fees from Portola, grants and personal fees from Sanofi, outside the submitted work.
Funding
This systematic review and meta-analysis received no funding or financial support from any parties whatsoever.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pandey, A.K., Xu, K., Zhang, L. et al. Efficacy and safety of low intensity vitamin K antagonists in Western and East-Asian patients with left-sided mechanical heart valves. J Thromb Thrombolysis 53, 697–707 (2022). https://doi.org/10.1007/s11239-021-02568-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-021-02568-3