Abstract
Objectives
To characterize contraceptive method use and satisfaction among Spanish-speaking Latina immigrants who attend their child’s well care visit.
Methods
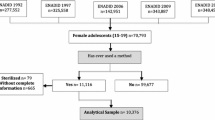
Spanish-speaking women whose youngest child was ≤ 4 years old completed an orally-administered Spanish-language survey in a pediatric clinic (N = 194). Survey items were based on previously published contraceptive use assessments among diverse populations. We used chi-square and Fisher exact test to describe maternal characteristics by contraceptive method effectiveness categories: Tier 1, most effective methods (hormonal implant, intrauterine device, tubal ligation, and vasectomy); Tier 2, very effective methods (hormonal injection, oral contraceptive pill, hormonal patch, and hormonal ring); Tier 3, effective methods (condoms), and no method.
Results
34% of women were using a Tier 1 method, 40% were using a Tier 2 method, and 17% had unmet contraceptive need (no pregnancy intention, no birth control); 84% were satisfied with their current method and 82% of women were uninsured. Tier 2 method or no method users were more likely than women using a Tier 1 method to have children < 9 months old (X2 (6, N = 190) = 20.4, p = .002).
Conclusions
Latina immigrants with young children who attend their child’s pediatric visit are mostly using effective contraceptives and are satisfied with their method. A culturally supportive medical home and access to no-cost long-acting reversible contraceptives through a temporary private grant likely contributed to high contraceptive use and satisfaction in our study. Describing maternal contraceptive use among Latina immigrant mothers can inform future equitable, culturally tailored, approaches to pediatric maternal contraceptive need screening.

Similar content being viewed by others
Data Availability
Yes.
Code Availability
Not applicable.
Notes
U.S. Census defines Latino(a) or Hispanic as a person of Cuban, Mexican, Puerto Rican, Central or South American, or other Spanish culture or origin regardless of race. We use Latino to be inclusive of our participants who collectively come from many countries.
References
Agénor, M. (2019). A Reproductive justice approach to patient-centered, structurally competent contraceptive care among diverse sexual minority US women. American Journal of Public Health, 109(12), 1626–1627.
Aiken, A. R., Creinin, M. D., Kaunitz, A. M., Nelson, A. L., & Trussell, J. (2014). Global fee prohibits postpartum provision of the most effective reversible contraceptives. Contraception, 90(5), 466–467. https://doi.org/10.1016/j.contraception.2014.08.005
American Academy of Pediatrics. (2021). AAP | National Resource Center for Patient/Family-Centered Medical Home. Retrieved October 1 from https://medicalhomeinfo.aap.org/Pages/default.aspx.
Ayoola, A. B., Zandee, G. L., Johnson, E., & Pennings, K. (2014). Contraceptive use among low-income women living in medically underserved neighborhoods. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 43(4), 455–464. https://doi.org/10.1111/1552-6909.12462
Bécares, L., Nazroo, J., & Kelly, Y. (2015). A longitudinal examination of maternal, family, and area-level experiences of racism on children’s socioemotional development: Patterns and possible explanations. Social Science and Medicine, 142, 128–135. https://doi.org/10.1016/j.socscimed.2015.08.025
Becerra, D., Androff, D., Messing, J. T., Castillo, J., & Cimino, A. (2015). Linguistic acculturation and perceptions of quality, access, and discrimination in health care among Latinos in the United States. Social Work in Health Care, 54(2), 134–157. https://doi.org/10.1080/00981389.2014.982267
Bello, J. K., Chavez, J., Liederbauer, V., Poston, L., Stones, R., & Stulberg, D. B. (2020). Perceptions of a Spanish language reproductive health self-assessment tool among Spanish-speaking women at a federally qualified health center. Journal of Immigrant and Minority Health. https://doi.org/10.1007/s10903-020-00988-6
Caskey, R., Stumbras, K., Rankin, K., Osta, A., Haider, S., & Handler, A. (2016). A novel approach to postpartum contraception: A pilot project of Pediatricians’ role during the well-baby visit. Contraception and Reproductive Medicine, 1, 7. https://doi.org/10.1186/s40834-016-0018-1
Center on the Develo** Child at Harvard University. (2021). Three Principles to Improve Outcomes for Children and Families, 2021 Update. https://develo**child.harvard.edu/.
Centers for Disease Control and Prevention. (2021). Unintended Pregnancy: Reproductive Health. (2021). https://www.cdc.gov/reproductivehealth/contraception/unintendedpregnancy/index.htm.
Cheng, T. L., Kotelchuck, M., & Guyer, B. (2012). Preconception women’s health and pediatrics: An opportunity to address infant mortality and family health. Academic Pediatric, 12(5), 357–359. https://doi.org/10.1016/j.acap.2012.04.006
Child Trends. (2018). Child Trends: Immigrant Children. Retrieved May 20, 2020 from https://www.childtrends.org/?indicators=immigrant-children.
Cooper, L. A., Hill, M. N., & Powe, N. R. (2002). Designing and evaluating interventions to eliminate racial and ethnic disparities in health care. Journal of General Internal Medicine, 17, 477–486.
Cosgrove, S., Moore-Monroy, M., Jenkins, C., Castillo, S. R., Williams, C., Parris, E., Tran, J. H., Rivera, M. D., & Brownstein, J. N. (2014). Community health workers as an integral strategy in the REACH US program to eliminate health inequities. Health Promotion Practice, 15(6), 795–802.
DeCamp, L. R., Polk, S., Chrismer, M. C., Giusti, F., Thompson, D. A., & Sibinga, E. (2015). Health care engagement of limited english proficient latino families: Lessons learned from advisory board development. Progress in Community Health Partnerships : Research, Education, and Action, 9(4), 521–530. https://doi.org/10.1353/cpr.2015.0068
DeCamp, L. R., Godage, S. K., Valenzuela-Araujo, D., Dominguez Cortez, J., Wu, L., Psoter, K. J., Quintanilla, K., Rivera Rodríguez, T., & Polk, S. (2020). A texting intervention in latino families to reduce ED use a randomized trial. Pediatrics https://doi.org/10.1542/peds.2019-1405
Dehlendorf, C., Rodriguez, M. I., Levy, K., Borrero, S., & Steinauer, J. (2010). Disparities in family planning. American Journal of Obstetrics and Gynecology, 202(3), 214–220. https://doi.org/10.1016/j.ajog.2009.08.022
Derose, K. P., Escarce, J. J., & Lurie, N. (2007). Immigrants and health care: sources of vulnerability. Health Affairs, 26(5), 1258–1268. https://doi.org/10.1377/hlthaff.26.5.1258
Downey, M. M., & Gomez, A. M. (2018). Structural competency and reproductive health. AMA Journal of Ethics, 20(3), 211–223. https://doi.org/10.1001/journalofethics.2018.20.3.peer1-1803
Downey, M. M., Arteaga, S., Villasenor, E., & Gomez, A. M. (2017). More than a destination: contraceptive decision making as a journey. Women’s Health Issues, 27(5), 539–545. https://doi.org/10.1016/j.whi.2017.03.004
El-Kamary, S. S., Higman, S. M., Fuddy, L., McFarlane, E., Sia, C., & Duggan, A. K. (2004). Hawaii’s healthy start home visiting program: Determinants and impact of rapid repeat birth. Pediatrics, 114(3), e317-326. https://doi.org/10.1542/peds.2004-0618
England, P., Mishel, E., & Caudillo, M. (2016). Increases in sex with same-sex partners and bisexual identity across cohorts of women (but not men). Sociological Science, 3, 951–970.
Finer, L. B., & Zolna, M. R. (2016). Declines in unintended pregnancy in the United States, 2008–2011. New England Journal of Medicine, 374(9), 843–852. https://doi.org/10.1056/NEJMsa1506575
Frost, J. J., Frohwirth, L., & Zolna, M. R. (2016). Contraceptive Needs and Services, 2014 Update. New York: Guttmacher Institute.
Fuentes-Afflick, E., Perrin, J. M., Moley, K. H., Diaz, A., McCormick, M. C., & Lu, M. C. (2021). Optimizing health and well-being for women and children. Health Aff (millwood), 40(2), 212–218. https://doi.org/10.1377/hlthaff.2020.01504
Garg, A., Jack, B., & Zuckerman, B. (2013). Addressing the social determinants of health within the patient-centered medical home: Lessons from pediatrics. JAMA, 309(19), 2001–2002. https://doi.org/10.1001/jama.2013.1471
Garg, A., Toy, S., Tripodis, Y., Silverstein, M., & Freeman, E. (2015). Addressing social determinants of health at well child care visits: A cluster RCT. Pediatrics, 135(2), e296. https://doi.org/10.1542/peds.2014-2888
Gresenz, C. R., Derose, K. P., Ruder, T., & Escarce, J. J. (2012). Health care experiences of hispanics in new and traditional US destinations. Medical Care Research and Review, 69(6), 663–678.
Guttmacher Institute. (2019). Unintended Pregnancy in the United States. Retrieved June, 2020 from https://www.guttmacher.org/fact-sheet/unintended-pregnancy-united-states#.
Harper, M. K. D., Loper, M. A. C., Louison, M. L. M., Morse, J. E., & Hill Nc, C. (2019). Stage-based implementation of Immediate Postpartum Long Acting Reversible Contraception Using a Reproductive Justice Framework. American Journal of Obstetrics and Gynecology. https://doi.org/10.1016/j.ajog.2019.11.1273
Harris, K., Sivamurthy, S., Mohiuddin, H., Aguila Gonzalez, A., Bui, T., Andrews, K., Cohen, J., McConnell, M., & Ahlers-Schmidt, C. (2020). Contraceptive counseling in the postpartum period: Could pediatricians have a role? Maternal and Child Health Journal, 24(7), 923–931. https://doi.org/10.1007/s10995-020-02947-x
Harris, P. A., Taylor, R., Thielke, R., Payne, J., Gonzalez, N., & Conde, J. G. (2009). Research electronic data capture (REDCap)-A metadata-driven methodology and workflow process for providing translational research informatics support. Journal of Biomedical Informatics, 42(2), 377–381.
Hasstedt, K., Desai, S., & Ansari-Thomas, Z. (2018). Immigrant Women’s Access to Sexual and Reproductive Health Coverage and Care in the United States. The Commonwealth Fund.
Hoffman, B. L., Schorge, J. O., Halvorson, L. M., Hamid, C. A., Corton, M. M., & Schaffer, J. I. (2020). Contraception and Sterilization. In Williams Gynecology, 4e. McGraw-Hill Education. obgyn.mhmedical.com/content.aspx?aid=1171528134
IMPLICIT Interconception Care Toolkit. (2016). (March of Dimes)
Interpregnancy Care: ACOG Obstetric Care Consensus. (2019). Obstetrics & Gynecology, 133.
Jackson, A. V., Karasek, D., Dehlendorf, C., & Foster, D. G. (2016). Racial and ethnic differences in women’s preferences for features of contraceptive methods. Contraception, 93(5), 406–411. https://doi.org/10.1016/j.contraception.2015.12.010
Jalisi, A., Vazquez, M. G., Bucay-Harari, L., Giusti, F., Contreras, J., Batkis, D., Batkis, M., Polk, S., Cook, B., & Page, K. R. (2018). “Testimonios”, A mental health support group for latino immigrants in an emergent latino community. Journal of Health Care for the Poor and Underserved, 29(2), 623–632. https://doi.org/10.1353/hpu.2018.0046
Kaiser Family Foundation. (2021). Postpartum Coverage Extension in the American Rescue Plan Act of 2021. Retrieved June 15 from https://www.kff.org/policy-watch/postpartum-coverage-extension-in-the-american-rescue-plan-act-of-2021/
Khoshnood, B., Lee, K.-S., Wall, S., Hsieh, H.-L., & Mittendorf, R. (1998). Short interpregnancy intervals and the risk of adverse birth outcomes among five racial/ethnic groups in the united states. American Journal of Epidemiology, 148(8), 798–805.
Kossler, K., Kuroki, L. M., Allsworth, J. E., Secura, G. M., Roehl, K. A., & Peipert, J. F. (2011). Perceived racial, socioeconomic and gender discrimination and its impact on contraceptive choice. Contraception, 84(3), 273–279. https://doi.org/10.1016/j.contraception.2011.01.004
Livingston, G. (2019a). A declining share of births in the US are to White women. Retrieved January 20, 2021 from https://pewrsr.ch/2YzvLa8.
Livingston, G. (2019b). Hispanic women no longer account for the majority of immigrant births in the US. https://www.pewresearch.org/fact-tank/2019/08/08/hispanic-women-no-longer-account-for-the-majority-of-immigrant-births-in-the-u-s/.
Luque, J. S., Soulen, G., Davila, C. B., & Cartmell, K. (2018). Access to health care for uninsured Latina immigrants in South Carolina. BMC Health Services Research, 18(1), 310. https://doi.org/10.1186/s12913-018-3138-2
National Survey of Family Growth. (2015-2017). Spanish CRQ Year 1 Female Birth Desires and Intentions. https://www.cdc.gov/nchs/data/nsfg/NSFG_2015-2017_FemaleCAPIlite_forPUF.pdf
Oakley, L. P., Harvey, S. M., & Lopez-Cevallos, D. F. (2018). Racial and ethnic discrimination, medical mistrust, and satisfaction with birth control services among young adult latinas. Women’s Health Issues, 28(4), 313–320. https://doi.org/10.1016/j.whi.2018.03.007
Palmer-Wackerly, A. L., Chadiez, V., Wayment, C., Baker, J., Adams, A., & Wheeler, L. A. (2020). Listening to the voices of community health workers: A multilevel, culture-centered approach to overcoming structural barriers in US latinx communities. Qualitative Health Research, 30(3), 423–436.
Perreira, K. M., & Pedroza, J. M. (2019). Policies of exclusion: Implications for the health of immigrants and their children. Annual Review of Public Health, 40, 147–166. https://doi.org/10.1146/annurev-publhealth-040218-044115
Pfizer. (2021). The Newest Vital Sign (NVS) A Health Literacy Assessment Tool for Patient Care and Research. https://www.pfizer.com/health/literacy/public-policy-researchers/nvs-toolkit.
Potter, J. E., Coleman-Minahan, K., White, K., Powers, D. A., Dillaway, C., Stevenson, A. J., Hopkins, K., & Grossman, D. (2017). Contraception after delivery among publicly insured women in Texas: Use compared with preference. Obstetrics and Gynecology, 130(2), 393–402. https://doi.org/10.1097/aog.0000000000002136
Potter, J. E., Hopkins, K., Aiken, A. R., Hubert, C., Stevenson, A. J., White, K., & Grossman, D. (2014). Unmet demand for highly effective postpartum contraception in Texas. Contraception, 90(5), 488–495. https://doi.org/10.1016/j.contraception.2014.06.039
Potter, J. E., Hubert, C., Stevenson, A. J., Hopkins, K., Aiken, A. R., White, K., & Grossman, D. (2016). Barriers to postpartum contraception in Texas and pregnancy within 2 years of delivery. Obstetrics and Gynecology, 127(2), 289–296. https://doi.org/10.1097/aog.0000000000001201
Rodriguez, M. I., Evans, M., & Espey, E. (2014). Advocating for immediate postpartum LARC: Increasing access, improving outcomes, and decreasing cost. Contraception, 90(5), 468–471. https://doi.org/10.1016/j.contraception.2014.07.001
Secura, G. M., Allsworth, J. E., Madden, T., Mullersman, J. L., & Peipert, J. F. (2010). The contraceptive CHOICE project: Reducing barriers to long-acting reversible contraception. American Journal of Obstetrics and Gynecology. https://doi.org/10.1016/j.ajog.2010.04.017
Sedgh, G., Ashford, L. S. Hussain, R. (2016). Unmet Need for Contraception In Develo** Countries Report. Guttmacher Institute. https://www.guttmacher.org/report/unmet-need-for-contraception-in-develo**-countries.
Shah, P. S., Balkhair, T., Ohlsson, A., Beyene, J., Scott, F., & Frick, C. (2011). Intention to become pregnant and low birth weight and preterm birth: A systematic review. Maternal and Child Health Journal, 15(2), 205–216. https://doi.org/10.1007/s10995-009-0546-2
Showell, N. N., Cole, K. W., Johnson, K., DeCamp, L. R., Bair-Merritt, M., & Thornton, R. L. J. (2016). Neighborhood and parental influences on diet and physical activity behaviors in young low-income pediatric patients. Clinical Pediatrics, 56(13), 1235–1243. https://doi.org/10.1177/0009922816684599
Srinivasan, S., Schlar, L., Rosener, S. E., Frayne, D. J., Hartman, S. G., Horst, M. A., Brubach, J. L., & Ratcliffe, S. (2018). Delivering interconception care during well-child visits: An IMPLICIT network study. Journal of the American Board of Family Medicine, 31(2), 201–210. https://doi.org/10.3122/jabfm.2018.02.170227
Tapales, A., Douglas-Hall, A., & Whitehead, H. (2018). The sexual and reproductive health of foreign-born women in the United States. Contraception, 98(1), 47–51. https://doi.org/10.1016/j.contraception.2018.02.003
Thiel de Bocanegra, H., Chang, R., Howell, M., & Darney, P. (2014). Interpregnancy intervals: impact of postpartum contraceptive effectiveness and coverage. American Journal of Obstetrics and Gynecology. https://doi.org/10.1016/j.ajog.2013.12.020
Troutman, M., Rafique, S., & Plowden, T. C. (2020). Are higher unintended pregnancy rates among minorities a result of disparate access to contraception? Contraception Reproductive Medicine, 5, 16. https://doi.org/10.1186/s40834-020-00118-5
U.S. Department of Health and Human Services. (2021). Social Determinants of Health; Healthy People 2030. Retrieved Sept 24 from https://health.gov/healthypeople/objectives-and-data/social-determinants-health
United States Census Bureau. (2017). American Community Survey (ACS) 1-year Estimates. Retrieved April 2020 from https://www.census.gov/programs-surveys/acs/technical-documentation/table-and-geography-changes/2017/1-year.html.
Upadhya, K. K., Burke, A. E., Marcell, A. V., Mistry, K., & Cheng, T. L. (2015). Contraceptive service needs of women with young children presenting for pediatric care. Contraception, 92(5), 508–512. https://doi.org/10.1016/j.contraception.2015.07.004
Upadhya, K. K., Psoter, K. J., Connor, K. A., Mistry, K. B., Levy, D. J., & Cheng, T. L. (2019). Cluster randomized trial of a pre/interconception health intervention for mothers in pediatric visits. Academic Pediatric. https://doi.org/10.1016/j.acap.2019.10.003
Venkataramani, M., Cheng, T. L., Solomon, B. S., & Pollack, C. E. (2017a). Addressing parental health in pediatrics: physician perceptions of relevance and responsibility. Clinical Pediatrics (phila), 56(10), 953–958. https://doi.org/10.1177/0009922817705189
Venkataramani, M., Cheng, T. L., Solomon, B. S., & Pollack, C. E. (2017b). How often are parents counseled about family planning during pediatric visits? results of a nationally representative sample. Academic Pediatric, 17(5), 476–478. https://doi.org/10.1016/j.acap.2016.03.001
Vespa, J., Medina, L., & Armstrong, D. M. (2020). Demographic Turning Points for the United States: Population Projections for 2020 to 2060. https://www.census.gov/content/dam/Census/library/publications/2020/demo/p25-1144.pdf.
Werth, S. R., Secura, G. M., Broughton, H. O., Jones, M. E., Dickey, V., & Peipert, J. F. (2015). Contraceptive continuation in Hispanic women. American Journal of Obstetrics and Gynecology, 212(3), 312.e311-318. https://doi.org/10.1016/j.ajog.2014.09.003
Whitener, K., & Corcoran, A. (2021). Getting Back on Track: A Detailed Look at Health Coverage Trends for Latino Children. Georgetown University Health Policy Institute Center for Children and Families. Retrieved October 1 from https://ccf.georgetown.edu/2021/06/08/health-coverage-trends-for-latino-children/.
Acknowledgements
The authors would like to thank Tatiahna Rivera, Sashini Godage,and Amanda Tuchler for their contributions to the study.
Funding
This study was supported by the Bright Futures Young Investigator Award from the Academic Pediatrics Association and funded by the Health Resources and Services Administration/Maternal and Child Health Bureau in cooperation with the American Academy of Pediatrics.
Author information
Authors and Affiliations
Contributions
Tania Caballero conceived and designed the study and wrote the manuscript. Dr Bou Delgado collected the data, Drs. Upadhya and Johnson approved the study design. Dr DeCamp approved the study design and analyzed the data. Dr Wu performed the statistical analysis. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
See Methods section.
Consent to Participate
See Methods section.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Caballero, T.M., Bou Delgado, L., Wu, L. et al. Mi Familia Entera: Contraceptive Use Among Spanish-Speaking Mothers of Young Children. Matern Child Health J 26, 139–148 (2022). https://doi.org/10.1007/s10995-021-03300-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-021-03300-6