Abstract
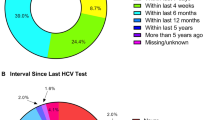
High uptake of HIV and hepatitis C (HCV) testing in Gay, bisexual, and other men who have sex with men (GBMSM) is needed to interrupt transmission. The objective was to identify subgroups with increased probability of lack of testing among HIV-negative GBMSM in Spain. Cross-sectional study including 3486 HIV-negative GBMSM attending prevention facilities in Madrid and Barcelona, 2018–2020. Data came from self-administered online sociodemographic, health, and risk behaviors questionnaires. Outcomes were lack of HCV (lifetime) and HIV (lifetime, last year) testing. Crude and adjusted prevalences and prevalence ratios were assessed for each outcome using negative binomial regression models. Lifetime lack of HIV and HCV testing prevalence was 6.3% and 35.8%, respectively, while lack of HIV testing in the last year was 22.4%. Prevalences were also substantial in GBMSM with high-risk behaviors. After sociodemographic adjustment, the highest probability of lack of HCV testing (lifetime) and HIV (last year) was among GBMSM with insufficient viral hepatitis knowledge, no history of STI, or HCV (or HIV) testing, aged < 25, non-outness about sex life with men, and less high-risk behaviors. Lack of HCV (lifetime) and HIV testing (last year) among HIV-negative GBMSM in Spain is still high, despite high-risk behaviors.

Similar content being viewed by others
Data Availability
The data that support the findings of this study may be available from the corresponding author upon reasonable request.
References
WHO Regional Office for Europe. (2022). European Centre for Disease Prevention and Control. HIV/AIDS surveillance in Europe 2022–2021 data. WHO Regional Office for Europe.
**, F., Dore, G. J., Matthews, G., Luhmann, N., Macdonald, V., Bajis, S., Baggaley, R., Mathers, B., Verster, A., & Grulich, A. E. (2021). Prevalence and incidence of hepatitis C virus infection in men who have sex with men: A systematic review and meta-analysis. Lancet Gastroenterol Hepatol, 6(1), 39–56. https://doi.org/10.1016/s2468-1253(20)30303-4
Bajis, S., Grebely, J., Hajarizadeh, B., Applegate, T., Marshall, A. D., Ellen Harrod, M., Byrne, J., Bath, N., Read, P., Edwards, M., Gorton, C., Hayllar, J., Cock, V., Peterson, S., Thomson, C., Weltman, M., Jefferies, M., Wood, W., & Haber, P. (2020). Hepatitis C virus testing, liver disease assessment and treatment uptake among people who inject drugs pre- and post-universal access to direct-acting antiviral treatment in Australia: The LiveRLife study. Journal of Viral Hepatitis, 27(3), 281–293. https://doi.org/10.1111/jvh.13233
WHO. (2022). Global health sector strategies on, respectively, HIV, viral hepatitis and sexually transmitted infections for the period 2022–2030. World Health Organization.
Rodger, A. J., Cambiano, V., Bruun, T., Vernazza, P., Collins, S., Degen, O., Corbelli, G. M., Estrada, V., Geretti, A. M., Beloukas, A., Raben, D., Coll, P., Antinori, A., Nwokolo, N., Rieger, A., Prins, J. M., Blaxhult, A., Weber, R., Van Eeden, A., & Lundgren, J. (2019). Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): final results of a multicentre, prospective, observational study. Lancet, 393(10189), 2428–2438. https://doi.org/10.1016/s0140-6736(19)30418-0
Rodger, A. J., Dunn, D., McCabe, L., Weatherburn, P., Lampe, F. C., Witzel, T. C., Burns, F., Ward, D., Pebody, R., Trevelion, R., Brady, M., Kirwan, P. D., Khawam, J., Delpech, V. C., Gabriel, M., Collaco-Moraes, Y., Phillips, A. N., & McCormack, S. (2020). Sexual risk and HIV testing disconnect in men who have sex with men (MSM) recruited to an online HIV self-testing trial. HIV Medicine, 21(9), 588–598. https://doi.org/10.1111/hiv.12919
European Centre for Disease Prevention and Control. (2020). Monitoring the responses to hepatitis B and C epidemics in EU/EEA Member States, 2019. ECDC.
Estirado Gómez, A., Justo Gil, S., Limia, A., Avellón, A., Arce Arnáez, A., González-Rubio, R., Diaz, A., & del Amo, J. (2021). Prevalence and undiagnosed fraction of hepatitis C infection in 2018 in Spain: Results from a national population-based survey. European Journal of Public Health, 31(6), 1117–1122. https://doi.org/10.1093/eurpub/ckab069
Nuñez, O., Hernando, V., & Díaz, A. (2018). Estimating the number of people living with HIV and the undiagnosed fraction in Spain in 2013. AIDS, 32(17), 2573–2581. https://doi.org/10.1097/qad.0000000000001989
Mocroft, A., Lundgren, J., Antinori, A., Monforte, A., Brännström, J., Bonnet, F., Brockmeyer, N., Casabona, J., Castagna, A., Costagliola, D., De Wit, S., Fätkenheuer, G., Furrer, H., Jadand, C., Johnson, A., Lazanas, M., Leport, C., Moreno, S., Mussini, C., & Kirk, O. (2015). Late presentation for HIV care across Europe: Update from the collaboration of observational HIV Epidemiological Research Europe (COHERE) study, 2010 to 2013. Eurosurveillance. https://doi.org/10.2807/1560-7917.Es.2015.20.47.30070
UNAIDS. (2022). IN DANGER: UNAIDS global AIDS update 2022. Joint United Nations Programme on HIV/AIDS.
Zheng, Y., Ying, M., Zhou, Y., Lin, Y., Ren, J., & Wu, J. (2021). Global burden and changing trend of hepatitis C virus infection in HIV-positive and HIV-negative MSM: A systematic review and meta-analysis. Frontiers in Medicine (Lausanne), 8, 774793. https://doi.org/10.3389/fmed.2021.774793
WHO. (2021). Interim guidance for country validation of viral hepatitis elimination. World Health Organization.
WHO. (2020). Consolidated guidelines on HIV testing services, 2019. World Health Organization.
Workowski, K. A., Bachmann, L. H., Chan, P. A., Johnston, C. M., Muzny, C. A., Park, I., Reno, H., Zenilman, J. M., & Bolan, G. A. (2021). Sexually transmitted infections treatment guidelines, 2021. MMWR - Recommendations and Reports, 70(4), 1–187. https://doi.org/10.15585/mmwr.rr7004a1
Werner, R. N., Gaskins, M., Nast, A., & Dressler, C. (2018). Incidence of sexually transmitted infections in men who have sex with men and who are at substantial risk of HIV infection - A meta-analysis of data from trials and observational studies of HIV pre-exposure prophylaxis. PLoS ONE, 13(12), e0208107. https://doi.org/10.1371/journal.pone.0208107
Han, R., Zhou, J., Francois, C., & Toumi, M. (2019). Prevalence of hepatitis C infection among the general population and high-risk groups in the EU/EEA: A systematic review update. BMC Infectious Diseases, 19(1), 655. https://doi.org/10.1186/s12879-019-4284-9
Nijmeijer, B. M., Koopsen, J., Schinkel, J., Prins, M., & Geijtenbeek, T. B. (2019). Sexually transmitted hepatitis C virus infections: current trends, and recent advances in understanding the spread in men who have sex with men. Journal of the International AIDS Society, 22(Suppl6), e25348. https://doi.org/10.1002/jia2.25348
Macgregor, L., Desai, M., Martin, N. K., Nicholls, J., Hickson, F., Weatherburn, P., Hickman, M., & Vickerman, P. (2020). Scaling up screening and treatment for elimination of hepatitis C among men who have sex with men in the era of HIV pre-exposure prophylaxis. EClinicalMedicine, 19, 100217. https://doi.org/10.1016/j.eclinm.2019.11.010
Hagan, H., Jordan, A. E., Neurer, J., & Cleland, C. M. (2015). Incidence of sexually transmitted hepatitis C virus infection in HIV-positive men who have sex with men. AIDS, 29(17), 2335–2345. https://doi.org/10.1097/qad.0000000000000834
Rockstroh, J. K., & Boesecke, C. (2020). Hepatitis C virus treatment as prevention: challenges and opportunities in men who have sex with men. The Journal of Infectious Diseases, 222(Supplement_9), S782–S788. https://doi.org/10.1093/infdis/jiaa096
The EMIS Network. (2019). EMIS-2017 – The European Men-Who-Have-Sex-With-Men internet Survey. Key findings from 50 countries. European Centre for Disease Prevention and Control.
Scott, C., Day, S., Low, E., Sullivan, A., Atkins, M., & Asboe, D. (2010). Unselected hepatitis C screening of men who have sex with men attending sexual health clinics. Journal of Infection, 60(5), 351–353. https://doi.org/10.1016/j.**f.2010.01.013
Koretz, R. L., Lin, K. W., Ioannidis, J. P., & Lenzer, J. (2015). Is widespread screening for hepatitis C justified? BMJ, 350, g7809. https://doi.org/10.1136/bmj.g7809
Hoornenborg, E., Achterbergh, R. C. A., Schim van der Loeff, M. F., Davidovich, U., Hogewoning, A., de Vries, H. J. C., Schinkel, J., Prins, M., & van de Laar, T. J. W. (2017). MSM starting preexposure prophylaxis are at risk of hepatitis C virus infection. AIDS, 31(11), 1603–1610. https://doi.org/10.1097/qad.0000000000001522
McFaul, K., Maghlaoui, A., Nzuruba, M., Farnworth, S., Foxton, M., Anderson, M., Nelson, M., & Devitt, E. (2015). Acute hepatitis C infection in HIV-negative men who have sex with men. Journal of Viral Hepatitis, 22(6), 535–538. https://doi.org/10.1111/jvh.12366
Garvey, L. J., Cooke, G. S., Smith, C., Stingone, C., Ghosh, I., Dakshina, S., Jain, L., Waters, L. J., Mahungu, T., Ferro, F., Sood, C., Freeman, C., Phillips, C., Dhairyawan, R., Burholt, R., Sharp, H., Ullah, S., Gilleece, Y., Brown, A., & Bhagani, S. (2021). Decline in hepatitis C virus (HCV) incidence in men who have sex with men living with human immunodeficiency virus: Progress to HCV microelimination in the United Kingdom? Clinical Infectious Disease, 72(2), 233–238. https://doi.org/10.1093/cid/ciaa021
Macgregor, L., Ward, Z., Martin, N. K., Nicholls, J., Desai, M., Hickson, F., Weatherburn, P., Hickman, M., & Vickerman, P. (2021). The cost-effectiveness of case-finding strategies for achieving hepatitis C elimination among men who have sex with men in the UK. Journal of Viral Hepatitis, 28(6), 897–908. https://doi.org/10.1111/jvh.13503
Ireland, G., Higgins, S., Goorney, B., Ward, C., Ahmad, S., Stewart, C., Simmons, R., Lattimore, S., & Lee, V. (2017). Evaluation of hepatitis C testing in men who have sex with men, and associated risk behaviours, in Manchester UK. Sex Transmitted Infections, 93(6), 404–409. https://doi.org/10.1136/sextrans-2016-052876
Braun, D. L., Hampel, B., Martin, E., Kouyos, R., Kusejko, K., Grube, C., Flepp, M., Stöckle, M., Conen, A., Béguelin, C., Schmid, P., Delaloye, J., Rougemont, M., Bernasconi, E., Rauch, A., Günthard, H. F., Böni, J., & Fehr, J. S. (2019). High number of potential transmitters revealed in a population-based systematic hepatitis C virus RNA screening among human immunodeficiency virus-infected men who have sex with men. Clinical Infectious Diseases, 68(4), 561–568. https://doi.org/10.1093/cid/ciy545
Marcus, U., Nöstlinger, C., Rosińska, M., Sherriff, N., Gios, L., Dias, S. F., Gama, A. F., Toskin, I., Alexiev, I., Naseva, E., Schink, S. B., & Mirandola, M. (2018). Behavioural and demographic correlates of undiagnosed HIV infection in a MSM sample recruited in 13 European cities. BMC Infectious Diseases, 18(1), 368. https://doi.org/10.1186/s12879-018-3249-8
Vourli, G., Noori, T., Pharris, A., Porter, K., Axelsson, M., Begovac, J., Cazein, F., Costagliola, D., Cowan, S., Croxford, S., D’Arminio Monforte, A., Delpech, V., Díaz, A., Girardi, E., Gunsenheimer-Bartmeyer, B., Hernando, V., Leierer, G., Lot, F., Nunez, O., & Touloumi, G. (2020). Human immunodeficiency virus continuum of care in 11 European Union Countries at the end of 2016 overall and by key population: Have we made progress? Clinical Infectious Diseases, 71(11), 2905–2916. https://doi.org/10.1093/cid/ciaa696
McCormack, S., Dunn, D. T., Desai, M., Dolling, D. I., Gafos, M., Gilson, R., Sullivan, A. K., Clarke, A., Reeves, I., Schembri, G., Mackie, N., Bowman, C., Lacey, C. J., Apea, V., Brady, M., Fox, J., Taylor, S., Antonucci, S., Khoo, S. H., & Gill, O. N. (2016). Pre-exposure prophylaxis to prevent the acquisition of HIV-1 infection (PROUD): Effectiveness results from the pilot phase of a pragmatic open-label randomised trial. Lancet, 387(10013), 53–60. https://doi.org/10.1016/s0140-6736(15)00056-2
Molina, J. M., Capitant, C., Spire, B., Pialoux, G., Cotte, L., Charreau, I., Tremblay, C., Le Gall, J. M., Cua, E., Pasquet, A., Raffi, F., Pintado, C., Chidiac, C., Chas, J., Charbonneau, P., Delaugerre, C., Suzan-Monti, M., Loze, B., Fonsart, J., & Delfraissy, J. F. (2015). On-demand preexposure prophylaxis in men at high risk for HIV-1 infection. New England Journal of Medicine, 373(23), 2237–2246. https://doi.org/10.1056/NEJMoa1506273
Leenen, J., Wijers, J. N. A. P., Daas, C. D., Wit, Jd., Hoebe, C. J. P. A., & Dukers-Muijrers, N. H. T. M. (2022). HIV testing behaviour and associated factors in men who have sex with men by level of urbanisation: A cross-sectional study in the Netherlands. British Medical Journal Open, 12(1), e049175. https://doi.org/10.1136/bmjopen-2021-049175
Mirandola, M., Gios, L., Sherriff, N., Marcus, U., Toskin, I., Rosinska, M., et al. (2018) Quantifying unmet prevention needs among MSM in Europe through a multi-site bio-behavioural survey. Euro Surveill. 23(49), 1800097. https://doi.org/10.2807/1560-7917.ES.2018.23.49.1800097
Vaux, S., Chevaliez, S., Saboni, L., Sauvage, C., Sommen, C., Barin, F., Alexandre, A., Jauffret-Roustide, M., Lot, F., & Velter, A. (2019). Prevalence of hepatitis C infection, screening and associated factors among men who have sex with men attending gay venues: a cross-sectional survey (PREVAGAY), France, 2015. BMC Infectious Diseases, 19(1), 315. https://doi.org/10.1186/s12879-019-3945-z
Brener, L., Ellard, J., Murphy, D., & Callander, D. (2013). Perceptions and deflections: Associations between attitudes towards people with hepatitis C and testing for hepatitis C among Australian gay and bisexual men. Sexual Health, 10(3), 268–274. https://doi.org/10.1071/SH12179
Lambers, F. A., Prins, M., Davidovich, U., & Stolte, I. G. (2014). High awareness of hepatitis C virus (HCV) but limited knowledge of HCV complications among HIV-positive and HIV-negative men who have sex with men. AIDS Care, 26(4), 416–424. https://doi.org/10.1080/09540121.2013.832721
Clerc, O., Darling, K., Calmy, A., Dubois-Arber, F., & Cavassini, M. (2016). Hepatitis C virus awareness among men who have sex with men in Southwest Switzerland. Sexually Transmitted Diseases, 43(1), 44–48. https://doi.org/10.1097/olq.0000000000000378
Knick, T., Sherbuk, J. E., & Dillingham, R. (2019). Knowledge of hepatitis C risk factors is lower in high incidence regions. Journal of Community Health, 44(1), 12–15. https://doi.org/10.1007/s10900-018-0545-6
Brener, L., Murphy, D. A., Cama, E. J., & Ellard, J. (2015). Hepatitis C risk factors, attitudes and knowledge among HIV-positive, HIV-negative and HIV-untested gay and bisexual men in Australia. Sex Health, 12(5), 411–417. https://doi.org/10.1071/sh14239
Shehata, N., Austin, T., Ha, S., & Timmerman, K. (2018). Barriers to and facilitators of hepatitis C virus screening and testing: A sco** review. Canada Communicable Disease Report, 44(7–8), 166–172. https://doi.org/10.14745/ccdr.v44i78a03
den Daas, C., Goenee, M., Bakker, B. H., de Graaf, H., & Op de Coul, E. L. (2015). Comparing databases: determinants of sexually transmitted infections, HIV diagnoses, and lack of HIV testing among men who have sex with men. BMC Public Health, 15, 1114. https://doi.org/10.1186/s12889-015-2445-3
Lian, J., Chen, X., Su, X., Si, M., Dai, Z., Fu, J., Yu, F., Mi, G., & Liu, Y. (2023). HIV testing and related factors among 50 years and older MSM in China: Results from a cross-sectional study. AIDS Care, 35(4), 608–613. https://doi.org/10.1080/09540121.2022.2060493
Wu, M. Y., Gong, H. Z., Hu, K. R., Zheng, H. Y., Wan, X., & Li, J. (2021). Effect of syphilis infection on HIV acquisition: A systematic review and meta-analysis. Sex Transmitted Infections, 97(7), 525–533. https://doi.org/10.1136/sextrans-2020-054706
Fernández-Dávila, P., Folch, C., Ferrer, L., Soriano, R., Diez, M., & Casabona, J. (2015). Hepatitis C virus infection and its relationship to certain sexual practices in men-who-have-sex-with-men in Spain: Results from the European MSM internet survey (EMIS). Enfermedades Infecciosas y Microbiologia Clinica, 33(5), 303–310. https://doi.org/10.1016/j.eimc.2014.07.012
Price, J. C., McKinney, J. E., Crouch, P. C., Dillon, S. M., Radix, A., Stivala, A., Carollo, J. R., & Fierer, D. S. (2019). Sexually acquired hepatitis C infection in HIV-uninfected men who have sex with men using preexposure prophylaxis against HIV. Journal of Infectious Diseases, 219(9), 1373–1376. https://doi.org/10.1093/infdis/jiy670
Fitzpatrick, T., Pan, S. W., Tang, W., Guo, W., & Tucker, J. D. (2018). HBV and HCV test uptake and correlates among men who have sex with men in China: A nationwide cross-sectional online survey. Sex Transmitted Infections, 94(7), 502–507. https://doi.org/10.1136/sextrans-2018-053549
Crowell, T. A., Qian, H., Tiemann, C., Lehmann, C., Boesecke, C., Stoehr, A., Hartikainen, J., Esser, S., Bickel, M., Spinner, C. D., Schneeweiß, S., Cordes, C., Brockmeyer, N., Jessen, H., Robb, M. L., Michael, N. L., Jansen, K., & Streeck, H. (2021). Factors associated with testing for HIV and hepatitis C among behaviorally vulnerable men in Germany: A cross-sectional analysis upon enrollment into an observational cohort. AIDS Research and Therapy, 18(1), 52. https://doi.org/10.1186/s12981-021-00378-4
Feldman, E. B., Balise, R., Schiff, E., Whitehead, N., & Thomas, E. (2017). Barriers to hepatitis C screening in a minority population: A comparison of hepatitis C and human immunodeficiency virus screening rates at a community STD clinic in Miami Florida. Journal of Community Health, 42(5), 921–925. https://doi.org/10.1007/s10900-017-0335-6
Rodriguez-Rincon, D., Hocking, L., Parks, S., Amato-Gauci, A. J., & Semenza, J. C. (2020). Barriers for the MSM population to access testing for HIV in France, Poland, the UK and across Europe: A qualitative study. Journal of HIV/AIDS and Infectious Diseases, 6, 1–27.
Acknowledgements
The Methysos Project Group: María del Carmen Burgos and César Pérez Romero (Instituto de Salud Carlos III, Madrid); José Antonio San Juan Bueno (Asociación Pink Peace, Madrid); Francisca Román Urrestarazu, Jesus E. Ospina, and Miguel Alarcón Gutiérrez (Agència de Salut Pública de Barcelona, Barcelona); Jorge del Romero, Carmen Rodríguez, Sonsoles del Corral Del Campo, Natividad Jerez Zamora, Marta Ruiz Fernández, and Montserrat González Polo (Centro Sanitario Sandoval, Madrid); María Jesús Barbera Gracia, Luis López Pérez, Claudia Broto Cortes, and Julio Morais Martin (UITS Drassanes, Barcelona).
Funding
This work was supported by the Instituto de Salud Carlos III—Acción Estratégica en Salud Intramural [PI18CIII/00047 to GB and PI17CIII/00037 to MJB] and Río-Hortega [CM20CIII/00001 to JP].
Author information
Authors and Affiliations
Consortia
Contributions
GB, MJB, and JP developed the study concept. JP, MJB, JMG, and GB designed the study. MJB, JMG, DP, OA, and JNG acquired the data. JP and MD reviewed the literature, analyzed the data, and interpreted the results. MJB, GB, and JMG assisted in the analyses and interpretation. GB, MJB, and JMG supervised data analysis. JP wrote the first draft. All authors were involved in data interpretation, revised the manuscript critically for important intellectual content and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
JP declares lecture fees from Gilead. All other authors have nothing to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The members of the The Methysos Project Group are listed in acknowledgements section.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Politi, J., Donat, M., Guerras, J.M. et al. Gaps in HIV and Hepatitis C Testing Among 3486 HIV-Negative Men Who have Sex with Men in Spain in the Era of Highly Effective Antiviral Therapies. J Community Health 49, 139–155 (2024). https://doi.org/10.1007/s10900-023-01259-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-023-01259-9