Abstract
Purpose
The ablation index (AI), developed as a radiofrequency (RF) catheter ablation composite component endpoint, which incorporates contact force (CF), time, and power in a weighted formula, has been reported to be useful for a durable pulmonary vein isolation (PVI) to treat atrial fibrillation (AF). No study has reported the target AI value for the SVC isolation (SVCI). In this study, we aimed to investigate the target AI for the SVCI.
Methods
Thirty-six AF patients who underwent an initial SVCI were enrolled. Ablation was performed at 556 points. The sites where dormant conduction was induced or additional ablation was needed were defined as touch up sites (n = 36). We compared the energy deliver time, power, generator impedance (GI) drop, local bipolar voltage, contact force (CF), force–time integral (FTI), and AI between the touch up sites and the no touch up sites (n = 520).
Results
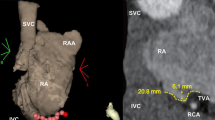
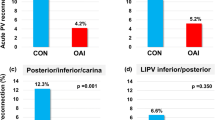
The FTI and AI were significantly lower at the touch up sites (touch up sites vs. no touch up sites; FTI, 126.5 [99.3–208.8] vs. 244 [184–340.8], p < 0.0001; AI, 350.1 ± 43.6 vs. 277.2 ± 21.8, p < 0.0001). The median value of the AI at the no touch up sites was 350, and no reconnections were seen where the minimum AI value was more than 308. Most of the touch up sites were located in the anterior wall and lateral wall (anterior wall, 20/36 sites [55.6%]; lateral wall, 10/36 sites [27.8%]; septal wall, 6/36 sites [16.7%]; posterior wall, 0/36sites [0.0%]).
Conclusion
The target AI value for the SVCI should be 350, and at least 308 would be needed.




Similar content being viewed by others
Availability of data and material
Available upon request.
Code availability
Available upon request.
References
Haissaguerre M, Jais P, Shah DC, et al. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med. 1998;339:659–66.
Terasawa T, Balk EM, Chung M, et al. Systematic review: comparative effectiveness of radiofrequency catheter ablation for atrial ablation. Ann Intern Med. 2009;151:191–202.
Calkins H, Hindricks G, Cappato R, et al. 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Heart Rhythm. 2017;14(10):e275–444.
Goya M, Ouyang F, Ernst S, et al. Electroanatomic map** and catheter ablation of breakthroughs from the right atrium to the superior vena cava in patients with atrial fibrillation. Circulation. 2002;106:1317–20.
Cappato R, Negroni S, Pecora D, et al. Prospective assessment of late conduction recurrence across radiofrequency lesions producing electrical disconnection at the pulmonary vein ostium in patients with atrial fibrillation. Circulation. 2003;108(13):1599–604.
Gerstenfeld EP, Callans DJ, Dixit S, et al. Incidence and location of focal atrial fibrillation triggers in patients undergoing repeat pulmonary vein isolation: implications for ablation strategies. J Cardiovasc Electrophysiol. 2003;14(7):685–90.
Ouyang F, Antz M, Ernst S, et al. Recovered pulmonary vein conduction as a dominant factor for recurrent atrial tachyarrhythmias after complete circular isolation of the pulmonary veins: lessons from double Lasso technique. Circulation. 2005;111(2):127–35.
Hitoshi M, Ritsushi K, Naokata S, et al. Relations between the ablation index, lesion formation, and incidence of steam pops. J Arrythm. 2019;35:636–44.
Das M, Loveday JJ, Wynn GJ, et al. Ablation index, a novel marker of ablation lesion quality: prediction of pulmonary vein reconnection at repeat electrophysiology study and regional differences in target values. Europace. 2017;19:775–83.
Nakagawa H, Ikeda A, Govari A, et al. Prospective study using a new formula incorporating contact force, radiofrequency power and application time (force-power-time index) for quantifying lesion formation to guide long continuous atrial lesions in the beating canine heart. Circulation. 2018;128:A12104(abstr).
Solimene F, Schillaci V, Shopova G, et al. Safety and efficacy of atrial fibrillation ablation guided by ablation index module. J Interv Card Electrophysiol. 2019;54:9–15.
Okamatsu H, Okumura K, Kaneko S, et al. Ablation index-guided high-power radiofrequency application shortens the procedure time with similar outcomes to conventional power application in atrial fibrillation ablation. Circ Rep. 2021;3:559–68.
Paula M, Stefan K, Spyridon L, et al. Ablation index for catheter ablation of atrial fibrillation -clinical applicability and comparison with force-time integral. Circ J. 2018;82:2722–7.
Lee So-Ryoung, Choi Eue-Keun, Lee Eui-Jae, et al. Efficacy of the optimal ablation index–targeted strategy for pulmonary vein isolation in patients with atrial fibrillation: the OPTIMUM study results. J Interv Card Electrophysiol. 2019;55:171–81.
Zhang T, Wang Y, Han Z, et al. Cavotricuspid isthmus ablation using ablation index in typical atrial flutter. J cardiovasc electrophysiol. 2019;30:2414–9.
Miyazaki S, Taniguchi H, Kusa S, et al. Conduction recovery after electrical isolation of superior vena cava – prevalence and electrophysiological properties. Circ J. 2013;77:352–8.
Sanchez-Quintana D, Cabrera JA, Climent V, et al. Anatomic relations between the esophagus and left atrium and relevance for ablation of atrial fibrillation. Circulation. 2005;112:1400–5.
Joseph BM, Prashanthan S, Neil CD, et al. Phased-array intracardiac echocardiography for defining cavotricuspid isthmus anatomy during radiofrequency ablation of typical atrial flutter. J Cardiovasc Electrophysiol. 2003;14:591–7.
Kholova I, Kautzner J. Morphology of atrial myocardial extensions into human caval veins. Circulation. 2004;110:483–8.
Nagashima K, Watanabe I, Okumura Y, et al. High-voltage zones within the pulmonary vein antra: Major determinants of acute pulmonary vein reconnections after atrial fibrillation ablation. J Interv Card Electrophysiol. 2017;49:137–45.
Suraj K, Benoit D, David JC, et al. Contact electroanatomic map** derived voltage criteria for characterizing left atrial scar in patients undergoing ablation for atrial fibrillation. J Cardiovasc Electrophysiol. 2014;25:1044–52.
Winkle RA, Moskovitz R, Hardwin Mead R, et al. Atrial fibrillation ablation using very short duration 50W ablations and contact force sensing catheters. J Interv Card Electrophysiol. 2018;52(1):1–8.
Chen S, Schmidt B, Bordignon S, et al. Ablation Index-guided 50W ablation for pulmonary vein isolation in patients with atrial fibrillation: procedural data, lesion analysis, and initial results from the FAFA AI high power study. J Cardiovasc Electrophysiol. 2019;30(12):2724–31.
Eran L, Cory MT, Michael B, et al. High-power and short-duration ablation for pulmonary vein isolation. ~Biophysical Characterization~. JACC: Clin Electrophysiol 2018;4(4):467–479.
Michael B, Fernando MC, Eran L, et al. High-power and short-duration ablation for pulmonary vein isolation: Safety, efficacy, and long-term durability. J Cardiovasc Electrophysiol. 2018;29:1287–96.
Shinsuke M, Kazuya Y, Kanae H, et al. SVC map** using an ultra-high resolution 3-dimensional map** system in patients with and without AF. JACC: Clin Electrophysiol 2019;5:958–967.
Acknowledgements
We appreciate the help in proofreading our manuscript by Mr. John Martin.
Author information
Authors and Affiliations
Contributions
HM and DK: study conception and design. MY, AK, MY, YG, and AS: data collection and data analysis. AH, KT, and IY: manuscript revision. HT and RK: study supervision.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the institutional review board.
Consent to participate/publication
All patients provided their informed consent to the procedure and publication.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kawano, D., Mori, H., Tsutsui, K. et al. The target ablation index values for electrical isolation of the superior vena cava. J Interv Card Electrophysiol 64, 687–694 (2022). https://doi.org/10.1007/s10840-021-01112-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-01112-w