Abstract
The study presented here was conducted over a period of 4 years (2001–2004) to investigate changes in the number of S. maltophilia isolates detected per 1,000 patient days and to look at the incidence density of nosocomial infections caused by S. maltophilia. The analysis was based on data provided by 34 German intensive care units participating continuously in the national project “Surveillance of Antimicrobial Use and Resistance in ICUs”; 31 of these ICUs reported nosocomial infections to the German infection surveillance system, KISS, during the study period.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In recent decades, Stenotrophomonas maltophilia has risen to prominence as an important nosocomial pathogen, particularly in immunosuppressed patients [1, 2]. It has been hypothesized that the increase in nosocomial infections caused by S. maltophilia is due partly to the changing nature of the hospital patient population and partly to changes in antibiotic usage [3, 4]. However, most reports of increases in the number of strains isolated and of nosocomial infections caused by S. maltophilia come from individual institutions and date from the 1980s and 1990s [5, 6]. The increase was often found to be associated with a greater use of carbapenems, a broad-spectrum class of antibiotic to which S. maltophilia is intrinsically resistant and which had only recently been introduced at that time [7]. Our objective was to analyze data from multiple German ICUs participating continuously in the Surveillance of Antimicrobial Use and Resistance in ICUs (SARI) project in order to investigate whether the rates of isolation and nosocomial infections caused by S. maltophilia rose between 2001 and 2004.
Materials and methods
Data from 34 intensive care units (ICUs) participating continuously in SARI from 2001 through 2004 were analyzed. SARI is a prospective unit- and laboratory-based surveillance system that collects data on 13 pathogens, i.e. Staphylococcus aureus, coagulase-negative staphylococci, Enterococcus faecalis, Enterococcus faecium, Pseudomonas aeruginosa, S. maltophilia (SM), Enterobacter cloacae, Citrobacter spp, Serratia marcescens, Acinetobater baumannii, Streptococcus pneumoniae, Escherichia coli and Klebsiella pneumoniae. Isolates documented were non-duplicate. The incidence density of S. maltophilia per 1,000 patient days (SM/1,000 pd) was determined by dividing the number of S. maltophilia isolates by the total number of patient days multiplied by 1,000. Monthly antimicrobial usage data were obtained from computerized hospital databases.
SARI ICUs report nosocomial infections (NI) using Centers for Disease Control and Prevention definitions for ventilator-associated pneumonia, central venous catheter-associated bloodstream infection, and catheter-associated urinary tract infection to KISS, the German infection surveillance system. In KISS, up to four pathogens isolated from the same patient can be recorded as causative pathogens of a NI. Structure parameters were obtained on the type of ICU (medical, surgical, interdisciplinary—all of the ICUs were for adults), affiliation status (university yes/no), size of hospital (< or ≥ 600 beds), length of stay (days), central venous catheter utilization (central line days per 100 patient days), ventilator utilization rate (ventilator days per 100 patient days) and urinary catheter utilization rate (number of urinary catheter days per 100 patient days). The study designs utilized by SARI and KISS have been described in detail elsewhere [8, 9]. To determine changes during this 4-year period, we compared the figures for 2001 with those for 2004, which we obtained using the incidence density test. ICU-based SM/1,000 pd was tested using Wilcoxon’s test. Furthermore, structure parameters were correlated with SM/1,000 pd and tested using the Wilcoxon t test for differences in ICUs with an increase in SM/1,000 pd and for those with a decrease.
All significance levels were set at p = 0.05, two-tailed. Statistical analysis were performed using SAS version 9.1, SPSS 12.0 and Epi-Info 6.04.
Results and discussion
From January 2001 through December 2004, 34 ICUs continuously provided data and were thus included in the analysis. The 34 ICUs are located in 21 geographically distinct hospitals. Of the 34 ICUs, 12 are in university hospitals, while 20 have an affiliation with a medical school; 13 ICUs are interdisciplinary, 12 are surgical and 9 are medical. ICU bed numbers range from 6 to 26, with a median of 12. The data covered a total of 51,536 isolates and 576,446 patient days.
The number of SARI isolates per 1,000 pd ranged from 17 to 165, with the median being 81. The pooled mean SM/1,000 pd was 2.2 (median 1.6, range 0.2–7.6). Nosocomial infection data from KISS were available from 31 SARI-ICUs. The pooled mean number of nosocomial infections caused by SM/1,000 pd was 0.134 (median 0.119, range 0–0.467). Fifteen of 31 ICUs (35%) reported no nosocomial infections caused by SM.
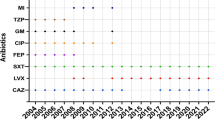
No significant increase in SM/1,000 pd test results obtained with the Wilcoxon test was observed over the 4-year period. The incidence density of SM/1,000 pd increased in 16 and decreased in 18 ICUs (see Fig. 1). However, when the SM/1,000 pd of all 34 SARI ICUs was tested with the incidence test, a significant decrease was evident (p = 0.002) in 2001 compared with 2004. The number of nosocomial infections caused by SM/1,000 pd did not change significantly (p = 0.772) in SARI ICUs according to the incidence density test (see Table 1). Correlation of SM/1,000 pd with structure parameters did not produce statistically significant results. Nor did the structure parameter differ in ICUs with an increase and in those with a decrease in SM/1,000 pd.
Using KISS data, we were actually able to identify nosocomial infections caused by SM per 1,000 pd (NI-SM/1,000 pd) over a period of 7 years (1998–2004): In 1998, 46 ICUs joined KISS and, collectively, they had a NI-SM/1,000 pd of 0.193. In 2004, 251 ICUs were participating in KISS, and the NI-SM/1,000 pd decreased to 0.121 (between 1997 and 2004 the mean was 0.140). If we consider nosocomial infections in which S. maltophilia was reported to be the only causative agent, the NI-only SM/1,000 pd was 0.054 in 1998 and 0.052 in 2004.
S. maltophilia is generally considered to be an opportunistic pathogen of growing significance [4, 10]. A large study conducted from 1997 to 2001 covering 18,569 non-fermentative gram-negative bacilli found that, at 8%, S. maltophilia was the third most frequently isolated pathogen from clinical specimens [11]. Studies conducted at individual centers report of S. maltophilia increasing at their institutions. Krcmery et al. [12] found that the number of S. maltophilia bacteremias at a cancer referral centre increased significantly from 1989 to 1996 following the introduction of imipenem in 1991. At a university hospital in the USA, the annual isolation rates doubled from 7.1 to 14.1 per 10,000 discharges within 4 years (1981–1984) [5]. At a Kuwaiti hospital, the number of S. maltophilia isolates increased between 1993 and 1997, and the change correlated significantly with an increase in the annual consumption of carbapenems [6]. Our data revealed an increase in the incidence density of SM/1,000 pd in 16 ICUs. However, the incidence of SM/1,000 pd decreased in the other 18 ICUs, suggesting that, overall, the situation is heterogeneous. Structure parameters did not differ in either group. When testing the data of the 34 ICUs with the incidence test, or, respectively, the incidence density test, a statistically significant decrease was found, even though total antibiotic use and carbapenem use increased slightly during the 4-year period. With respect to nosocomial infections caused by S. maltophilia, we did not observe a significant change over a period of 4 years in the SARI-ICUs reporting NIs to the KISS system. Even over a period of 7 years (1998–2004), nosocomial infections caused by SM in KISS-ICUs fluctuated between 0.193 and 0.121, but did not increase.
In conclusion, S. maltophilia is an important nosocomial pathogen that displays significant morbidity and mortality. Our results can be used as benchmarking data and show a mean incidence density of 2.2 SM/1,000 pd and a mean incidence density of nosocomial infections caused by S. maltophilia (SM-NI/1,000 pd) of 0.134. However, our multicenter data indicated that the incidence density of S. maltophilia is heterogeneous within individual ICUs, as is the incidence density of NIs caused by this pathogen, but that, overall, S. maltophilia did not increase in German SARI-ICUs between the years 2001 and 2004.
References
Senol E (2004) Stenotrophomonas maltophilia: the significance and role as a nosocomial pathogen. J Hosp Infect 57:1–7
Calza L, Manfredi R, Chiodo F (2003) Stenotrophomonas (Xanthomonas) maltophilia as an emerging opportunistic pathogen in association with HIV infection: a 10-year surveillance study. Infection 31:155–161
Villarino ME, Stevens LE, Schable B et al (1992) Risk factors for epidemic Xanthomonas maltophilia infection/colonization in intensive care unit patients. Infect Control Hosp Epidemiol 13:201–206
Denton M, Kerr KG (1998) Microbiological and clinical aspects of infection associated with Stenotrophomonas maltophilia. Clin Microbiol Rev 11:57–80
Morrison Jr AJ, Hoffmann KK, Wenzel RP (1986) Associated mortality and clinical characteristics of nosocomial Pseudomonas maltophilia in a university hospital. J Clin Microbiol 24:52–55
Sanyal SC, Mokaddas EM (1999) The increase in carbapenem use and emergence of Stenotrophomonas maltophilia as an important nosocomial pathogen. J Chemother 11:28–33
Elting LS, Khardori N, Bodey GP et al (1990) Nosocomial infection caused by Xanthomonas maltophilia: a case-control study of predisposing factors. Infect Control Hosp Epidemiol 11:134–138
Gastmeier P, Geffers C, Sohr D et al (2003) Five years working with the German nosocomial infection surveillance system (Krankenhaus Infektions Surveillance System). Am J Infect Control 31:316–321
Meyer E, Jonas D, Schwab F et al (2003) Design of a surveillance system of antibiotic use and bacterial resistance in German intensive care units (SARI). Infection 31:208–215
Gulmez D, Hascelik G (2005) Stenotrophomonas maltophilia: antimicrobial resistance and molecular ty** of an emerging pathogen in a Turkish university hospital. Clin Microbiol Infect 11:880–886
Jones RN, Sader HS, Beach ML (2003) Contemporary in vitro spectrum of activity summary for antimicrobial agents tested against 18,569 strains of non-fermentative gram-negative bacilli isolated in the SENTRY Antimicrobial Surveillance Program (1997–2001). Int J Antimicrob Agents 22:551–556
Krcmery V Jr, Sykora P, Trupl J et al (2001) Antibiotic use and development of resistance in blood culture isolates: 8 years of experience from a cancer referral center. J Chemother 13:133–142
Acknowledgements
Declaration of competing interests: SARI is part of the SIR (Spread of Nosocomial Infections and Resistant Pathogens) research network supported by the Federal Ministry of Education and Research. This study was supported by a grant from the Federal Ministry of Education and Research (01Kl 9907).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Meyer, E., Schwab, F., Gastmeier, P. et al. Is the prevalence of Stenotrophomonas maltophilia isolation and nosocomial infection increasing in intensive care units?. Eur J Clin Microbiol Infect Dis 25, 711–714 (2006). https://doi.org/10.1007/s10096-006-0198-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-006-0198-8