Abstract
Background
As part of a large prospective randomized Austrian multicenter trial evaluating recurrence rates and complications of open and laparoscopic unilateral inguinal hernia repairs we assessed postoperative pain and quality of life.
Methods
Approximately 151 patients were randomized to Shouldice repair, Bassini operation, or laparoscopic transabdominal preperitoneal hernioplasty (TAPP). Pain was recorded preoperatively and on the first four postoperative days. Quality of life was recorded preoperatively and 1 month postoperatively.
Results
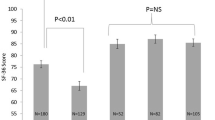
Patients having Shouldice repairs had significantly higher visual analog-scale scores for pain on the fourth postoperative day (P=0.048) and significantly higher scores in McGill pain questionnaires on the first four postoperative days (P=0.046) compared with the other groups. Apart from a significantly lower score in postoperative bodily pain in the Shouldice group (P=0.039), no significant differences in quality of life were apparent among the three methods.
Conclusions
The TAPP and Bassini repairs result in less short-term postoperative pain.







Similar content being viewed by others
References
Dierking GW, Ostergaard E, Ostergaard HT, Dahl JB (1992) Effect of pre- versus postoperative inguinal field block on postoperative pain after herniorrhaphy. Br J Anaesth 68:344–348
Dueholm S, Forrest M, Hjortso E, Lemvigh E (1989) Pain relief following herniotomy: a double-blind randomized comparison between naproxen and placebo. Acta Anaesthesiol Scand 33:391–394
Sinclair R, Cassuto J, Hogstrom S, Linden I, Faxen A, Hedner T, Ekman R (1988) Topical anesthesia with lidocaine aerosol in the control of postoperative pain. Anesthesiology 68:895–901
Fitzgibbons RJ, Camps J, Cornet DA, Nguyen NX, Litke BS, Annibali R, Salerno GM (1995) Laparoscopic inguinal herniorrhaphy: results of a multicenter trial. Ann Surg 221:3–13
Kozol R, Lange PM, Kosir M, Beleski K, Mason K, Tennenberg S, Kubinec SM, Wilson RF (1997) A prospective randomized study of open versus laparoscopic inguinal hernia repair. An assessment of postoperative pain. Arch Surg 132:292–295
Liem MSL, van der Graaf Y, van Steensel CJ, Boelhouwer RU, Clevers GJ, Meijer WS, Stassen LP, Vente JP, Weidema WF, Schrijvers AJ, van Vroonhoven TJ (1997) Comparison of conventional anterior surgery and laparoscopic surgery for inguinal hernia repair. N Engl J Med 336:1541–1547
The MRC Laparoscopic Groin Hernia Trial Group (1999) Laparoscopic versus open repair of groin hernia: a randomised comparison. Lancet 354:185–190
Stoker DL, Spiegelhalter DJ, Singh R, Wellwood JM (1994) Laparoscopic versus open inguinal hernia repair: randomised prospective trial. Lancet 343:1243–1245
Huskisson EC (1974) Measurement of pain. Lancet 9:1127–1131
Melzack R (1987) The short-form McGill Pain Questionnaire. Pain 30:191–197
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). Conceptual framework and item selection. Med Care 30:473–483
Moher D, Jones A, Lepage L, for the consort Group (2001) Use of the consort statement and quality of reports of randomized trials: a comparative before and after evaluation? JAMA 285:1992–1995
Berndsen F, Arvidsson D, Enander LK, Leijonmarck CE, Wingren U, Rudberg C, Smedberg S, Wickbom G, Montgomery A (2002) Postoperative convalescence after inguinal hernia surgery: prospective randomized multicenter study of laparoscopic versus shouldice inguinal hernia repair in 1042 patients. Hernia 6:56–61
Leibl B, Daubler P, Schwarz J, Ulrich M, Bittner R (1995) Standardized laparoscopic hernia repair (TAPP) versus Shouldice repair. Results of a randomized trial. Chirurgie 66:895–898
Tschudi J, Wagner M, Klaiber C, Brugger J-J, Frei E, Krahenbuhl L, Inderbitzi R, Husler J, Schmitz SH (1996) Controlled multicenter trial of laparoscopic transabdominal preperitoneal hernioplasty vs Shouldice herniorrhaphy. Surg Endosc 10:845–847
Junge K, Peiper C, Rosch R, Lynen P, Schumpelick V (2002) Effect of tension induced by Shouldice repair on postoperative course and long-term outcome. Eur J Surg 168:329–33
Peiper C, Junge K, Futing A, Bassalay P, Conze J, Schumpelick V (2001) Inguinal tensile strength and pain level after Shouldice repair. Hernia 5:129–134
Barkun JS, Wexler MJ, Hinchey EJ, Thibeault D, Meakins JL (1995) Laparoscopic versus open inguinal herniorrhaphy: preliminary results of a randomized controlled trial. Surgery 118:703–709
Lawrence K, McWhinnie D, Goodwin A, Doll H, Gordon A, Gray A, Britton J, Collin J (1995) Randomised controlled trial of laparoscopic versus open repair of inguinal hernia: Early results. BMJ 311:981–985
Liem MS, Halsema JA, van der Graaf Y, Schrijvers AJ, van Vroonhoven TJ (1997) Cost-effectiveness of extraperitoneal laparoscopic inguinal hernia repair: a randomized comparison with conventional herniorrhaphy. Coala trial group. Ann Surg 226:668–675
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pokorny, H., Klingler, A., Scheyer, M. et al. Postoperative pain and quality of life after laparoscopic and open inguinal hernia repair: results of a prospective randomized trial. Hernia 10, 331–337 (2006). https://doi.org/10.1007/s10029-006-0105-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-006-0105-3