Abstract
Background
Bladder cancer (BCa) is among the most prevalent malignant tumors affecting the urinary system. Due to its highly recurrent nature, standard treatments such as surgery often fail to significantly improve patient prognosis. Our research aims to predict prognosis and identify precise therapeutic targets for novel treatment interventions.
Methods
We collected and screened genes related to the TGF-β signaling pathway and performed unsupervised clustering analysis on TCGA-BLCA samples based on these genes. Our analysis revealed two novel subtypes of bladder cancer with completely different biological characteristics, including immune microenvironment, drug sensitivity, and more. Using machine learning classifiers, we identified SMAD6 as a hub gene contributing to these differences and further investigated the role of SMAD6 in bladder cancer in the single-cell transcriptome data. Additionally, we analyzed the relationship between SMAD6 and immune checkpoint genes. Finally, we performed a series of in vitro assays to verify the function of SMAD6 in bladder cancer cell lines.
Results
We have revealed two novel subtypes of bladder cancer, among which C1 exhibits a worse prognosis, lower drug sensitivity, a more complex tumor microenvironment, and a ‘colder’ immune microenvironment compared to C2. We identified SMAD6 as a key gene responsible for the differences and further explored its impact on the molecular characteristics of bladder cancer. Through in vitro experiments, we found that SMAD6 promoted the prognosis of BCa patients by inhibiting the proliferation and migration of BCa cells.
Conclusion
Our study reveals two novel subtypes of BCa and identifies SMAD6 as a highly promising therapeutic target.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
BCa ranks as the second most common malignant tumor in the urinary system. As of 2020, it annually accounts for approximately 570,000 new cases and 210,000 deaths worldwide (Sung et al. 2021). With the rise in tobacco consumption and smoking rates, the incidence of BCa is also increasing (Lenis et al. 2020). Classified by stage, BCa can be categorized into non-muscle-invasive bladder cancer (NMIBC) and muscle-invasive bladder cancer (MIBC) (Witjes et al. 2021). Among patients diagnosed with non-muscle-invasive bladder cancer, one-third to three-quarters experience recurrence within five years after surgery, and about 15% progress to MIBC (Bajorin et al. 2021). Surgery and chemotherapy are traditional means of managing BCa. However, due to its recurrent and progressive nature, the prognosis and survival rates are generally poor (Balar et al. 2021). With the emergence of targeted therapy and immunotherapy, identifying reliable treatment targets is essential for a comprehensive improvement in BCa management (de Jong et al. 2021). On the other hand, a deep exploration of the biological mechanisms underlying the occurrence and development of BCa is crucial for develo** new treatment approaches and extending the survival time of advanced-stage patients.
The TGF-β signaling pathway is a complex and highly conserved signaling pathway within living organisms (Derynck et al. 2021). It has been demonstrated to be associated with several hallmarks of cancer, such as evasion of immune surveillance, resistance to cell death, and activation of invasion and metastasis (Massagué, 2008). The TGF-β signaling pathway has a broad impact, with increased TGF-β expression observed in almost all solid tumor cells. The TGF-β latent complex binds to TGF-β receptors on the cell membrane, leading to phosphorylation and activation of SMAD2 and SMAD3 (Derynck and Budi 2019). Subsequently, these SMADs are transported into the cell nucleus, where they bind to transcription factors, activating or inhibiting the transcription of target genes (Syed 2016). Additionally, the TGF-β signaling pathway is closely related to pathways associated with cancer progression, such as Myc, Notch, Wnt, and PI3K/AKT, among others (Bierie and Moses 2006). In urine samples collected by some researchers, samples from BCa show higher expression of TGFβ-mRNA, TGFβ1 protein, and its receptors compared to samples from the healthy group (Lu et al. 2022). Epithelial-mesenchymal transition (EMT) refers to the process in which epithelial cells lose their original biological characteristics and acquire features of mesenchymal cells (Goulet et al. 2019). EMT promotes the invasive and migratory activity of cancer cells. Studies have found that TGF-β can promote EMT in BCa by activating transcription factors such as ZEB1/2 through the SMAD3/4 pathway, activating stromal genes, and inhibiting epithelial genes (Hao et al. 2019). Researchers have also found that the TGF-β signaling pathway is significantly upregulated in MIBC compared to NMIBC, further indicating its association with BCa progression (Katoh and Nakagama 2014). The TGF-β signaling pathway can also influence tumor progression and treatment by regulating the tumor microenvironment (Najafi et al. 2019). TGF-β has been demonstrated to exert an immunosuppressive role within the microenvironment, inhibiting the production of the cytokine IFNγ, which promotes the proliferation of CD8 + T cells (Yang et al. 2010). Furthermore, TGF-β can inhibit dendritic cell immune surveillance and antigen presentation (Tauriello et al. 2022). These characteristics suggest that the TGF-β signaling pathway may impact immune checkpoint inhibitor (ICI) therapy.
This study utilized consensus clustering in the TCGA-BLCA cohort to identify two TGF-β related subtypes with distinct clinical and molecular characteristics. Subsequently, machine learning classifiers were employed to identify the gene SMAD6 as a causative factor for these differences. Integrating single-cell and pan-cancer transcriptome data, we analyzed the potential role of SMAD6 in various cancers, including BCa, revealing that lower expression of SMAD6 in BCa is associated with a worse prognosis. Finally, these findings were validated in in vitro experiments. Our research offers novel insights into the influence of the TGF-β signaling pathway on BCa and identifies SMAD6 as a potential therapeutic biomarker.
Materials and methods
Data collection and preprocessing
Various BCa datasets were involved in this study, TCGA-BLCA (n = 406) was achieved from UCSC Xena (https://xenabrowser.net/). GSE32894 and corresponding clinical data were retrieved from the Gene Expression Omnibus (GEO) (https://www.ncbi.nlm.nih.gov/geo/). All raw mRNA sequencing data were filtered and normalized before analysis. The single-cell RNA sequencing data was downloaded from SRP280327 in the Sequence Read Archive (https://www.ncbi.nlm.nih.gov/sra), which contained 8 bladder carcinoma tumor samples and 3 normal tissues (Chen et al. 2023). The activated TGF-β signaling pathway in CAFs can also inhibit cell death and play a role in cancer progression (Yoshida 2020).
Bladder cancer molecular subtypes and biological characteristics vary among different subgroups. This study elucidates that the EMT activity is more pronounced in C1, indicating a propensity for progression and metastasis in tumors of C1. Additionally, the tumor microenvironment of C1 exhibits more severe hypoxia, which has been previously associated with tumor progression and drug resistance. We also found that angiogenesis is more active in C1, which is correlated with tumor cell vitality due to its role in nutrient and oxygen supply to tumors (Li et al. 2019). Furthermore, we observed upregulation of the TNFα-NFκB and Kras signaling pathways in the C1 subtype, which have been implicated in the progression and drug resistance of various cancers (Girouard et al. 2020; Timar and Kashofer 2020; Kim et al. 2023). Some research has found that the androgen receptor (AR)-mediated ADAR2/FNTA pathway alters the invasion of BCa cells and their sensitivity to cisplatin by activating the Kras signaling pathway (Chen et al. 2020a). The metabolic landscape of bladder cancer reveals distinct metabolic characteristics between C1 and C2. Methionine metabolism is involved in numerous cellular functions, including redox reactions, folate metabolism, and methylation processes, all of which are implicated in the pathogenesis of cancer (Sanderson et al. 2019). Research has shown that the accumulation of methionine metabolism products may lead to hypermethylation of tumor suppressor genes, thereby increasing the risk of bladder cancer progression (Wojtczyk-Miaskowska and Schlichtholz 2019; Li et al. 2023a). Animal experiments have demonstrated the therapeutic effects of methionine-restricted diets in chemotherapy-resistant colorectal cancer xenograft models (Gao et al. 2019). Additionally, studies have found that methionine-restricted diets can effectively inhibit platinum resistance in bladder cancer patients, thereby enhancing the efficacy of chemotherapy (Yang et al. 2023). The relationship between methionine metabolism and the TGFβ signaling pathway warrants further investigation. At the biochemical level, glutathione metabolism is closely linked to cellular hypoxia, and the higher levels of glutathione metabolism in C1 compared to C2 are consistent with previous findings. Glutathione is one of the most important antioxidants in mammalian cells, protecting cells from damage by reactive oxygen species and lipid peroxidation. The antioxidant system regulated by glutathione is crucial in maintaining the homeostasis of cancer cells (Kennedy et al. 2020). A series of studies have demonstrated the association of glutathione with cancer cell proliferation, differentiation, metastasis, and treatment response. Glutathione metabolism is involved in the metabolic reprogramming of cancer cells during cancer progression. In this process, cancer cells can enhance their tolerance to adverse microenvironments(Estrela et al. 2006). Research has found that glutathione metabolism is associated with a form of regulated cell death induced by excessive lipid peroxidation, known as ferroptosis (Li et al. 2024). Glutathione can promote tumor growth by inhibiting ferroptosis.
Given the differences between the C1 and C2 subtypes of BCa mentioned above, identifying key genes that contribute to these differences may lead us to identify a novel biomarker for BCa. Machine learning classifiers can identify the key factors causing differences based on input expression matrices, with high precision and sensitivity. Combining the results of classification from five machine learning algorithms with survival analysis, we ultimately determined that SMAD6 can serve as a prognostic biomarker for bladder cancer. The SMAD family, as downstream signaling receptors of the TGF-β family, consists of eight members. SMAD6 is a key negative regulator in the classical TGF-β signaling pathway, capable of inhibiting TGF-β receptor activity in the cytoplasm and acting as a transcriptional inhibitory protein in the cell nucleus (Derynck and Zhang 2003). Previous research has suggested that the TGF-β/SMAD pathway induces cell proliferation, angiogenesis, and epithelial-mesenchymal transition (Song and Zhou 2021). Additionally, studies have indicated that inhibiting SMAD signaling can reduce the expression of PD-L1 and PD-L2, implying that the TGF-β/SMAD pathway creates an immune-suppressive microenvironment (MaruYama et al. 2022). However, among the SMAD family members, it remains unclear which one is the key regulatory gene. Through machine learning screening, this study revealed that the TGF-β/SMAD signaling plays an important role in the progression of bladder cancer, with SMAD6 identified as a significant regulator. To elucidate the role of SMAD6 in bladder cancer, single-cell data analysis revealed a correlation between SMAD6 expression and clinical outcomes, predicting patients' overall survival (OS). Simultaneously, GSEA results demonstrated that biological processes such as the P53 pathway and G2M checkpoint are more active in epithelial cells with low SMAD6 expression. The role of the G2M checkpoint is to prevent cells with genomic DNA damage from entering the mitotic phase, indicating that cancer cells with low SMAD6 expression exhibit more severe DNA damage and greater genomic mutation diversity. P53, as a classical tumor-suppressive pathway, plays a crucial role in tumorigenesis when mutated or deactivated. Enrichment analysis results revealed a connection between low SMAD6 expression and p53 mutations. In summary, the overexpression of SMAD6 led to the downregulation of the TGF-β signaling pathway in bladder cancer, thereby inhibiting cancer cell EMT and reducing the progression and metastasis of bladder cancer. Additionally, SMAD6 is associated with the tumor microenvironment, where high SMAD6 expression enhances immune-mediated tumor killing effects. These factors may contribute to SMAD6’s impact on patient survival. The influence of SMAD6 on bladder cancer drug sensitivity may be regulated through alterations in bladder cancer metabolism. Based on metabolism landscape results, SMAD6 likely upregulates methionine metabolism in cancer cells by mediating the TGF-β signaling pathway, leading to cisplatin resistance in cancer cells.
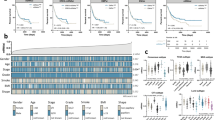
Simultaneously, we also analyzed the role of SMAD6 in various cancers. Survival analysis demonstrated that the role of SMAD6 varies in different cancers. In LUAD, STAD, and KIRC, low expression of SMAD6 implies a worse prognosis, while the opposite is observed in BRCA and COAD. The role of the TGF-β/SMAD signaling pathway has been extensively documented across various cancers (He et al. 2022). SMAD transcriptional regulatory events play complicated roles in the pathogenesis of cancers in the intestinal mucosa, pancreas, and liver (Du et al. 2021). Additionally, the TGF-β/SMAD signaling pathway participates in regulating tumor stromal cells and the immune system (Zhang et al. 2022). Literature has reported that SMAD6 acts as a downstream target of miRNA to regulate the TGF-β signaling pathway, thereby further inhibiting cancer cell proliferation (Bayat et al. 2021).
Conclusion
In summary, our study reveals two bladder cancer patient subtypes based on the TGF-β pathway. The C1 is associated with a poorer prognosis, a colder immune microenvironment, and higher drug resistance. We identified that SMAD6 plays a crucial regulatory role in the TGF-β/SMAD pathway in bladder cancer, and several biological characteristics of the C1 may be related to the deficiency of SMAD6. Our research emphasizes the importance of the TGF-β/SMAD pathway in the progression of bladder cancer and provides potential targets and strategies for the precise therapy of bladder cancer.
Data availability
The data are available from TCGA database (https://portal.gdc.cancer.gov/), the GEO database (http://www.ncbi.nlm.nih.gov/geo/, GSE32984).
References
Antoni S, Ferlay J, Soerjomataram I, Znaor A, Jemal A, Bray F (2017) Bladder cancer incidence and mortality: a global overview and recent trends. Eur Urol 71(1):96–108. https://doi.org/10.1016/j.eururo.2016.06.010
Bajorin DF, Witjes JA, Gschwend JE, Schenker M, Valderrama BP, Tomita Y et al (2021) Adjuvant nivolumab versus placebo in muscle-invasive urothelial carcinoma. N Engl J Med 384(22):2102–2114. https://doi.org/10.1056/NEJMoa2034442
Balar AV, Kamat AM, Kulkarni GS, Uchio EM, Boormans JL, Roumiguié M et al (2021) Pembrolizumab monotherapy for the treatment of high-risk non-muscle-invasive bladder cancer unresponsive to BCG (KEYNOTE-057): an open-label, single-arm, multicentre, phase 2 study. Lancet Oncol 22(7):919–930. https://doi.org/10.1016/s1470-2045(21)00147-9
Bayat Z, Ghaemi Z, Behmanesh M, Soltani BM (2021) Hsa-miR-186-5p regulates TGFβ signaling pathway through expression suppression of SMAD6 and SMAD7 genes in colorectal cancer. Biol Chem 402(4):469–480. https://doi.org/10.1515/hsz-2019-0407
Becker WR, Nevins SA, Chen DC, Chiu R, Horning AM, Guha TK et al (2022) Single-cell analyses define a continuum of cell state and composition changes in the malignant transformation of polyps to colorectal cancer. Nat Genet 54(7):985–995. https://doi.org/10.1038/s41588-022-01088-x
Benjamin DJ, Lyou Y (2021) Advances in immunotherapy and the TGF-β resistance pathway in metastatic bladder cancer. Cancers (basel). https://doi.org/10.3390/cancers13225724
Bierie B, Moses HL (2006) TGF-beta and cancer. Cytokine Growth Factor Rev 17(1–2):29–40. https://doi.org/10.1016/j.cytogfr.2005.09.006
Chen J, Sun Y, Ou Z, Yeh S, Huang CP, You B et al (2020a) Androgen receptor-regulated circFNTA activates KRAS signaling to promote bladder cancer invasion. EMBO Rep 21(4):e48467. https://doi.org/10.15252/embr.201948467
Chen Z, Zhou L, Liu L, Hou Y, **ong M, Yang Y et al (2020b) Single-cell RNA sequencing highlights the role of inflammatory cancer-associated fibroblasts in bladder urothelial carcinoma. Nat Commun 11(1):5077. https://doi.org/10.1038/s41467-020-18916-5
de Jong FC, Rutten VC, Zuiverloon TCM, Theodorescu D (2021) Improving anti-PD-1/PD-L1 therapy for localized bladder cancer. Int J Mol Sci. https://doi.org/10.3390/ijms22062800
Derynck R, Budi EH (2019) Specificity, versatility, and control of TGF-β family signaling. Sci Signal. https://doi.org/10.1126/scisignal.aav5183
Derynck R, Zhang YE (2003) Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature 425(6958):577–584. https://doi.org/10.1038/nature02006
Derynck R, Turley SJ, Akhurst RJ (2021) TGFβ biology in cancer progression and immunotherapy. Nat Rev Clin Oncol 18(1):9–34. https://doi.org/10.1038/s41571-020-0403-1
Du H, Gu J, Peng Q, Wang X, Liu L, Shu X et al (2021) Berberine suppresses EMT in liver and gastric carcinoma cells through combination with TGFβR regulating TGF-β/Smad pathway. Oxid Med Cell Longev 2021:2337818. https://doi.org/10.1155/2021/2337818
Estrela JM, Ortega A, Obrador E (2006) Glutathione in cancer biology and therapy. Crit Rev Clin Lab Sci 43(2):143–181. https://doi.org/10.1080/10408360500523878
Fang Z, Meng Q, Xu J, Wang W, Zhang B, Liu J et al (2023) Signaling pathways in cancer-associated fibroblasts: recent advances and future perspectives. Cancer Commun (lond) 43(1):3–41. https://doi.org/10.1002/cac2.12392
Fujii R, Jochems C, Tritsch SR, Wong HC, Schlom J, Hodge JW (2018) An IL-15 superagonist/IL-15Rα fusion complex protects and rescues NK cell-cytotoxic function from TGF-β1-mediated immunosuppression. Cancer Immunol Immunother 67(4):675–689. https://doi.org/10.1007/s00262-018-2121-4
Gao X, Sanderson SM, Dai Z, Reid MA, Cooper DE, Lu M et al (2019) Dietary methionine influences therapy in mouse cancer models and alters human metabolism. Nature 572(7769):397–401. https://doi.org/10.1038/s41586-019-1437-3
Girouard J, Belgorosky D, Hamelin-Morrissette J, Boulanger V, D’Orio E, Ramla D et al (2020) Molecular therapy with derivatives of amino benzoic acid inhibits tumor growth and metastasis in murine models of bladder cancer through inhibition of TNFα/NFΚB and iNOS/NO pathways. Biochem Pharmacol 176:113778. https://doi.org/10.1016/j.bcp.2019.113778
Goulet CR, Champagne A, Bernard G, Vandal D, Chabaud S, Pouliot F et al (2019) Cancer-associated fibroblasts induce epithelial-mesenchymal transition of bladder cancer cells through paracrine IL-6 signalling. BMC Cancer 19(1):137. https://doi.org/10.1186/s12885-019-5353-6
Hänzelmann S, Castelo R, Guinney J (2013) GSVA: gene set variation analysis for microarray and RNA-seq data. BMC Bioinformatics 14:7. https://doi.org/10.1186/1471-2105-14-7
Hao Y, Baker D, Ten Dijke P (2019) TGF-β-mediated epithelial-mesenchymal transition and cancer metastasis. Int J Mol Sci. https://doi.org/10.3390/ijms20112767
He R, Shi J, Xu D, Yang J, Shen Y, Jiang YS et al (2022) SULF2 enhances GDF15-SMAD axis to facilitate the initiation and progression of pancreatic cancer. Cancer Lett 538:215693. https://doi.org/10.1016/j.canlet.2022.215693
Katoh M, Nakagama H (2014) FGF receptors: cancer biology and therapeutics. Med Res Rev 34(2):280–300. https://doi.org/10.1002/med.21288
Kennedy L, Sandhu JK, Harper ME, Cuperlovic-Culf M (2020) Role of glutathione in cancer: from mechanisms to therapies. Biomolecules. https://doi.org/10.3390/biom10101429
Kim D, Herdeis L, Rudolph D, Zhao Y, Böttcher J, Vides A et al (2023) Pan-KRAS inhibitor disables oncogenic signalling and tumour growth. Nature 619(7968):160–166. https://doi.org/10.1038/s41586-023-06123-3
Lenis AT, Lec PM, Chamie K, Mshs MD (2020) Bladder cancer: a review. JAMA 324(19):1980–1991. https://doi.org/10.1001/jama.2020.17598
Li S, Xu HX, Wu CT, Wang WQ, ** W, Gao HL et al (2019) Angiogenesis in pancreatic cancer: current research status and clinical implications. Angiogenesis 22(1):15–36. https://doi.org/10.1007/s10456-018-9645-2
Li T, Tan YT, Chen YX, Zheng XJ, Wang W, Liao K et al (2023a) Methionine deficiency facilitates antitumour immunity by altering m(6)A methylation of immune checkpoint transcripts. Gut 72(3):501–511. https://doi.org/10.1136/gutjnl-2022-326928
Li Z, Qin Y, Liu X, Chen J, Tang A, Yan S et al (2023b) Identification of predictors for neurological outcome after cardiac arrest in peripheral blood mononuclear cells through integrated bioinformatics analysis and machine learning. Funct Integr Genomics 23(2):83. https://doi.org/10.1007/s10142-023-01016-0
Li W, Shen Y, Yang C, Ye F, Liang Y, Cheng Z et al (2024) Identification of a novel ferroptosis-inducing micropeptide in bladder cancer. Cancer Lett 582:216515. https://doi.org/10.1016/j.canlet.2023.216515
Lu H, Wu J, Liang L, Wang X, Cai H (2022) Identifying a novel defined pyroptosis-associated long noncoding RNA signature contributes to predicting prognosis and tumor microenvironment of bladder cancer. Front Immunol 13:803355. https://doi.org/10.3389/fimmu.2022.803355
Maeser D, Gruener RF, Huang RS (2021) oncoPredict: an R package for predicting in vivo or cancer patient drug response and biomarkers from cell line screening data. Brief Bioinform. https://doi.org/10.1093/bib/bbab260
MaruYama T, Chen W, Shibata H (2022) TGF-β and cancer immunotherapy. Biol Pharm Bull 45(2):155–161. https://doi.org/10.1248/bpb.b21-00966
Massagué J (2008) TGFbeta in cancer. Cell 134(2):215–230. https://doi.org/10.1016/j.cell.2008.07.001
Monjazeb AM, Tietze JK, Grossenbacher SK, Hsiao HH, Zamora AE, Mirsoian A et al (2014) Bystander activation and anti-tumor effects of CD8+ T cells following Interleukin-2 based immunotherapy is independent of CD4+ T cell help. PLoS ONE 9(8):e102709. https://doi.org/10.1371/journal.pone.0102709
Najafi M, Farhood B, Mortezaee K (2019) Extracellular matrix (ECM) stiffness and degradation as cancer drivers. J Cell Biochem 120(3):2782–2790. https://doi.org/10.1002/jcb.27681
Olivier M, Hollstein M, Hainaut P (2010) TP53 mutations in human cancers: origins, consequences, and clinical use. Cold Spring Harb Perspect Biol 2(1):a001008. https://doi.org/10.1101/cshperspect.a001008
Sanderson SM, Gao X, Dai Z, Locasale JW (2019) Methionine metabolism in health and cancer: a nexus of diet and precision medicine. Nat Rev Cancer 19(11):625–637. https://doi.org/10.1038/s41568-019-0187-8
Shapouri-Moghaddam A, Mohammadian S, Vazini H, Taghadosi M, Esmaeili SA, Mardani F et al (2018) Macrophage plasticity, polarization, and function in health and disease. J Cell Physiol 233(9):6425–6440. https://doi.org/10.1002/jcp.26429
Singh SV, Xu BH, Jani JP, Emerson EO, Backes MG, Rihn C et al (1995) Mechanism of cross-resistance to cisplatin in a mitomycin C-resistant human bladder cancer cell line. Int J Cancer 61(3):431–436. https://doi.org/10.1002/ijc.2910610326
Song C, Zhou C (2021) HOXA10 mediates epithelial-mesenchymal transition to promote gastric cancer metastasis partly via modulation of TGFB2/Smad/METTL3 signaling axis. J Exp Clin Cancer Res 40(1):62. https://doi.org/10.1186/s13046-021-01859-0
Sun D, Guan X, Moran AE, Wu LY, Qian DZ, Schedin P et al (2022) Identifying phenotype-associated subpopulations by integrating bulk and single-cell sequencing data. Nat Biotechnol 40(4):527–538. https://doi.org/10.1038/s41587-021-01091-3
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Syed V (2016) TGF-β Signaling in Cancer. J Cell Biochem 117(6):1279–1287. https://doi.org/10.1002/jcb.25496
Tauriello DVF, Sancho E, Batlle E (2022) Overcoming TGFβ-mediated immune evasion in cancer. Nat Rev Cancer 22(1):25–44. https://doi.org/10.1038/s41568-021-00413-6
Timar J, Kashofer K (2020) Molecular epidemiology and diagnostics of KRAS mutations in human cancer. Cancer Metastasis Rev 39(4):1029–1038. https://doi.org/10.1007/s10555-020-09915-5
Tuleta I, França CN, Wenzel D, Fleischmann B, Nickenig G, Werner N et al (2014) Hypoxia-induced endothelial dysfunction in apolipoprotein E-deficient mice; effects of infliximab and L-glutathione. Atherosclerosis 236(2):400–410. https://doi.org/10.1016/j.atherosclerosis.2014.08.021
van Dijk N, Funt SA, Blank CU, Powles T, Rosenberg JE, van der Heijden MS (2019) The cancer immunogram as a framework for personalized immunotherapy in urothelial cancer. Eur Urol 75(3):435–444. https://doi.org/10.1016/j.eururo.2018.09.022
Witjes JA, Bruins HM, Cathomas R, Compérat EM, Cowan NC, Gakis G et al (2021) European association of urology guidelines on muscle-invasive and metastatic bladder cancer: summary of the 2020 guidelines. Eur Urol 79(1):82–104. https://doi.org/10.1016/j.eururo.2020.03.055
Wojtczyk-Miaskowska A, Schlichtholz B (2019) Tobacco carcinogens and the methionine metabolism in human bladder cancer. Mutat Res Rev Mutat Res 782:108281. https://doi.org/10.1016/j.mrrev.2019.06.001
Wu F, Yang J, Liu J, Wang Y, Mu J, Zeng Q et al (2021) Signaling pathways in cancer-associated fibroblasts and targeted therapy for cancer. Signal Transduct Target Ther 6(1):218. https://doi.org/10.1038/s41392-021-00641-0
**ao Y, Ma D, Zhao S, Suo C, Shi J, Xue MZ et al (2019) Multi-omics profiling reveals distinct microenvironment characterization and suggests immune escape mechanisms of triple-negative breast cancer. Clin Cancer Res 25(16):5002–5014. https://doi.org/10.1158/1078-0432.Ccr-18-3524
Yang L, Pang Y, Moses HL (2010) TGF-beta and immune cells: an important regulatory axis in the tumor microenvironment and progression. Trends Immunol 31(6):220–227. https://doi.org/10.1016/j.it.2010.04.002
Yang C, Ou Y, Zhou Q, Liang Y, Li W, Chen Y et al (2023) Methionine orchestrates the metabolism vulnerability in cisplatin resistant bladder cancer microenvironment. Cell Death Dis 14(8):525. https://doi.org/10.1038/s41419-023-06050-1
Yoshida GJ (2020) Regulation of heterogeneous cancer-associated fibroblasts: the molecular pathology of activated signaling pathways. J Exp Clin Cancer Res 39(1):112. https://doi.org/10.1186/s13046-020-01611-0
Zeng D, Ye Z, Shen R, Yu G, Wu J, **ong Y et al (2021) IOBR: multi-omics immuno-oncology biological research to decode tumor microenvironment and signatures. Front Immunol 12:687975. https://doi.org/10.3389/fimmu.2021.687975
Zhang T, He X, Caldwell L, Goru SK, Ulloa Severino L, Tolosa MF et al (2022) NUAK1 promotes organ fibrosis via YAP and TGF-β/SMAD signaling. Sci Transl Med 14(637):eaaz4028. https://doi.org/10.1126/scitranslmed.aaz4028
Acknowledgements
We thank the public database for providing data for our research.
Funding
This work was supported by the National Natural Science Foundation of China (No.81802569, 82373222), Leading Talent Program by Shanghai Municipal Health Commission (2022LJ008), Medical Innovation Research Special Project by Science and Technology Commission of Shanghai Municipality (22Y21900200), Clinical Scientific and Technological Innovation Project by Shanghai Hospital Development Center (SHDC12021104).
Author information
Authors and Affiliations
Contributions
ZC and YO made equal contributions to this study. ZC conducted the bioinformatic analysis and wrote the manuscript. YO: contributed to methodology, writing-review, and editing. FY and WL contributed to data collection. HJ supervised and funded this study and revised the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Ethical approval
Ethical approval was not required for the studies on humans in accordance with the local legislation and institutional requirements because only commercially available established cell lines were used.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, Z., Ou, Y., Ye, F. et al. Machine learning identifies the role of SMAD6 in the prognosis and drug susceptibility in bladder cancer. J Cancer Res Clin Oncol 150, 264 (2024). https://doi.org/10.1007/s00432-024-05798-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00432-024-05798-z