Abstract
Background
Postoperative complications related to gastric conduit reconstruction are still common issues after McKeown esophagectomy. A novel endoscopic mucosal ischemic index is desired to predict anastomotic complications after McKeown esophagectomy.
Aims and methods
The purpose of this study was to prospectively evaluate the safety and efficacy of endoscopic examinations of the anastomotic region in the acute period after esophagectomy.
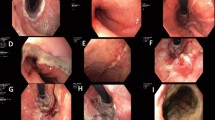
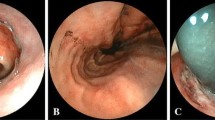
Endoscopic examinations were performed on postoperative days (PODs) 1 and 8. The severity of ischemia was prospectively validated according to the endoscopic mucosal ischemic index (EMII).
Results
A total of 58 patients were included after evaluating the safety and feasibility of the endoscopic examination on POD 1 in 10 patients. Anastomotic leakage occurred in 6 patients. Stricture occurred in 13 patients. A greater than 67% circumference and lesion length greater than 20 mm of anastomotic ischemic area (AIA) on POD 1 were associated with develo** anastomotic leakage after esophagectomy (OR: 14.5; 95% CI: 1.8–306.5; P = 0.03, OR: 19.4; 95% CI: 1.7–536.8; P = 0.03). More than 67% circumferential ischemic mucosa and ischemic mucosal lengths greater than 20 mm of AIA on POD 1 were associated with develo** anastomotic strictures after esophagectomy (OR: 6.4; 95% CI: 1.4–31.7; P = 0.02, OR: 5.9; 95% CI: 1.2–33.1; P = 0.03). Patients with either more than 67% circumferential ischemic mucosa or ischemic mucosal lengths greater than 20 mm of AIA on POD 1 were defined as EMII-positive patients. The sensitivity, specificity, and positive and negative predictive values of EMII positivity on POD 1 for leakage were 100%, 78.8%, 35.3%, and 100%, respectively. The sensitivity, specificity, and positive and negative predictive values of the EMII positivity on POD 1 for strictures were 69.2%, 82.2%, 52.9%, and 90.2%, respectively.
Conclusions
The application of an endoscopic classification system to mucosal ischemia after McKeown esophagectomy is both appropriate and satisfactory in predicting anastomotic complications.
Trial registration
Clinical Trial.gov Registry, ID: NCT02937389, Registration date: Oct 17, 2015.



Similar content being viewed by others
Data availability
Raw data were generated at Nagasaki University. Derived data supporting the findings of this study are available from the corresponding author SK on request.
Change history
16 February 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00423-023-02824-5
Abbreviations
- MIE:
-
Minimally invasive esophagectomy
- CPK:
-
Creatine phosphokinase
- CRP:
-
C-reactive protein
- POD:
-
Postoperative day
- SD:
-
Standard deviation
- IQR:
-
Interquartile range
- ROC:
-
Receiver operating characteristic
- AUC:
-
Area under the ROC curve
- OR:
-
Odds ratio
- CI:
-
Confidence interval
- inf:
-
Infinity
- OE:
-
Open esophagectomy
- WBC:
-
White blood cells
- CD:
-
Clavien‒Dindo
- ICU:
-
Intensive care unit
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
References
Blencowe NS, Strong S, McNair AG et al (2012) Reporting of short-term clinical outcomes after esophagectomy: a systematic review. Ann Surg 255:658–666
Raymond DP, Seder CW, Wright CD et al (2016) Predictors of major morbidity or mortality after resection for esophageal cancer: a society of thoracic surgeons general thoracic surgery database risk adjustment model. Ann Thorac Surg 102:207–214
Dhungel B, Diggs BS, Hunter JG et al (2010) Patient and peri-operative predictors of morbidity and mortality after esophagectomy: American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP), 2005–2008. J Gastrointest Surg 14:1492–1501
Takeuchi H, Miyata H, Ozawa S et al (2017) Comparison of short-term outcomes between open and minimally invasive esophagectomy for esophageal cancer using a nationwide database in Japan. Ann Surg Oncol 24:1821–1827
Biere SS, van Berge Henegouwen MI, Maas KW et al (2012) Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet 379:1887–1892
Kassis ES, Kosinski AS, Ross P Jr et al (2013) Predictors of anastomotic leak after esophagectomy: an analysis of the society of thoracic surgeons general thoracic database. Ann Thorac Surg 96:1919–1926
Sabra MJ, Alwatari YA, Wolfe LG et al (2020) Ivor Lewis vs Mckeown esophagectomy: analysis of operative outcomes from the ACS NSQIP database. Gen Thorac Cardiovasc Surg 68:370–379
Nishikawa K, Fujita T, Yuda M et al (2016) Early postoperative endoscopy for targeted management of patients at risks of anastomotic complications after esophagectomy. Surg 160:1294–1301
Fujiwara H, Nakajima Y, Kawada K et al (2016) Endoscopic assessment 1 day after esophagectomy for predicting cervical esophagogastric anastomosis-relating complications. Surg Endosc 30:1564–1571
Kobayashi S, Kanetaka K, Nagata Y et al (2018) Predictive factors for major postoperative complications related to gastric conduit reconstruction in thoracoscopic esophagectomy for esophageal cancer: a case control study. BMC Surg 18:15
Page RD, Asmat A, McShane J et al (2013) Routine endoscopy to detect anastomotic leakage after esophagectomy. Ann Thorac Surg 95:292–298
Schaible A, Sauer P, Hartwig W et al (2014) Radiologic versus endoscopic evaluation of the conduit after esophageal resection: a prospective, blinded, intraindividually controlled diagnostic study. Surg Endosc 28:2078–2085
Muller PC, Morell B, Vetter D et al (2021) Preemptive endoluminal vacuum therapy to reduce morbidity after minimally invasive Ivor Lewis esophagectomy: including a novel grading system for postoperative endoscopic assessment of GI-anastomoses. Ann Surg 274:751–757
Nishikawa K, Fujita T, Yuda M et al (2020) Early prediction of complex benign anastomotic stricture after esophagectomy using early postoperative endoscopic findings. Surg Endosc 34:3460–3469
Akesson O, Heyman I, Johansson J, et al (2021) Early endoscopic assessment after esophagectomy can predict anastomotic complications: a novel scoring system. Surg Endosc
Loske G, Muller J, Schulze W et al (2022) Pre-emptive active drainage of reflux (PARD) in Ivor-Lewis oesophagectomy with negative pressure and simultaneous enteral nutrition using a double-lumen open-pore film drain (dOFD). Surg Endosc 36:2208–2216
Kuwano H, Nishimura Y, Oyama T et al (2015) Guidelines for diagnosis and treatment of carcinoma of the esophagus April 2012 edited by the Japan Esophageal Society. Esophagus 12:1–30
Edge SB BD, Compton CC, Fritz AG, Greene FL, Trotti, A. , ed AJCC cancer staging manual, 7th ed: Springer; 2010.
Li H, Yang S, Zhang Y et al (2012) Thoracic recurrent laryngeal lymph node metastases predict cervical node metastases and benefit from three-field dissection in selected patients with thoracic esophageal squamous cell carcinoma. J Surg Oncol 105:548–552
Herman J, Chavalitdhamrong D, Jensen DM et al (2011) The significance of gastric and duodenal histological ischemia reported on endoscopic biopsy. Endoscopy 43:365–368
Le Naoures P, Hamy A, Lerolle N et al (2017) Risk factors for symptomatic esophageal stricture after caustic ingestion-a retrospective cohort study. Dis Esophagus 30:1–6
Yano T, Yoda Y, Satake H et al (2013) Radial incision and cutting method for refractory stricture after nonsurgical treatment of esophageal cancer. Endosc 45:316–319
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiol 143:29–36
Lasko TA, Bhagwat JG, Zou KH et al (2005) The use of receiver operating characteristic curves in biomedical informatics. J Biomed Inform 38:404–415
van Heijl M, Gooszen JA, Fockens P et al (2010) Risk factors for development of benign cervical strictures after esophagectomy. Ann Surg 251:1064–1069
Mendelson AH, Small AJ, Agarwalla A et al (2015) Esophageal anastomotic strictures: outcomes of endoscopic dilation, risk of recurrence and refractory stenosis, and effect of foreign body removal. Clin Gastroenterol Hepatol 13(263–71):e1
Ikeda Y, Niimi M, Kan S et al (2001) Clinical significance of tissue blood flow during esophagectomy by laser Doppler flowmetry. J Thorac Cardiovasc Surg 122:1101–1106
Servais EL, Rizk NP, Oliveira L et al (2011) Real-time intraoperative detection of tissue hypoxia in gastrointestinal surgery by wireless pulse oximetry. Surg Endosc 25:1383–1389
Nishikawa K, Fujita T, Yuda M et al (2020) Quantitative assessment of blood flow in the gastric conduit with thermal imaging for esophageal reconstruction. Ann Surg 271:1087–1094
Zehetner J, DeMeester SR, Alicuben ET et al (2015) Intraoperative assessment of perfusion of the gastric graft and correlation with anastomotic leaks after esophagectomy. Ann Surg 262:74–78
Noma K, Shirakawa Y, Kanaya N et al (2018) Visualized evaluation of blood flow to the gastric conduit and complications in esophageal reconstruction. J Am Coll Surg 226:241–251
Acknowledgements
The authors thank Shuntaro Sato, who helped with the statistical analysis.
Funding
Funding was received for writing the manuscript. This study was supported by Grant-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (17K16569 Shinichiro Kobayashi, and 21K16400 Shinichiro Kobayashi) and Takeda Science Foundation.
Author information
Authors and Affiliations
Contributions
S.K. designed the study, analyzed the data, and wrote the initial draft of the manuscript. Kengo Kanetaka, Kazuma Kobayashi, and Naoyuki Yamaguchi contributed substantially to the interpretation of data and supervised patient treatment. A.Y., Y.N., S.Y., Y.M., and H.M. substantially participated in the discussion and assisted in the preparation of the manuscript. S.E. supervised the patient treatment and assisted substantially in editing the manuscript. All other authors contributed to the data collection and interpretation and critically reviewed the manuscript. All authors have approved the final version of the manuscript and agree to be accountable for all aspects of the work and ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Ethics Committee of Nagasaki University Hospital (16082215). The data of this study were prospectively analyzed. Written informed consent was obtained from the patients before esophagectomy.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kobayashi, S., Kanetaka, K., Yoneda, A. et al. Endoscopic mucosal ischemic index for predicting anastomotic complications after esophagectomy: a prospective cohort study. Langenbecks Arch Surg 408, 37 (2023). https://doi.org/10.1007/s00423-023-02783-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-02783-x