Abstract
Aim of the study
Anal canal duplications (ACDs) are extremely rare with only approximately 90 cases described in the literature. We report on three additional patients.
Methods
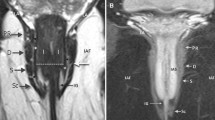
Cases were analyzed to evaluate presenting symptoms, physical exam and MRI findings. A comprehensive literature review was performed to compare our patients to previously described cases. IRB approval was obtained for this study (19-0394).
Main results
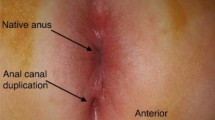
The first female patient presented with an asymptomatic ACD at 2 years old. The second patient was a 13-year-old female with perianal drainage that was initially mistaken for a fistula-in-ano and ultimately found to have an ACD associated with a dermoid cyst. Both posterior midline duplications shared a common wall with the rectum, but did not communicate with it. The ACDs and dermoid cyst were successfully excised through a posterior sagittal approach with no postoperative complications. Histology demonstrated the presence of both squamous epithelium and transitional anal epithelium in each case. The third patient was 8 months old and had a tethered cord, hemisacrum, presacral mass, and anal duplication that was initially undiagnosed. These results corroborate patterns identified in other reports of ACDs with over 90% being female and in the posterior midline. The majority are asymptomatic, but may present with symptoms of local or even systemic infection.
Conclusion
An opening in the midline posterior to the anus should raise clinical suspicion for anal canal duplication. An associated presacral mass must be ruled out. Complete excision through a posterior sagittal approach is recommended upon diagnosis to avoid symptomatic presentations. The key part of the operation is the separation of the ACD from the posterior rectal wall.




Similar content being viewed by others
References
Honda S, Minato M, Miyagi H, Okada H, Taketomi A (2017) Anal canal duplication presenting with abscess formation. Pediatr Int 59(4):500–501
Koga H, Okazaki T, Kato Y, Lane GJ, Yamataka A (2010) Anal canal duplication: experience at a single institution and literature review. Pediatr Surg Int 26(10):985–988
Sinnya S, Curtis K, Walsh M, Wong D, Kimble R (2013) Late presentation of anal canal duplication in an adolescent female—a rare diagnosis. Int J Colorectal Dis 28(8):1175–1176
Carpentier H, Maizlin I, Bliss D (2009) Anal canal duplication: case reviews and summary of the world literature. Pediatr Surg Int 25(10):911–916
La Quaglia MP, Feins N, Eraklis A, Hendren WH (1990) Rectal duplications. J Pediatr Surg 25(9):980–984
Tagart RE (1977) Congenital anal duplication: a cause of para-anal sinus. Br J Surg 64(7):525–528
Hata YSK (1978) Duplication of the rectum and/or anal canal. Jpn J Pediatr Surg 14:105–109
Palazon P, Julia V, Saura L et al (2017) Anal canal duplication and triplication: a rare entity with different presentations. Pediatr Surg Int 33(5):609–617
Dukes CE, Galvin C (1956) Colloid carcinoma arising within fistulae in the anorectal region. Ann R Coll Surg Engl 18(4):246–261
Aaronson I (1970) Anterior sacral meningocele, anal canal duplication cyst and covered anus occurring in one family. J Pediatr Surg 5(5):559–563
Pampal A, Ozbayoglu A, Kaya C et al (2013) Rectal duplications accompanying rectovestibular fistula: report of two cases. Pediatr Int 55(4):e86–89
Van Biervliet S, Maris E, Vande Velde S et al (2013) Anal canal duplication in an 11-year-old-child. Case Rep Gastrointest Med 2013:503691
Mirzaei R, Mahjubi B, Alvandipoor M, Karami MY (2015) Late presentation of anal canal duplication in adults: a series of four rare cases. Ann Coloproctol 31(1):34–36
Kratz JR, Deshpande V, Ryan DP, Goldstein AM (2008) Anal canal duplication associated with presacral cyst. J Pediatr Surg 43(9):1749–1752
Tiryaki T, Senel E, Atayurt H (2006) Anal canal duplication in children: a new technique. Pediatr Surg Int 22(6):560–561
Choi SO, Park WH (2003) Anal canal duplication in infants. J Pediatr Surg 38(5):758–762
Ochiai K, Umeda T, Murahashi O, Sugitoh T (2002) Anal-canal duplication in a 6-year-old child. Pediatr Surg Int 18(2–3):195–197
Lisi G, Illiceto MT, Rossi C, Broto JM, Jil-Vernet JM, Lelli Chiesa P (2006) Anal canal duplication: a retrospective analysis of 12 cases from two European pediatric surgical departments. Pediatr Surg Int 22(12):967–973
Ponson AE, Festen C (2001) Postanal sinus: single or different etiologies? Pediatr Surg Int 17(1):45–47
Jacquier C, Dobremez E, Piolat C, Dyon JF, Nugues F (2001) Anal canal duplication in infants and children: a series of 6 cases. Eur J Pediatr Surg 11(3):186–191
Hamada Y, Sato M, Hioki K (1996) Anal canal duplication in childhood. Pediatr Surg Int 11(8):577–579
Arai T, Miyano T, Tanno M, Kohno S, Hamasaki Y (1990) Tubular anal duplication: experiences with two cases. Z Kinderchir 45(5):311–313
Lippert SJ, Hartin CW Jr, Ozgediz DE (2012) Communicating anal canal duplication cyst in an adolescent girl. Colorectal Dis 14(5):e270–271
Vietan D, Patel RV, Huddart SN (2009) Duplicated proctodeum. Pediatr Surg Int 25(6):535–536
Cheng LS, Courtier J, MacKenzie TC (2013) Anal duplication in a one-year-old girl. J Pediatr Surg Case Rep 1(10):373–374
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Trecartin, A.C., Peña, A., Lovell, M. et al. Anal duplication: is surgery indicated? A report of three cases and review of the literature. Pediatr Surg Int 35, 971–978 (2019). https://doi.org/10.1007/s00383-019-04509-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-019-04509-x