Abstract
Purpose
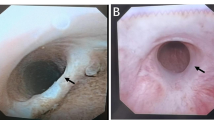
Excessive vesicourethral anastomotic leak (EVAL) is a rare but severe complication after radical prostatectomy (RP). Epithelialized vesicourethral cavity formation (EVCF) usually develops during prolonged catheterization. To our knowledge, there is no description of postoperative outcomes, complications, or functional assessment of these patients who received conservative therapy after EVAL.
Methods
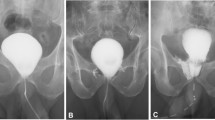
We identified 70 patients (0.56%) with radiographic evidence of EVCF out of 12,434 patients who received RP in 2016–2020 at our tertiary care center. Postoperative radiographic cystograms (CG) were retrospectively re-examined by two urologists individually. We assessed urinary continence (UC), the need for intervention due to anastomotic stricture formation, urinary tract infection (UTI), and symphysitis during the first year of follow-up post-RP.
Results
The median age was 66 years [interquartile range (IQR) 61–70 years], the median body mass index was 27.8 kg/m2 (IQR 25.5–30.3 kg/m2), and the median prostate specific antigen before RP was 7.1 ng/ml (IQR 4.7–11.8 ng/ml). The median catheter insertion time was 44.5 days (IQR 35.2–54 days). One-year continence follow-up was available for 27 patients (38.6%), of which 22 (81.5%) reported the use of ≤ one pad, two patients reported the use of two (7.4%) pads/24 h, and three (11.1%) patients reported use > two pads/24 h. Overall, four (5.7%) patients needed surgical reintervention for anastomotic stricture, eight (11.5%) patients presented with symphysitis, and 55 (77.1%) presented with UTI.
Conclusion
UC in 81.5% 1-year post-RP suggests that conservative treatment in EVAL is a treatment option with an acceptable outcome on UC and should be considered before reintervention for anastomotic insufficiency.


Similar content being viewed by others
Data availability
Data assessment was performed using our prospective institutional database (FileMaker Pro 10; FileMaker, Inc.).
References
D’Amico AV, Whittington R, Malkowicz SB, Schultz D, Blank K, Broderick GA et al (1998) Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 280(11):969–974
Hwang TJ, Gyawali B (2019) Association between progression-free survival and patients’ quality of life in cancer clinical trials. Int J Cancer 144(7):1746–1751
Pompe RS, Tian Z, Preisser F, Tennstedt P, Beyer B, Michl U et al (2017) Short- and long-term functional outcomes and quality of life after radical prostatectomy: patient-reported outcomes from a tertiary high-volume center. Eur Urol Focus 3(6):615–620
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Tilki D, Preisser F, Karakiewicz P, Shariat SF, Graefen M, Huland H et al (2018) The impact of time to catheter removal on short-, intermediate- and long-term urinary continence after radical prostatectomy. World J Urol 36(8):1247–1253
Castillo OA, Alston C, Sanchez-Salas R (2009) Persistent vesicourethral anastomotic leak after laparoscopic radical prostatectomy: laparoscopic solution. Urology 73(1):124–126
Lim JH, You D, Jeong IG, Park HK, Ahn H, Kim CS (2013) Cystoscopic injection of N-butyl-2-cyanoacrylate followed by fibrin glue for the treatment of persistent or massive vesicourethral anastomotic urine leak after radical prostatectomy. Int J Urol 20(10):980–985
Budäus L, Isbarn H, Schlomm T, Heinzer H, Haese A, Steuber T et al (2009) Current technique of open intrafascial nerve-sparing retropubic prostatectomy. Eur Urol 56(2):317–324
Beyer B, Huland H, Feick G, Graefen M (2015) “Expanded prostate cancer index composite” (EPIC-26): results of functional treatment in patients with localized prostate cancer. Urol A 54(11):1591–1595
Pompe RS, Beyer B, Haese A, Preisser F, Michl U, Steuber T et al (2018) Postoperative complications of contemporary open and robot-assisted laparoscopic radical prostatectomy using standardised reporting systems. BJU Int 122(5):801–807
Haese A, Knipper S, Isbarn H, Heinzer H, Tilki D, Salomon G et al (2019) A comparative study of robot-assisted and open radical prostatectomy in 10 790 men treated by highly trained surgeons for both procedures. BJU Int 123(6):1031–1040
Lardas M, Liew M, van den Bergh RC, De Santis M, Bellmunt J, Van den Broeck T et al (2017) Quality of life outcomes after primary treatment for clinically localised prostate cancer: a systematic review. Eur Urol 72(6):869–885
Shrestha A, Martin C, Burton M, Walters S, Collins K, Wyld L (2019) Quality of life versus length of life considerations in cancer patients: a systematic literature review. Psychooncology 28(7):1367–1380
Ziesel C, Frees S, Thomas C, Stein R, Gillitzer R, Thüroff JW (2016) Pubic symphysitis after transurethral resection of the prostate. World J Urol 34(2):275–280
Acknowledgements
There was no external financial support for this study.
Author information
Authors and Affiliations
Contributions
DKF: protocol/project development, data collection or management, data analysis, manuscript writing/editing. MG: protocol/project development, manuscript writing/editing. MF: manuscript writing/editing. TS: manuscript writing/editing. HH: manuscript writing/editing. RJS: data collection or management, data analysis, manuscript writing/editing. MK: data collection or management, manuscript writing/editing. PT: data collection or management, data analysis. LH: data collection or management, manuscript writing/editing. TL: data collection or management, data analysis, manuscript writing/editing. PM: manuscript writing/editing. JLH: manuscript writing/editing. RMP: protocol/project development, data collection or management, data analysis, manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest. In accordance with federal and institutional guidelines, all men signed an institutional review board-approved, protocol-specific informed consent form before study entry. The study was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. Anonymized data were used.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Filipas, D.K., Graefen, M., Fisch, M. et al. Outcome of patients with epithelialized cavity formation after excessive vesicourethral anastomotic leak post radical prostatectomy. World J Urol 41, 2327–2333 (2023). https://doi.org/10.1007/s00345-023-04479-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04479-9