Abstract
Rationale and Objective
Percutaneous thermal ablative technique is a common radiological procedure for malignant lesions treatment. Controlled assisted ventilation during general anesthesia is the usual mode of ventilation, but high-frequency jet ventilation (HFJV) can be a helpful alternative for the operator. The objective was to evaluate the safety of HFJV during thermal ablation procedures.
Materials and Methods
This monocentric prospective analysis included adult patients undergoing percutaneous thermal ablation procedures for abdominal tumor performed under HFJV. Procedures with a transpulmonary path were excluded. The primary outcome was the incidence of respiratory complications. Secondary outcomes included gas exchange modifications (hypercapnia, hypoxemia, pulmonary atelectasis) and the incidence of barotrauma.
Results
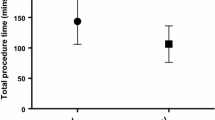
Sixty patients were included during the study period. The mean duration time was 88 min. All procedures went according to the protocol and there was no respiratory complication. There was no barotrauma event. Three patients had an exhaled capnia above 45 mmHg at the end of the procedure which normalized within 10 min of conventional ventilation.
Conclusion
HFJV during thermal ablation procedures is safe regarding gas exchange and barotrauma. This technique could be an interesting alternative to conventional ventilation during image-guided thermal ablation procedures.
Clinical Trials database
This study was registered in Clinical Trials database (NCT04209608).

Similar content being viewed by others
References
Cutress ML, Ratan HL, Williams ST, O’Brien MF. Update on the management of T1 renal cortical tumours. BJU Int. 2010;106:1130–6.
Guenette JP, Dupuy DE. Radiofrequency ablation of colorectal hepatic metastases. J Surg Oncol. 2010;102:978–87.
Rempp H, Boss A, Helmberger T, Pereira P. The current role of minimally invasive therapies in the management of liver tumors. Abdom Imag. 2011;36:635–47.
Sonntag PD, Hinshaw JL, Lubner MG, Brace CL, Lee FT Jr. Thermal ablation of lung tumors. Surg Oncol Clin N Am. 2011;20:369–87.
Wong SL, Mangu PB, Choti MA, Crocenzi TS, Dodd GD 3rd, Dorfman GS, et al. American society of clinical oncology 2009 clinical evidence review on radiofrequency ablation of hepatic metastases from colorectal cancer. J Clin Oncol. 2010;28:493–508.
Bourgain JL, Chollet M, Fischler M, Gueret G, Mayne A. Guide for the use of jet-ventilation during ENT and oral surgery. Ann Fr Anesth Reanim. 2010;29:720–7.
Ehlers M, Pezzano C, Leduc L, Brooks J, Silva P, Oechsner H, et al. Use of jet ventilation in thoracoscopic tracheo-esophageal fistula repair-Can both surgeons and anesthesiologists be happy? Paediatr Anaesth. 2015;25:860–2.
Fritz P, Kraus HJ, Mühlnickel W, Sassmann V, Hering W, Strauch K. High-frequency jet ventilation for complete target immobilization and reduction of planning target volume in stereotactic high single-dose irradiation of stage I non-small cell lung cancer and lung metastases. Int J Radiat Oncol Biol Phys. 2010;78:136–42.
Abderhalden S, Biro P, Hechelhammer L, Pfiffner R, Pfammatter T. CT-guided navigation of percutaneous hepatic and renal radiofrequency ablation under high-frequency jet ventilation: feasibility study. J Vasc Interv Radiol. 2011;22:1275–8.
Engstrand J, Toporek G, Harbut P, Jonas E, Nilsson H, Freedman J. Stereotactic CT-guided percutaneous microwave ablation of liver tumors with the use of high-frequency jet ventilation: an accuracy and procedural safety study. AJR Am J Roentgenol. 2017;208:193–200.
Denys A, Lachenal Y, Duran R, Chollet-Rivier M, Bize P. Use of high-frequency jet ventilation for percutaneous tumor ablation. Cardiovasc Intervent Radiol. 2014;37:140–6.
Chung DY, Tse DM, Boardman P, Gleeson FV, Little MW, Scott SH, et al. High-frequency jet ventilation under general anesthesia facilitates CT-guided lung tumor thermal ablation compared with normal respiration under conscious analgesic sedation. J Vasc Interv Radiol. 2014;25:1463–9.
Goode JS Jr, Taylor RL, Buffington CW, Klain MM, Schwartzman D. High-frequency jet ventilation: utility in posterior left atrial catheter ablation. Heart Rhythm. 2006;3:13–9. https://doi.org/10.1016/j.hrthm.2005.09.013.
Mucksavage P, Mayer WA, Mandel JE, Van Arsdalen KN. High-frequency jet ventilation is beneficial during shock wave lithotripsy utilizing a newer unit with a narrower focal zone. Can Urol Assoc J. 2010;4:333–5.
Uakritdathikarn T, Chongsuvivatwong V, Geater AF, Vasinanukorn M, Thinchana S, Klayna S. Perioperative desaturation and risk factors in general anesthesia. J Med Assoc Thai. 2008;91:1020–9.
Altun D, Çamcı E, Orhan-Sungur M, Sivrikoz N, Başaran B, Özkan-Seyhan T. High frequency jet ventilation during endolaryngeal surgery: risk factors for complications. Auris Nasus Larynx. 2018;45:1047–52.
Fernandez-Bustamante A, Ibañez V, Alfaro JJ, de Miguel E, Germán MJ, Mayo A, Jimeno A, Pérez-Cerdá F, Escribano PM. High-frequency jet ventilation in interventional bronchoscopy: factors with predictive value on high-frequency jet ventilation complications. J Clin Anesth. 2006;18:349–56.
Gammon RB, Shin MS, Buchalter SE. Pulmonary barotrauma in mechanical ventilation. Patterns Risk Factors Chest. 1992;102:568–72.
Miura MC, Ribeiro de Carvalho CR, Yamada da Silveira LT, de Moraes RM, Petri Damiani L, Fu C. The effects of recruitment maneuver during noninvasive ventilation after coronary bypass grafting: a randomized trial. J Thorac Cardiovasc Surg. 2018;156:2170–7.
Filippiadis DK, Binkert C, Pellerin O, Hoffmann RT, Kra**a A, Pereira PL. Cirse quality assurance document and standards for classification of complications: the cirse classification system. Cardiovasc Intervent Radiol. 2017;40:1141–6.
De Cassai A, Boscolo A, Tonetti T, Ban I, Ori C. Assignment of ASA-physical status relates to anesthesiologists’ experience: a survey-based national-study. Korean J Anesthesiol. 2019;72:53–9.
Galmén K, Jakobsson JG, Freedman J, Harbut P. High Frequency Jet Ventilation during stereotactic ablation of liver tumours: an observational study on blood gas analysis as a measure of lung function during general anaesthesia. F1000Research. 2019;8:386.
Heines SJ, Strauch U, Roekaerts PM, Winkens B, Bergmans DC. Accuracy of end-tidal CO2 capnometers in post-cardiac surgery patients during controlled mechanical ventilation. J Emerg Med. 2013;45:130–5.
Rackley CR. Monitoring during mechanical ventilation. Respir Care. 2020;65:832–46.
Buchan T, Walkden M, Jenkins K, Sultan P, Bandula S. High-frequency jet ventilation during cryoablation of small renal tumours. Cardiovasc Intervent Radiol. 2018;41:1067–73.
Funding
This work was supported by the Centre Hospitalier et Universitaire de Nantes (RC19_0416).
Author information
Authors and Affiliations
Contributions
All authors attest that they meet the current International Committee of Medical Journal Editors (ICMJE) criteria for Authorship. We disclose no conflict of interest and state that all the authors have contributed to this work. Their participation is as follows: TT: conceptualization, methodology, writing - original draft, writing - review & editing. ND-D: conceptualization, funding acquisition, investigation, project administration, writing - original draft. NG: conceptualization, methodology, investigation, writing - original draft, supervision. FF: methodology, data curation, formal analysis. DL: conceptualization, design. RL: investigation. FD: investigation. RD: conceptualization, methodology, investigation, writing - original draft, supervision. AD: conceptualization, methodology, investigation, writing - original draft, writing - review & editing, supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Human Rights
The authors declare that the work described has been carried out in accordance with the Declaration of Helsinki of the World Medical Association revised in 2013 for experiments involving humans.
Informed Consent and Patient Details
The authors declare that this report does not contain any personal information that could lead to the identification of the patients and that all patients gave their oral consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Co-first author: Nathalie Desfriches-Doria
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Trochu, T., Desfriches-Doria, N., Grillot, N. et al. Safety of High-Frequency Jet Ventilation During Image-Guided Thermal Ablation Procedures. Cardiovasc Intervent Radiol 46, 360–368 (2023). https://doi.org/10.1007/s00270-023-03358-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-023-03358-5