Abstract
Background
The COVID-19 pandemic has raised global health concerns and posed challenges for postoperative follow-up care for patients undergoing bariatric surgery due to social distancing rules.
Methods
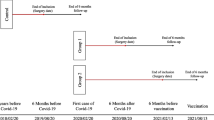
This was a cohort study on patients with morbid obesity who underwent bariatric surgery and had been enrolled in Tehran Obesity Treatment Study. Patients who had surgery between March 2020 and March 2021 were classified as those undergoing the procedure amid the COVID-19 pandemic, while those who had surgery between March 2017 and March 2018 were categorized as the pre-pandemic group.
Results
The study included 982 patients in the pre-COVID-19 pandemic group and 602 patients in the COVID-19 pandemic group, with mean ages of 39.61 and 39.51 years, respectively. After adjusting for preoperative body mass index (BMI) and surgery type, the patients who underwent surgery during the COVID-19 pandemic demonstrated comparable results to the pre-COVID-19 group in terms of total weight loss %, excess weight loss %, BMI reduction, and fat mass reduction during the 12-month postoperative period. Additionally, the rate of complications with a grade≥III based on the Clavien–Dindo classification was significantly lower in patients who underwent surgery during the COVID-19 pandemic. Notably, there were no deaths reported in either group.
Conclusion
Despite social isolation and unfavorable lifestyle modifications, bariatric surgery-induced weight loss after one year was the same in patients undergoing the procedure either before or after the implementation of social distancing measures. More research is needed to analyze the influence of the COVID-19 pandemic on the long-term outcomes of bariatric surgery.


Similar content being viewed by others
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
References
Cascella M, Rajnik M, Aleem A, Dulebohn SC, Di Napoli R. Features, evaluation, and treatment of coronavirus (COVID-19). Statpearls [internet]. 2022.
Elective surgery cancellations due to the COVID-19 pandemic: global predictive modelling to inform surgical recovery plans. Journal of British Surgery. 2020;107(11):1440–9.
Moussa O, Zakeri R, Arhi C, O’Kane M, Snowdon-Carr V, Menon V et al (2021) Impact of COVID-19 on obesity management services in the United Kingdom (The COMS-UK study). Obes Surg 31(2):904–908
Tyrrell CS, Mytton OT, Gentry SV, Thomas-Meyer M, Allen JLY, Narula AA et al (2021) Managing intensive care admissions when there are not enough beds during the COVID-19 pandemic: a systematic review. Thorax 76(3):302–312
Sen-Crowe B, Sutherland M, McKenney M, Elkbuli A (2021) A closer look into global hospital beds capacity and resource shortages during the COVID-19 pandemic. J Surg Res 260:56–63
Rubino F, Cohen RV, Mingrone G, le Roux CW, Mechanick JI, Arterburn DE et al (2020) Bariatric and metabolic surgery during and after the COVID-19 pandemic: DSS recommendations for management of surgical candidates and postoperative patients and prioritisation of access to surgery. Lancet Diabetes Endocrinol 8(7):640–648
Wiggins T, Guidozzi N, Welbourn R, Ahmed AR, Markar SR (2020) Association of bariatric surgery with all-cause mortality and incidence of obesity-related disease at a population level: A systematic review and meta-analysis. PLoS Med 17(7):e1003206
Simonnet A, Chetboun M, Poissy J, Raverdy V, Noulette J, Duhamel A et al (2020) high prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation. Obesity 28(7):1195–1199
Ahmed B, Altarawni M, Ellison J, Alkhaffaf BH (2021) Serious impacts of postponing bariatric surgery as a result of the COVID-19 pandemic: the patient perspective. J Patient Exp 8:23743735211008280
Santa-Cruz F, Siqueira LT, Coutinho LR, Leão LHA, Almeida ACA, Kreimer F et al (2022) Is COVID-19 severity impacted by bariatric surgery in the early postoperative period? Obes Surg 32(4):1178–1183
Mamidanna R, Askari A, Patel K, Adil MT, Jain V, Jambulingam P et al (2021) Safety and feasibility of resuming bariatric surgery under the cloud of COVID-19. Ann R Coll Surg Engl 103(7):524–529
Conceição E, de Lourdes M, Ramalho S, Félix S, Pinto-Bastos A, Vaz AR (2021) Eating behaviors and weight outcomes in bariatric surgery patients amidst COVID-19. Surg Obes Relat Dis 17(6):1165–1174
Crovari F, Inzunza M, Irarrázaval MJ, Romero C, Achurra P, Quezada N et al (2021) Safety of bariatric surgery during the opening phase after the first wave of the COVID-19 pandemic: experience at an academic center. Obes Surg 31(12):5376–5382
Singhal R, Tahrani AA, Sakran N, Herrera M, Menon V, Khaitan M et al (2021) Effect of COVID-19 pandemic on global bariatric surgery PRActiceS: The COBRAS study. Obes Res Clin Pract 15(4):395–401
Barzin M, Hosseinpanah F, Motamedi MA, Shapoori P, Arian P, Daneshpour MA et al (2016) Bariatric surgery for morbid obesity: tehran obesity treatment study (TOTS) rationale and study design. JMIR research protocols 5(1):e8
Verhoeff K, Mocanu V, Dang J, Wilson H, Switzer NJ, Birch DW, Karmali S (2022) Effect of the COVID-19 pandemic on bariatric surgery in North America: a retrospective analysis of 834,647 patients. Surg Obes Relat Dis 18(6):803–811
Huang EY, Grunvald E, Blitzer RR, Lee AM, Broderick RC, Li JZ, Jacobsen GR (2023) Despite regression of healthy lifestyle habits, weight loss after bariatric surgery is not affected during the COVID-19 pandemic. Surg Endosc 37(1):607–612
Alhareb A, Barajas-Gamboa JS, Tat C, Lee-St John T, Diaz Del Gobbo G, Abril C et al (2022) Resuming bariatric surgery procedures during COVID-19 pandemic: early surgical outcomes at a tertiary referral center in the Middle East. Bariatr Surg Pract Patient Care 17(2):115–20
Messiah SE, **e L, Mathew MS, Marroquin Marroquín E, Almandoz JP, Qureshi FG, de la Cruz-Muñoz N (2022) Impact of the COVID-19 pandemic on metabolic and bariatric surgery utilization and Safety in the United States. Obes Surg 32(7):2289–2298
Hardy K, Anistratov A, He W, Daeninck F, Gu J, Vergis A (2022) Bariatric patient experience with virtual care during the COVID-19 pandemic. Obes Surg 32(3):940–3
McMaster T, Wright T, Mori K, Stelmach W, To H (2012) Current and future use of telemedicine in surgical clinics during and beyond COVID-19: a narrative review. Ann Med Surg 2021(66):102378
Tewksbury C, Deleener ME, Dumon KR, Williams NN (2021) Practical considerations of develo** and conducting a successful telehealth practice in response to COVID-19. Nutr Clin Pract 36(4):769–774
Lewis C-A, de Jersey S, Seymour M, Hopkins G, Hickman I, Osland E (2020) Iron, vitamin B12, folate and copper deficiency after bariatric surgery and the impact on anaemia: a systematic review. Obes Surg 30(11):4542–4591
Barzin M, Tasdighi E, Ebadinejad A, Khalaj A, Mahdavi M, Valizadeh M, Hosseinpanah F (2022) Anemia after sleeve gastrectomy and one-anastomosis gastric bypass: an investigation based on the tehran obesity treatment study (TOTS). World J Surg 46(7):1713–1720. https://doi.org/10.1007/s00268-022-06528-7
Acknowledgements
The authors would like to thank the hospital staff, assistants, and coordinators who took part in this research. Also, special thanks to Mohammadreza Golsibi for his assistance and support in working with the electronic patient data system.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
AE, MB, FH, AK, and MV contributed to study conception and design. AE, MB, SF, FG, MRT, and SAE contributed to drafting and revising the manuscript. MM contributed to analysis and interpretation of data. AE, SF, FH, FG, MRT, AK, MM, SAE, MV, and MB contributed to final approval.
Corresponding author
Ethics declarations
Competing interest
The authors declare that they have no financial or non-financial competing interests.
Ethical approval
All the procedures performed in the study were approved by the Research Ethics Committee of the Research Institute for Endocrine Sciences of Shahid Beheshti University of Medical Sciences and were in accordance with the ethical standards of the institutional Human Research Review Committee (IR.SBMU.ENDOCRINE.REC.1401.068) and the 1964 Helsinki declaration and its later amendments. Informed written consent was obtained from all participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ebadinejad, A., Ghazy, F., Hosseinpanah, F. et al. A Comparative Analysis of Safety and Efficacy of Bariatric Surgery During the COVID-19 Pandemic and Pre-Pandemic Period: Insights from the Tehran Obesity Treatment Study. World J Surg 47, 2949–2957 (2023). https://doi.org/10.1007/s00268-023-07214-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-023-07214-y