Abstract
Background
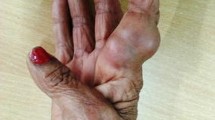
Phaeohyphomycosis is a fungal infection caused by heterogenous group of fungi known as phaeoid or dematiaceous fungi. It manifests in four clinical forms—cutaneous, subcutaneous, systemic and cerebral phaeohyphomycosis. The subcutaneous form is the most common presentation. Clinically these subcutaneous swellings resemble benign skin and soft tissue neoplasms like lipoma, sebaceous cyst or neurofibroma. Histopathology serves as a very useful tool in diagnosing these cysts by identifying the fungal elements.
Methods
A retrospective review of all cases diagnosed as phaeohyphomycosis in the department of Pathology at a tertiary care centre in South India over 9 years (January 2009–December 2017) was done. The clinical, histopathological findings of these cases were reviewed and analysed.
Results
Sixty-six cases of subcutaneous phaeohyphomycosis were reported during the 9 year period. Sixty-two per cent of these patients were diagnosed as skin and soft tissue neoplasms. In 94% cases, the extremities were affected. Multiple cysts were seen in 11% of patients. Fine needle aspiration cytology was done in 29 cases with fungal hyphae identified in all cases on cytology.
Conclusion
Subcutaneous phaeohyphomycosis mimics benign skin and soft tissue neoplasms clinically. Histopathological examination along with cytology plays a major role in diagnosis of phaeohyphomycosis and thus helps in appropriate patient management.





Similar content being viewed by others
References
Chester R, Cooper JR (2005) Deep phaeohyphomycosis. In: Merz WG, Hay RJ (eds) Topley and Wilsons microbiology and microbial infections. Hodder Arnold, London, pp 739–748
Matsumoto T (2011) Chromoblastomycosis and phaeohyphomycosis. In: Guerrant RL, Walker DH, Weller PF (eds) Tropical infectious diseases—principles, pathogens and practice. Churchill Livingstone: Elsevier Saunders, London, pp 569–572
Revankar SG, Patterson JE, Sutton DA et al (2002) Disseminated phaeohyphomycosis: review of an emerging mycosis. Clin Infect Dis 34:467–476
Ajello L, George LK, Steigbigel RT et al (1974) A case of phaeohyphomycosis caused by new species of Phialophora. Mycology 66:490–498
Chander J (2008) Phaeohyphomycosis. In: Textbook of medical mycology. Mehta Publishers, New Delhi, pp 187–199
Pappagianis D, Ajello L (1994) Dematiaceous—a mycological misnomer? J Med Vet Mycol 32:319–321
Shivaswamy KN, Pradhan P, Laxmisha C et al (2007) Disseminated phaeohyphomycosis. Int J Dermatol 46:278–281
Kimura M, Furuta T, Satou T et al (2003) Multifocal subcutaneous phaeohyphomycosis caused by Phialophora verrucosa. Arch Pathol Lab 127:91–93
Jacobson ES (2000) Pathogenic roles for fungal melanins. Clin Microbiol Rev 13:708–717
Schnitzler N, Peltroche-Liacsahuanga H, Bestier N et al (1999) Effect of melanins and carotenoids of Exophiala (Wangiella) dermatitidis on phagocytosis, oxidative burst, and killing by human neutrophils. Infect Immun 67:94–101
Haridasan S, Parameshwaran S, Bheemanathi SH et al (2017) Subcutaneous phaeohyphomycosis in kidney transplant recipients: a series of seven cases. Transpl Infect Dis 19:e12788
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
**kala, S.R., Basu, D., Neelaiah, S. et al. Subcutaneous Phaeohyphomycosis: A Clinical Mimic of Skin and Soft Tissue Neoplasms—A Descriptive Study from India. World J Surg 42, 3861–3866 (2018). https://doi.org/10.1007/s00268-018-4745-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4745-0