Abstract
Purpose
There is a dilemma as to whether the presence of degenerative changes of lateral meniscus is a contraindication to medial unicompartmental knee arthroplasty (UKA). Therefore, the purpose of this study is to assess the influence of preoperative MRI-detected lateral meniscal intra-substance signal abnormalities on mid-term functional outcomes following mobile-bearing UKA.
Methods
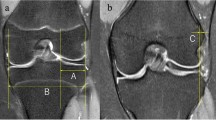
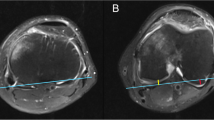
We performed a retrospective review of the record on a consecutive series of patients who have undergone mobile-bearing medial UKA from September 2020 to June 2023. The mean duration of follow-up was 2.34 years. All records were collected from case system. MRI assessment of lateral meniscus was performed with the use of the Stoller’s classification system. Patients were categorized into two groups (grade 0 and ≥ grade 1). Patient-reported outcomes were assessed with the use of the American Knee Society functional Score (AKSS-F), American Knee Society Objective Score (AKSS-O), and Oxford Knee Score (OKS) preoperatively and at latest follow-up. Furthermore, range of motion (ROM) and hip-knee-ankle angle (HKA) were measured in preoperative and postoperative periods.
Results
A total of 92 patients (101 knees) were included in our study. No differences in AKSS-F, AKSS-O, OKS, HKA, or ROM were found between those who showed normal or abnormal signal change of lateral meniscus preoperatively (P < 0.05). Furthermore, there were also no significant differences between two groups concerning AKSS-F, AKSS-O, OKS, HKA, or ROM at latest postoperative follow-up (P < 0.05). Age and duration of disease were independent predictors of low postoperative AKSS-F and AKSS-O (P < 0.05). Nevertheless, ROM was an independent predictor of high postoperative AKKS-O (P < 0.05). Age and female were independent predictors of high postoperative OKS (P < 0.05).
Conclusion
The presence of preoperative MRI-detected lateral meniscal degenerative changes did not affect mid-term functional outcomes in patients who underwent mobile-bearing medial UKA. On the basis of the results of the current study, we believe that the presence of degenerative changes of lateral meniscus is acceptable in mobile-bearing medial UKA.

Similar content being viewed by others
Data availability
All of the data are available in contact with the correspondence author.
References
Crawford DA, Berend KR, Thienpont E (2020) Unicompartmental knee arthroplasty: US and global perspectives. Orthop Clin North Am 51:147–159. https://doi.org/10.1016/j.ocl.2019.11.010
Guo WS, Zhang QD, Liu ZH, Cheng LM, Yue DB, Wang WG, Zhang NF, Li ZR (2015) Minimally invasive unicompartmental knee arthroplasty for spontaneous osteonecrosis of the knee. Orthop Surg 7:119–124. https://doi.org/10.1111/os.12172
Flury A, Weigelt L, Camenzind RS, Fritz B, Hasler J, Baumgaertner B, Helmy N, Fucentese SF (2021) Total and unicondylar knee arthroplasty are equivalent treatment options in end-stage spontaneous osteonecrosis of the knee, and the size of the lesion has no influence on the results. Knee Surg Sports Traumatol Arthrosc 29:3254–3261. https://doi.org/10.1007/s00167-020-06132-z
Johal S, Nakano N, Baxter M, Hujazi I, Pandit H, Khanduja V (2018) Unicompartmental knee arthroplasty: the past, current controversies, and future perspectives. J Knee Surg 31:992–998. https://doi.org/10.1055/s-0038-1625961
Tyagi V, Farooq M (2017) Unicompartmental knee arthroplasty: indications, outcomes, and complications. Conn Med 81:87–90
Ge J, Liu C, Sun X, Zhang Q, Ji B, Guo W (2023) Gap balance difference of unicompartmental knee arthroplasty between hanging leg and supine leg position: a prospective cohort study. Int Orthop 47:745–753. https://doi.org/10.1007/s00264-022-05680-y
Kennedy JA, Matharu GS, Hamilton TW, Mellon SJ, Murray DW (2018) Age and outcomes of medial meniscal-bearing unicompartmental knee arthroplasty. J Arthroplast 33:3153–3159. https://doi.org/10.1016/j.arth.2018.06.014
**a Z, Liow MHL, Goh GS, Chong HC, Lo NN, Yeo SJ (2018) Body mass index changes after unicompartmental knee arthroplasty do not adversely influence patient outcomes. Knee Surg Sports Traumatol Arthrosc 26:1691–1697. https://doi.org/10.1007/s00167-017-4703-7
Misir A, Uzun E, Kizkapan TB, Gunay AE, Ozcamdalli M, Husrevoglu K (2020) Lateral and patellofemoral compartment osteoarthritis progression after medial unicompartmental knee arthroplasty: A five- to 10-year follow-up study. Knee 27:1135–1142. https://doi.org/10.1016/j.knee.2020.05.021
Tay ML, McGlashan SR, Monk AP, Young SW (2022) Revision indications for medial unicompartmental knee arthroplasty: a systematic review. Arch Orthop Trauma Surg 142:301–314. https://doi.org/10.1007/s00402-021-03827-x
Castiello E, Affatato S (2020) Progression of osteoarthritis and reoperation in unicompartmental knee arthroplasty: a comparison of national joint registries. Int J Artif Organs 43:203–207. https://doi.org/10.1177/0391398819879697
Kazarian GS, Barrack TN, Okafor L, Barrack RL, Nunley RM, Lawrie CM (2020) High prevalence of radiographic outliers and revisions with unicompartmental knee arthroplasty. J Bone Joint Surg Am 102:1151–1159. https://doi.org/10.2106/JBJS.19.01277
Tay ML, Bolam SM, Maxwell AR, Hooper GJ, Monk AP, Young SW (2023) Similar survivorship but different revision reasons for uncemented mobile-bearing and cemented fixed-bearing medial UKA: a long-term population-based cohort study of 2015 patients. J Bone Joint Surg Am 105:755–761. https://doi.org/10.2106/JBJS.22.00686
Matar HE, Duckett SP, Raut V (2019) Degenerative meniscal tears of the knee: evaluation and management. Br J Hosp Med (Lond) 80:46–50. https://doi.org/10.12968/hmed.2019.80.1.46
Park SJ (2021) Midterm results of medial unicompartmental knee arthroplasty performed in patients with lateral meniscus abnormalities on preoperative mri without symptoms related to lateral meniscus. J Arthroplast 36:2759–2764. https://doi.org/10.1016/j.arth.2021.03.054
Tanaka T, Hiranaka T, Anjiki K, Fujishiro T, Okamoto K (2020) MRI-determined preoperative lateral meniscus degeneration is not associated with adverse mid-term clinical results after mobile-bearing unicompartmental knee arthroplasty. Knee 27:1279–1284. https://doi.org/10.1016/j.knee.2020.06.011
Stoller DW, Martin C, Crues JV 3rd, Kaplan L, Mink JH (1987) Meniscal tears: pathologic correlation with MR imaging. Radiology 163:731–735. https://doi.org/10.1148/radiology.163.3.3575724
Martimbianco AL, Calabrese FR, Iha LA, Petrilli M, Lira Neto O, Carneiro Filho M (2012) Reliability of the “American Knee Society Score” (AKSS). Acta Ortop Bras 20:34–38. https://doi.org/10.1590/S1413-78522012000100007
Tuğay BU, Tuğay N, Güney H, Kınıklı Gİ, Yüksel İ, Atilla B (2016) Oxford knee score: cross-cultural adaptation and validation of the Turkish version in patients with osteoarthritis of the knee. Acta Orthop Traumatol Turc 50:198–206. https://doi.org/10.3944/AOTT.2015.15.0127
Kreitz TM, Maltenfort MG, Lonner JH (2015) The valgus stress radiograph does not determine the full extent of correction of deformity prior to medial unicompartmental knee arthroplasty. J Arthroplast 30:1233–1236. https://doi.org/10.1016/j.arth.2015.02.008
Strawbridge JC, Schroeder GG, Garcia-Mansilla I, Singla A, Levine BD, Motamedi K, Jones KJ, Kremen TJ Jr (2021) The reliability of 3-T magnetic resonance imaging to identify arthroscopic features of meniscal tears and its utility to predict meniscal tear reparability. Am J Sports Med 49:3887–3897. https://doi.org/10.1177/03635465211052526
Uzun E, Misir A, Kizkapan TB, Ozcamdalli M, Gunay AE, Husrevoglu K (2020) Mid-term functional, clinical, and radiological outcomes with factors affecting revision of mobile-bearing medial unicompartmental knee arthroplasty. Knee 27:527–534. https://doi.org/10.1016/j.knee.2019.11.012
Severino FR, de Oliveira VM, de Paula Leite Cury R, Severino NR, de Moraes Barros Fucs PM (2022) Causes of knee pain evaluated by arthroscopy after knee arthroplasty: a case series. Int Orthop 46:697–703. https://doi.org/10.1007/s00264-021-05048-8
Citak M, Cross MB, Gehrke T, Dersch K, Kendoff D (2015) Modes of failure and revision of failed lateral unicompartmental knee arthroplasties. Knee 22:338–340. https://doi.org/10.1016/j.knee.2015.03.008
Kinsey TL, Anderson DN, Phillips VM, Mahoney OM (2018) Disease progression after lateral and medial unicondylar knee arthroplasty. J Arthroplast 33:3441–3447. https://doi.org/10.1016/j.arth.2018.07.019
Kaplan LM, Siljander MP, Verner JJ, Baker KC, Gehrke CK, Salisbury MR, Baker EA (2019) Analysis of retrieved unicompartmental knee implants and tissue: third-body wear as a potential contributor to progression of arthritis to adjacent compartments. Orthopedics 42:149–157. https://doi.org/10.3928/01477447-20190424-06
Slaven SE, Cody JP, Sershon RA, Ho H, Hopper RH Jr, Fricka KB (2020) The impact of coronal alignment on revision in medial fixed-bearing unicompartmental knee arthroplasty. J Arthroplast 35:353–357. https://doi.org/10.1016/j.arth.2019.09.038
Man GS, Mologhianu G (2014) Osteoarthritis pathogenesis - a complex process that involves the entire joint. J Med Life 7:37–41
Driban JB, Harkey MS, Barbe MF, Ward RJ, MacKay JW, Davis JE, Lu B, Price LL, Eaton CB, Lo GH, McAlindon TE (2020) Risk factors and the natural history of accelerated knee osteoarthritis: a narrative review. BMC Musculoskelet Disord 21:332. https://doi.org/10.1186/s12891-020-03367-2
Rodeo SA, Monibi F, Dehghani B, Maher S (2020) Biological and mechanical predictors of meniscus function: basic science to clinical translation. J Orthop Res 38:937–945. https://doi.org/10.1002/jor.24552
Kamatsuki Y, Furumatsu T, Hiranaka T, Okazaki Y, Kintaka K, Kodama Y, Miyazawa S, Ozaki T (2023) Epidemiological features of acute medial meniscus posterior root tears. Int Orthop Advance online publication. https://doi.org/10.1007/s00264-023-05848-0
Howell R, Kumar NS, Patel N, Tom J (2014) Degenerative meniscus: Pathogenesis, diagnosis, and treatment options. World J Orthop 5:597–602. https://doi.org/10.5312/wjo.v5.i5.597
Ahmad R (2021) Intra-substance meniscal changes and their clinical significance: a meta-analysis. Sci Rep 11:3642. https://doi.org/10.1038/s41598-021-83181-5
Hurst JM, Berend KR, Morris MJ, Lombardi AV Jr (2013) Abnormal preoperative MRI does not correlate with failure of UKA. J Arthroplast 28:184–186. https://doi.org/10.1016/j.arth.2013.05.011
Beckers L, Ooms D, Berger P, Van Laere K, Scheys L, Vandenneucker H (2019) Reduced bone activity in the native compartments after medial mobile-bearing unicompartmental knee arthroplasty. A prospective SPECT/CT study. Bone Joint J 101-B:915–921. https://doi.org/10.1302/0301-620X.101B8.BJJ-2018-1569.R1
Funding
This work was supported by National High Level Hospital Clinical Research Funding, Elite Medical Professionals Project of China-Japan Friendship Hospital (grant number ZRJY2021-GG08) and National Natural Science Foundation of China (grant numbers 81972130, 82072494).
Author information
Authors and Affiliations
Contributions
Handong Chen, Qidong Zhang, and Wanshou Guo designed the study; Handong Chen and Changquan Liu did the data collection. Changquan Liu and Yesihati Mulatibieke did the data analysis. Handong Chen wrote the article. Qidong Zhang and Wanshou Guo revised the article. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the institutional review board of China-Japan Friendship Hospital (approval number 2020–50-k28).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
All authors had consented to the submission of the article to the journal.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Handong Chen and Changquan Liu are co-first authors.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, H., Liu, C., Mulatibieke, Y. et al. The impact of preoperative MRI-detected lateral meniscal intra-substance signal abnormalities on mid-term functional outcomes following mobile-bearing unicompartmental knee arthroplasty. International Orthopaedics (SICOT) 47, 2467–2475 (2023). https://doi.org/10.1007/s00264-023-05919-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-05919-2