Abstract
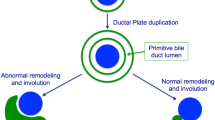
Fibropolycystic liver diseases (FLDs) make up a rare spectrum of heritable hepatobiliary diseases resulting from congenital ductal plate malformations (DPMs) due to the dysfunction of proteins expressed on the primary cilia of cholangiocytes. The embryonic development of the ductal plate is key to understanding this spectrum of diseases. In particular, DPMs can result in various degrees of intrahepatic duct involvement and a wide spectrum of cholangiopathies, including congenital hepatic fibrosis, Caroli disease, polycystic liver disease, and Von Meyenberg complexes. The most common clinical manifestations of FLDs are portal hypertension, cholestasis, cholangitis, and (in rare cases) cholangiocarcinoma. This article reviews recent updates in the pathophysiology, imaging, and clinical management of FLDs.















Similar content being viewed by others
References
Lasagni, A., et al., Fibrocystic liver disease: novel concepts and translational perspectives. Transl Gastroenterol Hepatol, 2021. 6: p. 26.
Waters, A.M. and P.L. Beales, Ciliopathies: an expanding disease spectrum. Pediatr Nephrol, 2011. 26(7): p. 1039-56.
Chen, I.Y., C.L. Whitney-Miller, and X. Liao, Congenital hepatic fibrosis and its mimics: a clinicopathologic study of 19 cases at a single institution. Diagn Pathol, 2021. 16(1): p. 81.
Finotti, M., et al., Liver transplantation for rare liver diseases and rare indications for liver transplant. Translational gastroenterology and hepatology, 2021. 6: p. 27-27.
Ogawa, M., et al., Generation of functional ciliated cholangiocytes from human pluripotent stem cells. Nat Commun, 2021. 12(1): p. 6504.
Lemaigre, F.P., Development of the Intrahepatic and Extrahepatic Biliary Tract: A Framework for Understanding Congenital Diseases. Annu Rev Pathol, 2020. 15: p. 1-22.
Leigh, M.W., et al., Clinical and genetic aspects of primary ciliary dyskinesia/Kartagener syndrome. Genet Med, 2009. 11(7): p. 473-87.
Roskams, T. and V. Desmet, Embryology of extra- and intrahepatic bile ducts, the ductal plate. Anat Rec (Hoboken), 2008. 291(6): p. 628-35.
Mitchison, H.M. and E.M. Valente, Motile and non-motile cilia in human pathology: from function to phenotypes. J Pathol, 2017. 241(2): p. 294-309.
Masyuk, A.I., T.V. Masyuk, and N.F. LaRusso, Cholangiocyte primary cilia in liver health and disease. Dev Dyn, 2008. 237(8): p. 2007-12.
Desmet, V.J., Congenital diseases of intrahepatic bile ducts: variations on the theme "ductal plate malformation". Hepatology, 1992. 16(4): p. 1069-83.
Mimatsu, K., et al., Preoperatively undetected solitary bile duct hamartoma (von Meyenburg complex) associated with esophageal carcinoma. Int J Clin Oncol, 2008. 13(4): p. 365-8.
Redston, M.S. and I.R. Wanless, The hepatic von Meyenburg complex: prevalence and association with hepatic and renal cysts among 2843 autopsies [corrected]. Mod Pathol, 1996. 9(3): p. 233-7.
Gunay-Aygun, M., Liver and kidney disease in ciliopathies. Am J Med Genet C Semin Med Genet, 2009. 151C(4): p. 296-306.
Liu, S., et al., Lesions of biliary hamartoms can be diagnosed by ultrasonography, computed tomography and magnetic resonance imaging. Int J Clin Exp Med, 2014. 7(10): p. 3370-7.
Semelka, R.C., et al., Biliary hamartomas: solitary and multiple lesions shown on current MR techniques including gadolinium enhancement. J Magn Reson Imaging, 1999. 10(2): p. 196-201.
Bachler, P., et al., Multimodality Imaging of Liver Infections: Differential Diagnosis and Potential Pitfalls. Radiographics, 2016. 36(4): p. 1001-23.
Baron, R.L., W.L. Campbell, and G.D. Dodd, 3rd, Peribiliary cysts associated with severe liver disease: imaging-pathologic correlation. AJR Am J Roentgenol, 1994. 162(3): p. 631-6.
Ryu, Y., et al., Multicystic biliary hamartoma: imaging findings in four cases. Abdom Imaging, 2010. 35(5): p. 543-7.
Xu, A.M., et al., Intrahepatic cholangiocarcinoma arising in multiple bile duct hamartomas: report of two cases and review of the literature. Eur J Gastroenterol Hepatol, 2009. 21(5): p. 580-4.
Bhalla, A., et al., Histopathological evidence of neoplastic progression of von Meyenburg complex to intrahepatic cholangiocarcinoma. Hum Pathol, 2017. 67: p. 217-224.
Rawat, D., et al., Phenotypic variation and long-term outcome in children with congenital hepatic fibrosis. J Pediatr Gastroenterol Nutr, 2013. 57(2): p. 161-6.
Johnson, C.A., P. Gissen, and C. Sergi, Molecular pathology and genetics of congenital hepatorenal fibrocystic syndromes. J Med Genet, 2003. 40(5): p. 311-9.
Zeitoun, D., et al., Congenital hepatic fibrosis: CT findings in 18 adults. Radiology, 2004. 231(1): p. 109-16.
Rock, N. and V. McLin, Liver involvement in children with ciliopathies. Clin Res Hepatol Gastroenterol, 2014. 38(4): p. 407-14.
Bayraktar, Y., et al., Congenital hepatic fibrosis associated with cavernous transformation of the portal vein. Hepatogastroenterology, 1997. 44(18): p. 1588-94.
Bergmann, C., et al., Clinical consequences of PKHD1 mutations in 164 patients with autosomal-recessive polycystic kidney disease (ARPKD). Kidney Int, 2005. 67(3): p. 829-48.
Adeva, M., et al., Clinical and molecular characterization defines a broadened spectrum of autosomal recessive polycystic kidney disease (ARPKD). Medicine (Baltimore), 2006. 85(1): p. 1-21.
Turkbey, B., et al., Autosomal recessive polycystic kidney disease and congenital hepatic fibrosis (ARPKD/CHF). Pediatr Radiol, 2009. 39(2): p. 100-11.
Srinath, A. and B.L. Shneider, Congenital hepatic fibrosis and autosomal recessive polycystic kidney disease. J Pediatr Gastroenterol Nutr, 2012. 54(5): p. 580-7.
Yonem, O. and Y. Bayraktar, Is portal vein cavernous transformation a component of congenital hepatic fibrosis? World J Gastroenterol, 2007. 13(13): p. 1928-9.
Brancatelli, G., et al., Fibropolycystic liver disease: CT and MR imaging findings. Radiographics, 2005. 25(3): p. 659-70.
Cannella, R., et al., Congenital Cystic Lesions of the Bile Ducts: Imaging-Based Diagnosis. Curr Probl Diagn Radiol, 2020. 49(4): p. 285-293.
Yoneda, N., et al., Benign Hepatocellular Nodules: Hepatobiliary Phase of Gadoxetic Acid-enhanced MR Imaging Based on Molecular Background. Radiographics, 2016. 36(7): p. 2010-2027.
Mamone, G., et al., Magnetic resonance imaging of fibropolycystic liver disease: the spectrum of ductal plate malformations. Abdom Radiol (NY), 2019. 44(6): p. 2156-2171.
CT/MRI LI-RADS® v2018 CORE. [Accessed 2022 04/22/2022]; Available from: https://www.acr.org/-/media/ACR/Files/RADS/LI-RADS/LI-RADS-2018-Core.pdf.
Arora, A. and S.K. Sarin, Multimodality imaging of obliterative portal venopathy: what every radiologist should know. Br J Radiol, 2015. 88(1046): p. 20140653.
Hartung, E.A., et al., Magnetic resonance elastography to quantify liver disease severity in autosomal recessive polycystic kidney disease. Abdom Radiol (NY), 2021. 46(2): p. 570-580.
D'Agnolo, H.M., et al., Creating an effective clinical registry for rare diseases. United European Gastroenterol J, 2016. 4(3): p. 333-8.
Lee-Law, P.Y., et al., Genetics of polycystic liver diseases. Curr Opin Gastroenterol, 2019. 35(2): p. 65-72.
Besse, W., et al., Isolated polycystic liver disease genes define effectors of polycystin-1 function. J Clin Invest, 2017. 127(5): p. 1772-1785.
Perugorria, M.J., et al., Polycystic liver diseases: advanced insights into the molecular mechanisms. Nat Rev Gastroenterol Hepatol, 2014. 11(12): p. 750-61.
Wills, E.S., R. Roepman, and J.P. Drenth, Polycystic liver disease: ductal plate malformation and the primary cilium. Trends Mol Med, 2014. 20(5): p. 261-70.
Kim, H., et al., Clinical Correlates of Mass Effect in Autosomal Dominant Polycystic Kidney Disease. PLoS One, 2015. 10(12): p. e0144526.
Qian, Q., et al., Clinical profile of autosomal dominant polycystic liver disease. Hepatology, 2003. 37(1): p. 164-71.
Van Keimpema, L., et al., Patients with isolated polycystic liver disease referred to liver centres: clinical characterization of 137 cases. Liver Int, 2011. 31(1): p. 92-8.
Zhang, Z.Y., Z.M. Wang, and Y. Huang, Polycystic liver disease: Classification, diagnosis, treatment process, and clinical management. World J Hepatol, 2020. 12(3): p. 72-83.
Waanders, E., et al., Carbohydrate antigen 19-9 is extremely elevated in polycystic liver disease. Liver Int, 2009. 29(9): p. 1389-95.
van Aerts, R.M.M., et al., Clinical management of polycystic liver disease. J Hepatol, 2018. 68(4): p. 827-837.
Bae, K.T., et al., Magnetic resonance imaging evaluation of hepatic cysts in early autosomal-dominant polycystic kidney disease: the Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease cohort. Clin J Am Soc Nephrol, 2006. 1(1): p. 64-9.
Mortelé, K.J. and H.E. Peters, Multimodality imaging of common and uncommon cystic focal liver lesions. Semin Ultrasound CT MR, 2009. 30(5): p. 368-86.
Gigot, J.F., et al., Adult polycystic liver disease: is fenestration the most adequate operation for long-term management? Ann Surg, 1997. 225(3): p. 286-94.
Schnelldorfer, T., et al., Polycystic liver disease: a critical appraisal of hepatic resection, cyst fenestration, and liver transplantation. Ann Surg, 2009. 250(1): p. 112-8.
Russell, R.T. and C.W. Pinson, Surgical management of polycystic liver disease. World J Gastroenterol, 2007. 13(38): p. 5052-9.
Drenth, J.P., et al., Medical and surgical treatment options for polycystic liver disease. Hepatology, 2010. 52(6): p. 2223-30.
Caroli, J., et al., [Congenital polycystic dilation of the intrahepatic bile ducts; attempt at classification]. Sem Hop, 1958. 34(8/2): p. 488-95/SP.
Soares, K.C., et al., Choledochal cysts: presentation, clinical differentiation, and management. J Am Coll Surg, 2014. 219(6): p. 1167-80.
Fevery, J., et al., Congenital dilatation of the intrahepatic bile ducts associated with the development of amyloidosis. Gut, 1972. 13(8): p. 604-9.
Tsuchiya, R., R. Nishimura, and T. Ito, Congenital cystic dilation of the bile duct associated with Laurence-Moon-Biedl-Bardet syndrome. Arch Surg, 1977. 112(1): p. 82-4.
Habib, S., et al., Caroli's disease and orthotopic liver transplantation. Liver Transpl, 2006. 12(3): p. 416-21.
Giovanardi, R.O., Monolobar Caroli's disease in an adult. Case report. Hepatogastroenterology, 2003. 50(54): p. 2185-7.
Waechter, F.L., et al., The role of liver transplantation in patients with Caroli's disease. Hepatogastroenterology, 2001. 48(39): p. 672-4.
Todani, T., et al., Congenital bile duct cysts: Classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg, 1977. 134(2): p. 263-9.
Ciambotti, G.F., et al., Right-sided monolobar Caroli's disease with intrahepatic stones: nonsurgical management with ERCP. Gastrointest Endosc, 1994. 40(6): p. 761-4.
Lewin, M., et al., Diffuse Versus Localized Caroli Disease: A Comparative MRCP Study. AJR Am J Roentgenol, 2021. 216(6): p. 1530-1538.
Fahrner, R., S.G. Dennler, and D. Inderbitzin, Risk of malignancy in Caroli disease and syndrome: A systematic review. World J Gastroenterol, 2020. 26(31): p. 4718-4728.
Fard-Aghaie, M.H., et al., The rate of cholangiocarcinoma in Caroli Disease A German multicenter study. HPB (Oxford), 2022. 24(2): p. 267-276.
Chung, Y.E., et al., Varying appearances of cholangiocarcinoma: radiologic-pathologic correlation. Radiographics, 2009. 29(3): p. 683-700.
Jhaveri, K.S. and H. Hosseini-Nik, MRI of cholangiocarcinoma. J Magn Reson Imaging, 2015. 42(5): p. 1165-79.
Soares, K.C., et al., Pediatric choledochal cysts: diagnosis and current management. Pediatr Surg Int, 2017. 33(6): p. 637-650.
Moslim, M.A., et al., Surgical Management of Caroli's Disease: Single Center Experience and Review of the Literature. J Gastrointest Surg, 2015. 19(11): p. 2019-27.
Arora, A., et al., Choledochal cysts: sequel of the malformed embryological ductal plate? Abdom Imaging, 2015. 40(6): p. 2062-4.
Kamisawa, T., et al., Diagnostic criteria for pancreaticobiliary maljunction 2013. J Hepatobiliary Pancreat Sci, 2014. 21(3): p. 159-61.
Shin, H.J., et al., Key imaging features for differentiating cystic biliary atresia from choledochal cyst: prenatal ultrasonography and postnatal ultrasonography and MRI. Ultrasonography, 2021. 40(2): p. 301-311.
Zhen, C., et al., Laparoscopic excision versus open excision for the treatment of choledochal cysts: a systematic review and meta-analysis. Int Surg, 2015. 100(1): p. 115-22.
Jones, R.E., et al., A narrative review of the modern surgical management of pediatric choledochal cysts. Transl Gastroenterol Hepatol, 2021. 6: p. 37.
Martins-Filho, S.N. and J. Putra, Hepatic mesenchymal hamartoma and undifferentiated embryonal sarcoma of the liver: a pathologic review. Hepat Oncol, 2020. 7(2): p. HEP19.
Chung, T., et al., Genetic, Clinicopathological, and Radiological Features of Intrahepatic Cholangiocarcinoma with Ductal Plate Malformation Pattern. Gut Liver, 2021.
Nguyen Canh, H., et al., Diversity in cell differentiation, histology, phenotype and vasculature of mass-forming intrahepatic cholangiocarcinomas. Histopathology, 2021. 79(5): p. 731-750.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sharbidre, K., Zahid, M., Venkatesh, S.K. et al. Imaging of fibropolycystic liver disease. Abdom Radiol 47, 2356–2370 (2022). https://doi.org/10.1007/s00261-022-03565-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03565-7