Abstract
Background
The role of MRI in evaluating children with an in situ gallbladder and suspected choledocholithiasis following a negative or inconclusive US is unclear.
Objective
To determine whether MRI benefits children with suspected choledocholithiasis and a normal common bile duct (CBD) without stones on US.
Materials and methods
We conducted a retrospective 10-year review of paired US and MRI (within 10 days) in children 18 years or younger with suspected choledocholithiasis. With MRI as a reference standard, two reviewers independently evaluated the images for CBD diameter, choledocholithiasis, cholelithiasis and pancreatic edema. Serum lipase was recorded. We calculated exact binomial confidence limits for test positive predictive values (PPVs) and negative predictive values (NPVs) using R library epiR.
Results
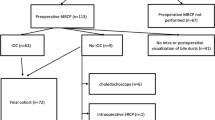
Of 87 patients (46 female, 41 male; mean age 14 years, standard deviation [SD] 4.6 years; mean interval between US and MRI 1.6 days, SD 1.8 days), 55% (48/87) had true-negative US, without CBD dilation/stones confirmed on MRI; 5% (4/87) had false-positive US showing CBD dilatation without stones, not confirmed on MRI; 33% (29/87) had true-positive US, with MRI confirming CBD dilatation; and 7% (6/87) had false-negative US, where MRI revealed CBD stones without dilatation (2 patients) and CBD dilatation with or without stones (4 patients). Patients with false-negative US had persistent or worsening symptoms, pancreatitis or SCD. The overall US false-negative rate was 17% (6/35). Normal-caliber CBD on US without stones had an NPV of 89% (48/54, 95% confidence interval: 0.77–0.96).
Conclusion
MRI adds little information in children with a sonographically normal CBD except in the setting of pancreatitis or worsening clinical symptoms. Further evaluation is warranted in children with elevated risk of stone disease.




Similar content being viewed by others
References
Lindholm EB, Meckmongkol T, Feinberg AJ et al (2019) Standardization of common bile duct size using ultrasound in pediatric patients. J Pediatr Surg 54:1123–1126
Cohen RZ, Tian H, Sauer CG et al (2021) Creation of a pediatric choledocholithiasis prediction model. J Pediatr Gastroenterol Nutr 73:636–641
Heller SL, Lee VS (2005) MR imaging of the gallbladder and biliary system. Magn Reson Imaging Clin N Am 13:295–311
Qiu Y, Yang Z, Li Z et al (2015) Is preoperative MRCP necessary for patients with gallstones? An analysis of the factors related to missed diagnosis of choledocholithiasis by preoperative ultrasound. BMC Gastroenterol 15:158
Samara O, Azzam MI, Alshrouf MA et al (2022) Diagnostic accuracy of ultrasonography compared with magnetic resonance cholangiopancreatography in the detection of choledocholithiasis. J Clin Ultrasound 50:247–253
Isherwood J, Garcea G, Williams R et al (2014) Serology and ultrasound for diagnosis of choledocholithiasis. Ann R Coll Surg Engl 96:224–228
Peterson CM, McNamara MM, Kamel IR et al (2019) ACR appropriateness criteria: right upper quadrant pain. J Am Coll Radiol 16:S235–S243
Capparelli MA, Alessandro PDD, Questa HA et al (2021) Development of a risk score for choledocholithiasis in pediatric patients. Pediatr Surg Int 37:1393–1399
Diez S, Müller H, Weiss C et al (2021) Cholelithiasis and cholecystitis in children and adolescents: does this increasing diagnosis require a common guideline for pediatricians and pediatric surgeons? BMC Gastroenterol 21:186
Chavhan GB, Babyn PS, Manson D, Vidarsson L (2008) Pediatric MR cholangiopancreatography: principles, technique, and clinical applications. Radiographics 28:1951–1962
Siegel J (2010) Pediatric sonography. Lippincott Williams & Wilkins, Philadelphia
Gwal K, Bedoya MA, Patel N et al (2015) Reference values of MRI measurements of the common bile duct and pancreatic duct in children. Pediatr Radiol 45:1153–1159
Peng R, Zhang L, Zhang XM et al (2015) Common bile duct diameter in an asymptomatic population: a magnetic resonance imaging study. World J Radiol 7:501–508
Singh A, Mann HS, Thukral CL, Singh NR (2014) Diagnostic accuracy of MRCP as compared to ultrasound/CT in patients with obstructive jaundice. J Clin Diagn Res 8:103–107
Boys JA, Doorly MG, Zehetner J et al (2014) Can ultrasound common bile duct diameter predict common bile duct stones in the setting of acute cholecystitis? Am J Surg 207:432–435
Nievelstein RA, Robben SG, Blickman JG (2011) Hepatobiliary and pancreatic imaging in children — techniques and an overview of non-neoplastic disease entities. Pediatr Radiol 41:55–75
Laing FC, Jeffrey RB Jr (1983) Choledocholithiasis and cystic duct obstruction: difficult ultrasonographic diagnosis. Radiology 146:475–479
Rothstein DH, Harmon CM (2016) Gallbladder disease in children. Semin Pediatr Surg 25:225–231
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Stock, M.R., Fine, R.O., Rivas, Y. et al. Magnetic resonance imaging following the demonstration of a normal common bile duct on ultrasound in children with suspected choledocholithiasis: what is the benefit?. Pediatr Radiol 53, 358–366 (2023). https://doi.org/10.1007/s00247-022-05537-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-022-05537-x