Abstract
Introduction and Hypothesis
Postpartum urinary retention is one of the most common complications in women during the immediate postpartum period. The objective was to systematically assess risk factors for postpartum urinary retention after vaginal delivery.
Methods
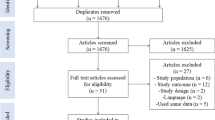
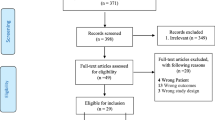
Following Preferred Reporting Items for Systematic Reviews and Meta-Analyses, we retrieved relevant studies from PubMed, Embase, Cochrane Library, Web of Science Core Collection, China National Knowledge Internet, Wangfang Database, and Chinese Biomedical Database for observational studies investigating the risk factors for postpartum urinary retention from inception to 11 November 2022. The Newcastle–Ottawa Scale and Joanna Briggs Institute's tool were used to assess the risk of bias. We conducted a meta-analysis using RevMan 5.3.
Results
In total, 3,074 articles were screened and data from 27 studies were used in the meta-analysis. Sixteen risk factors were identified, namely, labor augmentation (OR = 1.72, 95% CI = 1.17–2.51), primiparity (OR = 2.36, 95% CI = 1.64–3.38), manual fundal pressure (OR = 2.84, 95% CI = 1.00–8.11), perineal hematoma (OR = 7.28, 95% CI = 1.62–32.72), vulvar edema (OR = 7.99, 95% CI = 5.50–11.63), the total duration of labor (MD = 90.10, 95% CI = 49.11–131.08), the duration of the first stage of labor (MD = 33.97, 95% CI = 10.28–57.65), the duration of the second stage of labor (MD = 14.92, 95% CI = 11.79–18.05), the duration of the second stage of labor > 60 min (OR = 3.18, 95% CI = 1.32–7.67), mediolateral episiotomy (OR = 3.65, 95% CI = 1.70–7.83), severe perineal tear (OR = 3.21, 95% CI = 1.84–5.61), epidural analgesia (OR = 3.23, 95% CI = 1.50–6.96), forceps delivery (OR = 4.95, 95% CI = 2.88–8.51), vacuum delivery (OR = 2.44, 95% CI = 1.30–4.58), neonatal birth weight > 4,000 g (OR = 3.61, 95% CI = 1.96–6.65), and neonatal birth weight > 3,500 g (OR = 1.89, 95% CI = 1.12–3.19).
Conclusions
Our results demonstrated that labor augmentation, primiparity, manual fundal pressure, perineal hematoma, vulvar edema, the total duration of labor, the duration of the first stage of labor, the duration of the second stage of labor, the duration of the second stage of labor > 60 min, mediolateral episiotomy, severe perineal tear, epidural analgesia, forceps delivery, vacuum delivery, and neonatal birth weight > 4,000 g and > 3,500 g were risk factors for postpartum urinary retention in women with vaginal delivery. The specific ranges of the first and the second stages of labor causing postpartum urinary retention need to be clarified.

Similar content being viewed by others
Data Availability
The data are available from the corresponding author on reasonable request.
References
Mohr S, Raio L, Gobrecht-Keller U, Imboden S, Mueller MD, Kuhn A. Postpartum urinary retention: what are the sequelae? A long-term study and review of the literature. Int Urogynecol J. 2022;33(6):1601–8. https://doi.org/10.1007/s00192-021-05074-5.
Yip SK, Brieger G, Hin LY, Chung T. Urinary retention in the post-partum period. The relationship between obstetric factors and the post-partum post-void residual bladder volume. Acta Obstet Gynecol Scand. 1997;76(7):667–72. https://doi.org/10.3109/00016349709024608.
Mulder FEM, Hakvoort RA, de Bruin JP, van der Post JAM, Roovers JWR. Comparison of clean intermittent and transurethral indwelling catheterization for the treatment of overt urinary retention after vaginal delivery: a multicentre randomized controlled clinical trial. Int Urogynecol J. 2018;29(9):1281–7. https://doi.org/10.1007/s00192-017-3452-y.
Mulder FEM, Hakvoort RA, Schoffelmeer MA, Limpens J, Van der Post JAM, Roovers JPWR. Postpartum urinary retention: a systematic review of adverse effects and management. Int Urogynecol J. 2014;25(12):1605–12. https://doi.org/10.1007/s00192-014-2418-6.
Stairs J, Rolnik DL, Pascali D, Clancy A. Association between obstetrical anal sphincter injury and postpartum urinary retention: a contemporary nationwide cohort study. Int Urogynecol J. 2022;33(12):3473–9. https://doi.org/10.1007/s00192-022-05346-8.
Tiberon A, Carbonnel M, Vidart A, Ben Halima M, Deffieux X, Ayoubi JM. Risk factors and management of persistent postpartum urinary retention. J Gynecol Obstet Human Reprod. 2018;47(9):437–41. https://doi.org/10.1016/j.jogoh.2018.08.002.
Mulder F, Schoffelmeer MA, Hakvoort RA, et al. Risk factors for postpartum urinary retention: a systematic review and meta-analysis. BJOG. 2012;119(12):1440–1446. https://doi.org/10.1111/j.1471-0528.2012.03459.x
Li Q, Zhu S, **ao X. The risk factors of postpartum urinary retention after vaginal delivery: a systematic review. Int J Nurs Sci. 2020;7(4):484–92. https://doi.org/10.1016/j.ijnss.2020.09.002.
Ain QU, Shetty N, Supriya K. Postpartum urinary retention and its associated obstetric risk factors among women undergoing vaginal delivery in tertiary care hospital. J Gynecol Obstet Human Reprod. 2021;50(2):101837. https://doi.org/10.1016/j.jogoh.2020.101837.
Lawal OO, Morhason Bello IO, Atalabi OM, Ojengbede OA. Incidence of postpartum urinary retention in a tertiary hospital in Ibadan, Nigeria. Int J Gynecol Obstet. 2022;156(1):42–7. https://doi.org/10.1002/ijgo.13659.
Musselwhite KL, Faris P, Moore K, Berci D, King KM. Use of epidural anesthesia and the risk of acute postpartum urinary retention. Am J Obstet Gynecol. 2007;196(5):471–2. https://doi.org/10.1016/j.ajog.2006.11.031.
Liang C, Wong S, Tsay P, et al. The effect of epidural analgesia on postpartum urinary retention in women who deliver vaginally. Int J Obstet Anesth. 2002;11(3):164–9. https://doi.org/10.1054/ijoa.2002.0951.
Barba M, Frigerio M, Manodoro S, et al. Postpartum urinary retention: absolute risk prediction model. Low Urin Tract Sympt. 2021;13(2):257–263. https://doi.org/10.1111/luts.12362.
Polat M, Şentürk MB, Pulatoğlu Ç, Doğan O, Kılıççı Ç, Budak MŞ. Postpartum urinary retention: evaluation of risk factors. J Turkish Soc Obstet Gynecol. 2018;15(2):70–4.https://doi.org/10.4274/tjod.43931.
Perú Biurrun G, Gonzalez-Díaz E, Fernández Fernández C, Fernández Corona A. Post partum urinary retention and related risk factors. Urology. 2020;143:97–102. https://doi.org/10.1016/j.urology.2020.03.061.
Mulder FEM, Rengerink KO, van der Post JAM, Hakvoort RA, Roovers JWR. Delivery-related risk factors for covert postpartum urinary retention after vaginal delivery. Int Urogynecol J. 2016;27(1):55–60. https://doi.org/10.1007/s00192-015-2768-8.
Kekre AN, Vijayanand S, Dasgupta R, Kekre N. Postpartum urinary retention after vaginal delivery. Int J Gynecol Obstet. 2011;112(2):112–5. https://doi.org/10.1016/j.ijgo.2010.08.014.
Gupta A, Pampapati V, Khare C, Murugesan R, Nayak D, Keepanasseril A. Postpartum urinary retention in women undergoing instrumental delivery: a cross-sectional analytical study. Acta Obstet Gynecol Scand. 2021;100(1):41–7. https://doi.org/10.1111/aogs.13954.
Ching-Chung L, Shuenn-Dhy C, Ling-Hong T, Ching-Chang H, Chao-Lun C, Po-Jen C. Postpartum urinary retention: assessment of contributing factors and long-term clinical impact. Aust N Z J Obstet Gynaecol. 2002;42(4):365–8. https://doi.org/10.1111/j.0004-8666.2002.00367.x.
Yanli J, Zhipu H. Establishment of the risk prediction model of urinary retention after vaginal delivery. Med Sci J Central South China. 2021;49(6):680–82. https://doi.org/10.15972/j.cnki.43-1509/r.2021.06.015.
Yip S, Sahota D, Pang M, Chang A. Screening test model using duration of labor for the detection of postpartum urinary retention. Neurourol Urodyn. 2005;24(3):248–53. https://doi.org/10.1002/nau.20111.
Hongjuan W, Jiannv H, Liying Z. Postpartum urinary retention and its risk factors among primiparas. Mater Child Health Care China. 2021;36(06):1376–8.
Xueqi G, **aohong L, Qingyuan L. Establishment and verification of postpartum urinary retention risk scoring. J Prev Med. 2018;30(10):1064–7. https://doi.org/10.19485/j.cnki.issn2096-5087.2018.10.024.
Cuixia S, Le M. Analysis of risk factors of postpartum urinary retention[D]. Capital Medical University. 2017.
Teo R, Punter J, Abrams K, Mayne C, Tincello D. Clinically overt postpartum urinary retention after vaginal delivery: a retrospective case-control study. Int Urogynecol J. 2007;18(5):521–4. https://doi.org/10.1007/s00192-006-0183-x.
Suzuki S, Kakizaki E, Kobayashi R, Teshima S. Risk factors for postpartum urinary retention after vaginal delivery at term without epidural anesthesia. J Matern Fetal Neonatal Med. 2019;32(20):3470–2. https://doi.org/10.1080/14767058.2018.1465559.
Rosenberg M, Many A, Shinar S. Risk factors for overt postpartum urinary retention—the effect of the number of catheterizations during labor. Int Urogynecol J. 2020;31(3):529–33. https://doi.org/10.1007/s00192-019-04010-y.
Pifarotti P, Gargasole C, Folcini C, et al. Acute post-partum urinary retention: analysis of risk factors, a case–control study. Arch Gynecol Obstet. 2014;289(6):1249–53. https://doi.org/10.1007/s00404-014-3144-5.
Oh JJ, Kim SH, Shin JS, Shin SJ. Risk factors for acute postpartum urinary retention after vaginal delivery: focus on episiotomy direction. J Matern Fetal Neonatal Med. 2015;29(3):408–11. https://doi.org/10.3109/14767058.2014.1002395.
Lamblin G, Chene G, Aeberli C, et al. Identification of risk factors for postpartum urinary retention following vaginal deliveries: a retrospective case-control study. Eur J Obstet Gynecol Reprod Biol. 2019;243:7–11. https://doi.org/10.1016/j.ejogrb.2019.10.001.
Cavkaytar S, Kokanali MK, Baylas A, Topcu HO, Laleli B, Tasci Y. Postpartum urinary retention after vaginal delivery: assessment of risk factors in a case-control study. J Turk Ger Gynecol Assoc. 2014;15(3):140–3. https://doi.org/10.5152/jtgga.2014.13102.
Cao D, Rao L, Yuan J, Zhang D, Lu B. Prevalence and risk factors of overt postpartum urinary retention among primiparous women after vaginal delivery: a case-control study. BMC Pregnancy Childbirth. 2022;22(1):26. https://doi.org/10.1186/s12884-021-04369-1.
Sufen Z, Aiwu H, **aobo J. Analysis of influencing factors of postpartum urinary retention after vaginal birth. Modern Pract Med. 2018;30(08):1070–2.
Caixia Y, Shuwen T, Shuhai L, **ling C. Clinical analysis of risk factors for postpartum urinary retention in 97 primiparas through vaginal delivery. J Int Obstet Gynecol. 2018;45(6):700–3. https://doi.org/10.3969/j.issn.1674-1870.2018.06.021.
Valsky DV, Cohen SM, Lipschuetz M, Hochner-Celnikier D, Daum H, Yagel I, Yagel S. Third- or fourth-degree intrapartum anal sphincter tears are associated with levator ani avulsion in primiparas. J Ultrasound Med. 2016;35(4):709–15. https://doi.org/10.7863/ultra.15.04032.
Hilde G, Stær-Jensen J, Siafarikas F, Engh ME, Bø K. Postpartum pelvic floor muscle training, levator ani avulsion and levator hiatus area: a randomized trial. Int Urogynecol J. 2023;34(2):413–23. https://doi.org/10.1007/s00192-022-05406-z.
Ashton Miller JA, Delancey JOL. Functional anatomy of the female pelvic floor. Ann N Y Acad Sci. 2007;1101(1):266–96. https://doi.org/10.1196/annals.1389.034.
Lima C, Brito GA, Karbage S, et al. Pelvic floor ultrasound finds after episiotomy and severe perineal tear: systematic review and meta-analysis. J Matern Fetal Neonatal Med. 2022;35(12):2375–86. https://doi.org/10.1080/14767058.2020.1786049.
Youssef A, Salsi G, Cataneo I, et al. Fundal pressure in second stage of labor (Kristeller maneuver) is associated with increased risk of levator ani muscle avulsion. Ultrasound Obstet Gynecol. 2019;53(1):95–100. https://doi.org/10.1002/uog.19085.
Wei S, Luo Z, Xu H, Fraser WD. The effect of early oxytocin augmentation in labor: a meta-analysis. Obstet Gynecol. 2009;114(3):641–9. https://doi.org/10.1097/AOG.0b013e3181b11cb8.
Jiang Q, ** Z, Wang W, Ji Q, Qi C. Retrospective study to assess the effect of epidural analgesia on labor progress and women’s pelvic floor muscle from the perspective of electromyography. J Matern Fetal Neonatal Med. 2023;36(1):2211198. https://doi.org/10.1080/14767058.2023.2211198.
Fong A, Wu E, Pan D, Chung JH, Ogunyemi DA. Temporal trends and morbidities of vacuum, forceps, and combined use of both. J Matern Fetal Neonatal Med. 2014;27(18):1886–91. https://doi.org/10.3109/14767058.2014.904282.
Rusavy Z, Paymova L, Kozerovsky M, et al. Levator ani avulsion: a systematic evidence review (laser). BJOG. 2022;129(4):517–28. https://doi.org/10.1111/1471-0528.16837.
Rodriguez A, Arenas EA, Osorio AL, Mendez O, Zuleta JJ. Selective vs routine midline episiotomy for the prevention of third- or fourth-degree lacerations in nulliparous women. Am J Obstet Gynecol. 2008;198(3):281–5. https://doi.org/10.1016/j.ajog.2007.11.007.
Yuan X, Balog BM, Lin DL, et al. Brain-derived neurotrophic factor is an important therapeutic factor in mesenchymal stem cell secretions for treatment of traumatic peripheral pelvic injuries. Front Cell Neurosci. 2022;16:866094. https://doi.org/10.3389/fncel.2022.866094.
Fitzpatrick M, Herlihy OC. The effects of labour and delivery on the pelvic floor. Best Pract Res Clin Obstet Gynaecol. 2001;15(1):63–79.https://doi.org/10.1053/beog.2000.0149.
Živković K, Orešković S, Cerovac A, et al. Effects of lateral episiotomy on the emergence of urinary incontinence during the first postpartum year in primiparas: prospective cohort study. Menopausal Rev. 2021;20(4):163–9.https://doi.org/10.5114/pm.2021.110956.
Foon R, Toozs-Hobson P, Millns P, Kilby M. The impact of anesthesia and mode of delivery on the urinary bladder in the postdelivery period. Int J Gynecol Obstet. 2010;110(2):114–7. https://doi.org/10.1016/j.ijgo.2010.03.024.
Anim-Somuah M, Smyth RM, Cyna AM, Cuthbert A. Epidural versus non-epidural or no analgesia for pain management in labour. Cochrane Database Syst Rev. 2018;5(5):CD000331. https://doi.org/10.1002/14651858.CD000331.pub4.
Lam KK, Leung M, Irwin MG. Labour analgesia: update and literature review. Hong Kong Med J. 2020;26(5):413–20. https://doi.org/10.12809/hkmj208632.
Callahan E, Yeh P, Carvalho B, George RB. A survey of labour epidural practices at obstetric anesthesia fellowship programs in the United States. Can J Anaesth. 2022;69(5):591–6. https://doi.org/10.1007/s12630-022-02192-6.
Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database Syst Rev. 2009. https://doi.org/10.1002/14651858.CD000081.pub2.
Jiang H, Qian X, Carroli G, Garner P. Selective versus routine use of episiotomy for vaginal birth. Cochrane Database Syst Rev. 2017;2(2):CD000081. https://doi.org/10.1002/14651858.CD000081.pub3.
Acknowledgements
The registration number is CRD42022368621.
Funding
No external funding.
Author information
Authors and Affiliations
Contributions
X.Y.: methodology, formal analysis, data curation, writing original draft; D.Z.: methodology, formal analysis, data curation, writing original draft; W.W.: methodology; Y.X.: conceptualization, writing, reviewing, and editing.
Corresponding author
Ethics declarations
None.
Additional information
Handling Editor: Tamara Serdinšek
Editor in Chief: Kaven Baessler
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
Search Method of PubMed
#1(((((((((((((((((((Postpartum Period[MeSH Terms]) OR (Postpartum Period[Title/Abstract])) OR (Period, Postpartum[Title/Abstract])) OR (Postpartum[Title/Abstract])) OR (Postpartum Women[Title/Abstract])) OR (Women, Postpartum[Title/Abstract])) OR (Puerperium[Title/Abstract])) OR (postnatal period[Title/Abstract])) OR (Delivery, Obstetric[MeSH Terms])) OR (Deliver*, Obstetric[Title/Abstract])) OR (Obstetric Deliver*[Title/Abstract])) OR (childbirth*[Title/Abstract])) OR (Parturition[MeSH Terms])) OR (Parturition*[Title/Abstract])) OR (Birth*[Title/Abstract])) OR (Labor, Obstetric[MeSH Terms])) OR (Labor, Obstetric[Title/Abstract])) OR (Obstetric Labor[Title/Abstract])) OR (Pregnancy[MeSH Terms])) OR (Pregnanc*[Title/Abstract]).
#2((((((((((urinary retention[MeSH Terms]) OR (urinary bladder[MeSH Terms])) OR (voiding difficulty[Title/Abstract])) OR (urinary retention[Title/Abstract])) OR (postpartum voiding dysfunction[Title/Abstract])) OR (urinary voiding dysfunction[Title/Abstract])) OR (postpartum urinary retention[Title/Abstract])) OR (voiding dysfunction[Title/Abstract])) OR (bladder care[Title/Abstract])) OR (obstetric bladder management[Title/Abstract])) OR (urinary bladder[Title/Abstract]).
#3 ((((((((((((((((((((((Risk[MeSH Terms]) OR (Risk[Title/Abstract])) OR (Risks[Title/Abstract])) OR (Relative Risk[Title/Abstract])) OR (Relative Risks[Title/Abstract])) OR (Risk, Relative[Title/Abstract])) OR (Risks, Relative[Title/Abstract])) OR (Risk Factors[MeSH Terms])) OR (Risk Factor*[Title/Abstract])) OR (Factor, Risk[Title/Abstract])) OR (Social Risk Factor*[Title/Abstract])) OR (Factor*, Social Risk[Title/Abstract])) OR (Risk Factor*, Social[Title/Abstract])) OR (Health Correlates[Title/Abstract])) OR (Correlates, Health[Title/Abstract])) OR (Population* at Risk[Title/Abstract])) OR (Risk Score*[Title/Abstract])) OR (Score, Risk[Title/Abstract])) OR (Risk Factor Score*[Title/Abstract])) OR (Score, Risk Factor[Title/Abstract])) OR (predictor*[Title/Abstract])) OR (Association[MeSH Terms])) OR (Association*[Title/Abstract]).
#4 #1 AND #2 AND #3.
Search Method of the Cochrane Library
#1 Postpartum Period OR Delivery, Obstetric OR Parturition OR Labor, Obstetric OR Pregnancy OR Postpartum Period OR Period,Postpartum OR Postpartum OR Postpartum Women OR Women,Postpartum OR Puerperium OR postnatal period OR Deliver*,Obstetric OR Obstetric Deliver* OR childbirth* OR Parturition* OR Birth* OR Labor,Obstetric OR Obstetric Labor OR Pregnanc*
#2 urinary retention[MeSH Terms] OR urinary bladder[MeSH Terms] OR voiding difficulty OR urinary retention OR postpartum voiding dysfunction OR urinary voiding dysfunction OR postpartum urinary retention OR voiding dysfunction OR bladder care OR obstetric bladder management OR urinary bladder.
#3 #1 AND #2.
Search Method of Embase
#1 'postpartum'/exp OR 'puerperium'/exp OR 'postnatal period'/exp OR 'obstetric delivery'/exp OR 'childbirth'/exp OR 'birth'/exp OR 'labor'/exp OR 'pregnancy'/exp OR 'postpartum period':ab,ti OR postpartum:ab,ti OR 'postpartum women':ab,ti OR puerperium:ab,ti OR 'postnatal period':ab,ti OR 'obstetric delivery':ab,ti OR childbirth:ab,ti OR birth:ab,ti OR parturition:ab,ti OR labour:ab,ti OR labor:ab,ti OR pregnancy:ab,ti.
#2'urinary retention'/exp OR 'impaired bladder emptying'/exp OR 'postpartum urinary retention'/exp OR 'voiding difficulty':ab,ti OR 'urinary retention':ab,ti OR 'postpartum voiding dysfunction':ab,ti OR 'urinary voiding dysfunction':ab,ti OR 'postpartum urinary retention':ab,ti OR 'voiding dysfunction':ab,ti OR 'bladder care':ab,ti OR 'obstetric bladder management':ab,ti OR 'urinary bladder':ab,ti.
#3 risk:ab,ti OR 'risk factor':ab,ti OR predictor:ab,ti OR association:ab,ti OR etiology:ab,ti OR correlate:ab,ti OR 'risk'/exp OR 'risk' OR 'risk factor'/exp OR 'risk factor' OR 'predictor variable'/exp OR 'predictor variable' OR 'etiology'/exp OR 'etiology'.
#4 #1 AND #2 AND #3.
Search Method of Web of Science Core Collection
#1 Postpartum Period (主题) or Period, Postpartum (主题) or Postpartum (主题) or Postpartum Women (主题) or Women, Postpartum (主题) or Puerperium (主题) or postnatal period (主题) or Deliver*, Obstetric (主题) or Obstetric Deliver* (主题) or childbirth* (主题) or Birth* (主题) or Parturition* (主题) or Labor, Obstetric (主题) or Obstetric Labor (主题) or Pregnanc* (主题).
#2 urinary retention (主题) or urinary bladder (主题) or voiding difficulty (主题) or postpartum voiding dysfunction (主题) or urinary voiding dysfunction (主题) or postpartum urinary retention (主题) or voiding dysfunction (主题) or bladder care (主题) or obstetric bladder management (主题) or urinary bladder (主题).
#3 Risk Factors (主题) or Factor, Risk (主题) or Risk Factor (主题) or Social Risk Factors (主题) or Factor, Social Risk (主题) or Factors, Social Risk (主题) or Factor, Social Risk (主题) or Risk Factors, Social (主题) or Social Risk Factor (主题) or Health Correlates (主题) or Correlates, Health (主题) or Population at Risk (主题) or Populations at Risk (主题) or Risk Scores (主题) or Risk Score (主题) or Score, Risk (主题) or Risk Factor Scores (主题) or Risk Factor Score (主题) or Score, Risk Factor (主题) or Risk (主题) or Risks (主题) or Relative Risk (主题) or Relative Risks (主题) or Risk, Relative (主题) or Risks, Relative (主题) or Association (主题) or predictor (主题) or Associations (主题) or Etiology (主题).
Search Method of the Chinese Biomedical Database
#1 (("产后期"[不加权:扩展]) OR "分娩"[不加权:扩展]) OR "剖宫产术"[不加权:扩展].
#2 "产褥期"[常用字段:智能] OR "产妇"[常用字段:智能] OR "阴道分娩"[常用字段:智能] OR "剖宫产"[常用字段:智能] OR "产后女性"[常用字段:智能].
#3 (#2) OR (#1).
#4 ("尿潴留"[不加权:扩展]) OR "排尿困难"[不加权:扩展].
#5 "尿潴留"[常用字段:智能] OR "排尿困难"[常用字段:智能] OR "产后尿潴留"[常用字段:智能] OR "膀胱护理"[常用字段:智能] OR "产后膀胱管理"[常用字段:智能].
#6 (#4) OR (#5).
#7 ("危险因素"[不加权:扩展]) OR "预测"[不加权:扩展].
#8 "危险因素"[常用字段:智能] OR "危险"[常用字段:智能] OR "预测"[常用字段:智能] OR "相关"[常用字段:智能].
#9 (#7) OR (#8).
#10 (#3) AND (#6) AND (#9).
Search Method of China National Knowledge Internet
#1 (主题 = 危险因素) OR (主题 = 预测) OR (主题 = 危险).
#2(主题 = 尿潴留) OR (主题 = 排尿困难) OR (主题 = 产后尿潴留) OR (主题 = 膀胱护理) OR (主题 = 产后膀胱管理).
#3 (主题 = 产后期) OR (主题 = 分娩) OR (主题 = 剖宫产) OR (主题 = 产褥期) OR (主题 = 产妇) OR (主题 = 阴道分娩) OR (主题 = 产后妇女).
#4 #1 AND #2 AND #3.
Search Method of the Wangfang Database
TI = '危险因素' or TI = '预测' or TI = '危险' or TI = '生态' or TI = '相关'.
TI = '尿潴留' or TI = '排尿困难' or TI = '产后尿潴留' or TI = '膀胱护理' or TI = '产后膀胱管理'.
TI = '产后期' or TI = '分娩' or TI = '剖宫产' or TI = '产褥期' or TI = '产妇' or TI = '阴道分娩' or TI = '产后妇女'.
(危险因素 + 预测 + 危险) * (尿潴留 + 排尿困难 + 产后尿潴留 + 膀胱护理 + 产后膀胱管理) * (产后期 + 分娩 + 剖宫产 + 产褥期 + 产妇 + 阴道分娩 + 产后妇女).
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yin, X., Zhang, D., Wang, W. et al. The Risk Factors of Postpartum Urinary Retention for Women by Vaginal Birth: A Systematic Review and Meta-Analysis. Int Urogynecol J (2024). https://doi.org/10.1007/s00192-024-05853-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00192-024-05853-w