Abstract
Renal fibrosis is a progressive and chronic process that influences kidneys with chronic kidney disease (CKD), irrespective of cause, leading to irreversible failure of renal function and end-stage kidney disease. Among the signaling related to renal fibrosis, transforming growth factor-β1 (TGF-β1) signaling is a major pathway that induces the activation of myofibroblasts and the production of extracellular matrix (ECM) molecules. Apamin, a component of bee venom (BV), has been studied in relation to various diseases. However, the effect of apamin on renal interstitial fibrosis has not been investigated. The aim of this study was to estimate the beneficial effect of apamin in unilateral ureteral obstruction (UUO)-induced renal fibrosis and TGF-β1-induced renal fibroblast activation. This study revealed that obstructive kidney injury induced an inflammatory response, tubular atrophy, and ECM accumulation. However, apamin treatment suppressed the increased expression of fibrotic-related genes, including α-SMA, vimentin, and fibronectin. Administration of apamin also attenuated the renal tubular cells injury and tubular atrophy. In addition, apamin attenuated fibroblast activation, ECM synthesis, and inflammatory cytokines such as TNF-α, IL-1β, and IL-6 by suppressing the TGF-β1-canonical and non-canonical signaling pathways. This study showed that apamin inhibits UUO-induced renal fibrosis in vivo and TGF-β1-induced renal fibroblasts activation in vitro. Apamin inhibited the inflammatory response, tubular atrophy, ECM accumulation, fibroblast activation, and renal interstitial fibrosis through suppression of TGF-β1/Smad2/3 and STAT3 signaling pathways. These results suggest that apamin might be a potential therapeutic agent for renal fibrosis.
Key messages
-
UUO injury can induce renal dysfunction; however, apamin administration prevents renal failure in UUO mice.
-
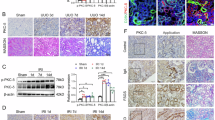
Apamin inhibited renal inflammatory response and ECM deposition in UUO-injured mice.
-
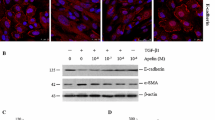
Apamin suppressed the activation of myofibroblasts in vivo and in vitro.
-
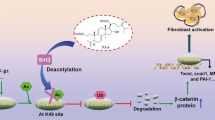
Apamin has the anti-fibrotic effect on renal fibrosis via regulation of TGF-β1 canonical and non-canonical signaling.





Similar content being viewed by others
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- α-SMA:
-
α-smooth muscle actin
- BUN:
-
Blood urea nitrogen
- BV:
-
Bee venom
- CKD:
-
Chronic kidney disease
- ECM:
-
Extracellular matrix
- FSP-1:
-
Fibroblast-specific marker-1
- IL-1β:
-
Interleukin-1β
- MCP-1:
-
Monocyte chemoattractant protein-1
- NGAL:
-
Neutrophil gelatinase-associated lipocalin
- SK channel:
-
Small conductance Ca2+-activated K+ channel
- STAT3:
-
Signal transducer and activator of transcription 3
- TβRI:
-
TGF-β type I receptor
- TβRII:
-
TGF-β type II receptor
- TGF-β1:
-
Transforming growth factor-β1
- UUO:
-
Unilateral ureteral obstruction
References
Grgic I, Kiss E, Kaistha BP, Busch C, Kloss M, Sautter J, Muller A, Kaistha A, Schmidt C, Raman G, Wulff H, Strutz F, Grone HJ, Kohler R, Hoyer J (2009) Renal fibrosis is attenuated by targeted disruption of KCa3.1 potassium channels. Proc Natl Acad Sci U S A 106(34):14518–14523
Eddy AA (2005) Progression in chronic kidney disease. Adv Chronic Kidney Dis 12(4):353–365
Zeisberg M, Neilson EG (2010) Mechanisms of tubulointerstitial fibrosis. J Am Soc Nephrol 21(11):1819–1834
Boor P, Ostendorf T, Floege J (2010) Renal fibrosis: novel insights into mechanisms and therapeutic targets. Nat Rev Nephrol 6(11):643–656
Iwano M, Neilson EG (2004) Mechanisms of tubulointerstitial fibrosis. Curr Opin Nephrol Hypertens 13(3):279–284
Jiang GT, Chen X, Li D, An HX, Jiao JD (2014) Ulinastatin attenuates renal interstitial inflammation and inhibits fibrosis progression in rats under unilateral ureteral obstruction. Mol Med Rep 10(3):1501–1508
Meng XM, Nikolic-Paterson DJ, Lan HY (2014) Inflammatory processes in renal fibrosis. Nat Rev Nephrol 10(9):493–503
Grande MT, Perez-Barriocanal F, Lopez-Novoa JM (2010) Role of inflammation in tubulo-interstitial damage associated to obstructive nephropathy. J Inflamm (Lond) 7:19
Guo G, Morrissey J, McCracken R, Tolley T, Liapis H, Klahr S (2001) Contributions of angiotensin II and tumor necrosis factor-alpha to the development of renal fibrosis. Am J Physiol Renal Physiol 280(5):F777–F785
Attisano L, Wrana JL (2002) Signal transduction by the TGF-beta superfamily. Science 296(5573):1646–1647
Shi Y, Massague J (2003) Mechanisms of TGF-beta signaling from cell membrane to the nucleus. Cell 113(6):685–700
Meng XM, Tang PM, Li J, Lan HY (2015) TGF-beta/Smad signaling in renal fibrosis. Front Physiol 6:82
Strutz F, Zeisberg M (2006) Renal fibroblasts and myofibroblasts in chronic kidney disease. J Am Soc Nephrol 17(11):2992–2998
Roberts IS, Burrows C, Shanks JH, Venning M, McWilliam LJ (1997) Interstitial myofibroblasts: predictors of progression in membranous nephropathy. J Clin Pathol 50(2):123–127
Essawy M, Soylemezoglu O, Muchaneta-Kubara EC, Shortland J, Brown CB, el Nahas AM (1997) Myofibroblasts and the progression of diabetic nephropathy. Nephrol Dial Transplant 12(1):43–50
Lebrin F, Goumans MJ, Jonker L, Carvalho RL, Valdimarsdottir G, Thorikay M, Mummery C, Arthur HM, ten Dijke P (2004) Endoglin promotes endothelial cell proliferation and TGF-beta/ALK1 signal transduction. EMBO J 23(20):4018–4028
Wrana JL, Attisano L, Wieser R, Ventura F, Massague J (1994) Mechanism of activation of the TGF-beta receptor. Nature 370(6488):341–347
Horvath CM (2000) STAT proteins and transcriptional responses to extracellular signals. Trends Biochem Sci 25(10):496–502
Ogata H, Chinen T, Yoshida T, Kinjyo I, Takaesu G, Shiraishi H, Iida M, Kobayashi T, Yoshimura A (2006) Loss of SOCS3 in the liver promotes fibrosis by enhancing STAT3-mediated TGF-beta1 production. Oncogene 25(17):2520–2530
Fuller GM, Zhang Z (2001) Transcriptional control mechanism of fibrinogen gene expression. Ann N Y Acad Sci 936:469–479
Kuratsune M, Masaki T, Hirai T, Kiribayashi K, Yokoyama Y, Arakawa T, Yorioka N, Kohno N (2007) Signal transducer and activator of transcription 3 involvement in the development of renal interstitial fibrosis after unilateral ureteral obstruction. Nephrology (Carlton) 12(6):565–571
Pang M, Ma L, Gong R, Tolbert E, Mao H, Ponnusamy M, Chin YE, Yan H, Dworkin LD, Zhuang S (2010) A novel STAT3 inhibitor, S3I-201, attenuates renal interstitial fibroblast activation and interstitial fibrosis in obstructive nephropathy. Kidney Int 78(3):257–268
Kwon YB, Lee JD, Lee HJ, Han HJ, Mar WC, Kang SK, Beitz AJ, Lee JH (2001) Bee venom injection into an acupuncture point reduces arthritis associated edema and nociceptive responses. Pain 90(3):271–280
Banks BE, Brown C, Burgess GM, Burnstock G, Claret M, Cocks TM, Jenkinson DH (1979) Apamin blocks certain neurotransmitter-induced increases in potassium permeability. Nature 282(5737):415–417
Mourre C, Fournier C, Soumireu-Mourat B (1997) Apamin, a blocker of the calcium-activated potassium channel, induces neurodegeneration of Purkinje cells exclusively. Brain Res 778(2):405–408
Moreno M, Giralt E (2015) Three valuable peptides from bee and wasp venoms for therapeutic and biotechnological use: melittin, apamin and mastoparan. Toxins (Basel) 7(4):1126–1150
Ovcharov R, Shkenderov S, Mihailova S (1976) Anti-inflammatory effects of apamin. Toxicon 14(6):441–447
Kim SJ, Park JH, Kim KH, Lee WR, An HJ, Min BK, Han SM, Kim KS, Park KK (2012) Apamin inhibits THP-1-derived macrophage apoptosis via mitochondria-related apoptotic pathway. Exp Mol Pathol 93(1):129–134
Kim WH, An HJ, Kim JY, Gwon MG, Gu H, Lee SJ, Park JY, Park KD, Han SM, Kim MK, Park KK (2017) Apamin inhibits TNF-alpha- and IFN-gamma-induced inflammatory cytokines and chemokines via suppressions of NF-kappaB signaling pathway and STAT in human keratinocytes. Pharmacol Rep 69(5):1030–1035
Lee WR, Kim KH, An HJ, Kim JY, Lee SJ, Han SM, Pak SC, Park KK (2014) Apamin inhibits hepatic fibrosis through suppression of transforming growth factor beta1-induced hepatocyte epithelial-mesenchymal transition. Biochem Biophys Res Commun 450(1):195–201
Chevalier RL, Forbes MS, Thornhill BA (2009) Ureteral obstruction as a model of renal interstitial fibrosis and obstructive nephropathy. Kidney Int 75(11):1145–1152
Better OS, Arieff AI, Massry SG, Kleeman CR, Maxwell MH (1973) Studies on renal function after relief of complete unilateral ureteral obstruction of three months' duration in man. Am J Med 54(2):234–240
Sacks SH, Aparicio SA, Bevan A, Oliver DO, Will EJ, Davison AM (1989) Late renal failure due to prostatic outflow obstruction: a preventable disease. BMJ 298(6667):156–159
Kim SJ, Park JH, Kim KH, Lee WR, Pak SC, Han SM, Park KK (2012) The protective effect of apamin on LPS/fat-induced atherosclerotic mice. Evid Based Complement Alternat Med 2012:305454–305410
Schaefer N, Tahara K, von Websky M, Wehner S, Pech T, Tolba R, Abu-Elmagd K, Kalff JC, Hirner A, Turler A (2008) Role of resident macrophages in the immunologic response and smooth muscle dysfunction during acute allograft rejection after intestinal transplantation. Transpl Int 21(8):778–791
Lin SL, Castano AP, Nowlin BT, Lupher ML Jr, Duffield JS (2009) Bone marrow Ly6Chigh monocytes are selectively recruited to injured kidney and differentiate into functionally distinct populations. J Immunol 183(10):6733–6743
Cranford TL, Enos RT, Velazquez KT, McClellan JL, Davis JM, Singh UP, Nagarkatti M, Nagarkatti PS, Robinson CM, Murphy EA (2016) Role of MCP-1 on inflammatory processes and metabolic dysfunction following high-fat feedings in the FVB/N strain. Int J Obes 40(5):844–851
Zhang L, Xu X, Yang R, Chen J, Wang S, Yang J, **ang X, He Z, Zhao Y, Dong Z, Zhang D (2015) Paclitaxel attenuates renal interstitial fibroblast activation and interstitial fibrosis by inhibiting STAT3 signaling. Drug Des Devel Ther 9:2139–2148
Kim JY, Kim KH, Lee WR, An HJ, Lee SJ, Han SM, Lee KG, Park YY, Kim KS, Lee YS, Park KK (2015) Apamin inhibits PDGF-BB-induced vascular smooth muscle cell proliferation and migration through suppressions of activated Akt and Erk signaling pathway. Vasc Pharmacol 70:8–14
Hu J, Zhu Q, Li PL, Wang W, Yi F, Li N (2015) Stem cell conditioned culture media attenuated albumin-induced epithelial-mesenchymal transition in renal tubular cells. Cell Physiol Biochem 35(5):1719–1728
Chen X, Wei SY, Li JS, Zhang QF, Wang YX, Zhao SL, Yu J, Wang C, Qin Y, Wei QJ, Lv GX, Li B (2016) Overexpression of heme oxygenase-1 prevents renal interstitial inflammation and fibrosis induced by unilateral ureter obstruction. PLoS One 11(1):e0147084
Ucero AC, Benito-Martin A, Izquierdo MC, Sanchez-Nino MD, Sanz AB, Ramos AM, Berzal S, Ruiz-Ortega M, Egido J, Ortiz A (2014) Unilateral ureteral obstruction: beyond obstruction. Int Urol Nephrol 46(4):765–776
Liu N, Tolbert E, Pang M, Ponnusamy M, Yan H, Zhuang S (2011) Suramin inhibits renal fibrosis in chronic kidney disease. J Am Soc Nephrol 22(6):1064–1075
Varelas X, Sakuma R, Samavarchi-Tehrani P, Peerani R, Rao BM, Dembowy J, Yaffe MB, Zandstra PW, Wrana JL (2008) TAZ controls Smad nucleocytoplasmic shuttling and regulates human embryonic stem-cell self-renewal. Nat Cell Biol 10(7):837–848
Bond CT, Herson PS, Strassmaier T, Hammond R, Stackman R, Maylie J, Adelman JP (2004) Small conductance Ca2+-activated K+ channel knock-out mice reveal the identity of calcium-dependent afterhyperpolarization currents. J Neurosci 24(23):5301–5306
Liu BC, Tang TT, Lv LL, Lan HY (2018) Renal tubule injury: a driving force toward chronic kidney disease. Kidney Int 93(3):568–579
Wynn TA (2008) Cellular and molecular mechanisms of fibrosis. J Pathol 214(2):199–210
Misseri R, Rink RC, Meldrum DR, Meldrum KK (2004) Inflammatory mediators and growth factors in obstructive renal injury. J Surg Res 119(2):149–159
Duffield JS (2011) Macrophages in kidney repair and regeneration. J Am Soc Nephrol 22(2):199–201
Ren J, Li J, Liu X, Feng Y, Gui Y, Yang J, He W, Dai C (2016) Quercetin inhibits fibroblast activation and kidney fibrosis involving the suppression of mammalian target of rapamycin and beta-catenin signaling. Sci Rep 6:23968
Sureshbabu A, Muhsin SA, Choi ME (2016) TGF-beta signaling in the kidney: profibrotic and protective effects. Am J Physiol Renal Physiol 310(7):F596–F606
Yeh YC, Wei WC, Wang YK, Lin SC, Sung JM, Tang MJ (2010) Transforming growth factor-{beta}1 induces Smad3-dependent {beta}1 integrin gene expression in epithelial-to-mesenchymal transition during chronic tubulointerstitial fibrosis. Am J Pathol 177(4):1743–1754
Shirakihara T, Horiguchi K, Miyazawa K, Ehata S, Shibata T, Morita I, Miyazono K, Saitoh M (2011) TGF-beta regulates isoform switching of FGF receptors and epithelial-mesenchymal transition. EMBO J 30(4):783–795
Shen B, Liu X, Fan Y, Qiu J (2014) Macrophages regulate renal fibrosis through modulating TGFbeta superfamily signaling. Inflammation 37(6):2076–2084
Cheng X, Song Y, Wang Y (2019) pNaKtide ameliorates renal interstitial fibrosis through inhibition of sodium-potassium adenosine triphosphatase-mediated signaling pathways in unilateral ureteral obstruction mice. Nephrol Dial Transplant 34(2):242–252
Tang PC, Zhang YY, Chan MK, Lam WW, Chung JY, Kang W, To KF, Lan HY, Tang PM (2020) The emerging role of innate immunity in chronic kidney diseases. Int J Mol Sci 21(11). https://doi.org/10.3390/ijms21114018
Meng XM, Nikolic-Paterson DJ, Lan HY (2016) TGF-beta: the master regulator of fibrosis. Nat Rev Nephrol 12(6):325–338
Lan HY, Chung AC (2012) TGF-beta/Smad signaling in kidney disease. Semin Nephrol 32(3):236–243
Derynck R, Zhang YE (2003) Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature 425(6958):577–584
Tang PM, Zhang YY, Lan HY (2018) LncRNAs in TGF-beta-driven tissue fibrosis. Noncoding RNA 4(4). https://doi.org/10.3390/ncrna4040026
Liu J, Zhong Y, Liu G, Zhang X, **ao B, Huang S, Liu H, He L (2017) Role of Stat3 signaling in control of EMT of tubular epithelial cells during renal fibrosis. Cell Physiol Biochem 42(6):2552–2558
Nakao A, Afrakhte M, Moren A, Nakayama T, Christian JL, Heuchel R, Itoh S, Kawabata M, Heldin NE, Heldin CH, ten Dijke P (1997) Identification of Smad7, a TGFbeta-inducible antagonist of TGF-beta signalling. Nature 389(6651):631–635
Funding
This work was supported by the Korea Institute of Planning and Evaluation for Technology in Food, Agriculture, Forestry (IPET) through the Useful Agricultural Life Resources Industry Technology Development Program, funded by the Ministry of Agriculture, Food and Rural Affairs (MAFRA) (grant number 120040-02-1).
Author information
Authors and Affiliations
Contributions
M.-G.G. and K.-K.P. participated in the design of the study. M.-G.G., H.-J.A., and H.G. performed the experiments. Y.-A.K. and S.M.H. performed the data analysis. M.-G.G. and K.-K.P. drafted the manuscripts. All authors discussed, revised, and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All protocols for animal study were approved by the Institutional Animal Care and Use Committee of the Catholic University of Daegu (EXP-IRB number: DCIAFCR-160705-6-Y). All animal experiments have been performed in accordance with the ethical standards outlined in the Best Practice Guidelines on Publishing Ethics.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Fig. S1
Establishment of the renal fibrosis models and schematic diagram of apamin treatment. a Establishment of the renal fibrosis model and schematic diagram of apamin administration. Apamin treatment at a concentration of 0.5 mg/kg was given via intraperitoneal injection twice a week (PNG 269 kb)
Fig. S2
Apamin attenuated the renal tubular injury in UUO mice. a The protein expressions of E-cadherin and NGAL, the markers of tubular injury, were analyzed with western blotting analysis. The quantitative graphs show protein expression of b E-cadherin and c NGAL normalized with GAPDH. *p < 0.05 compared to the normal control group; †p < 0.05 compared to the UUO group (PNG 617 kb)
Rights and permissions
About this article
Cite this article
Gwon, MG., An, HJ., Gu, H. et al. Apamin inhibits renal fibrosis via suppressing TGF-β1 and STAT3 signaling in vivo and in vitro. J Mol Med 99, 1265–1277 (2021). https://doi.org/10.1007/s00109-021-02087-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-021-02087-x